You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
A thorough assessment of a patient’s medical status is a standard of care when any medication is administered during the course of dental care. While this is true for procedures performed under local anesthesia alone, the information gathered may be even more vital for proper patient management if the dentist is planning sedation or general anesthesia for dental treatment. In addition to any past and current medical conditions of the patient, the medical history must include all current medications and baseline vital signs, including hemoglobin saturation by pulse oximetry (SpO2). Principles of preoperative assessment have been reviewed in previous articles.1,2
Airway management is the most important aspect of patient care and examination of the patient’s airway is an essential component of the preoperative assessment. Documentation of a Mallampati airway classification, or more specifically the Samsoon and Young modification of the original classification, has become a standard of care when providing any level of sedation or general anesthesia3,4 (Figure 1). Patients having Class III and IV airways are more likely to obstruct and are more difficult to ventilate or intubate if this becomes necessary. Unless one has training in advanced airway management, deeper levels of sedation should be avoided, especially in these patients. Additional factors that warn of difficult mask seal and ventilation include patients who are fully bearded, edentulous, have a short thyromental distance, and those who have a large neck circumference. When planning deep sedation or general anesthesia, lung sounds should be auscultated to confirm no evidence of lower airway compromise is present.
Primary Assessment and Oxygenation
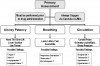
The management of any medical urgency or emergency should commence with a primary assessment, predicated on the emphasis of the airway, breathing, and circulation (ABCs) taught during all courses in basic and advanced life support. Although recent recommendations for the lay public emphasize a C-A-B approach to cardiopulmonary resuscitation, this modification does not apply to healthcare providers.5 While it is common and appropriate for the office team to assess these parameters simultaneously, airway patency must be given initial priority. There is little purpose for assessing ventilation first if any degree of obstruction is present. The head should be tilted back while the chin is lifted, and the mouth and throat examined for any foreign material. In the unconscious patient, it may be necessary to also thrust the jaw forward into a protrusive position in addition to the head-tilt, chin-lift procedure. Together these interventions are described as the ‘‘triple airway maneuver.’’ Once the airway is in an optimal position for maximizing its patency, attention is directed to assessing for breathing or ventilation. We must reiterate that any decision regarding breathing status cannot be made unless a triple airway maneuver has been accomplished, including the jaw protruded.
Ask a conscious patient to take a slow, deep breath. If the patient is unconscious, you should ‘‘look, listen, and feel’’ for ventilatory effort and airflow. A useful caveat is to place one hand on the diaphragm because during quiet breathing the chest does not always rise noticeably, and use the other hand to feel for air movement while the other rescuer performs the triple airway maneuver. If breathing is still in question, use a stethoscope to auscultate the apices of both lungs for breath sounds. The carotid pulse can be palpated either during or following this assessment. Unless significant hypotension exists, the pulse oximeter is generally reliable in confirming that a pulse is present and that the circulation is at least marginal, if not adequate. While airway patency and breathing are being assessed by the doctor and principal auxiliary, other portions of primary assessment should be performed by additional team members. One should record the pulse rate and SpO2 by pulse oximeter, which confirms the presence of a radial pulse; the blood pressure should also be recorded at frequent intervals. One of the team members should be providing supplemental oxygenation or confirming an adequate flow rate if oxygen is already provided. An enriched oxygen concentration is indicated for patients who are spontaneously breathing, regardless of their level of consciousness during medical urgencies and emergencies. This will improve oxygen content within the patient’s functional residual capacity and delay hypoxemia should apnea or obstruction develop. A summary of all components of a primary assessment are illustrated in Figure 2.
Devices for Supplemental Oxygenation
The equipment required to provide supplemental oxygen includes a 100% oxygen source, a regulator, tubing, and either a nasal cannula or mask. Every office should be equipped with a portable E-cylinder of oxygen, regardless of whether treatment rooms are plumbed from a central oxygen source, because emergencies can occur anywhere in the office. E-cylinders provide the most appropriate balance of having sufficient oxygen for an emergency, yet being small enough to be portable. A full tank holds over 600 L and will show a pressure of approximately 2,000 psi. They should be replaced when their content falls to 500 psi. Estimates of time remaining in oxygen cylinders can be approximated by using the following formula where F = 0.3 for E-cylinders and 3.0 for large H-cylinders that supply central plumbing: (psi x F) ÷ (L/min of flow) = time remaining in minutes. For example, if a flow of 10 L/min were administered from an E-cylinder containing 500 psi, the time remaining would be only 15 minutes.
