You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
If there are changes in the structure of the root surface, they are most commonly diagnosed based on the presence of decay, abfraction, abrasion, or erosion.1-2 Since the introduction of CaMBRA (Caries Management by Risk Assessment), it is recommended that clinicians first accurately classify carious lesions and then treat individual patients based on their risk category assignment.3-9 The presence of gingival recession increases tooth decay risk. If coupled with other risk factors, a patient may be at a high or an extremely high risk for caries development. Therefore, it is important to classify the root-surface quality when determining if a root surface should be remineralized or restored. However, at present, there is an inadequate amount of literature classifying root-surface quality when treatment planning restorative dentistry.
In 1994, Lynch investigated the variation of color, texture, and the distance from the gingival margin of carious lesions on the root surfaces of 395 teeth. Although an increased amount of lactobacillus was found on black, leathery root surfaces, this study concluded that root surface texture and the distance of the carious lesion from the gingival margin is a more predictable indicator of active caries than color.10 The use of the International Caries Detection and Assessment System11 (ICDAS) for the diagnosis of clinical, radiographic, and root caries is an exceptionally thorough resource; however, this system does not offer assessment criteria for root demineralization of surfaces that have responded to remineralization therapy.
The use of technology in the diagnosis of caries is encouraging;12 however, the routine office use of fluorescein-enhanced quantitative light-induced fluorescence,13 electrical measurements,14 electrical and mechanical measurements,15 and infrared photothermal radiometry and modulated luminescence16 for the diagnosis of root caries in the clinical setting appears limited at this time.
The objective of the authors is to introduce a simple, efficient classification system for root-surface quality to aid the practitioner in diagnosis, treatment planning, and assessing the outcome of remineralization therapy.
Classification System
When examining a root surface, it is important to recognize changes on the root surface that may be indicative of disease. Additionally, it is important to accurately document root-surface quality so that it can be monitored for changes at every recare appointment.
A healthy exposed root surface has a firm, velvety surface.11,17 This can be evaluated visually or by palpating the surface of the root with the side of an explorer. (Note that using the tip of an explorer can actually inoculate the tooth surface with bacteria14 or damage the root surface.18 ) Changes in surface hardness, texture, color, and consistency are the primary indicators of the demineralization or caries process. A demineralized root surface may exhibit changes in one or more of these surface characteristics. The process of root-surface caries is described as the loss of mineral, color changes, softening of the surface, and cavitation.11 The CaMBRA protocols recommend treating all patients with early demineralization or active caries with a process of remineralization prior to restoring the carious lesions.3-9 The rationale for this therapy is to attempt to create an optimal oral environment by neutralizing pH and minimizing bacteria, while replenishing the demineralized tooth structure with calcium, phosphate, and fluoride. This will potentially impede the decay process and give the tooth structure an opportunity to be remineralized, thereby promoting an improved environment in which to place a more conservative restoration. The authors have created a simple classification system for the demineralization and remineralization of dental root surfaces. These changes in root surfaces due to demineralization and to subsequent remineralization were classified by the following system. Note that while other treatment options—eg, gingival grafting—can be used to restore exposed root surfaces, for the purpose of this article, the author limited the treatment discussion to remineralization and/or restorations only.
Location
It is essential to document the location of the changes of the root surface. This can be accomplished by noting specifically which root surface has been affected with changes.
The coding system is as follows: (M) mesial; (MB) mesiobuccal; (ML) mesiolingual; (D) distal; (DB) distobuccal; (DL) distolingual; (B) buccal; and (L) lingual.
Classification of Root-Surface Quality
Root-surface quality is classified by stage of demineralization and stage of remineralization, with NC indicating no change in root-surface quality.
No Change in Root-Surface Quality (NC)
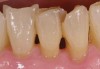
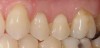
A patient with no change in root-surface quality (Figure 1) will present with gingival recession that exposes the root surfaces and no change due to disease is noted. Clinically, the root surfaces are firm, smooth, and velvety upon exploration. No color changes are noted.
Stage 1 Demineralization (D1)
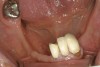
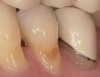
A patient with Stage 1 demineralization (Figure 2) presents with exposed root surfaces that appear dull when dried and illuminated. When palpated with the side of the explorer, the root surface feels rough and slightly soft to pressure from the side of the explorer. Color changes associated with D1 root-surface lesions may range from no color change to a darkening of the yellow color of the cementum. There is no cavitation of the root surface, and these patients may be unaware of the gingival recession occurring in their mouth. Although some patients may not present with specific concerns related to gingival recession, many patients present with sensitivity to cold and a negative perception of esthetics in the recession areas. The recommended treatment for D1 root-surface lesions includes remineralization with products (pastes and varnishes) containing fluoride, calcium, and phosphate. It is the experience of the authors that remineralization of root surfaces is often coupled with a marked decrease in sensitivity. In addition, it is critical for the clinician to determine the cause of the gingival recession to prevent the worsening of the condition.
