You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
After removal of a maxillary or mandibular second molar, whether due to caries or endodontic, periodontal, or traumatic reasons, the need to replace the tooth with a dental implant restoration is a subject of debate. Some investigators suggest it is unnecessary,1-3 while others believe second-molar implantation is important, because it restores diminished masticatory capacity and prevents extrusion that could cause occlusal discrepancies.4-6
To evaluate the impact of losing a second molar and the benefits of replacing it, several factors need to be considered, including chewing efficiency, effects on the remaining dentition, restorative considerations, and personal preferences of the patient. This article addresses available data and examines diverse opinions related to this issue and reviews the pros and cons of replacing an extracted second molar with an implant restoration. In this regard, practical guidelines are suggested to assist decision-making.
Masticatory Efficiency
Occlusal Requirements for Effective Chewing
The presence of all teeth in functional positions without dental or oral pathosis ensures optimal chewing performance. Although, as individuals age, tooth loss increases7-9 and masticatory ability concomitantly diminishes.10-12 Thus, the question arises as to how many teeth are needed to maintain health.13 Gotfredsen and Walls noted that the minimum number of teeth required to masticate well was 20 with nine to 10 of them contacting the opposing dentition.14 Others also indicated that satisfactory chewing was attained when 20 or more teeth were present.15,16 However, these reports did not delineate what percentage of masticatory function persisted after extraction of teeth, nor did they consider that quantification of teeth may overestimate chewing efficiency, because it may not take into account their functional positions.12 Furthermore, the reported minimal threshold of 20 retained teeth may not satisfy the esthetic, functional, or psychological needs of a given patient.
Investigators reported that molars are the most commonly extracted teeth, and this is due to caries or periodontitis.7-9 Removal of a second molar is estimated to cause a 5%17 or 7%18 decrease in chewing efficiency. The question of whether or not replacement of a second molar is needed after it is removed has often been debated. Broadbent interpreted the literature to indicate that occlusion to midway of the first molar provides 90% chewing efficiency and that most masticatory function occurs in the premolar-first molar region.19 Misch also noted that 90% of chewing was performed anterior to the second molars.17,20 This idea was supported by others who found that in most subjects the main occluding area in a normal dentition was recorded in the first maxillary and mandibular molar areas.21 Further evidence suggesting that second molars may not substantially contribute to masticatory efficiency can be derived from a denture study that demonstrated no difference in chewing efficacy of dentures with and without second molars.22
From another perspective, orthodontic removal of second molars is sometimes performed to create room for first-molar distalization, and this is considered a viable alternative for correcting an Angle class II malocclusion.23,24 Among patients with such conditions the absence of second molars has not been reported to hinder chewing efficiency. Additional backing for the concept of not having to replace second molars is derived from investigations that found their absence and the absence of first molars, which resulted in a shortened dental arch, did not impede chewing comfort.25,26
Benefits of Replacing Missing Second Molars With Respect to Masticatory Performance
In contrast to the above findings, other investigators found that replacement of second molars provides increased chewing ability and patient satisfaction.27,28 Nam et al evaluated 21 individuals before and 1 month after cementation of implant crowns to replace missing second molars.28 They noted that after restoration of second molars the load-bearing contact area increased from 13.3 mm2 to 15.5 mm2 and maximum occlusal force (Newtons) improved from 405 N to 411 N. Similarly, Kim et al assessed the masticatory function of 20 patients after replacement of second molars with an implant restoration and found increased chewing performance, which was determined by measuring the mean particle size of peanuts after 20 chewing strokes.27 A questionnaire revealed that 90% of patients were satisfied with their chewing improvement. Differences detected between test and control groups in both of these studies were statistically significant.27,28 Still, these findings may not necessarily be clinically relevant, because patients may masticate efficiently without a second molar.17,19,20 On the other hand, final questionnaires in both studies indicated that patient satisfaction improved after crown cementation.27,28
Over-eruption of Unopposed Posterior Teeth
