You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
OXYGEN CYLINDERS AND REGULATORS
Every dental office must be equipped with an oxygen source. Hospitals and other large healthcare facilities rely on bulk liquid oxygen supply systems that reduce cost and storage space. For outpatient facilities, oxygen is transported as compressed gas in steel or alloy cylinders of various sizes. Large H-cylinders and portable E-cylinders are most commonly used in the dental environment. Regardless of whether treatment rooms are plumbed with central oxygen sources (generally H-cylinders), emergencies may occur anywhere in the office and a portable E-cylinder of oxygen should always be available. At least one additional backup cylinder should be kept in reserve.
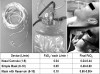
All cylinders contain a small valve stem at its top that is turned counterclockwise using a wrench or hand wheel to release oxygen into an attached regulator. Regulators come in various designs, but they all have three essential components: (a) a pressure gauge that registers the content of the tank in pounds per square inch (psi) when the valve stem is turned on; (b) a flow meter that registers the oxygen flow in liters per minute; and (c) a corrugated adaptor to which standard oxygen tubing can be attached. This tubing then connects to a supplemental or positive pressure device. The ideal regulator should allow for an oxygen flow of at least 15 liters per minute (Figure 1).
E-cylinders provide the most appropriate balance of having sufficient oxygen for an emergency, yet are small enough to be portable. A full E-cylinder holds over 600 liters of oxygen and will indicate a pressure of approximately 2,200 psi (Figure 1). They should be replaced when their content falls to 500 psi. Estimates of time remaining in oxygen cylinders can be approximated using the following formula where the conversion factor (F) = ~0.3 for E-cylinders and ~3.0 for large H-cylinders that supply central plumbing: (psi x F) ÷ L/min = time remaining in minutes.1 For example, if a flow of 15 L/min is required from an E-cylinder containing 500 psi, the time remaining would be only 10 minutes. A full tank would provide approximately 44 minutes.
DEVICES FOR SUPPLEMENTAL OXYGENATION
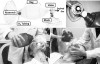
Nasal cannulas, nasal hoods, various mask designs, and certain resuscitation bags may be used to provide supplemental oxygen for the spontaneously breathing patient (Figure 2). The nasal cannula is ideal for administering supplemental oxygen to sedated patients as well as those experiencing a medical complication. Facemasks provide higher oxygen concentrations but such concentrations may not be required depending upon the situation. Each liter per minute of oxygen provided via nasal cannula increases the percent oxygen inspired (FIO2) by approximately 4% above room air (FIO2 = 20 + [4 x L/min]).1 This formula approximates oxygen concentration delivered by nasal cannula only. It is not applicable to full masks or nasal masks (nasal hoods) used with nitrous oxide/oxygen units. Flow rates greater than 4 L/min may become uncomfortable over time, but 4 L/min to 6 L/min delivering 36% to 44% oxygen should be adequate supplementation for most medical emergencies if the patient is breathing. For routine supplementation during minimal or moderate procedural sedation, 2 L/min or 28% oxygen is conventional.
Oxygen masks are available in countless designs. Traditionally, pre-hospital emergency responders set the mask flow at 10 L/min as standard practice. Regardless of the mask design, a minimum of 6 L/min should be delivered to the mask before placing it on the patient. The simple oxygen mask has no reservoir bag and will provide approximately 60% oxygen at 10 L/min.1 This concentration is adequate for virtually all medical emergencies, and the simple mask is straightforward in use. Nasal masks (hoods) used with nitrous oxide/oxygen machines are also easy to use, but precise oxygen concentrations inspired for each L/min of oxygen delivered have not been established. At 6 L/min to 10 L/min, one might reasonably presume that FIO2 will be higher than those with nasal cannulas but less than those with full masks.
