You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The use of dental implants to replace natural teeth is highly predictable. Placement of single implants is one of the most common procedures in dental implant therapy. According to many studies, more than 95% of single dental implants are successful over 30 years, and full-arch prostheses demonstrate a similar success rate over a 10-year period.1 Despite these results, some implantologists might still say that "if a clinician hasn't seen a failure, it simply means that he or she hasn't placed enough implants."
Implants fail for a variety of reasons, and dental practitioners must be prepared for the different scenarios that can prompt implant complications. Being aware of the causes of dental implant failures can help the practitioner to recognize these situations and intervene before an implant actually fails. Being proactive is a key to successful, long-term dental implant therapy.
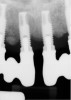
According to the European Association for Osseointegration's third Consensus Conference in 2012, 63% of patients with implants experience peri-implant mucositis, and one in five of these patients will develop peri-implantitis within 5 years of placement.2 Peri-implantitis is an inflammatory condition that develops as a response to bacteria lingering around the neck of the implant. Froum and Rosen defined peri-implantitis as peri-implant disease that has progressed beyond gingivitis or peri-implant mucositis to the point of bone loss.3 This bone loss is best identified on periapical radiographs, where the crestal bone and implant threads are clearly visualized (Figure 1). Oftentimes, computed tomography (CT) scans produce scatter radiation that can interfere with clear identification of bone loss at the neck of the implant.
Causes of implant failure can be categorized as local or systemic. Local factors affecting the health of peri-implant tissues include poor oral hygiene, residual subgingival cement, occlusal overload, quantity/quality of bone, implant location, and potentially, a reaction to a foreign body. Systemic factors include smoking and chronic inflammation, such as that associated with periodontitis, diabetes, and stress.4
Quality of Soft Tissue
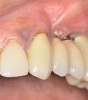
Whether or not to probe around dental implants has been a topic of debate in the dental community for years. Recent consensus supports periodic probing around dental implants so that changes in probing, such as the presence of bleeding on probing, suppuration, and probing depth, can be identified over time.5 If bleeding on probing is present, then the cause(s) of this bleeding should be identified and a proactive treatment approach taken before bone loss begins to occur around the implant. Bleeding may result from poor oral hygiene or a lack of adequate keratinized tissue around the implant (Figure 2). And insufficient keratinized tissue in the presence of poor oral hygiene may lead to an even greater level of peri-implantitis.6 This can result in increases in gingival bleeding, plaque index, pocket depth, and bleeding on probing. Therefore, the presence of adequate thickness and keratinization of soft tissue around dental implants is a necessity.
Dental Biofilm
Research has recognized that there is a difference in biofilm between healthy implant sites and areas affected by peri-implantitis.7 Subgingivally, the biofilm in patients with peri-implantitis has exhibited more bacteria from the orange complex, which are known to cause periodontitis. Some of these pathogens can be identified via salivary diagnostics. Typically, patients with periodontitis are more prone to developing bone loss around dental implants. This may be due to the type of bacteria in the biofilm. The frequency of Porphyromonas gingivalis and Aggregatibacter actinomycetemcomitans, which are classified as aggressive pathogens, was found to be similar between cases of periodontitis and peri-implantitis.8 Various laboratories provide salivary diagnostics, including testing for pathogenic bacteria such as P gingivalis and A actinomycetemcomitans (Figure 3).
Further investigations into the diversity of the peri-implant microbiota will be essential to understand and develop preventive and therapeutic strategies for peri-implantitis. Bacterial biofilm is a key component in many disease processes, and the development of more precise laboratory testing has allowed scientists to better understand its role in bone loss.9
Salivary diagnostics can also determine if a patient is interleukin-1 genotype positive, which indicates that the patient is more prone to bone loss in response to inflammation. If a patient is found to have aggressive periodontal pathogens in the presence of inflammation and peri-implantitis, treatment should be administered as soon as possible with the goal of improving the patient's oral hygiene and disrupting the biofilm.
