You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Edentulous patients and those with terminal dentition suffer a disability of oral function and deterioration in their appearance and quality of life, which can also adversely affect self-esteem and social confidence. Moreover, these patients tend to avoid foods with high nutritional value such as raw fruits and vegetables, which can be difficult to chew, due to discomfort from ill-fitting dentures, advanced periodontal disease, malocclusion, temporomandibular disorders (TMD), and compromised dentition. This masticatory disability often results in inadequate consumption of protein and vital nutrients required for good health.1 Although the challenges suffered by edentulous patients are understood, dental professionals sometimes under-appreciate the plight of the soon-to-be-edentulous. These patients not only suffer with functional impairments, chronic oral inflammation, pain, halitosis, and an increased incidence of systemic diseases, but they are also wary of losing their teeth and facing the prospect of wearing a denture.2,3
Conventional approaches to full-arch fixed rehabilitation of edentulous or soon-to-be edentulous patients involve staged treatments, including tooth removal, bone and soft-tissue grafting, placement of dental implants, and delayed restoration. These approaches involve lengthy treatment times and are often cost prohibitive. While edentulous patients may accept wearing a denture during this process, soon-to-be edentulous patients typically demand a fixed provisional restoration and may be reluctant to proceed with treatment if they are required to wear a denture.
The All-on-4 full-arch immediate-function treatment concept represents both a beneficial solution for patients and a paradigm shift for clinicians. Patients treated with the All-on-4 treatment concept report high levels of satisfaction and the majority would recommend this treatment to others.4 In simple terms, this concept makes maximum use of available bone in the anterior maxilla and mandible, and achieves improved prosthesis support from use of longer, distally tilted posterior implants to improve implant distribution and reduce cantilevers. In most cases, only four implants are required. In other cases involving advanced atrophy or anatomic limitations, additional implants may be indicated. Following implant placement, angular corrections between 0° and 30° are accomplished by specialized multi-unit abutments, and an esthetic hybrid provisional prosthesis is typically delivered on the same day.
Scientific Basis for All-on-4 Full-Arch Immediate-Function Treatment Concept
In 1995, Brånemark and coworkers were among the first to determine that implant distribution is as important as the number of implants supporting a fixed prosthesis.5 In a 10-year retrospective study of 150 consecutive patients treated with full-arch fixed prostheses, the same survival rate resulted for restorations with four versus six implants.5 In 2000, Krekmanov and coworkers6 performed a study testing the effect of tilting posterior implants on implant distribution, cantilever length, and biomechanical support for full-arch fixed implant prosthesis. Among 47 consecutive patients, there were 36 mandibular and 30 maxillary implants placed at angles between 25° and 35°, with mean follow-up periods of 40 and 53 months, respectively. A mean gain in prosthesis support of 6.5 mm in the mandible and 9.3 mm in the maxilla resulted. Cumulative survival rates for tilted implants were 98% versus 93% for the non-tilted axial implants. The investigators concluded that tilting posterior implants at angles between 25° and 35° led to improved implant distribution for prosthesis support, use of longer implants with bi-cortical anchorage in dense bone, and avoidance of maxillary sinus lifts and mandibular nerve repositioning. In-vivo strain-gauge biomechanical measurements performed in this study identified no negative effects of load distribution when tilted implants were part of prosthesis support and produced a desirable reduction of implant forces by decreasing cantilever lengths.
Maló and Rangert7 coined the terminology and introduced the “All-on-4” immediate-function concept for edentulous mandibles in 2003, and, in 2005, for edentulous maxillary arches.8 Numerous supporting scientific studies9-12 and prospective and retrospective clinical studies13-25 have since been published in the past decade.
Diagnostically Driven Planning and Execution of All-on-4 Treatment Concept
The protocol for the “All-on-4” treatment concept that the authors are presenting (known as the Sclar Center Protocol) provides numerous advantages compared to first-generation protocols. These include: reduced surgical and restorative chairtime; restoration-driven surgery; simplified restorative procedures; avoidance of surgical site disruption; improved strength, durability, and esthetics of the provisional restoration; and improved patient comfort and convenience. Moreover, an impressive percentage of doctors who were trained on the described protocol have been able to successfully implement the All-on-4 concept in their practices. Requisites for implementation of this protocol include an in-depth understanding of the following: pre-treatment patient evaluation; case selection criteria; contraindications; risk factors for complications; and diagnostically driven interdisciplinary treatment planning. Moreover, precise execution of surgical and prosthetic procedures by a treatment team that has gained the required clinical skills through post-graduate education and/or mentorship specific to the All-on-4 treatment concept is required for optimal outcomes. For pre-treatment and patient evaluation details, see Table 1.
Diagnostically Driven Treatment Planning
Once the surgeon and the restorative dentist have consulted with the patient and performed a pre-treatment patient evaluation, interdisciplinary treatment planning to identify treatment options for the patient’s dental rehabilitation is completed. The surgeon should have completed and documented a dentofacial and intraoral patient evaluation as well as a radiographic diagnosis and treatment planning survey using cone beam computed tomography (CBCT) (Figure 1) to explore possible treatment options from a surgical perspective. After review of this information, the restorative dentist performs model-based diagnosis and treatment planning. The clinicians jointly review the surgical and restorative treatment planning information and select the treatment option that can be strongly recommended, as well as viable alternatives, for patient education and case presentation.
