You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Vertical ridge augmentation techniques are often required in areas where bone and/or tissue volume loss has occurred as a result of tooth extraction, trauma, and/or changes in tooth position.1-3 These areas typically require staged surgical interventions (ie, delayed grafting) to augment the tissue through bone and/or tissue grafting to increase the vertical and horizontal dimensions of the ridge and enhance overall bone quality and quantity for future implant placement.4,5 Once bone healing and successful tissue thickening have occurred, implants can be placed in the site, along with an abutment and provisional restoration.6
Vertical Ridge Augmentation Development
The research, development, and evolution of vertical ridge augmentation techniques utilizing guided bone regeneration (GBR) with membranes can best be discussed in terms of three significant time periods. The development period of such techniques generally occurred between 1989 and 1996, during which time several preclinical and clinical research studies were performed. From 1996 through 2005, results from those initial investigations were consolidated for both retrospective and prospective long-term evaluation. Since then, the third period has been characterized by the simplification of older procedures in efforts to make vertical ridge augmentation treatments less invasive and more predictable for patients.
Vertical ridge augmentation technique development began with animal research in dogs.7 Implants were placed in the bone to a depth of approximately 4 mm, with their coronal portion protruding approximately 5 mm. The defect was covered with a nonresorbable membrane (eg, Gore-Tex® ePTFE), and the space under the membrane filled with peripheral venous blood clot without any filling material. The sites were allowed to heal for approximately 4 months. Radiographic examination 4 months after surgery compared to initial placement revealed complete bone regeneration. Histologic and histomorphometric analysis showed a significantly larger amount of bone fill at the test site, and clinical evaluation revealed that the implants were completely covered by tissue resembling bone. In most instances, bone had grown to the top of the membrane, whereas in the control site, no bone formation was present and a complete collapse of soft tissue occurred.7
When initial clinical research was undertaken, investigators studied the effect of adding demineralized freeze-dried bone allograft or autogenous bone chips to a membrane technique for vertical bone regeneration in humans.8 Two groups of partially edentulous patients with vertical jawbone defects were treated: 10 partially edentulous patients with membrane (eg, Gore-Tex) and demineralized freeze-dried bone allograft particles condensed under the membrane; and 10 partially edentulous patients with autogenous bone chips.8 The membranes were left completely covered by the soft tissue during healing. At reentry after between 7 and 11 months, the membranes were removed. Clinical and histologic results showed a beneficial effect of the addition of demineralized freeze-dried bone allograft or autogenous bone particles to vertical ridge augmentation procedures in humans.8
As vertical ridge augmentation techniques further developed, research efforts focused on reducing the amount of bone that had to be harvested from the patient. In particular, efficacy of a 1:1 mixture of deproteinized bovine bone mineral (DBBM) and autogenous bone graft associated with an expanded-polytetrafluoroethylene (e-PTFE) membrane was evaluated from a histological and histomorphometrical perspective when placed for vertical ridge augmentation in human subjects.9
The vertical augmentation procedures were performed on seven patients with partially edentulous mandibular jaws who required vertical ridge augmentation. A combination of a titanium-reinforced e-PTFE Gore-Tex membrane and a composite graft with a 1:1 ratio of DBBM (Bio-Oss®, Geistlich Pharma North America Inc., www.geistlich-na.com) and autogenous bone was placed, along with implants, and a 6-month healing period was allowed. Tissue samples from regenerated areas were analyzed histologically and histomorphometrically.9
The histological analysis showed new bone formation, and ongoing remodeling of the autogenous bone and the DBBM particles was observed. Clinically, the implants appeared stable and submerged by hard regenerated tissue similar to bone at the abutment connection. The results, therefore, supported the use of a 1:1 combination of DBBM and autogenous bone chips for vertical ridge augmentation with GBR techniques.9
Vertical Ridge Augmentation Technique
There are essentially two approaches for regenerating the bone vertically and horizontally: the simultaneous approach and the staged approach (Figure 1). The simultaneous approach is reserved for easier cases, those usually not in the esthetic zone. It is ideal for small defects and can be performed 2 months after tooth extraction. The implant can be positioned and the bone regenerated around the defect with autogenous bone chips and usually a resorbable membrane to cover the implant surface. After a healing period of 4 months, the second-stage surgery is performed, at which time the implant abutment is connected and, after 1 month of healing, the provisional restoration is placed.