A potential consequence of not replacing an extracted second molar may be migration of the opposing tooth in the vertical and/or horizontal planes (rotation or tipping).29 Terms used synonymously to denote over-eruption include supraeruption, super-eruption, hyper-eruption, and extrusion.30 When super-eruption occurs the periodontium (gingival and osseous level) may maintain its relationship with the extruded tooth and move vertically, or the level of periodontium may not change thereby increasing the tooth's crown-to-root ratio and exposing the tooth's root surfaces.31,32 This latter type of super-eruption is most commonly reported when there is no opposing tooth, whereas the former typically happens when there is attrition of occlusal surfaces and hyper-eruption occurs to sustain occlusal contacts.29 The precise mechanism that causes tooth extrusion is unclear.15,29,33 However, Ten Cate provided strong evidence that tooth eruption is due to modeling of the periodontal ligament, and fibroblasts drive the movement.34 Nevertheless, the causation of eruption is thought to be multifactorial.33,35
Numerous studies have addressed the prevalence and degree of posterior tooth extrusion when there is no opposing tooth (Table 1).29,30,35-39 The data varied among investigations, because different age groups were assessed for varied time periods and diverse methodologies were employed to evaluate hyper-eruption. For instance, Kiliaridis et almeasured super-eruption using straight lines drawn from cusp tip to cusp tip to determine when teeth hyper-erupted.36 Others took into account the curve of the dental arch29,38; it was suggested that drawing a straight line between cusps flattens the natural occlusal curve and may produce a false impression of over-eruption.
Approaches to quantify the amount of over-eruption differ. Some studies provided means with respect to vertical migration of unhampered molars,29,30,37,38 while others supplied partial frequency distributions (Table 1).29,35,36 Some investigators noted the range of super-eruption, which extended from 0 to 5.4 mm29,35-38 (Note: In this discussion, the authors use the terms unopposed, unimpeded,and unhamperedinterchangeably.)
The prevalence of posterior teeth extrusion when there is no opposing tooth was high in all investigations, ranging from 79.3% to 100% of the monitored sites (Table 1).29,30,35-39 Several investigators reported how often more than 2 mm over-eruption of unopposed posterior teeth occurred: 20.7%,30 24%,36 27%,29 and 32%35 (Table 1). Others noted that 99% of unimpeded posterior teeth manifested less than 1 mm of extrusion (mean follow-up 6.9 years).40
No studies discussed the clinical relevance of a specific amount of extrusion as it relates to occlusal interferences. Several investigators interpreted the clinical significance of their findings. For instance, Kiliaridis et al found that 76% of molar teeth did not erupt enough to be of clinical significance (76% of molars extruded less than 2 mm); they interpreted their data to refute the concept that all missing second molars need to be replaced.36 However, they did not explain why a 2 mm change was selected to represent a clinically important finding. In contrast, Craddock et al noted 92% of posterior teeth extruded (mean 1.68 mm) and 27% over-erupted more than 2 mm.29 These researchers thought their data was clinically meaningful and that unopposed posterior teeth should be monitored frequently.
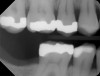
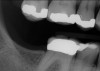
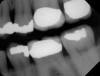
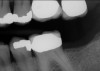
Another consideration is mean vertical displacement of unhampered posterior teeth, which in some studies was minimal: 0.8 mm37 and 0.9 mm30 (Table 1). Yet, there could have been sites where the amount of extrusion was clinically relevant. When Lindskog-Stokland et al assessed the risk of over-eruption using 1 mm as a threshold, they stated there was an odds ratio of 3.3 that unimpeded molars would extrude 1 mm compared to opposed molars.30 Based on their calculations, however, it is unclear which patients with a missing molar are at risk of over-eruption (Figure 1 through Figure 4). Indeed, if susceptible individuals could be identified, then restorative therapy could be initiated to stabilize their occlusion (eg, tooth replacement). Furthermore, odds ratios can be highly misleading, and predictive values would provide clinicians a better perspective as to what percentage of sites may experience significant extrusion.41,42
With respect to periodontally involved teeth (loss of clinical attachment and osseous support), Christou and Kiliaridis described an increased magnitude of super-eruption compared to uncompromised teeth during a 10-year monitoring period (1.94 mm versus 0.8 mm).37 Craddock et al also found that periodontally afflicted teeth extruded more than healthy teeth.29 They suggested that periodontally compromised teeth were a predictor for future extrusion, but no odds ratios or predictive values were calculated. Numerous other researchers also suggested that bone loss associated with periodontal destruction predisposes teeth to over-eruption.30,37,43 This finding is biologically plausible, because a reduced periodontium may not provide the same stability as one that is uncompromised.