Model-Based Diagnosis and Treatment Planning
The authors’ All-on-4 treatment planning protocol relies on conventional diagnostic records, including mounted study models. When a single arch will be rehabilitated without changes to the incisal plane, occlusal plane, or the occlusal scheme of the opposing arch, diagnostic models are mounted on a hinge articulator with the aid of a bite registration. However, whenever changes to the incisal plane, occlusal plane, or occlusal scheme of the opposing arch are indicated or when skeletal inter-arch discrepancies require correction, diagnostic study models are mounted in duplicate on an adjustable articulator at the patient’s VDO aided by a facebow transfer and bite registration. When combined with clinical information gained from pre-treatment patient evaluations, all of the information required for interdisciplinary treatment planning is available.
An important advantage of this approach is the ability to simulate bone reduction on the models and verify the presence of 15 mm to 17 mm and 13 mm to 15 mm of required inter-occlusal space for maxillary and mandibular restorations, respectively. This creates a platform for a diagnostic wax-up of the proposed dental rehabilitation and fabrication of wax prosthesis try-ins when necessary. Finally, a modified All-on-4 provisional prosthesis surgical and restorative guide developed by the authors for restoration-driven surgery and simplified restorative procedures is fabricated (Figure 2 through Figure 8).
Surgical Protocol
Surgery can be performed under local anesthesia, intravenous sedation, or oral sedation. Profound local anesthesia is required. Full-arch incisions are best located to preserve keratinized tissue for adaptation around the restorative abutments.
In the maxilla, the flap is elevated to expose the entire ridge and to identify and explore the following: maxillary midline; incisive canal; infraorbital nerves; piriform apertures and nasal floor; anterior sinus wall, and the tuberosity and pterygomaxillary junction.
In the mandible, the flap is elevated to expose, identify, and explore the mental nerve foramen and anterior loops. Lingual flap elevation is limited to what is needed to perform the necessary bone reduction.
Tooth extractions are performed and bone reduction is completed using side-cutting bone rongeurs and bone reduction burs to create a level and convex implant ridge platform. The objective of bone reduction is to provide restorative space and ensure that the transition zone between the prosthesis and the ridge tissue is not visible in a fully animated smile. This also ensures a sufficient bulk of acrylic in the provisional prosthesis to evenly distribute controlled occlusal forces to the implants, thereby avoiding biomechanical implant complications such as prosthesis fracture, peri-implant crestal bone loss, and implant failure.
Multiple bone reduction and implant placement guides have been advocated in first-generation treatment protocols.7,8,13,18 Instead of fabrication of multiple costly guides, the provisional prosthesis guide developed and used by the authors is a cost-effective solution that aids in restoration-driven bone reduction, implant placement, abutment orientation, and simplified restorative and laboratory procedures.
Implants are placed to engage dense basilar bone and achieve high primary stability via under-preparation of the osteotomies. Implant placement is initiated with a handpiece, but is finished with a manual torque wrench at insertion torques between 35 Ncm and 70 Ncm. The posterior tilted implants are always placed first.
First-generation surgical protocols use the Maló guide, which is secured in a midline osteotomy after the malleable titanium band is bent to follow the arc of the opposing arch. Although this guide aids posterior angled implant placements between 30° and 45°, it does not provide landmarks required for restoration-driven surgery. However, in the authors’ protocol, the provisional prosthesis guide provides the advantage of restoration-driven surgery not afforded by previous methods. Benefits of this include: visual verification of bone reduction, restoration-driven implant placement, and abutment orientation—all of which reduce chairtime and improve surgical accuracy and decision making (Figure 9). Once abutments and protective caps are secured, the soft tissues are carefully closed after circumferential adaptation of keratinized tissues.
Prosthetic and Laboratory Protocol
Contrary to the first-generation direct “in the mouth” techniques used for denture conversion, the described prosthetic protocol uses an indirect conversion “in the laboratory” technique that is designed to: reduce chairtime; improve the quality, strength, and finish of the provisional prosthesis; and improve patient comfort, convenience, and overall satisfaction.
The following 10 steps performed in sequence make up the authors’ restorative and laboratory protocol: 1) surgical impression; 2) surgical indexing; 3) bite registration; 4) verification of the VDO; 5) laboratory fabrication of a master cast with soft-tissue model and laboratory verification; 6) indirect laboratory denture conversion; 7) delivery of the provisional restoration; 8) occlusal adjustment; 9) esthetic evaluation; 10) phonetic evaluation.