The staged approach is appropriate for more advanced defects in the most difficult clinical cases. Approximately 2 months after tooth extraction to allow for complete soft-tissue healing, bone regeneration with a submerged, nonresorbable e-PTFE membrane is initiated prior to implant placement. Between 6 to 8 months are allowed for healing before reopening the site, at which time the membrane is removed and the implant placed. The implant remains submerged for approximately 4 months, at which point second-stage surgery is performed (approximately 12 months after extraction), an abutment is placed, and the implant provisionalized.
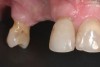
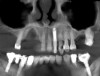
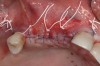
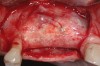
For an example of the staged approach, a female patient presented with a large residual defect following removal of a cyst in the affected area (Figure 2). The palatal bone plate was very thin, and some fenestrations were also present (Figure 3). Two vertical releasing incisions were made to facilitate a large full-thickness flap, and the periosteum was completely elevated, leaving the least possible amount of connective and soft tissue on the bone site. The palatal flap was also elevated, after which the adjacent tooth root was carefully planed. The bone was curettaged to ensure that no connective tissue remained in the site; the goal was not to regenerate connective tissue, but only bone.
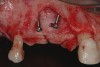
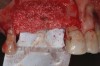
Two dentine screws were placed to support the nonresorbable titanium-reinforced membrane both horizontally and vertically and to avoid collapse of the membrane itself toward the defect (Figure 4). A dense e-PTFE membrane was cut and folded to adapt it to the anatomical situation, and the graft was placed (Figure 5). The graft was a mixture of 30% deproteinized bone and 70% autogenous bone chips harvested from the mandibular retromolar area. The membrane was then adapted and fixed with free tacks in the buccal and palatal positions (Figure 6).
The flap was released with a single, continuous cut from mesial to distal through the periosteum to ensure the flap would be sufficiently loose to facilitate suturing without any tension. Three horizontal mattress sutures (Teflon™ PTFE) were placed in such a way that the two flaps could be reflected at a subsequent appointment. Suturing was completed with a series of very thin, interrupted stitches (Prolene 6-0) (Figure 7).
At the second-stage surgery for implant placement, no inflammation was present. A full-thickness flap was made and detached from the membrane surface, the dense PTFE membrane was removed, and the tacks were removed using a periosteal elevator. Good quality bone was observed (Figure 8).
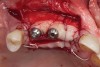
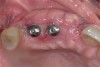
The implants and healing caps were placed (Figure 9). Implant stability was verified, and a second incision was made to prevent tension on the flap. A second layer of deproteinized bovine bone was placed to augment the site volume as much as possible, after which a collagen matrix was placed to augment the soft-tissue thickness. Horizontal mattress sutures were placed without tension, followed by very thin stitches.
After 4 months of healing, the implants were uncovered by making an apically repositioned flap to move the keratinizing mucosa from the palatal aspect to the buccal aspect. Two vertical releasing incisions, along with a partial-thickness palatal incision, were made to expose the implants, enable removal of the cover screws, and facilitate removal of the keratinized mucosa. The connective tissue graft and a portion of the palatal flap was moved coronally to close the area, after which the site was sutured and allowed to heal for a secondary intention.
After 15 days of healing, a nice volume of keratinized mucosa and tissue was present (Figure 10). This indicated that the prosthodontist could proceed with provisionalization (Figure 11), which would condition the soft tissue for creating an esthetic emergence profile for the definitive implant-supported restorations (Figure 12).6
Retrospective and Prospective Observations
The long-term results of these types of treatments are significant, because while immediate and short-term success is encouraging, the long-term implications of such therapies impact treatment longevity. A retrospective study evaluated, after 1 to 5 years of prosthetic loading, a total of 123 implants that were consecutively inserted at the time of vertical ridge augmentation in four practices.10 At the time of implant surgery, three different techniques were used. The implants were protruded between 2 mm and 7 mm from the bone, and an e-PTFE membrane was placed to protect either a blood clot, an allograft, or an autograft. One implant failed immediately after second-stage surgery and was replaced with a new implant after 1 month. The remaining implants were clinically stable, with no signs of radiolucency at the bone–implant interface; they were determined to be successfully osseointegrated. Radiographic analysis revealed stable bone crest levels, with a mean bone loss of 1.35 mm for blood clots, 1.87 mm for allografts, and 1.71 mm for autografts. Two implants demonstrated increased crestal bone loss of 3.5 mm and 4 mm, respectively, at the first-year examination.
