You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Compromised masticatory efficiency and an impaired quality of life are associated with partial or complete edentulism, leading to a significant oral health burden.1-3 Available data indicate that the prevalence of comorbidities such as periodontal diseases and caries as well as socioeconomic constraints may have skewed the geographical distribution of edentulism more toward the developing countries.4 However, a significant proportion of patients worldwide have nonrestorable terminal dentitions. Inadequate anatomical support and tooth structure along with cost implications of a full-mouth reconstruction are arduous challenges for treatment. Furthermore, complaints such as pain, instability, gagging, and lack of retention, as well as diminished oral sensory function and minimal masticatory efficiency, limit the acceptability of conventional dentures.5
While osseointegrated implant prostheses significantly overcome the challenges associated with conventional dentures, traditional protocols involve an osseointegration period of at least 3 months to load a definitive prosthesis. Maló et al introduced the “All-on-4” treatment concept,6 which involves immediate loading of a full-arch fixed prosthesis anchored with four implants in the maxilla or mandible. The All-on-4 treatment concept is associated with substantial reductions in treatment time and cost with predictable long-term outcomes and patient satisfaction.7,8 This article describes a protocol for effectively using this concept in implant dentistry.
Overview of the All-on-4 Concept
Following teeth removal, a completely edentulous jaw is often characterized by resorption-related minimization of bone volume and a reduction in bone quality. These features may necessitate bone grafting before implants are placed. Bone augmentation techniques such as sinus augmentation with a lateral window approach (in the maxilla) and onlay grafts or nerve transposition (in the mandible) are traditional approaches, however they add significant costs and lengthen the duration of treatment. Other alternatives such as the use of long distal cantilevers, short implants, or implants placed into the zygoma or pterygoid plate offer advantages but require significant expertise for predictable success.
Utilizing two axially orientated implants in the anterior region and two tilted posterior implants (Figure 1), the All-on-4 concept facilitates an avoidance of anatomical structures as well as the accurate placement of longer implants into better quality bone anteriorly. The tilted posterior implants are key components of this concept. In the mandible, tilted posterior implants facilitate excellent bone anchorage without interfering with the mental foramina. In the resorbed posterior maxilla, the tilted implants are an alternative to sinus floor augmentation.
Biomechanical measurements reported by Krekmanov et al indicate that tilted implants as part of a prosthetic support do not have any negative impact on load distribution.9 To the contrary, tilted distal implants facilitate a better spread of the implants along the alveolar crest. This feature is beneficial for load distribution and allows the final prosthesis to hold as many as 12 teeth with only short cantilevers. This advantage of tilted implants in minimizing cantilevers is significant, as a longer cantilever can produce significant biomechanical stress on the implants. Furthermore, tilted implants allow an increased interimplant space congenial for oral hygiene procedures.
Capelli et al showed that marginal bone loss is similar between tilted and axially placed implants.10 Thus, angulating implants causes no deleterious effects to the osseointegration process. Furthermore, the All-on-4 concept is associated with a cumulative implant survival rate of 92.2% to 100%.6,7,11-15
Treatment Considerations
Presurgical Workup
The components of the presurgical workup for administering the All-on-4 techniques are outlined below. Along with these assessments, a cone-beam computed tomographic scan is important to assess bone volume. Bone profile measures > 5 mm in width and > 10 mm in vertical height are optimal prognostic indicators for the placement of implants. Computerized software planning with surgical guides can be utilized to allow for the optimal implant position.
Inclusion criteria—The All-on-4 technique can be considered an option for treating edentulism in patients with:
• good general health and acceptable oral hygiene
• sufficient bone for four implants of ≥ 10 mm in length
• implants that have sufficient stability for immediate function
Extraoral examination—The following assessments should be performed:
• An examination to assess the presence of a high or low smile line will determine the visibility of the transition zone between the junction of the soft tissues and the bridge.