Over-eruption was found to be greater in the maxilla than in the mandible.29,30 Craddock et al, for example, reported the following mean amounts of extrusion: maxilla 1.91 mm versus mandible 1.03 mm.29 In contrast, Kiliaridis et al noted that maxillary and mandibular molars super-extruded equivalently.36 Data in the literature is too limited to comment about this finding.
Several studies compared the amount of posterior hyper-eruption that occurred when an opposing molar was and was not present.29,30,37 Investigators consistently reported that molars without an opposing tooth demonstrated more super-eruption than those with an antagonist tooth. Interestingly, even if there was an opposing tooth, a small amount of extrusion occurred. For example, Craddock et al noted the mean over-eruption of unimpeded posterior teeth was 1.68 mm,29 whereas for opposed posterior teeth the amount of super-eruption was 0.24 mm within 5 years. Similarly, Lindskog-Stokland et al found that unhampered molars vertically migrated 0.9 mm compared to 0.04 mm within 12 years if molars were opposed.30 Extrusion was attributed to dental wear, and eruption compensation occurred to maintain occlusal levels. This finding is expected because teeth continuously erupt to compensate for attrition.44
Craddock reported over-eruption of posterior teeth occurred if there was no antagonist tooth despite partial contact with a tooth adjacent to the opposing edentate site.45 He stated that if there was less than 30% overlap with the opposing contiguous tooth, hyper-eruption due to tipping was not reduced or inhibited.
Vertical migration of teeth opposite an unopposed posterior was also associated with horizontal tooth displacement.36,45,46 Kiliaridis et al described the percentage of times unimpeded molars manifest movements as follows: no rotation, 60%; less than 15-degree rotation, 31%; and more than 15-degree rotation, 10%.36 Tipping did not occur for 62% (n = 52) of the unopposed molars.36 Large positional alterations can affect restorative procedures through decreased interocclusal space, altered angulation of abutment teeth, and undesirable embrasure contours.32
Over-eruption has been said to induce occlusal interferences, which can present negative consequences such as fractured cusps, increased tooth mobility, muscle fatigue, tooth wear, temporomandibular joint disorders,47,48 and changes in the occlusal plane.49 Pertinently, several studies assessed the relationship between occlusal interferences and over-eruption of unopposed posterior teeth.35,50,51 These investigations found that the percentage of unhampered posterior teeth that demonstrated retruded or protrusive position contacts or excursive interferences was 51.6%,35 53%,50 and 40%.51 Hakeem et al reported more occlusal interferences among patients with unopposed molars than those that had an antagonist, but the difference was not statistically significant.51 Overall, the strength of the relationship between the occurrence of occlusal interferences and the degree of extrusion was noted as follows: not statistically significant,51 statistically weak,35 and an association.50 Thus, it is questionable to cite concern regarding extrusion of an opposing tooth as a cogent reason for recommending replacement of a second molar.
Other findings reported in the literature concerning over-eruption underscored that age is a factor that can impact the frequency of super-erupting molars. Kiliaridis et al stated that patients who lost molars as adults had a smaller chance of manifesting hyper-eruption compared to individuals who had a molar extracted in their youth.36 With respect to the chronology of molar super-eruption, it was described to occur within a few years after extraction of an antagonist tooth.52 Similarly, it has been observed that most extrusion happens early in the post-extraction period.38,39 Thus, if a patient presents many years after a second molar was removed, the chance that the antagonist tooth will greatly over-erupt is diminished.