Stage 2 Demineralization (D2)
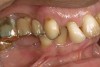
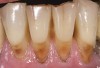
D2 root-surface lesions (Figure 3) are characterized by the dull surface demonstrated with D1 root-surface lesions. In addition, the surface feels sticky and somewhat soft when palpating with the side of the explorer. The examiner may notice that the root surface slightly resists gentle exploration over the root surface with the side of the explorer. Color changes in D2 root-surface lesions may range from dark yellow to orange/light brown. No cavitation of the root surface exists. The recommended treatment for D2 root-surface lesions includes remineralization with products (pastes and varnishes) containing fluoride, calcium, and phosphate. If the area is in the esthetic zone, the patient may request restoration, despite intact root structure.
It is common for practitioners to press the tip of the explorer into these root surfaces and decide to restore these “carious” areas. When pressing an explorer into a D2 root surface, a clinician may feel a definite softened surface or a “stick.” It is vital to either use the side of the explorer or visual inspection when determining these lesions. Aggressive exploration with the tip of the explorer may cavitate these root surfaces, which can lead to mechanical damage of the root surface and a decrease of the likelihood of successfully remineralizing the surface.
Stage 3 Demineralization (D3)
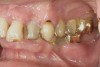
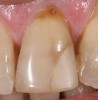
Most practitioners are currently taught to diagnose a D3 root-surface lesion (Figure 4) as active caries. The root surface is soft, sticky, cavitated, and may have debris that is easily removed with gentle palpation with the side of the explorer. Color changes may range from yellow orange/light brown to dark brown/black. The recommended treatment for D3 root-surface lesions includes remineralization of the root surface with products (pastes and varnishes) containing fluoride, calcium, and phosphate and subsequent restoration of the lost root-surface structure.
It is the experience of the authors that remineralization therapy applied to D3 root surfaces has the potential to result in root surfaces that, although discolored and cavitated, are completely hardened to a glassy, shiny surface. This allows the practitioner to preserve tooth structure that would otherwise be removed during preparation and provide a minimally invasive restoration. In cases where there is minimal cavitation in non-esthetic areas, the practitioner may opt to monitor the root surface for further change instead of placing a restoration. This classification system will aid the practitioner in diagnosing and monitoring these root surfaces.
Stage 1 Remineralization (R1)
R1 root surfaces (Figure 5) appear yellow and shiny upon visual inspection. In addition, the root surface will feel smooth, hard, and glass-like upon gentle exploration with the side of the explorer. The fluoride, calcium, and phosphate that remineralizes these root surfaces leaves them with a decreased risk for stain, sensitivity, and decay. No restoration is necessary for a patient with R1 root surfaces.
It is the experience of the authors that these patients present with sensitivity that is greatly reduced or eliminated. This greatly improves the oral health-related quality of life for such patients, as these positive results provide them with a restored or improved perception of their oral health and comfort. Moreover, these patients generally prefer to remain on the remineralization protocols indefinitely due to the noticeable positive impact from the remineralization protocols. This has resulted in increased profitability, patient retention, and referrals for the private practice.
Stage 2 Remineralization (R2)
Upon visual inspection, R2 root surfaces (Figure 6) appear shiny and dark yellow to orange/light brown. Gentle exploration reveals a hard, smooth, glass-like surface. These remineralized root surfaces do not require a restoration; however, if the color of the root surface is unesthetic, the patient may request restoration of this surface.
This classification system is useful for this specific category because it is common for D2 root surfaces to be planned by the dentist for restorations. Allowing the root surfaces an opportunity to remineralize prior to final diagnosis may result in a more conservative restoration if a restoration is required. This provides a minimally invasive approach to treatment planning and promotes patient education. In addition, it empowers patients to take responsibility for reducing their caries risk.
Stage 3 Remineralization (R3)
The R3 root surface (Figure 7) appears shiny and brown to black. Although the surface may range from pitted to cavitated, gentle exploration will reveal a hard, solid surface. This root surface is remineralized, but a restoration is required to restore the lost tooth structure.
When the patient returns after 4 weeks of remineralization/risk-reduction therapy with a R3 root surface, the dentist may decide to bond a restoration into the defect or conservatively prepare the surface for retention of a bonded or amalgam restoration. This approach minimizes the loss of tooth structure. Moreover, it is encouraging for patients to witness the positive changes in the diseased root surfaces. It reinforces the benefit of their efforts to minimize their caries risk and empowers them to play an active role in their caries management and overall oral health.
Stage 4 Remineralization (R4)
Despite the remineralization process, the R4 root surface (Figure 8) has clinical caries that is too extensive and cannot be reversed. The R4 root surface appears discolored—color can range from dark yellow to brown-black—hard, and shiny at the periphery. The central portion of the lesion is discolored, soft, and sticky. A restoration is recommended after caries removal.
In this clinical situation, although active caries is still present and restorative therapy is required for this tooth, the less involved portion of the carious lesion can remineralize. This allows the practitioner to place a smaller, shallower, less invasive restoration once the carious tooth structure is removed.