• An asssessment for the requirement of a flange for lip support; removing the dentures or flange from a denture will help in assessing the need for a flange to support proper lip contour.
• An occlusal vertical dimension (OVD) assessment will help in determining the height of the lower facial third.
Intraoral examination—The intraoral examination should include checking:
• the thickness of mucosa and keratinization of tissues
• the interarch relationship
• that there is sufficient interarch space
• the incisal edge position (esthetically driven patients may require 2 mm to 3 mm of incisal display at repose position)
• for signs of parafunction or dental disease
Surgical Protocol
Prophylactic antibiotics and preoperative anti-inflammatories are recommended. Instructing patients on oral hygiene practices, including the use of a chlorhexidine mouthrinse before and during the healing process, is also recommended. The key procedural components of the surgical protocol are described as follows:
Begin by measuring the OVD by making two marks on the face (chin and nose), which will allow the copying of the previous OVD or modification if required. After crestal incisions, elevate full-thickness mucoperiosteal flaps to expose the bony ridge, and extract any tooth that requires removal. If necessary, perform an alveolectomy with bone rongeurs, burs, or Piezosugery® to level the ridge and, if required, to remove the desired amount of crestal bone to allow the transition zone (the junction between the final bridge and tissues) to be hidden under the lip line.
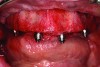
In the maxilla, the two distal implants placed in the posterior region are tilted anterior to the maxillary antrum, normally at an angle of 30° to 45° (Figure 2). In the mandible, position the implants anterior to the mental foramen and insert them at an angle of 30° to 45°. Place the All-on-4 surgical guide into a 2-mm osteotomy made in the midline position of the maxilla or mandible, and contour the titanium band to follow the arc of the opposing arch (Figure 3). Alternatively, a conventional surgical guide can be used. Use the vertical lines on the guide as a reference for drilling at the correct angulation (≤ 45°). The implant chosen should have a design and osseoconductive surface appropriate for ensuring sufficient primary stability for immediate function. A manual torque wrench is used to check the final torque, which should attain 35 Ncm to allow immediate function.
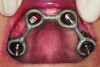
The transmucosal abutments are then placed onto the implants using either straight or 17-degree multi-unit abutments and 30-degree angulated abutments with different collar heights (Figure 4). Abutments should be orientated so that the screw access is in a favorable position. Bone grafts can be used to augment any exposed threads, extractions sockets, or other localized defects. Carefully reposition the tissues and perform suturing to form a tight seal around the abutments.
Prosthetic Protocol
The procedural steps of the provisional and final prosthetic protocols are outlined below. A primary goal of immediate loading of the provisional prostheses is to attain sufficient primary stability and then control the forces subjected to the prostheses.
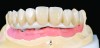
Steps for the provisional prosthetic protocol are as follows: Place open-tray multi-unit impression copings onto the multi-unit abutments, and splint the copings with a low-shrinkage autopolymerizing resin (the authors prefer GC Pattern Resin™ [GC America Inc., www.gcamerica.com]) and wire bars (Figure 5) to improve the accuracy of the impression in order to attain passive fit of the restoration. Then create an open-tray impression with a rigid vinylpolysiloxane (VPS) material to capture the positions of the implants and the soft tissues. This will allow the dental laboratory to construct a provisional all-acrylic resin prosthesis (Figure 6) that can be issued to the patient. An alternate method is to convert the pre-completed new or a well-fitting existing denture by picking up the implants in the mouth and refining the prosthesis extraorally. The provisional prosthesis should be carefully assessed for correct fit, esthetics, and function. If all is correct then the provisional prosthesis is tightened to 15 Ncm. The occlusion then is carefully adjusted so that there are contacts only in the intercanine region and no premature contacts posteriorly.11,12 At this point, the patient is given strict instructions on oral hygiene with a chlorhexidine mouthwash as well as a soft diet protocol for a period of 6 weeks to minimize micromotion.