Patient Preferences and Restorative Considerations
Treatment planning with respect to replacing a lost tooth should be based on an individual's functional requirements and preferences.14,53 Some patients may want to replace their lost second molar because of a perceived decreased chewing ability or sense of "gaps" in their dentition, or they may be concerned about extrusion of opposing teeth. For these individuals several good therapeutic options are available to manage a missing second molar, including a fixed prosthesis if a suitable third molar is present to function as a terminal abutment, a removable prosthesis, or a dental implant restoration.
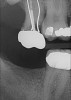
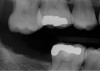
If a patient chooses not to replace a missing second molar but desires to preclude over-eruption of an opposing molar, a preventive restoration may be fabricated. Examples of such a restoration may include bonding to an adjacent tooth, a metal splint bonded to adjacent teeth, a removable prosthesis, an extended prosthetic length of arch with a cantilever, or the use of a nightguard. This could prevent molar hyper-eruption, which may predispose an individual to plaque retention that could cause caries or periodontitis (Figure 5).40 Potential loss of interocclusal space also must be addressed with patients, because extraction of a second molar can result in migration of an unopposed tooth, which may complicate the replacement of the antagonist (Figure 6). Importantly, a super-erupted tooth may need to be significantly reduced before fabricating an opposing implant prosthesis, or an extruded tooth may need to be devitalized, crown-lengthened, or intruded to provide proper interocclusal space for a restoration.
Discussion
Whether or not a removed second molar needs to be replaced with an implant restoration is a controversial subject. Various issues must be critically addressed to facilitate decision-making regarding the prudence of routine replacement of a missing second molar.
The extraction of a second molar reduces masticatory efficiency,17,18 but it is the authors' opinion that most patients are satisfied with their masticatory ability after losing a second molar, since 90% chewing efficiency is provided by first-molar occlusion.17,19,20 Data does not support the concept that the absence of a second molar reduces chewing efficiency to a degree that it impairs food mastication or nutritional intake or interferes with social aspects of eating. This statement is in accord with the reasoning of other clinicians.1,3,40,54
Historically, masticatory ability was assessed subjectively with a questionnaire,55,56 but recently a few objective studies evaluated the capacity of second-molar replacement to enhance chewing ability.27,28 Investigators studied whether or not smaller food particle size could be achieved, the effect on the load-bearing contact area, and the amount of generated occlusal forces.27,28 A statistically significant improvement in masticatory performance was found after implant replacement of a missing second molar.27,28 However, it should be noted that when a test and control group are compared, the finding that there is a statistically significant difference between groups for an assessed factor denotes the event did not occur by chance; it does not indicate that the finding is important or large.57 Accordingly, it is appropriate for clinicians to discuss with patients the practical versus the statistical benefit of replacing a second molar with regard to improved chewing performance.
Occlusal interferences associated with extruded unopposed teeth commonly occur.29,30,35-39 Nonetheless, these data need to be interpreted in light of the fact that in a general population when there are no concerns about over-erupted unopposed teeth, an occlusal contact, usually defined as an interference, can affect up to approximately 89% of individuals at one site.55 Furthermore, it was reported that the association between the amount of extrusion and the presence of an occlusal interference is statistically weak35 or statistically insignificant.51 With respect to the prevalence and degree of extrusion, the authors believe that a significant finding could be defined as an event that dictated the need to change therapy (eg, replace a missing tooth), because it would help avoid adverse consequences (eg, fractured cusps). However, selection of a threshold to initiate therapy based on the prevalence of super-eruption (percentage occurrence) or amount of hyper-eruption may predispose clinicians to initiate unnecessary therapy, because minor extrusions usually do not interfere with function.50,55,58
On the other hand, not all occlusal interferences can be ignored. Clinicians, therefore, need to differentiate between physiologic and pathologic occlusions. Physiologic occlusion is defined as an "occlusion in harmony with the functions of the masticatory system"59 and the patient is asymptomatic. Because occlusion is rarely ideal and many interferences are benign, it has been suggested that decisions with respect to restoring missing teeth should be made based on an individual's needs and not assumptions about potential negative consequences due to extrusion.5 Contrastingly, pathologic occlusion denotes that the masticatory system is unable to provide a functional, healthy, and comfortable equilibrium and the patient is symptomatic. For these individuals appropriate therapy (eg, occlusal equilibration, restorative procedures) should be initiated.