The nasal cannula is ideal for administering supplemental oxygen to conscious patients who may be frightened by a mask. Each liter per minute of oxygen provided via cannula increases the percent oxygen inspired (FiO2) by approximately 4% above room air (FiO2 = 20 + [4 x L/min]).6 This formula approximates oxygen concentration delivered by nasal cannula only. It is not applicable to full or nasal masks. Flow rates greater than 4 L/min may become uncomfortable over time, but delivering 36% oxygen should be adequate supplementation for most situations in which the patient is breathing.
The non-rebreather mask with a reservoir or a nasal hood is appropriate to deliver higher oxygen concentrations to unconscious, breathing patients. When using any mask, the flow rate should be at least 6 L/min to avoid feelings of suffocation. Provided the non-rebreather mask has a reservoir, this flow rate will deliver an oxygen concentration of approximately 60%, and each additional L/min will increase FiO2 by approximately 5%. As stated by Cairo and Pilbean,7 ‘‘Non-rebreathing masks can theoretically deliver 100% oxygen, assuming that the mask fits snugly on the patient’s face and the only source of gas being inhaled by the patient is derived from the oxygen flowing into the mask-reservoir system. In actual practice, disposable rebreathing masks can deliver FiO2 of 0.6 to 0.8.’’ There are no data on precise FiO2 for nasal hoods, but one can presume they would be intermediate between those for nasal cannulas and non-rebreather masks. Previous concern regarding oxygen supplementation depressing hypoxemic drive in patients with chronic obstructive pulmonary disease (COPD) is no longer considered valid. Current thinking is to provide whatever concentration is required to maintain oxygen saturation by pulse oximeter above 90%.8 Generally, this can be accomplished with the nasal cannula or nasal hood at flow rates described above.
Devices for Positive Pressure Ventilation and Airway Adjuncts
The unconscious patient who is apneic will require positive pressure ventilation. Bag-valve-mask (BVM) devices with reservoirs or full-face anesthesia masks can provide 90% to 95% oxygen concentrations, but their proper use requires considerable skill on the part of the operator. Proper head position, effective mask seal, and bag compression are skills that must be developed if they are to be used effectively. Training in BVM ventilation is offered on manikins during healthcare provider basic life-support courses. If ventilation remains difficult, airway adjuncts are indicated.
Oropharyngeal airways are adjuncts that improve airway patency by keeping the teeth and lips apart and preventing the base of the tongue from sagging against the posterior pharyngeal wall. The Guedel airway is hollow and facilitates insertion of a suction catheter to clear the pharynx of secretions. The Berman style lacks a lumen for this purpose. Both styles are available in various sizes ranging from 0 to 5 based on their length. Selection of proper size can be accomplished by choosing one that extends from the anterior lips to the angle of the mandible. Oropharyngeal airways must be inserted cautiously in order to avoid pushing the tongue caudally and worsening the obstruction. This is accomplished either by depressing the tongue with a tongue blade or inserting the airway upside down until reaching the soft palate and twisting it into proper position. Oropharyngeal airways are not tolerated by the conscious patient.
Nasopharyngeal airways are softened tubes available in various sizes based on their diameter. They are inserted through a nostril and maintain patency between the tongue and posterior pharyngeal wall. Unlike oral airways described above, nasal airways are tolerated by both sedated patients who remain conscious as well as unconscious patients. However, improper insertion can produce significant trauma. They must be thoroughly lubricated and inserted carefully in a downward direction parallel to the hard palate. They should not be used without proper training and are contraindicated for anticoagulated patients or those with nasal deformities or history of nose bleeds. Figure 3 illustrates positioning of oropharyngeal versus nasopharyngeal airways.