Iatrogenesis
Surgical skill is a key factor in the success or failure of an implant. Clinicians' understanding of proper technique is instrumental in both surgical implant placement and the restoration of dental implants. It is important that practitioners recognize their limitations. Moreover, they should be prepared to treat potential complications-which means knowing in advance what those potential complications may be-before engaging in any surgical procedure. An analysis of the performance of 21 different oral surgeons and periodontists over a period of 28 years revealed varying failure rates between surgeons.10
The quantity and quality of bone should be assessed via CT scan before surgery. In a recent retrospective study of 1,592 implants, the authors concluded that a history of periodontitis and a two-stage surgical protocol with a bone graft in the lower jaw increased the risk of inflammatory problems during the first 6 months of implant placement.11 Whether or not the patient was a smoker and the clinician's surgical experience were two important factors for early implant failure in this study. In routine practice, peri-implantitis seems to be more often associated with surgical protocols in the posterior mandible.12
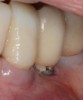
The presence of excess subgingival cement also has been implicated in the development of peri-implantitis (Figure 4).13 To reduce this risk, a crown margin should be cemented at the gingival margin to allow for cement visualization and easy cleanup. In addition, the use of a radiopaque cement is recommended, and an x-ray image should be taken to ensure that no cement is left behind. The use of screw-retained restorations, when possible, is recommended over cement-retained ones to help avoid this problem.
Bruxism
Bruxism is recognized to be the most significant risk factor related to long-term implant failures.14 Although the effects of bruxism on dental implants do not manifest themselves until some time has passed, it is important to identify patients with this condition prior to implant placement. This may be difficult, because most bruxers are not aware of their habit, and many do not have obvious tooth wear. Indications of bruxism include an increase in size of the temporal and masseter muscles, limited occlusal opening, increased tooth mobility, cervical abfraction, and fractured restorations.15 The wear pattern on a nightguard can be examined to diagnose the extent of a patient's nocturnal parafunctional habits.
Bruxism is not a contraindication for implant placement, but it will alter the dental implant treatment plan. For these cases, additional implants and reinforced restorations may be necessary, and narrow-diameter implants should be avoided because they can fracture more readily. During healing time, a partial or full denture can also negatively affect implant stability and integration if excessive force or rocking movements are placed on the implants, even if the implants are submerged. Excessive force is the primary cause of fractures in implants and implant-retained prostheses.16
Prosthetic risk factors that result in mechanical overload are common in implant failure. In a 2009 systematic review by Salvi and Brägger, the absence of a metal framework in overdentures, the presence of cantilever extension(s) greater than 15 mm, and bruxism were associated with an increased incidence of mechanical and technical complications.17
Medical Factors
A thorough evaluation of each patient's medical history prior to implant surgery is critical to achieving a successful result. A correlation exists between certain categories of medications described by the American Society of Anesthesiologists, the number of medications that a patient is taking, and implant failure.15 This is due to the fact that a healthy bone turnover process is a vital requirement for dental implant success. Medications, immune problems, poor diet, and tobacco use can impede this process, which in turn, may generate more implant failures.
The need for implant treatment is greater among older patients, and as people age, the risk of chronic illnesses increases. Studies have shown that approximately 80% of elderly individuals have at least one chronic disease.16 The frequency of diabetes and other immune problems increase with age as well. Diabetes mellitus, the seventh leading cause of death in United States, affects a large percentage of the population.18 Many patients are not aware that they have diabetes; therefore, a physical medical examination should be conducted 6 months before any implant procedure is performed. The correlation between diabetes and periodontitis has been recognized for a long time.19 A significant reduction in bone-to-implant contact and a lack of osseointegration is found in patients with uncontrolled diabetes, and immediately following surgery, these patients possess a much higher risk of infection.20 Conversely, if a patient's diabetes is well-controlled, then it does not significantly affect long-term implant survival.21
Several medications, including aspirin, nonsteroidal anti-inflammatory drugs (NSAIDs), and corticosteroids, can impede short-term healing; however, other medications can affect bone metabolism and long-term healing. For example, bisphosphonates impede the osteoclast function in the bone and prevent the osseointegration of dental implants. This medication is used intravenously for metastatic bone cancer treatment and orally for reversing osteoporosis. When taking a patient's medical history, it is imperative that practitioners specifically ask if he or she has taken or is taking bisphosphonates and in what form. This medication causes pathologic conditions including osteonecrosis of the jaw. In 2002, reports emerged of serious side effects from these medications after dental surgery. Osteonecrosis of the jaw primarily affects patients taking IV-administered bisphosphonates; however, a small percentage of cases involve patients taking oral bisphosphonates, such as Fosamax.22 These medications are absorbed into the bone and can affect bone metabolism for up to 10 years.