Facemasks with oxygen reservoir bags provide higher concentrations (60% to 80%) than simple facemasks, but the reservoir must be inflated before placing the mask on the patient.1 During inspiration, oxygen is drawn from the attached reservoir, and during expiration a one-way valve closes while the bag refills and expired gas exits through exhalation ports on the sides of the mask. This design is described as ‘‘partial rebreathing’’ because room air and expired gas can be inspired back through these same exhalation ports. This ‘‘partial rebreathing’’ provides the basis for additional designs described as non-rebreathing masks that have thin flaps on the mask’s exhalation ports that act as one-way valves directing oxygen from the reservoir bag to the patient during inspiration. They open during expiration and close during inspiration, preventing reentry of room air or expired gas (see mask with reservoir bag in Figure 2). These variations in design have little significance during short-term supplementation when managing medical complications. Any mask design is acceptable. However, two rules should always be followed: (a) oxygen flow should be established to the mask before placing it on the patient; and (b) if a reservoir bag is present it should be filled prior to placement.
Dated concerns regarding oxygen supplementation depressing hypoxemic drive in patients with chronic obstructive pulmonary disease (COPD) are not valid during emergency interventions.
Supplemental oxygen should be supplied to keep arterial saturations >90%. Hypoxemic respiratory drive plays a small role in patients with COPD. Studies have demonstrated that in patients with both acute and chronic hypercarbia, the administration of supplemental oxygen does not reduce minute ventilation.2
DEVICES FOR POSITIVE PRESSURE: SUPPLEMENTAL AND CONTROLLED VENTILATION
Every dental office must have the ability to deliver oxygen with positive pressure. This may be accomplished with either oxygen-powered resuscitators (eg, Robertshaw or Elder Demand Valves) or with resuscitation bag-valve-mask (BVM) devices. For reasons that will be addressed below, a BVM device is preferred over oxygen-powered resuscitators.
During positive pressure ventilation, there is always a significant risk for gastric distention and subsequent regurgitation or vomiting. This is due to the fact that when oxygen is introduced into the pharynx via positive pressure, it has equal access to the esophagus as well as the trachea. Gas entry into the trachea is favored when the head is properly positioned and ventilatory efforts are gentle and not forced. The usefulness and safety of cricoid pressure (Sellick maneuver) to avoid gastric distension is no longer recommended during positive pressure ventilation nor as a routine maneuver during tracheal intubation.3-5 If ventilation proves difficult using a BVM device and chest rise cannot be ascertained, the introduction of basic airway adjuncts are indicated.
The goal of positive pressure ventilation is to ensure that an adequate volume of oxygen reaches the lungs. If inspiratory pressure exceeds 20 cm of water pressure, the epiglottis may be forced down occluding the glottis, resulting in some or all of the delivered volume pressurizing the stomach. Pressurizing the gastric contents during resuscitative efforts frequently results in emesis and aspiration. Obesity, bronchospasm/asthma, and emphysema may require ventilation pressures exceeding 20 cm. To understand the pressures required for adequate ventilation, the use of bag-valve-mask devices with built-in pressure manometers may be of value. If increasing airway pressures indicate that the volume delivered may be going to the stomach after head tilt, chin lift, and jaw extension have been optimized, changes in respiratory efforts such as increasing inspiratory time, thus decreasing respiratory rate, may be useful. This maneuver may provide adequate oxygenation but not ventilation. Ventilation pressures over 40 cm also indicate the potential for barotrauma to the lungs. Ventilation is always confirmed during bag-valve-mask positive pressure ventilation by observing condensation in the facemask, chest rise, and the presence of breath sounds by auscultation and, if available, by the presence of end-tidal carbon dioxide on exhalation. Oxygenation is confirmed by oximetry.
Although oxygen-powered resuscitators appear simple to use, their delivered inspiratory pressures cannot be modified easily, and the loss of the feel of chest compliance may easily lead to gastric insufflation and also produce lung barotrauma. Bag-valve-mask devices are the preferred equipment to deliver positive pressure ventilation to the apneic patient. A typical BVM device is illustrated in Figure 3. With oxygen flow at 15 L/min, a BVM with reservoir will provide 90% to 95% inspired oxygen concentrations. Proper use requires training and skill on the part of the operator, including proper head position, effective mask seal, respiratory pressures, and rate. Training in BVM ventilation should include both 1-person and 2-person exercises, and this training should be continually refreshed.