Tracheal intubation is the ‘‘gold standard’’ for securing airway patency. However, its use is limited to those having advanced anesthesia training such as oral and maxillofacial surgeons and dentist anesthesiologists. If intubation is unsuccessful, or the provider is not trained in this procedure, supraglottic airways have gained status as the ‘‘second-best’’ airway adjunct because they are generally effective and technically less difficult to insert. However, training in the insertion of these devices on simulation manikins or live patients is still necessary to be able to accomplish it successfully in an actual emergency.
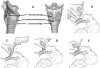
Supraglottic airways (SGA) are devices that fit over the top of the larynx. Several of these devices have been introduced, but the most familiar of these is the laryngeal mask airway (LMA). The apex of the partially inflated mask is inserted into the mouth and pressed against the hard palate; it is advanced toward the uvula and continued through the natural bend of the oropharynx until resistance is felt where it comes to rest over the pyriform fossa at the glottis. At this point the cuff around the mask is fully inflated with enough air to create a relatively airtight seal. The mask from a BVM or anesthesia circuit is removed, and the bag or anesthesia tubing is directly attached to the standard 15-mm connector of the device. Ventilation is confirmed by auscultation of breath sounds in the axillae and/or lung apices subsequent to squeezing the bag. Figure 4 illustrates insertion of an LMA supraglottic airway and summarizes various sizes and volumes for cuff inflation.
While most available SGA devices require inflation of a cuff surrounding the laryngeal mask, a relatively new device, i-gel, does not require cuff inflation. This particular SGA is a single-use device that has a bite block, a gastric tube channel, and a soft, non-inflatable cuff that adapts to the hypopharyngeal anatomy after blind placement (Figure 5). The i-gel SGA has been found to be safe and effective during positive pressure ventilation in adults and in non-obese children.9,10 However, it may not provide as tight a seal as those having inflatable cuffs. One study looking at 280 uses of the i-gel yielded 3 cases of regurgitation, with one resulting in nonfatal aspiration.11
When attempting to ventilate a patient, there is significant risk for gastric distention and subsequent vomiting. This is because the gas introduced into the pharynx has equal access to the esophagus and trachea. Gas entry to the trachea is favored when the head is properly extended and bag compressions are gentle, not forceful. The usefulness and safety of cricoid pressure (Sellick maneuver) has been impressively challenged and can no longer be recommended, even as a routine to facilitate tracheal intubation.12,13 When managing the apneic patient, a reasonable stepped approach is to attempt ventilation with a BVM or anesthesia mask alone, followed, if necessary, by insertion of an oropharyngeal or nasal airway. If this proves futile, one must consider advanced airway adjuncts such as tracheal intubation or insertion of a supraglottic airway, eg, LMA. The moderate sedation provider should be skilled in the proper use of a BVM, nasal and oral airways, and the supraglottic airway. Furthermore, emergency preparedness should also include staff training to allow for assistance with these devices and two-person BVM ventilation. Skills required for advanced airway management were formerly emphasized in all advanced cardiac life-support training, but today this occurs sporadically at best. However, this training is provided in human simulation courses sponsored by the American Dental Society of Anesthesiology. The suggested minimum devices for supplemental and positive pressure oxygenation are illustrated in Figure 6. Practitioners with advanced anesthesia training should also be fully equipped with armamentarium for tracheal intubation, including laryngoscope with three blade sizes, appropriate sizes of endotracheal tubes, stylet, and Magill forceps.
Management of Respiratory Depression
In general, the use of sedation has a positive influence on patients undergoing dental procedures. By reducing fear and anxiety, there is less stress on the cardiovascular system, and vasovagal reactions are less likely to occur. When compared with local anesthesia alone, the two most significant negative variables introduced by any level of sedation or general anesthesia are the added risks for either respiratory depression (ie, hypoventilation) or airway obstruction. Respiratory depression may present as a decrease in depth and/or rate of ventilation and is attributed to depression of respiratory control centers that normally trigger breathing as carbon dioxide levels in the blood rise slightly above the normal threshold. All sedatives, opioids, and potent inhalation general anesthesia agents have the potential to depress central hypercapnic and/or peripheral hypoxemic drives. While this risk is minimal with moderate sedation, some degree of depression is likely during deep sedation and general anesthesia. Regardless of the level of sedation intended, one must be thoroughly skilled in managing respiratory depression in the event it should occur.