One way to assess bone turnover is by checking a patient's C-terminal telopeptide (CTx) levels following a morning fast. These telopeptides are released in the blood as a byproduct of bone remodeling. If the serum CTx level is below 150 pg/ml, dental implant surgery is not recommended. For these cases, the Marx protocol suggests a physician-approved drug holiday for 3 to 9 months,during which time no bisphosphonate is administered, then the patient's CTx level can be retested. When the serum level reaches a value above 150 pg/ml, then implant surgery can be performed.23
Vitamin D
Vitamin D, which has received much attention in the medical field in recent years, is actually a hormone that is involved in many functions of the body, including those involving the skin, liver, kidneys, and bone formation. Patients undergoing dental implant surgery must have an adequate level of vitamin D, which can easily be assessed via a blood spot test. Currently, there is a nationwide epidemic of low levels of vitamin D. Vitamin D deficiency results in an inability to absorb calcium in the bone, and recent studies in animals suggest that there is a decrease in bone-to-implant contact when the vitamin D level is low.24 Because the recommended optimal level of vitamin D changes as new research is conducted, it is important for clinicians to stay abreast of current recommendations. Presently, the recommended vitamin D level is 50 ng/ml to 80 ng/ml.
Tobacco Use
The association between smoking and delayed wound healing has long been recognized in medicine. The three most toxic compounds associated with smoking tobacco are nicotine, carbon monoxide, and hydrogen cyanide. Nicotine reduces blood flow to the wound area and diminishes the proliferation of red blood cells, fibroblasts, and macrophages, which results in increased infection rates among smokers. Carbon monoxide decreases oxygen uptake in the cell, and hydrogen cyanide inhibits the ability of the cell to function properly by poisoning metabolic enzymes.25
Smoking is also associated with decreased calcium absorption, an important mineral in the bone. Because smoking contributes to the depletion of beneficial bacteria and an increase in periodontopathogenic bacteria, it has been associated with higher levels of periodontal disease.26 The prevalence and severity of periodontitis among former smokers is lower when compared with current smokers, providing evidence that smoking cessation is beneficial.27
Patients who smoke should be informed in detail about the risks of dental implant failure and that these are higher among smokers than among non-smokers. Smokers should be advised to stop smoking at least 2 weeks prior to surgery and remain smoke-free for as long as possible during the healing period, which is typically 4 to 6 months for dental implant osseointegration. Ideally, the first 8 weeks after implant placement should be a smoke-free period to allow the osteoblasts to function properly.
Conclusion
Although dental implants have exhibited high predictability and good long-term success rates, clinicians must be cognizant of the complications and failures that can occur. Understanding the factors that can affect implant failure, including soft-tissue quality, bacterial biofilm, proper technique, bruxism, medical history, vitamin D levels, and smoking, can help clinicians improve the success of patient outcomes. Taking a robust medical history allows clinicians to really understand the patient's overall health status, not just the disease status, which is key to optimizing the healing process from any surgery.
About the Author
Sanda Moldovan, DDS, MS, CNS
Beverly Hills Dental Healthand Wellness
Beverly Hills, California
References
1. Jemt T. Single-implant survival: more than 30 years of clinical experience. Int J Prosthodont. 2016;30(6):551-558.
2. Atieh MA, Alsabeeha NH, Faggion CM Jr, Duncan WJ. The frequency of peri-implant diseases: a systematic review and meta-analysis. J Periodontol. 2013;84(11):1586-1598.
3. Froum SJ, Rosen PS. A proposed classification for peri-implantitis. Int J Periodontics Restorative Dent. 2012;32(5):533-540.
4. Daubert DM, Weinstein BF, Bordin S, et al. Prevalence and predictive factors for peri-implant diseases and implant failure: a cross-sectional analysis. J Periodontol. 2015;86(3):337-347.
5. Albrektsson, T, Buser D, Chen ST, et al. Statements from the Estepona consensus meeting on peri-implantitis, February 2-4, 2012. Clin Implant Dent Relat Res. 2012;14(6):781-782.
6. Pranskunas M, Poskevicius L, Juodzbalys G, et al. Influence of peri-implant soft tissue condition and plaque accumulation on peri-implantitis: a systematic review. J Oral Maxillofac Res. 2016;7(3):e2.