To start, a surgical impression is performed. Open-tray impression copings are secured to the restorative abutments, and a denture-strengthening bar is attached to the copings using a low-expansion pattern resin. The “salt and pepper” technique is used for precise control of the material, thereby avoiding contact with the surgery site and more effectively controlling working time. A plastic impression tray is modified in the occlusal areas where the impression copings will emerge and is tried-in to verify that there are no interferences. Polyvinylsiloxane impression putty is mixed and adapted over the impression copings and denture-strengthening bar. Impression material is also placed in the tray prior to seating. The impression coping screws are exposed and disengaged, allowing the impression to be easily removed. Rigid stabilization of the copings in the impression is verified (Figure 10 through Figure 12). The surgical index is performed using the same provisional prosthesis guide used during the surgery. Only the two anterior implants are indexed. The provisional prosthesis guide is seated to verify the absence of interferences with the two anterior temporary cylinders, and cold-cure acrylic material is applied through the access windows using a “salt and pepper” technique (Figure 13). The prosthesis is held in place with light pressure on the prosthesis guide over the palate or the posterior lingual mandibular ridge until the resin is cured. The VDO is verified after guiding the patient into occlusion with a bite registration recorded in the laboratory. Esthetic and functional parameters are verified, and the indexed prosthesis is removed with the attached temporary cylinders, and it is then disinfected in cold sterile solution.
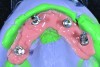
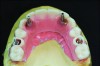
The dental technician fabricates a master cast with a soft-tissue model while the indexing and VDO procedures are performed. A silicone material is added around the implant analogues in the surgical impression before model pouring with zero expansion stone (Figure 14 and Figure 15). The soft-tissue model is removed to verify a precise fit of the temporary titanium cylinders indexed in the mouth to the master cast. The indexed provisional prosthesis is modified to allow passive attachment of the posterior temporary cylinders to the prosthesis using heat-cured acrylic processed under pressure. The technician then removes the cold-cure acrylic that was used to index the two anterior temporary components and re-secures them with fresh heat-cured acrylic under pressure (Figure 16). The intaglio surface of the provisional prosthesis is finished with cold-cure acrylic on the master cast and polished to ensure a convex surface with sufficient space to allow for tissue swelling and access for hygiene.
By following the described protocol, insertion and delivery of the provisional prosthesis should proceed without any difficulty. Retaining screws are secured at 15 Ncm. Access holes are filled with Teflon tape and temporary filling material. Functional occlusal adjustments are performed intraorally to achieve light bicuspid and anterior contacts. Esthetic and phonetic parameters are evaluated after full recovery of the anesthesia. Follow-up visits to monitor healing and occlusion are scheduled at 1 and 3 weeks post procedure. The prosthesis is not removed for 8 weeks, at which time an implant assessment is performed to evaluate implant integration and peri-implant health. The authors believe that any complications are better addressed at this stage of the treatment.
The definitive prosthesis is delivered between 6 and 12 months later, allowing time for tissue remodeling. Typically, the preferred definitive restoration is a highly esthetic acrylic hybrid prosthesis secured over a CAD/CAM-milled titanium bar designed for a full acrylic wrap on the intaglio surface of the restoration with pink restorative material that simulates gingiva. This type of restoration is cost-effective and easily repaired or modified. Alternative options include fixed zirconium bridges, fixed zirconium framework with individual cemented crowns, and porcelain-fused-to-metal restorations. Regular recall every 3 to 4 months is paramount for maintenance and to identify and rapidly treat potential biologic or biomechanical complications.
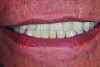
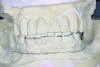
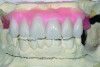
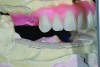
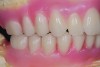
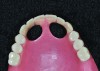
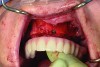
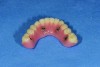
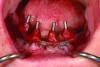
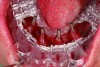
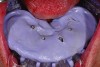
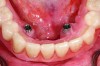
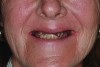
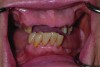
Dental rehabilitation with the All-on-4 treatment concept is often a life-changing event for edentulous and terminal dentition patients that results in unprecedented quality of life improvements (Figure 17 through Figure 20).
Conclusion
Diagnostically driven planning and execution of the All-on-4 treatment concept are the key components of the described protocol, providing advantages for patients and clinicians alike. These benefits include: reduced surgical and restorative chairtime; restoration-driven surgery; simplified restorative procedures; avoidance of surgical site disruption; improved strength, durability, and esthetics of the provisional restoration; improved patient comfort and convenience; and unprecedented ease of implementation for clinicians.
Editor’s Note
This article first appeared in the May 2015 edition of Compendium of Continuing Education in Dentistry.
Reference List AND QUIZ
Access the references and quiz for this article by going to insidedentaltech.com/idt929.
This article was double-blind peer reviewed by members of the IDT and Compendium Editorial Advisory Boards
About the authors
Anthony G. Sclar, DMD
Founder, Sclar Center for Advanced Implant Dentistry Learning • Miami, Florida
Director of Clinical Research and Dental Implant Surgery
Department of Oral and Maxillofacial Surgery
Nova Southeastern University School of Dentistry
Fort Lauderdale, Florida
Private Practice
Sclar Oral Surgery & Implant Dentistry • Miami, Florida
Juan D. Cardenas, DDS
Prosthodontist
Dental Solutions of Miami
Miami, Florida
Uli Von Haussen, CDT
President
Implant Technical Support, Inc.
Miami, Florida