You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Restorative dentistry is the art and science of reconstructing natural teeth that have been damaged, decayed, or lost in the human oral cavity. Currently, implants are the restoration of choice when replacement of teeth is necessary. Endosseous implant treatment revolutionized oral rehabilitation both for partially and fully edentulous patients. Implants provide a solution to replace missing teeth without preparing (grinding down) healthy adjacent teeth to accept a fixed bridge.1 This rapid rise in demand for implant-anchored dental prosthetics has increased demand for radiographic examinations. Three distinct modalities of dental imaging are: conventional spiral tomography, spiral multi-slice computed tomography, and cone-beam computed tomography.5
One very critical component in
selecting candidates for implant placement is their body’s ability to accept or reject an implant. Osseointegration refers to the fusion of the implant surface with the surrounding bone.3 Osseointegration of oral implants is aided by cone-beam computed tomography (CBCT) to create a predictable surgical placement. A preoperative assessment of the bone volume and quality may offer the means to better predict the likelihood of implant acceptance and therefore achieve a successful implant placement outcome.3 For a dental implant procedure to work, there must be enough bone in the jaw, and the bone has to be strong enough to hold and support the implant. The only way to truly determine whether there is sufficient bone to support an implant is to take a radiographic image that includes a measure of density. An analysis of bone quality and quality evaluations must be conducted during treatment planning. During treatment follow-up, implant stability, marginal bone level, and bone implant contact must be analyzed.8 Some studies have conclude that CBCT was not found to be reliable for measuring bone density, but that it might have potential for structural analysis of the bone.8 Implant placement directly after planning of implant position using CBCT and surgical templates can be reliable for preoperative assessment of implant size, position, and anatomical challenges. It is also indicative of cases amendable to flapless surgery.6
Conventional spiral tomography radiologic technology was not well suited to qualifying density and the true strength of bone. While dental x-rays could show bone, volume, and detail, they were very crude. The panoramic could detect a full image of the bone; however, details and density were lacking as well. It was only when cone-beam tomography entered dentistry that detailed images were clear, concise, and readily available to verify accurate placement of dental implants, thus leading to a considerable increase in implant success. The ideal application of radiological rendering is to attain the most information on the jawbone while also minimizing the radiation exposure to the patient, in accordance with the ALARA (As Low as Reasonably Achievable) principle.1
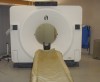
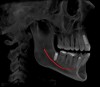
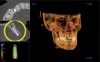
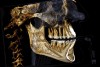
A conventional computed tomography (CT) apparatus, which is generally designed for body imaging, tends to be large in size and delivers a high radiation dose to the patient; it is also very expensive (Figure 1).2 An excellent tool for dental implant placement (Figure 2), cone beam is ideal for maxillofacial imaging.2 Its superior imaging provides details of bone morphology and bone dimensions, as well as locations of vital structures, by producing cross-sectional images along the arch (Figure 3).5,12 The apparatus is used for pre-implant evaluation, treatment planning, and the actual placement process. In addition, it is useful in follow-up evaluation of the implant (Figure 4). In terms of CBCT’s value in the pre-implant process, the ability of this imaging process to evaluate the quality of the bone in the designated implant location is outstanding. The 3D technology available with cone-beam computed tomography enables the volume (thickness and composition) of the bone to be easily evaluated in different areas. This is helpful in terms of guiding the practitioner during the implant process.3,14
Cone-beam computed tomography, digital volume tomography, and cone beam imaging,2,12 were actually initiated in the area of dentomaxillofacial (mouth, jaw, and neck) imaging as early as 1998.9 In dental maxillofacial imaging, there are four primary areas for its use: pre-surgical visualization on third molars, temporal mandibular joint dysfunction, jaw disease, and dental implant planning (Figure 5). CBCT, which was specifically developed for the maxillofacial region, produces better images than the conventional computed tomography at a considerably lower radiation dose and cost.6 In the past, imaging of these areas of dental and maxillofacial diseases had been performed using plain film and panoramic imaging, but CBCT can enhance a radiographic diagnosis (Figure 6).