Like any complication, management of respiratory depression should commence with standard airway support as noted above. Appropriate airway support and ventilation of unconscious patients are generally routine practice for the dentist or oral and maxillofacial surgeon having advanced anesthesia training. However, pharmacologic reversal of sedative medications is indicated whenever a dentist with training to a level of minimal or moderate sedation is faced with an unconscious patient. The unconscious patient is far more likely to experience apnea and airway complications such as laryngospasm, anatomical obstruction, and aspiration. Pharmacologic reversal should be at least considered when unintentional apnea occurs during treatment by those with advanced training, particularly if ventilation becomes difficult. Among the drug classes used for sedation and anesthesia, opioids are the most powerful respiratory depressants. If an opioid has been included in the regimen, naloxone (Narcan) should be the first reversal drug administered. Depending on the perceived urgency of the situation, it can be titrated intravenously in 0.1-mg to 0.4-mg increments every 3 to 5 minutes or 0.4 mg injected sublingually or intramuscularly every 5 minutes. Careful titration in no more than 0.1-mg increments is advised for any patient susceptible to cardiac irritability or hypertension, as it has been known to trigger ventricular dysrhythmias and acute pulmonary edema. Opioids normally suppress sympathetic tone, and their sudden reversal may result in heightened sympathetic activity. In addition to caution in this group of patients, naloxone should not be administered to a patient having a current history of opioid dependence, unless the event is life-threatening and other interventions have been futile. Generally, the maximum recommended dose is 0.8 mg, followed by a search for other causes if the response is inadequate.
Although less likely to cause respiratory depression when used alone compared to narcotics, benzodiazepines can be reversed using the specific antagonist, flumazenil (Romazicon). Depending on the perceived urgency of the situation, it can be titrated intravenously in 0.1-mg to 0.2-mg increments every 1 to 3 minutes up to 1 mg total, with most patients, according to the FDA-approved package insert, responding to doses of 0.6 mg to 0.8 mg. Although minimal research is available on the speed and efficacy of intramuscular or sublingual injections of flumazenil in patients overdosed on benzodiazepines, it may be injected via those routes if intravenous access is not readily available.14 In general, a noncaustic drug that is approved for intravenous administration should be able to be administered submucosally provided one uses the same concentration and the volume is not too large. Scientific confirmation of this general principle is not cost-effective for drug manufacturers to investigate for every drug but, based on the extensive vascularity of the tongue and floor of the mouth, the onset of a sublingual or intralingual injection should empirically be intermediate between that following intravenous and intramuscular injections. Flumazenil should not be administered to patients having a history of dependence on benzodiazepines or a seizure disorder managed by a benzodiazepine. A summary of the appropriate airway management for the unconscious patient is summarized as an algorithm in Figure 7.
Management of Pathological Airway Obstruction
Airway obstruction must be distinguished from respiratory depression. In other words, we need to tell the difference between the ‘‘cannot breathe’’ and ‘‘will not breathe’’ situation. Although obstruction may result in hypoventilation, the patient’s actual drive to ventilate (breathe) may or may not be obtunded. Upper airway obstruction may be attributed to anatomical structures or foreign material, both of which are addressed during the initial ‘‘airway patency’’ portion of the primary assessment (Figure 7). When these procedures fail to establish patency, pathological causes of obstruction must be considered, namely laryngospasm or laryngeal edema. These events can be distinguished visually by those trained in direct laryngoscopy, but otherwise the distinction is made empirically as will be explained below.