7. da Silva ES, Feres M, Figueiredo LC, et al. Micro-biological diversity of peri-implantitis biofilm by Sanger sequencing. Clin Oral Implants Res. 2014;25(10):1192-1199.
8. Cortelli SC, Cortelli JR, Romeiro RL, et al. Frequency of periodontal pathogens in equivalent peri-implant and periodontal clinical statuses. Arch Oral Biol. 2013;58(1):67-74.
9. Faveri M, Figueiredo LC, Shibli JA, Pérez-Chaparro PJ, Feres M. Microbiological diversity of peri-implantitis biofilms. Adv Exp Med Biol. 2015;830:85-96.
10. Jemt T, Olsson M, Renouard F, et al. Early implant failures related to individual surgeons: an analysis covering 11,074 operations performed during 28 years. Clin Implant Dent Relat Res. 2016;18(5):861-872.
11. Antoun H, Karouni M, Abitbol J, et al. A retrospective study on 1592 consecutively performed operations in one private referral clinic. Part I: Early inflammation and early implant failures. Clin Implant Dent Relat Res. 2017;19(3):404-412.
12. Jemt T, Karouni M, Abitbol J, et al. A retrospective study on 1592 consecutively performed operations in one private referral clinic. Part II: Peri-implantitis and implant failures. Clin Implant Dent Relat Res. 2017;19(3):413-422.
13. Staubli N, Walter C, Schmidt JC, et al. Excess cement and the risk of peri-implant disease - a systematic review. Clin Oral Implants Res. 2016 Sep 19. doi: 10.1111/clr.12954.
14. Yadav K, Nagpal A, Agarwal SK, Kochhar A. Intricate assessment and evaluation of effect of bruxism on long-term survival and failure of dental implants: a comparative study. J Contemp Dent Pract. 2016;17(8):670-674.
15. Misch CE. Contemporary Implant Dentistry. 3rd ed. Maryland Heights, MO: Mosby Elsevier; 2008.
16. Misch CE. The effect of bruxism on treatment planning for dental implants. Dent Today. 2002;21
(9):76-81.
17. Salvi GE, Brägger U. Mechanical and technical risks in implant therapy. Int J Oral Maxillofac Implants. 2009;24(suppl):69-85.
18. National Center for Health Statistics. Health, United States, 2016. With Chartbook on Long-term Trends in Health. Hyattsville, MD: Centers for Disease Control and Prevention, US Dept of Health and Human Services; 2017.
19. Abariga SA, Whitcomb BW. Periodontitis and gestational diabetes mellitus: a systematic review and meta-analysis of observational studies. BMC Pregnancy Childbirth. 2016;16(1):344.
20. Balshi TJ, Wolfinger GJ. Dental implants in the diabetic patient: a retrospective study. Implant Dent. 1999;8(4):355-359.
21. Anner R, Grossmann Y, Anner Y, Levin L. Smoking, diabetes mellitus, periodontitis, and supportive periodontal treatment as factors associated with dental implant survival: a long-term retrospective evaluation of patients followed for up to 10 years. Implant Dent. 2010;19(1):57-64.
22. Chaudhry AN, Ruggiero SL. Osteonecrosis and bisphosphonates in oral and maxillofacial surgery. Oral Maxillofac Surg Clin North Am. 2007;19(2):199-206.
23. Marx, Robert. Osteoporosis - Its Controversies, Treatment and Complications. The Oral - Systemic Health Connection, Quintessence, 2014.
24. Zhou C, Li Y, Wang X, et al. 1,25Dihydroxy vitamin D(3) improves titanium implant osseointegration in osteoporotic rats. Oral Surg Oral Med Oral Pathol Oral Radiol. 2012;114(5 suppl):S174-S178.
25. Silverstein P. Smoking and wound healing. Am J Med. 1992;93(1A):22S-24S.
26. Karasneh JA, Al Habashneh RA, Marzouka NA, Thronhill MH. Effect of cigarette smoking on subgingival bacteria in healthy subjects and patients with chronic periodontitis. BMC Oral Health. 2017;
17(1):64.
27. Haber J. Smoking is a major risk factor for periodontitis. Curr Opin Periodontol. 1994:12-18.