For many, the use of an advanced radiographic method was nearly prohibitive due to factors such as the enormous expenditure of resources, lack of accessibility, and increased radiation dose. The advantage of CBCT includes a decrease in patient dose due to the scanner’s ability to scan in small areas, thus reducing the size of the irradiated area. Additionally, there have been published reports that have shown evidence that the use of CBCT significantly reduces patient radiation dose compared to that of a routine radiographic survey of the teeth. The radiation dose for a full-head cone-beam image is equivalent to that of about four panoramic radiographs. In comparison, the CBCT requires 30 to 90 times less radiation than the conventional computed tomography apparatus used presently.4,14 A voxel is a volume element (volumetric pixel) representing a value in the 3D space (expressed in units of mm3); it corresponds to a pixel for a given slice thickness. Voxels are frequently used in the visualization and analysis of medical data. The CT pixel intensity is proportional to the signal intensity of the appropriate voxel. Voxels are associated with CT numbers.10 Cone-beam computed tomography reconstructions peform with smaller voxels compared to conventional computed tomography, which is beneficial in attaining a more accurate image of the 3D surfaces of the teeth and bone.7 Furthermore, the detail of the CBCT image is far greater than that of conventional CT due to the make-up of the CBCT voxels. Also, the CBCT unit is much smaller and less expensive than conventional computed tomography, which makes it easy to house in a dental laboratory.4,5
CBCT uses an orthogonal projection of radiation, indicating that the radiation or x-ray beams run approximately parallel to one another, and the position of the object is very close to the detector. It uses low radiation doses, a short scanning time, and reduces the purchase cost in comparison to conventional computed tomography.2 There are, however, some disadvantages associated with CBCTs, including their inability to discriminate bone and soft-tissue boundaries, scattered radiation, and beam-hardening artifacts. These artifacts may seriously affect the quality of the radiologic rendering produced by CBCT.2 Beam-hardening artifacts occur from two different artifacts—cupping artifacts and streaks artifacts. Cupping artifacts occur when radiation passes directly through the center of the object and therefore become harder than the ones passing through the edges, leaving misleading images
on the radiograph.2 Streaks artifacts have the distinct visual look of dark streaks between two dense objects. This is commonly seen while radiographing two closely placed implants. Also, exposure quality and number of artifacts have a direct correlation to the total number of dental restorations. The total restorations include implants, crown, bridges, and fillings, regardless of the material. The strongest correlation was observed for bridges and metallic restorations (Figure 6).9
Once a radiographic rendering of the oral bone structure is attained, the use of computer-aided design and manufacturing (CAD/CAM) is used to produce a surgical stent or guide, as well as to transfer relevant information about the patient’s bone to the dental team(Figure 7). During the dental implant placement, a CT-based template should facilitate precise implant placement and reduce the risk of damage to adjacent vital structures.6 A CBCT-guided surgical plan technique uses stereolithography, a laser-sintered polymerization process that fabricates surgical guides.4,13 Using the CT scanning software, the surgeon is able to select the optimal sites for implant placement. The stereolithographic drill/surgical guide allows the surgeon to have a complete physical transfer of the information from the planning process to the patient’s oral cavity.4,11
Conclusion
As the trends continue and implants are more sought after than their previous and more invasive predecessors, restorative options including proper planning and placement of implants in the human dentomaxillofacial become vital to success. As more dental technologists collaborate and share their expertise during the planning stages, knowledge is imperative for their constant professional growth. Dental technologists increasingly find themselves working alongside surgeons, not only manipulating the sophisticated CAD/CAM, but truly applying their professional expertise and competence for the sake of an optimal outcome. Dental laboratories are embracing the same technology and becoming extensions of the surgeons by acting as members of the planning team for implant placement rather than becoming involved “after the fact,” as has
been traditional.
Acknowledgement
The author would like to extend his gratitude for the insights provided by his friend and colleague, Professor Jennett M. Ingrassia, MSRS, RT(R), assistant professor in the department of radiologic technology and medical imaging at New York City College of Technology, The City University of New York. The author would also like to thank Mark Jackson, RDT, for
his contributions.
References
1. Guerrero ME, Jacobs R, Loubele M, et al. State-of-the-art on cone beam CT imaging for preoperative planning of implant placement. Clin Oral Investig. 2006;10(1):1-7.
2. Razavi T, Palmer RM, Davis J, et al. Accuracy of measuring the cortical bone thickness adjacent to dental implants using cone beam computed tomography. Clin Oral Implants Res. 2010;21(7):718-725.
3. Van Assche N, van Steenberghe D, Guerrero ME, et al. Accuracy of implant placement based on pre-surgical planning of three-dimensional cone-beam images: a pilot study. J Clin Periodentol. 2007;34(9):816-821.
4. van der Zel JM. Implant planning and placement using optical scanning and cone beam CT technology. J Prosthodont. 2008;17(6):476-481.
5. Chau AC, Fung K. Comparison of radiation dose for implant imaging using conventional spiral tomography, computed tomography, and cone-beam computed tomography. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107(4):559-565.
6. Nickenig HJ, Eitner S. Reliability of implant placement after virtual planning of implant positions using cone beam CT data and surgical (guide) templates. J Craniomaxillofac Surg. 2007;35(4-5):207-211.
7. Hassan B, Couto Souza P, Jacobs R, et al. Influence of scanning and reconstruction parameters on quality of three-dimensional surface models of the dental arches from cone beam computed tomography. Clin Oral Investig. 2010;14(3):303-310.
8. Corpas Ldos S, Jacobs R, Quirynen M, et al. Peri-implant bone tissue assessment by comparing the outcome of intra-oral radiograph and cone beam computed tomography analyses to the histological standard. Clin Oral Implants Res. 2011;22(5)492-499.
9. Ritter L, Mischkowski RA, Neugebauer J, et al. The influence of body mass index, age, implants, and dental restorations on image quality of cone beam computed tomography. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;108(3):e108-116.
10. Nickenig HJ, Eitner S. An alternative method to match planned and achieved position of implants, after virtual planning using cone-beam CT data and surgical guide templates-- a method reducing patient radiation exposure (part I). J Craniomaxillofac Surg. 2010;38(6):436-440.
11. Belser UC, Schmid B, Higginbottom F, Buser D. Outcome analysis of implant restorations located in the anterior maxilla: a review of the recent literature. Int J Oral Maxillofac Implants. 2004;19(suppl):30-42.
12. Besimo C, Lambrecht JT, Guindy JS. Accuracy of implant treatment planning utilizing template-guided reformatted computed tomography. Dentomaxillofac Radiol. 2000;29(1):46-51.
13. Fortin T, Coudert JL, Champleboux G, et al. Computer-assisted dental implant surgery using computed tomography. J Image Guid Surg. 1995;1(1):53-58.
About the Author
Daniel Alter, CDT, MDT
Assistant Professor,
Department of Restorative Dentistry,
New York City College of Technology,
The City University of New York
Brooklyn, New York