Fabrication of the definitive bridge can be initiated at the 3-to-6–month appointment once integration is verified.
Steps for the final prosthetic protocol are as follows: First, assess the implants for integration, and check the abutments and tighten them as necessary, per the manufacturer’s instructions. Finalize the esthetics and occlusion of the provisional prostheses, taking note of any modifications that may be needed. Then, the final impressions can be made with a heavy or rigid VPS material with splinted impression copings as per the provisional protocol. The final impressions can then be verified using verification jigs to ensure accuracy and complete passive fit of the models (Figure 7).
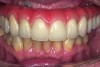
The final restorative solution can be either fixed or removable. Fixed solutions may include: computer-aided designed/computer-aided manufactured (CAD/CAM) fixed prostheses with a titanium (Figure 8 and Figure 9) or zirconia (Figure 10 and Figure 11) framework; fixed prostheses with a CAD/CAM-designed titanium or zirconia framework with acrylic veneering (Figure 12); or fixed prostheses with cast metal and veneering porcelain. Removable solutions may include a milled bar overdenture with attachments, such as locators or an MK1 Attachment (MK1 Dental Attachment GMBH, www.MK1.de) (Figure 13). Removable solutions that allow for simpler hygiene-related practices may be beneficial for elderly patients. In addition, removable solutions may be necessary for patients who require sufficient lip support, as the flange on a removable solution can assist in supporting the contours of the face. It is important to discuss the relative advantages and disadvantages of fixed and removable solutions during the informed consent process.
The occlusal scheme should be designed with the following guidelines taken into consideration16: bilateral balanced occlusion with an opposing complete denture; group function occlusion with shallow anterior guidance when opposing natural dentition; and no working and balancing contact on a cantilever.
Critial to the long-term success of this treatment, both the patient and the clinician must follow an implant maintenance protocol to promote the health of the oral tissues and allow for assessment on a regular basis.
Conclusion
The All-on-4 concept is a treatment solution for patients with edentulism and is associated with predictable outcomes.7 The placement and angulation of implants in the All-on-4 concept is a paradigm shift compared with the traditional axial placement in a vertical manner. In addition to facilitating an avoidance of anatomical structures, these angulations allow the use of longer implants. This increases bone-to-implant contact and enables implant placement into better quality bone anteriorly. Furthermore, this facilitates biomechanical advantages via a reduction in posterior cantilevers and allows for well-spaced implants. The latter is beneficial for hygiene because it allows for ease of cleaning. The All-on-4 concept has definitive cost and time advantages because this technique avoids the need for major grafting in a majority of cases. Reductions in the number of implants and components needed further augment the cost-effectiveness of this concept compared with traditional implant reconstructions.
A concern raised by some clinicians is the possibility of failure of one implant and the subsequent inability to support a fixed prosthesis, which requires a minimum of four implants. However, implant failures with this technique are relatively rare, and early failures can be addressed by modifying the provisional prosthesis and the implant can be replaced and used within the same prosthesis. After this, the final prosthesis can be constructed after the verification of optimal integration. In patients with greater risk factors, the placement of additional implants such as an all-on-5 in the mandible or an all-on-6 in the maxilla can be considered.
The long-term efficacy of the All-on-4 technique and its numerous advantages, such as immediate function and esthetics, reduced morbidity, high patient satisfaction, and relatively lower costs, should be considered when assessing treatment options for an edentulous jaw.
ACKNOWLEDGMENT
The authors would like to thank Mr. Brad Grobler (dental ceramist) for the technical and artistic expertise of the restorations included in this article.
DISCLOSURE
The author has no affiliation with any of the products mentioned in this article.
REFERENCES
1. Müller F, Naharro M, Carlsson GE. What are the prevalence and incidence of tooth loss in the adult and elderly population in Europe? Clin Oral Implants Res. 2007;18(suppl 3):2-14.