Clinical Use of this Classification System
Using this system, the clinician would document a patient’s clinical condition as follows. For a patient presenting with an exposed facial root surface on tooth No. 6 with a stage D2 demineralized lesion within an abfraction with a depth of 1 mm, the code F-D2-1 would be entered on the dental chart. The amount of gingival recession would already be noted on the completed periodontal chart. If the patient had been provided with remineralization therapy, the practitioner might note that this lesion could change into a F-R2-1 at a subsequent recall. Conversely, the practitioner could recognize negative changes in this root surface—eg, progression of the caries process or worsening of the abfraction lesion—and could recommend an appropriate treatment plan for this root surface. The use of this classification system would allow the practitioner to monitor the location, surface character, and horizontal depth of the exposed root surface.
Conclusion
It is fundamental for a practitioner to accurately document the condition of tooth/root structure to precisely recognize changes in the surface of the tooth before initiating treatment of any kind. These changes may include root-surface quality; decreases in root structure due to abrasion, abfraction, or erosion; or diminished periodontal support, resulting in increased root exposure. In addition, demineralization of the root surface may subsequently exhibit positive changes in the morphology of the root surface. These changes may occur as a result of the contact of the cementum and dentin of the root surface with fluoride and calcium and phosphate therapies, followed by restoration if needed or desired. The authors have introduced this simple, efficient, and accurate classification system for root-surface quality as an aid to the practitioner when monitoring changes in root surfaces, and in determining when and whether to remineralize or restore carious lesions on root surfaces.
References
1. Wilkins, EM. Clinical Practice of the Dental Hygienist. 8th ed. Baltimore, Maryland: Lippincott, Williams & Wilkins; 2009.
2. Daniel S, Harfst SA. Mosby’s Dental Hygiene Concepts, Cases, and Competencies. St. Louis, Missouri: Mosby; 2002.
3. Kidd EA. Caries management. Dent Clin North Am. 1999;43(4):743-764.
4. Jenson L, Budenz AW, Featherstone JD, et al. Clinical protocols for caries management by risk assessment. J Calif Dent Assoc. 2007;35(10):714-723.
5. Steinberg S. Adding caries diagnosis to caries risk assessment: the next step in caries management by risk assessment (CAMBRA). Compend Contin Educ Dent. 2009;30(8):522-526.
6. Fontana M, >Wolff MS. Evidence-based caries, risk assessment, and treatment. Dent Clin North Am. 2009;53(1):149-161.
7. Featherstone JD. The caries balance: the basis for caries management by risk assessment. Oral Health Prev Dent. 2004;2 Suppl 1:259-264.
8. Gutkowski S, Gerger D, Creasey J, et al. The role of dental hygienists, assistants, and office staff in CAMBRA. J Calif Dent Assoc. 2007;35(11):786-793.
9. Young DA, Featherstone JD, Roth JR, et al. Caries management by risk assessment: implementation guidelines. J Calif Dent Assoc. 2007;35(11):799-805.
10. Lynch E, Beighton D. A comparison of primary root caries lesions classified according to color. Caries Res. 1994;28(4):233-239.
11. International Caries Detection and Assessment System Coordinating Committee. Rationale and Evidence for the International Caries Detection and Assessment System (ICDAS II). Sept. 2005.
12. Young DA. New caries detection technologies and modern caries management: merging the strategies. Gen Dent. 2002;50(4):320-331.
13. Pretty IA, Ingram GS, Agalamanyi EA, et al. The use of fluorescein-enhanced quantitative light-induced fluorescence to monitor de- and re-mineralization of in vitro root caries. J Oral Rehabil. 2003;30(12):1151-1156.
14. Longbottom C, Huysmans MC. Electrical measurements for use in caries clinical trials. J Dent Res. 2004;83 Spec No C:C76-C79.
15. Baysan A, Prinz JF, Lynch E. Clinical criteria used to detect primary root caries with electrical and mechanical measurements in vitro. Am J Dent. 2004;17(2):94-98.
16. Jeon RJ, Hellen A, Matvienko A, et al. In vitro detection and quantification of enamel and root caries using infrared photothermal radiometry and modulated luminescence. J Biomed Opt. 2008;13(3):034025.
17. Banting, DW. The Diagnosis of Root Caries. Presentation to the NIH Consensus Development Conference on Diagnosis and Management of Dental Caries Throughout Life. March 2001.
18. Warren JJ, Levy SM, Wefel JS. Explorer probing of root caries lesions: an in-vitro study. Spec Care Dentist. 2003;23(1):18-21.
About the Authors
Pamela M. Maragliano-Muniz, DMD
Assistant Clinical Professor
Tufts University School of Dental Medicine
Boston, Massachusetts
Private Practice
Boston, Massachusetts
Dona R. Roberts, RDH
Private Practice
Boston, Massachusetts
Robert J. Chapman, DMD
Professor Emeritus
Department of Prosthodontics and Operative Dentistry
Tufts University School of Dental Medicine
Boston, Massachusetts
Private Practice
Boston, Massachusetts