Laryngospasm is a reflex closure or spasm of the glottic muscles including the false and true vocal cords. The conscious or moderately sedated patient is unlikely to experience laryngospasm, but if it occurs, it is very transient and followed by a cough to clear the foreign material or secretions that irritated the larynx. Laryngospasm is far more likely during deep sedation or light planes of general anesthesia, and the obtunded patient may not be able to clear the irritating material. In these cases the laryngospasm produces a complete obstruction and can be dangerously prolonged. It occurs more frequently in children and in adults who are smokers. The patient is generally unconscious and their head, neck, and upper torso exhibit a ‘‘bucking’’ or ‘‘rocking’’ movement as they attempt to ventilate against the obstruction. Rather than the upper abdomen and the chest rising simultaneously during attempts to breathe, these movements will alternate. In most cases, the spasm will relax following a mild, sustained pressure using a BVM or anesthesia mask, but hypoxemia may result if the spasm does not resolve quickly, particularly if supplemental oxygen was not provided prior to the spasm. The airway should be suctioned followed by a forceful jaw thrust to open the upper airway, and a BVM or anesthesia mask should then be placed with enough force to establish a tight mask seal. Gently apply continuous pressure from the bag until ventilations are successful; muscles will generally relax as their oxygen supply declines. For dentists trained only in moderate sedation, sedative medications should be immediately reversed, and as the patient regains consciousness the laryngospasm should resolve following vigorous coughing. For practitioners with advanced anesthesia training, a neuromuscular blocker such as succinylcholine can be administered in the event cords fail to relax and severe hypoxemia develops. Generally, a very small subparalyzing intravenous dose (0.1 mg/kg to 0.2 mg/kg) is all that is required and should only supplement the continued application of positive pressure using a BVM or anesthesia mask. Succinylcholine should be administered only by those with training in deep sedation and general anesthesia. It should be avoided in patients susceptible to hyperkalemia, such as those with muscular dystrophy or other myopathies. A full intubating dose of succinylcholine (1 mg/kg to 2 mg/kg) should be considered if tracheal intubation is anticipated.
Laryngeal edema is among the constellation of events associated with major allergic (anaphylactoid) reactions. The swelling of laryngeal mucosa, as well as neighboring pharyngeal mucosa and tongue, may accompany anaphylactoid reactions and will generally present as stridor or high-pitched crowing sounds during ventilation. The conscious patient will grasp their throat and complain of throat tightness or tongue swelling. Management will require administration of epinephrine which ‘‘decongests’’ the mucosa via vasoconstriction.15,16 It may be administered by several routes and doses listed among the other emergency drugs summarized in Table 1. The most conventional dose is 0.3 mg intramuscularly but, in severe cases, 0.5 mg may be indicated. Intravenous titration of 0.1-mg increments is reserved for only the most severe or refractory episodes.
Bronchospasm is a lower airway obstruction due to contraction or spasm of bronchial smooth muscle. It may be a consequence of a hyperreactive airway typical in asthmatic patients or the result of an anaphylactoid reaction, independent of or in combination with laryngeal edema. Regardless of the cause for bronchospasm, the patient will exhibit dyspnea and wheezing attributed to obstruction in the chest, not the throat or mouth. Bronchial smooth muscle is under autonomic nervous control and requires beta-2 sympathomimetics for relaxation. Following primary assessment, including oxygen supplementation, a selective beta-2 agonist such as albuterol should be administered by metered inhaler. This is preferred over epinephrine because it is less likely to produce positive cardiotonic side effects attributed to stimulation of cardiac beta-1 receptors. It should be mentioned that patients must cooperate if inhalants are to be administered effectively.
Spacer chambers can be attached to inhalers and minimize the need for a coordinated effort on the part of the patient. However, if a patient becomes hysterical, or for other reasons cannot be administered an inhalant, parenteral epinephrine can be administered in dosages identical to those for anaphylactoid reactions. A complete summary of medications addressed in this article is provided in Table 1.
Additional agents mentioned frequently in dental literature for managing asthma, allergic, or anaphylactoid reactions include aminophylline and corticosteroids. These are not recommended for initial acute treatment because of limited efficacy, significant toxicity (aminophylline), or delayed onset, eg, several hours for corticosteroids. Minor allergic reactions manifest cutaneously as pruritus or rash and are not life-threatening. Unlike anaphylactoid reactions, which are mediated by powerful autacoids such as leukotrienes, minor reactions are attributed to histamine release and can be managed with an antihistamine such as diphenhydramine (Benadryl).
Management of Vomiting and Aspiration
Nausea and vomiting are distinct entities and they may occur at any point during or following a clinical procedure. Vomiting or emesis is the actual oral expulsion of gastrointestinal contents and is the result of contractions of gut and thoraco-abdominal wall musculature. This is in contrast to regurgitation, which is the effortless passage of gastric contents into the mouth. Retching is the term used to describe the muscular events of vomiting without the actual expulsion of vomitus, ie, dry heaves. The term nausea refers to a subjective feeling of the need to vomit. The nauseated patient does not necessarily vomit or retch.