Financial concerns also need to be considered when contemplating replacement of second molars.60 For some individuals, implant placement and restoration are prohibitively expensive and alternate therapies (eg, partial dentures) should be discussed. For others, finances may not be a critical issue.
There also may be anatomical reasons that impede replacing a second molar. For instance, there may be inadequate height or width of bone to accommodate an implant without the use of bone grafting, or the position of the inferior alveolar nerve or maxillary sinus may preclude placing a second-molar implant without performing osseous augmentation. These situations would require further discussion with the patient prior to proceeding with second-molar replacement.
Finally, there is no right or wrong answer as to the sensibility of replacing a missing second molar with an implant restoration. Usually, it is a matter of patient preference. To help clinicians and patients decide on whether or not to restore a missing second molar, suggested guidelines are presented in Table 2.
Conclusion
Based on the information available to them, clinicians and patients can make appropriate decisions regarding the need to replace a missing second molar with an implant restoration. Evidence on both sides of the argument-pros and cons-has been presented, along with guidelines for management of missing second molars. While it is not necessarily wrong to restore a second molar, in the authors' opinion routinely doing so because of concerns related to loss of chewing efficiency or development of occlusal interferences is questionable. Conversely, a patient may desire a second molar, and replacing it does provide some benefits, including avoiding the potential of over-eruption of an unopposed molar. Ultimately, second-molar replacement usually is driven by a patient's preferences and values.
About the Authors
Gary Greenstein, DDS, MS
Clinical Professor, Department of Periodontics, College of Dental Medicine, Columbia University, New York, New York; Private Practice, Periodontics and Surgical Implantology, Freehold, New Jersey
Ben Greenstein, DMD
Private Practice, Periodontics and Surgical Implantology, Freehold, New Jersey
Joseph Carpentieri, DDS
Clinical Assistant Professor, Department of Prosthodontics, College of Dental Medicine, Columbia University; Private Practice, Surgical Implantology and Prosthodontics, White Plains, New York
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Faggion CM Jr, Giannakopoulos NN, Listl S. How strong is the evidence for the need to restore posterior bounded edentulous spaces in adults? Grading the quality of evidence and the strength of recommendations. J Dent. 2011;9(2):108-116.
2. Gragg KL, Shugars DA, Bader JD, et al. Movement of teeth adjacent to posterior bounded edentulous spaces. J Dent Res. 2001;80(11):2021-2024.
3. Misch CE. Single tooth implants: difficult, yet overused. Dent Today. 1992;11(3):46,48-51.
4. Firestone JM. Missing posterior teeth. J Am Dent Assoc. 2001;132(1):14,16,18.
5. Carlsson GE, Kiliaridis S. Tooth movement. Br Dent J. 2005;198(7):420-421.
6. Lyka I, Carlsson GE, Wedel A, Kiliaridis S. Dentists' perception of risks for molars without antagonists. A questionnaire study of dentists in Sweden. Swed Dent J. 2001;25(2):67-73.
7. Battistuzzi P, Käyser A, Peer P. Tooth loss and remaining occlusion in a Dutch population. J Oral Rehabil. 1987;14(6):541-547.
8. Salonen L. Oral health status in an adult Swedish population. A cross-sectional epidemiological study of the northern Älvsborg county. Swed Dent J Suppl. 1990;70:1-49.
9. Walter MH, Wolf BH, Rieger C, Boening KW. Prosthetic treatment need in a representative German sample. J Oral Rehabil. 2001;28(8):708-716.
10. Hsu KJ, Yen YY, Lan SJ, et al. Relationship between remaining teeth and self-rated chewing ability among population aged 45 years or older in Kaohsiung City, Taiwan. Kaohsiung J Med Sci. 2011;27(10):457-465.
11. Bortoluzzi MC, Traebert J, Lasta R, et al. Tooth loss, chewing ability and quality of life. Contemp Clin Dent. 2012;3(4):393-397.
12. Naka O, Anastassiadou V, Pissiotis A. Association between functional tooth units and chewing ability in older adults: a systematic review. Gerodontology. 2014;31(3):166-177.