BASIC AIRWAY ADJUNCTS
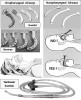
Oropharyngeal airways are adjuncts that improve airway patency by keeping the mouth open and overcome soft tissue obstruction caused by the base of the tongue sagging against the posterior pharyngeal wall. They are inserted in unconscious, nonresponsive patients who cannot be ventilated adequately using simple head-tilt and chin-lift alone (Figure 4). The Guedel airway is hollow and facilitates insertion of a flexible suction catheter to clear the pharynx of secretions. The Berman style lacks this side channel. Both styles are available in various sizes ranging from 0 to 5 based on their length. Selection of proper size can be accomplished by choosing one that extends from the corner of the mouth to the angle of the mandible. Oropharyngeal airways must be inserted cautiously in order to avoid pushing the tongue caudally and worsening the obstruction. This is accomplished either by depressing the tongue with a tongue blade or inserting the airway upside down until reaching the soft palate and twisting it into proper position.
Nasopharyngeal airways are softened tubes available in various sizes based on their diameter. They are inserted through a nostril and maintain patency between the tongue and posterior pharyngeal wall. In contrast to oral airways, consciously sedated patients as well as unconscious patients may tolerate nasopharyngeal airways. However, improper insertion can produce significant trauma. They must be thoroughly lubricated and inserted carefully in a downward direction parallel to the hard palate. Nasopharyngeal airways should not be used without proper training and are contraindicated for patients who are anticoagulated, have bleeding diatheses, or have nasal deformities or a history of nosebleeds. They are most useful for maintaining airway patency during deep sedation or general anesthesia.
During any airway emergency, a Yankauer suction device (‘‘tonsil suction’’) should be available to clear the posterior pharynx of secretions and debris. The Yankauer suction handle and tubing typically requires an adapter to fit the high-speed suction system found on dental units. Saliva ejectors and typical high-speed suction devices are inadequate for this purpose.
If during an emergency, the patient is breathing spontaneously, the application of supplemental oxygen via nasal cannula, nasal hood, or facemask will increase the inspired oxygen concentration. The immediate diagnosis of hypoventilation, soft-tissue obstruction, and apnea is critical in any emergency situation. Basic airway rescue algorithms all follow a step-wise approach beginning with attempts at opening the airway via head tilt, chin lift, and jaw extension, proceeding to positive pressure ventilation with a bag-valve-mask system and, if needed, the insertion of an oropharyngeal or nasopharyngeal airway. Advanced airway rescue by trained dentists may involve the use of supraglottic airways and tracheal intubation. Equipment and skills required for basic airway management are discussed in Basic Life Support for Health Care Providers and advanced airway management in Advanced Cardiac Life Support training courses, but actual ‘‘hands on’’ tasks and team training vary. Continuing education and continuing refresher courses incorporating simulation scenarios, such as those sponsored by the American Dental Society of Anesthesiology, are integral to maintain proficiency and ensure correct resuscitative actions by the dental team in emergency management.
REFERENCES
1. Cairo JM. Mosby’s Respiratory Care Equipment. 9th ed. St Louis, MO: Elsevier Mosby Inc; 2014:67, 83-88, 150-154.
2. Reilly JJ, Silverman EK, Shapiro SD. Chronic obstructive pulmonary disease. In: Longo DL, Fauci AS, Kasper DL, et al, eds. Harrison’s Principles of Internal Medicine. 18th ed. New York, NY: McGraw Hill; 2012.
3. Ellis DY, Harris T, Zideman, D. Cricoid pressure in emergency department rapid sequence tracheal intubations: a risk-benefit analysis. Ann Emerg Med. 2007;50:653-665.
4. Harris T, Ellis DY, Foster L, Lockey D. Cricoid pressure and laryngeal manipulation in 402 pre-hospital emergency anaesthetics: essential safety measure or a hindrance to rapid safe intubation? Resuscitation. 2010;81:810-816.
5. Neumar TW, Otto CW, Link MS, et al. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. 2010;122:S729-S767.
About the Authors
Daniel E. Becker, DDS
Associate Director of Education
General Dental Practice Residency
Miami Valley Hospital
Dayton, Ohio
Morton B. Rosenberg, DMD
Professor of Oral Maxillofacial Surgery
Head, Division of Anesthesia and Pain Control
Associate Professor of Anesthesia
Tufts University Schools of Dental Medicine and Medicine
Boston, Massachusetts
James C. Phero, DMD
Professor Emeritus Anesthesiology
College of Medicine
University of Cincinnati Medical Center
Cincinnati, Ohio