If a patient experiences nausea, vomiting, or regurgitation, proper management can minimize any significant consequences. The nauseated patient may be more comfortable in a Fowler’s or semi-Fowler’s position, but if vomiting or regurgitation occurs, or appears imminent, the patient should be placed in a reclined position with the head lower than the chest and abdomen; a partial or full Trendelenburg position is preferred. This will reduce the risk for aspiration (Figure 8). Also, the patient should be turned on their right side based on anatomical considerations. The right primary bronchus branches at a less acute angle from the trachea, and aspirated material is more likely to enter the right lung, at least initially. Turning the patient to the right side may spare the left lung from aspirant. While positioning the patient, initiate high-volume suctioning using a tonsil or Yankauer tip. Avoid placing the suction tip too deeply into the oropharynx to avoid triggering more retching and pushing vomitus further into the airway.
When vomiting ceases, it is essential to evaluate the patient for possible aspiration. The patient should be supported with supplemental oxygen and both lungs auscultated. If there is any evidence of abnormal sounds such as wheezing or rhonchi, or if oxygen saturation determined by pulse oximetry is decreased despite oxygen supplementation, the patient should be immediately transferred to an emergency department for further evaluation. If bronchospasm is suspected, management should follow that for an asthmatic attack; a bronchodilator should be administered, eg, albuterol 2 to 4 inhalations. If the patient cannot cooperate with this form of drug administration, epinephrine 0.3 mg (a 1:1,000 concentration) should be administered intramuscularly. Intubation of the patient should be considered only when hypoxemia remains severe, eg, SpO2 <80%, despite conventional efforts at oxygenation.
Other treatment options such as bronchial lavage or administration of antibiotics and glucocorticosteroids are controversial and rarely, if ever, viable.17,18 These may be indicated in the most severe cases, but they will be addressed more appropriately by the emergency room physician.
Invasive Emergency Airways
Although rarely, if ever, indicated in routine practice, our review would not be complete without some discussion of invasive emergency airways such as cricothyrotomy. Apnea with upper airway obstruction is a dire life-threatening medical emergency associated with deep sedation and general anesthesia care. An inability to ventilate an apneic patient requires sequential attempts following a proscribed algorithm beginning with basic airway rescue maneuvers and escalating to the use of airway adjuncts such as oral, nasal, and supraglottic airways and either orotracheal or nasotracheal intubation (Figure 7). It is highly unlikely that proper use of these interventions will fail to stabilize the patient. However, should attempts with all these techniques fail to secure the airway and provide adequate oxygenation, an invasive emergency airway may be indicated. According to all airway algorithms, the final option in the ‘‘cannot ventilate, cannot intubate,’’ is the cricothyrotomy. With proper patient selection and risk assessment, adherence to accepted techniques, and monitoring, the need for an invasive emergency airway should be a measure of last resort and rarely done in the ambulatory sedation/anesthesia dental model.
The definitive invasive procedure to create an emergency airway is the surgical tracheotomy, but this is a complex procedure and should not be attempted as an emergency intervention. The invasive emergency procedure of choice is the cricothyrotomy, also referred to variably as cricothyroidotomy or coniotomy. The cricothyrotomy consists of entry into the trachea via the cricothyroid membrane, an area easily identified, free of significant vascular or neural structures and below the level of the larynx inferior to any upper airway obstruction. Oxygen can then be delivered through this opening.
A number of techniques have been advocated for this procedure accompanied by many devices and kits. Some are designed to be accomplished surgically (surgical cricothyrotomy), while others require only needle insertion (needle cricothyrotomy). While the experienced oral and maxillofacial surgeon may be familiar with other forms of emergency airway access, a needle cricothyrotomy is most simplistic and can be life-saving.
Needle Cricothyrotomy
It is important to appreciate that needle cricothyrotomy will not provide a large enough entry to enable adequate ventilation of an apneic patient. However, it can provide access adequate to oxygenate most patients. While employing this technique, arterial carbon dioxide tension (PaCO2) will elevate and some degree of respiratory acidosis will develop.19,20 However, the goal of this technique is to oxygenate the patient and prevent significant hypoxemia when advanced airway adjuncts have proven unsuccessful. It is an emergency bridge until a definitive airway can be placed.