13. Baba K, Igarashi Y, Nishiyama A, et al. Patterns of missing occlusal units and oral health-related quality of life in SDA patients. J Oral Rehabil. 2008;35(8):621-628.
14. Gotfredsen K, Walls AW. What dentition assures oral function? Clin Oral Implants Res. 2007;18 Suppl 3:34-45.
15. Steedle JR, Proffit WR. The pattern and control of eruptive tooth movements. Am J Orthod. 1985;87(1):56-66.
16. Sheiham A, Steele J. Does the condition of the mouth and teeth affect the ability to eat certain foods, nutrient and dietary intake and nutritional status amongst older people? Public Health Nutr. 2001;4(3):797-803.
17. Misch CE. Single-tooth replacement: treatment options. In: Misch CE. Contemporary Implant Dentistry. 3rd ed. St. Louis, MO: Mosby; 2008:327-366.
18. Missing Few Teeth. Posterior Teeth Replacement (Dental Implants for Back Teeth). Scientific™ Dental Clinic website. http://www.scientificdentalclinic.com/missing-few-teeth. Accessed September 20, 2018.
19. Broadbent JM. Chewing and occlusal function. Funct Orthod. 2000;17(4):34-39.
20. Misch CE. Posterior single tooth replacement. In: Dental Implant Prosthetics. Misch CE, ed. St. Louis, MO: Elsevier Mosby; 2005:350.
21. Kato H, Furuki Y, Hasegawa S. Observation on the main occluding area in mastication. J Jpn Soc Stomatognath Funct. 1996;2:119-127.
22. Iegami CM, Barbosa WF, Furuyama RJ, et al. Masticatory efficiency in complete denture wearers with reduced dental arches-a randomised cross-over study. J Oral Rehabil. 2014;41(8):619-623.
23. Schroeder MA, Schroeder DK, Santos DJS, Leser MM. Molar extractions in orthodontics. Dental Press J Orthod. 2011;16(6):130-157.
24. Lee W, Wong RW, Ikegami T, Hägg U. Maxillary second molar extractions in orthodontic treatment. World J Orthod. 2008;9(1):52-61.
25. Khan SB, Chikte UM, Omar R. An overview of systematic reviews related to aspects of the shortened dental arch and its variants in adults. Int J Prosthodont. 2017;30(4):357-366.
26. Korduner EK, Söderfeldt B, Kronström M, Nilner K. Attitudes toward the shortened dental arch concept among Swedish general dental practitioners. Int J Prosthodont. 2006;19(2):171-176.
27. Kim MS, Lee JK, Chang BS, Um HS. Masticatory function following implants replacing a second molar. J Periodontal Implant Sci. 2011;41(2):79-85.
28. Nam DH, Lee DW, Chung CJ, et al. Change in masticatory ability with the implant restoration of second molars. J Prosthet Dent. 2014;111(4):286-292.
29. Craddock HL, Youngson CC, Manogue M, Blance A. Occlusal changes following posterior tooth loss in adults. Part 1: a study of clinical parameters associated with the extent and type of supraeruption in unopposed posterior teeth. J Prosthodont.2007;16(6):485-494.
30. Lindskog-Stokland B, Hakeberg M, Hansen K. Molar position associated with a missing opposed and/or adjacent tooth: a follow up study in women. Swed Dent J. 2013;37(2):97-104.
31. Shifman A, Laufer BZ, Chweidan H. Posterior bite collapse-revisited. J Oral Rehabil. 1998;25(5):376-385.
32. Craddock HL. Consequences of tooth loss: 2. Dentist considerations-restorative problems and implications. Dent Update. 2010;37(1):28-32.
33. Marks SC Jr, Schroeder HE. Tooth eruption: theories and facts. Anat Rec. 1996;245(2):374-393.
34. Ten Cate AR, Deporter DA, Freeman E. The role of fibroblasts in the remodeling of periodontal ligament during physiologic tooth movement. Am J Orthod. 1976;69(2):155-168.
35. Craddock HL, Youngson CC. A study of incidence of overeruption and occlusal interferences in unopposed posterior teeth. Br Dent J. 2004;196(6):341-348.