Such results confirmed previous research regarding regenerated bone. They also supported conclusions that vertically augmented bone using GBR techniques for implant placement responds similarly to native, nonregenerated bone. In fact, the main crestal bone loss was only between 1.3 mm and 1.9 mm.
More recently, a 13- to 21-year retrospective was published that evaluated vertical ridge augmentation with GBR in patients who received machined-surface implants.11 Of the original 76 patients treated with 197 implants, 33 patients who received 91 implants placed in vertically augmented ridges by means of GBR techniques could be found. After a mean follow-up of 15 years, a total of 88 implants were in function (ie, 97% survival rate), but nine exhibited peri-implantitis (ie, 9.9%). Between the baseline evaluation at 1 year after loading and the final visit sometime 13 to 21 years later, a mean radiographic bone loss of 1.02 mm was observed. These findings suggest that machined-surface implants placed in vertically augmented bone remain stable after many years of function.
Conclusion
After years of research, development, and evolution, vertical ridge augmentation techniques utilizing GBR with membranes and grafts for implant placement have shown to be successful in contributing to long-term implant efficacy and function. Results from initial investigations and subsequent efforts to simplify procedures demonstrate that vertical ridge augmentation techniques can successfully augment and regenerate bone tissue for patients in defective sites. Additionally, implants placed in those sites have remained stable and functioned predictably for the long term, on average with minimal bone loss.
ABOUT THE AUTHOR
Massimo Simion, MD, DDS
Professor, Department of Periodontology, University of Milan School of Dentistry, Milan, Italy
REFERENCES
1. Doonquah L, Lodenquai R, Mitchell AD. Surgical techniques for augmentation in the horizontally and vertically compromised alveolus. Dent Clin North Am. 2015;59(2):389-407.
2. Petropoulou A, Pappa E, Pelekanos S. Esthetic considerations when replacing missing maxillary incisors with implants: a clinical report. J Prosthet Dent. 2013;109(3):140-144.
3. Shah KC, Lum MG. Treatment planning for the single-tooth implant restoration—general considerations and the pretreatment evaluation. J Calif Dent Assoc. 2008;36(11):827-834.
4. Aloy-Prósper A, Peñarrocha-Oltra D, Peñarrocha-Diago M, et al. Peri-implant hard and soft tissue stability in implants placed simultaneously versus delayed with intraoral block bone grafts in horizontal defects: a retrospective case series study. Int J Oral Maxillofac Implants. 2016;31(1):133-141.
5. Buser D, Dula K, Hirt HP, Schenk RK. Lateral ridge augmentation using autografts and barrier membranes: a clinical study with 40 partially edentulous patients. J Oral Maxillofac Surg. 1996;54(4):420-432.
6. Shor A, Schuler R, Goto Y. Indirect implant-supported fixed provisional restoration in the esthetic zone: fabrication technique and treatment workflow. J Esthet Restor Dent. 2008;20(2):82-95.
7. Simion M, Dahlin C, Rocchietta I, et al. Vertical ridge augmentation with guided bone regeneration in association with dental implants: an experimental study in dogs. Clin Oral Implants Res. 2007;18(1):86-94.
8. Simion M, Jovanovic SA, Trisi P, et al. Vertical ridge augmentation around dental implants using a membrane technique and autogenous bone or allografts in humans. Int J Periodontics Restorative Dent. 1998;18(1):8-23.
9. Simion M, Fontana F, Rasperini G, Maiorana C. Vertical ridge augmentation by expanded-polytetrafluoroethylene membrane and a combination of intraoral autogenous bone graft and deproteinized anorganic bovine bone (Bio Oss). Clin Oral Implants Res. 2007;18(5):620-629.
10. Simion M, Jovanovic SA, Tinti C, Benfenati SP. Longterm evaluation of osseointegrated implants inserted at the time or after vertical ridge augmentation. A retrospective study on 123 implants with 1-5 year follow-up. Clin Oral Implants Res. 2001;12(1):35-45.
11. Simion M, Ferrantino L, Idotta E, Zarone F. Turned implants in vertical augmented bone: a retrospective study with 13 to 21 years follow-up. Int J Periodontics Restorative Dent. 2016;36(3):309-317.