Needle cricothyrotomy begins with identifying the cricothyroid membrane and inserting a 12- to 14-gauge angiocatheter attached to a 3-mL syringe containing 1 mL to 2 mL normal saline. Once the trachea is thought to be entered, aspiration of air into the fluid-containing syringe confirms that the catheter is in the lumen of the trachea. The needle is then withdrawn leaving the catheter in place as a conduit for delivery of oxygen. This procedure is illustrated in Figure 9.
Following needle insertion, techniques vary in terms of the actual oxygen source that is applied to the catheter hub. Yealy et al20 have demonstrated that ventilation can be accomplished only by using a high-flow oxygen source—15 L/min at 50 psi. This procedure is referred to either as translaryngeal jet ventilation or percutaneous transtracheal jet ventilation. However, this particular procedure has two disadvantages. It requires additional equipment that may not be normally available in the office setting. (However, tubing and supplies are available commercially for purchase.) Secondly, a high flow such as this may introduce the possibility of barotrauma if the airway is completely obstructed or nearly so.19-21 In practice, the actual degree of obstruction is generally an unknown.
When equipment for jet ventilation is not available, providing oxygenation using a bag-valve device connected to a 100% oxygen source is appropriate.21 Whereas about 1 L/sec can be delivered through 14-gauge catheters using a high-pressure source, only 150 mL/sec to 200 mL/sec can be delivered using a bag-valve device.20 However, if one considers that a normal tidal volume is 500 mL and contains only 20% oxygen (room air), it is presumable that a fraction of this volume containing 100% oxygen can provide acceptable oxygenation for a short term. A system for attaching the bag-valve device to the catheter hub must be in place. Two options are acceptable, both using adapters that have been removed from endotracheal tubes. The adapters allow attachment of the bag-valve device to the catheter hub and are illustrated in Figure 10.
Alternative Devices
Several devices and kits are available as alternatives to the simple needle cricothyrotomy described above. As an example, a 6 French reinforced ethylene propylene emergency transtracheal airway catheter that is kink resistant is available through Cook Medical. Another example of a cricothyrotomy device is the Quicktrach emergency cricothyrotomy device (VBM Medizintechnik GmbH) that consists of an airway catheter that also has a removable stopper that prevents inserting the device too deeply to avoid perforating the rear tracheal wall.
Gaining in popularity are percutaneous cricothyrotomy kits that rely upon the Seldinger technique to gain access to the trachea via the cricothyroid membrane. This is followed by a dilator that allows for the easy insertion of the emergency airway catheter. The larger diameters of the airway catheters included in most of these kits allow direct connection with a bag-valve ventilating device or to an anesthesia circuit.
In addition to the techniques and devices described thus far, surgical cricothyrotomy also deserves mention. Direct surgical cricothyrotomy is performed by making a horizontal incision through the cricothyroid membrane, stretching the opening using the handle of the scalpel, and inserting an endotracheal tube. It carries a significant risk for scarring and possible tracheal stenosis that limits its use to the most extreme circumstances and when other equipment is unavailable.
REFERENCES
1. Becker DE. Preoperative medical evaluation: part 1: general principles and cardiovascular considerations. Anesth Prog. 2009;56:92-102.
2. Becker DE. Preoperative medical evaluation: part 2: pulmonary, endocrine, renal and miscellaneous considerations. Anesth Prog. 2009;56:135-144.
3. Mallampati SR, Gatt SP, Gugino LD, et al. A clinical sign to predict difficult tracheal intubation: a prospective study. Can Anaesth Soc J. 1985;23:429-434.
4. Samsoon GL, Young JR. Difficult tracheal intubation: a retrospective study. Anaesthesia. 1987;42:487-490.
5. Neumar TW, Otto CW, Link MS, et al. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122:S729-S767.
6. American Thoracic Society, Standards for the diagnosis and care of patients with chronic obstructive pulmonary disease (COPD). Am J Respir Crit Care Med. 1995;152:s77-s120.