36. Kiliaridis S, Lyka I, Friede H, et al. Vertical position, rotation, and tipping of molars without antagonists. Int J Prosthodont. 2000;13(6):480-486.
37. Christou P, Kiliaridis S. Three-dimensional changes in the position of unopposed molars in adults. Eur J Orthod. 2007;29(6):543-549.
38. Hakeem S, Mohsin A, Abdulrazzaq A. Frequency of overeruption in unopposed posterior teeth. Pakistan Oral & Dental Journal. 2012;32(1):159-164.
39. Love WD, Adams RL. Tooth movement into edentulous areas. J Prosthet Dent.1971;25(3):271-278.
40. Shugars DA, Bader JD, Phillips SW Jr, et al. The consequences of not replacing a missing posterior tooth. J Am Dent Assoc. 2000;131(9):1317-1323.
41. Greenstein G, Lamster I. Understanding diagnostic testing for periodontal diseases. J Periodontol. 1995;66(8):659-666.
42. Kramer MS. Clinical Epidemiology and Biostatistics: A Primer for Clinical Investigators and Decision-Makers. Berlin, Hiedelberg, Germany: Springer-Verlag; 1988:64-68.
43. Fujita T, Montet X, Tanne K, Kiliaridis S. Overeruption of periodontally affected unopposed molars in adult rats. J Periodontal Res. 2010;45(2):271-276.
44. Craddock HL, Youngson CC. Eruptive tooth movement-the current state of knowledge. Br Dent J. 2004;197(7):385-391.
45. Craddock HL. An investigation of overeruption of posterior teeth with partial occlusal contact. J Oral Rehabil. 2007;34(4):246-250.
46. Kaplan P. Drifting, tipping, supraeruption, and segmental alveolar bone growth. J Prosthet Dent. 1985;54(2):280-283.
47. McCullock AJ. Making occlusion work: I. Terminology, occlusal assessment and recording. Dent Update. 2003;30(3):150-157.
48. McCullock AJ. Making occlusion work: 2. Practical considerations. Dent Update. 2003;30(4):211-219.
49. Craddock HL, Youngson CC, Manogue M. Deviation from the Broadrick occlusal curve following posterior tooth loss. J Oral Rehabil. 2006;33(6):423-429.
50. Craddock HL. Occlusal changes following posterior tooth loss in adults. Part 3. A study of clinical parameters associated with the presence of occlusal interferences following posterior tooth loss. J Prosthodont. 2008;17(1):25-30.
51. Hakeem S, Ahmed AR, Mohsin A. Association of occlusal interferences with over-erupted posterior teeth. J Pak Dent Assoc. 2013;22(1):19-22.
52. Compagnon D, Woda A. Supraeruption of the unopposed maxillary first molar. J Prosthet Dent. 1991;66(1):29-34.
53. Drummond JR, Newton JP, Yemm R. Dentistry for the elderly: a review and an assessment of the future. J Dent. 1988;16(2):47-54.
54. Levin B. Editorial: "The 28-tooth syndrome"-or should all teeth be replaced. Dent Surv. 1974;50(7):47.
55. Agerberg G, Sandström R. Frequency of occlusal interferences: a clinical study in teenagers and young adults. J Prosthet Dent. 1988;59
(2):212-217.
56. Boretti G, Bickel M, Geering AH. A review of masticatory ability and efficiency. J Prosthet Dent. 1995;74(4):400-403.
57. Greenstein G. Clinical versus statistical significance as they relate to the efficacy of periodontal therapy. J Am Dent Assoc. 2003;134(5):583-591.
58. Clark GT, Tsukiyama Y, Baba K, Watanabe T. Sixty-eight years of experimental occlusal interference studies: what have we learned? J Prosthet Dent. 1999;82(6):704-713.
59. The Glossary of Prosthodontic Terms: Ninth Edition. J Prosthet Dent. 2017;117(5S):e1-e105.
60. Teófilo LT, Leles CR. Patients' self-perceived impacts and prosthodontic needs at the time and after tooth loss. Braz Dent J. 2007;18(2):91-96.