2. Wu B, Liang J, Plassman BL, et al. Edentulism trends among middle-aged and older adults in the United States: comparison of five racial/ethnic groups. Community Dent Oral Epidemiol. 2012;40(2):145-153.
3. Doğan BG, Gökalp S. Tooth loss and edentulism in the Turkish elderly. Arch Gerontol Geriatr. 2012;54(2):e162-e166.
4. Esan TA, Olusile AO, Akeredolu PA, Esan AO. Socio-demographic factors and edentulism: the Nigerian experience. BMC Oral Health. 2004;4(1):3.
5. Preoteasa E, Marin M, Imre M, et al. Patients’ satisfaction with conventional dentures and mini implant anchored overdentures. Rev Med Chir Soc Med Nat Iasi. 2012;116(1):310-316.
6. Maló P, Nobre Mde A, Petersson U, Wigren S. A pilot study of complete edentulous rehabilitation with immediate function using a new implant design: case series. Clin Implant Dent Relat Res. 2006;8(4):223-232.
7. Maló P, de Araújo Nobre M, Lopes A, et al. “All-on-4” immediate-function concept for completely edentulous maxillae: a clinical report on the medium (3 years) and long-term (5 years) outcomes. Clin Implant Dent Relat Res. 2012;14(suppl 1):e139-e150.
8. Di P, Lin Y, Li JH, et al. Clinical study of “All-on-4” implant immediate function in edentulous patients [in Chinese]. Zhonghua Kou Qiang Yi Xue Za Zhi. 2010;45(6):357-362.
9. Krekmanov L, Kahn M, Rangert B, Lindström H. Tilting of posterior mandibular and maxillary implants for improved prosthesis support. Int J Oral Maxillofac Implants. 2000;15(3):405-414.
10. Capelli M, Zuffetti F, Del Fabbro M, Testori T. Immediate rehabilitation of the completely edentulous jaw with fixed prostheses supported by either upright or tilted implants: a multicenter clinical study. Int J Oral Maxillofac Implants. 2007;22(4):639-644.
11. Maló P, Rangert B, Nobre M. “All-on-Four” immediate-function concept with Brånemark System implants for completely edentulous mandibles: a retrospective clinical study. Clin Implant Dent Relat Res. 2003;5(suppl 1):2-9.
12. Maló P, Rangert B, Nobre M. All-on-4 immediate-function concept with Brånemark System implants for completely edentulous maxillae: a 1-year retrospective clinical study. Clin Implant Dent Relat Res. 2005;7(suppl 1):S88-S94.
13. Maló P, de Araújo Nobre M, Lopes A. The use of computer-guided flapless implant surgery and four implants placed in immediate function to support a fixed denture: preliminary results after a mean follow-up period of thirteen months. J Prosthet Dent. 2007;97(6 suppl):S26-S34.
14. Pomares C. A retrospective clinical study of edentulous patients rehabilitated according to the ‘all on four’ or the ‘all on six’ immediate function concept. Eur J Oral Implantol. 2009;2(1):55-60.
15. Testori T, Del Fabbro M, Capelli M, et al. Immediate occlusal loading and tilted implants for the rehabilitation of the atrophic edentulous maxilla: 1-year interim results of a multi-center prospective study. Clin Oral Implants Res. 2008;19(3):227-232.
16. Kim Y, Oh T-J, Misch CE, Wang HL. Occlusal considerations in implant therapy: clinical guidelines with biomechanical rationale. Clin Oral Implants Res. 2005;16(1):26-35.
ABOUT THE AUTHORS
Christopher CK Ho, BDS, Grad Dip Clin Dent, M Clin Dent
Private Practice, Sydney, NSW, Australia
Sascha A. Jovanovic, DDS, MS
Academic Chairman, gIDE Dental Institute, Los Angeles, California; Private Practice in Periodontics and Implant Dentistry, Los Angeles, California
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.