7. Cairo JM, Pilbean SP. Mosby’s Respiratory Care Equipment. 7th ed. Philadelphia, PA: Mosby Inc; 2004:62-88.
8. Reilly JJ, Silverman EK, Shapiro SD. Chronic obstructive pulmonary disease. In: Kasper DL, Braunwald E, Fauci AS, et al, eds. Harrison’s Principles of Internal Medicine. 16th ed. NewYork, NY: McGraw Hill, 2005:1547-1554.
9. Richez B, Saltel L, Banchereau F, Torrielli R, Cros AM. A new single use supraglottic airway device with a noninflatable cuff and an esophageal vent: an observational study of the i-gel. Anesth Analg. 2008;106:1137-1139.
10. Beylacq L, Bordes M, Semjen F, Cros AM. The I-gel, a single-use supraglottic airway device with a noninflatable cuff and an esophageal vent: an observational study in children. Acta Anaesthesiol Scand. 2009;53:376-379.
11. Gibbison B, Cook TM, Seller C. Case series: protection from aspiration and failure of protection from aspiration with the i-gel airway. Br J Anaesth. 2008;100:415-417.
12. Ellis DY, Harris T, Zideman D. Cricoid pressure in emergency department rapid sequence tracheal intubations: a risk-benefit analysis. Ann Emerg Med. 2007;50:653-665.
13. Harris T, Ellis DY, Foster L, Lockey D. Cricoid pressure and laryngeal manipulation in 402 pre-hospital emergency anaesthetics: essential safety measure or a hindrance to rapid safe intubation? Resuscitation. 2010;81:810-816.
14. Heniff MS, Moore GP, Trout A, Cordell WH, Nelson DR. Comparison of routes of flumazenil administration to reverse midazolam-induced respiratory depression in a canine model. Acad Emerg Med. 1997;4:1115-1118.
15. Sampson HA, Munoz-Furlong A, Campbell RL, et al. Second symposium on the definition and management of anaphylaxis: summary report—second National Institute of Allergy and Infectious Disease/Food Allergy and Anaphylaxis Network symposium. Ann Emerg Med. 2006;47:373-380.
16. Hazinski MF, Chameides L, Hemphill R, et al. 2005 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2005;112(suppl):IV1-IV196.
17. Marik PE. Aspiration pneumonitis and aspiration pneumonia. N Engl J Med. 2001;344:665-671.
18. Anderson E. Aspiration pneumonia and lung abscess. In: Tintinalli JE, Kelen GD, Stapczynski JS. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 6th ed. Access Emergency Medicine. New York, NY: McGraw Hill Co, 2010.
19. Nagy K. Cricothyrotomy. In: Reichman EF, Simon RR. Emergency Medicine Procedures. NewYork, NY: McGraw-Hill Co, 2004.
20. Yealy DM, Stewart RD, Kaplan RM. Myths and pitfalls in emergency translaryngeal ventilation: correcting misimpressions. Ann Emerg Med. 1988;17:690-692.
21. Cabel KJ. Percutaneous transtracheal jet ventilation. In: Reichman EF, Simon RR, eds. Emergency Medicine Procedures. New York, NY: McGraw-Hill Co, 2004, xx-xx.
About the Authors
Daniel E. Becker, DDS
Associate Director of Education
General Dental Practice Residency
Miami Valley Hospital
Dayton, Ohio
Daniel A. Haas, DDS, PhD, FRCD(C)
Associate Dean, Clinical Sciences
Professor and Head of Dental Anaesthesia
Faculty of Dentistry, University of Toronto
Toronto, Ontario, Canada



![Figure 4. Insertion of supraglottic airways (SGA) and suggested sizes. (A) The tip of the cuff is pressed upward against the hard palate by the index finger, while the middle finger opens the mouth. (Insertion is often facilitated by adding a small volume of air [approximately 5 mL] to the cuff.) (B) The SGA is pressed backward in a smooth movement. Notice that the nondominant hand is used to extend the head. (C) The SGA is advanced until definite resistance is felt. (D) Before the index finger is removed, the nondominant hand presses down on the SGA to prevent dislodgment during removal of the index finger. The cuff is subsequently inflated fully, and outward movement of the tube is often observed during this inflation (courtesy of LMA North America Inc, San Diego, CA).](/media/thumbnail/1925)