You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Methamphetamine is a potent central nervous system stimulant with a strong affinity for addiction and abuse. It is a white, odorless, bitter-tasting crystalline powder that readily dissolves in water or alcohol. It is ingested in several ways: orally in tablet form, intranasal or snorting of the powder form, smoking of the crystalline form, and/or through injection. It is called by many different names, including ice, crystal, speed, glass, tweak, rock, yuba (tablet form), and several others.1 According to one national survey, approximately 10 million people in the United States have tried methamphetamine at least once.2
Methamphetamine abuse leads to devastating medical, psychological, and social consequences. Adverse health effects include memory loss, aggression, psychotic behavior, heart damage, malnutrition, and severe dental problems. Methamphetamine abuse also contributes to increased transmission of infectious diseases, such as hepatitis and HIV/AIDS, and can infuse whole communities with new waves of crime, unemployment, child neglect or abuse, and other social ills.2
The good news is that methamphetamine abuse can be prevented and methamphetamine addiction can be treated. Prevention strategies around the country are proving to be effective in minimizing experimentation and use and for addicts seeking recovery. People do recover, but only when effective treatments that address the multitude of problems resulting from methamphetamine abuse are readily available.2,3
The deleterious effects on the teeth often cause addicts to seek dental treatment. Because dentists are the first healthcare professionals that this demographic usually seeks out, the dental profession can have a large impact in getting the user the needed treatment for their dental problems, as well as serving as a link to potential treatment for their addiction.
The intent of this article is to enlighten the reader to the drug’s mechanism of action, to identify the oral effects of using the drug, to discuss the scope of the problem, and to advise on successful modalities to treat both the dental effects of the drug as well as the addiction.
Mechanism of Action
Neurologically, methamphetamine is structurally similar to amphetamine and the neurotransmitter dopamine, but it is quite different from cocaine. Although these stimulants have similar behavioral and physiological effects, there are some major differences in the basic mechanisms of how they work.2
In contrast to cocaine, which is quickly removed and almost completely metabolized in the body, methamphetamine has a much longer duration of action and a larger percentage of the drug remains unchanged in the body. This results in methamphetamine being present in the brain longer, which ultimately leads to prolonged stimulant effects (up to 12 hours). Although both methamphetamine and cocaine increase levels of the brain chemical dopamine, animal studies reveal much higher levels of dopamine after administration of methamphetamine due to the different mechanisms of action within nerve cells in response to these drugs.2
Cocaine prolongs dopamine actions in the brain by blocking dopamine re-uptake. While at low doses methamphetamine blocks dopamine re-uptake, it also increases the release of dopamine, leading to much higher concentrations in the synapse, which can be toxic to nerve terminals.2 In the short term, a user of methamphetamine will experience an intense rush of pleasure, a loss of appetite, long periods of wakefulness, increased respiration and blood pressure, tremors/convulsions (tweaks), and hyperthermia.4 Addiction can occur quickly in early stages of use. After a prolonged use of the drug, the user will almost always experience dependence and/or addiction.4 There will be episodes of delusional psychosis and paranoia, hallucinations, extreme and sudden mood changes, repetitive motor activity, stroke, weight loss, extreme tooth damage/periodontitis, damage to up to 50% of the brain’s dopamine-producing cells (sometimes irreversible), and skin sores. Addicted users report that they can go on drug binges that can last for up to 10 days without sleep and with minimal nutritional sustenance.
As the user becomes more dependent, a tolerance develops. This tolerance initiates cravings for an increased amount of the drug or a change of intake to achieve the same high. The user will usually progress from pill form (least risk) or snorting to smoking and then to injection (highest risk) as the means for intake. As the amount of drug increases and the intake modality becomes more risky, users put themselves at risk for severe liver, kidney, heart, or brain damage. Also, because of the strong association of precarious sexual behavior, users are also at a higher risk to contract various sexually transmitted diseases, Hepatitis B and C, and HIV infection.
Oral Effects
Methamphetamine use has devastating effects on the oral cavity, and are severe enough to prompt the user to seek dental care because of pain and/or esthetic issues. It causes decreased salivary flow, resulting in pronounced xerostomia. Without the buffering and cleansing capacity of adequate saliva, teeth are highly susceptible to decay. Users tend to drink soft drinks high in caffeine and sugar (such as Mountain Dew) to reduce mouth dryness and increase the high.
Oral hygiene is generally poor. Food and nutrition will be secondary to taking another hit of the drug. Periodontal problems, therefore, become a common sequela of continued neglect and reduced blood supply to the gingiva.
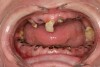
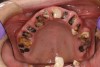
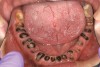
When smoked, methamphetamine produces highly toxic and corrosive fumes of lithium, muriatic, and sulfuric acids that can destroy enamel rapidly. With continued use, methamphetamine can produce severe, rampant caries, similar to early childhood caries. Patients have reported noticing changes in the appearance of tooth structure in as little as 3 months of use. The affected surfaces are the buccal and labial smooth surfaces, as well as the interproximal surfaces (Figure 1 through Figure 3). Because in the general population the vast majority of decay is found in the posterior molars, when someone presents with rampant anterior lesions it should be a red flag for methamphetamine use.5
While high on the drug, users exhibit repetitive motor activities such as clenching and grinding of their teeth. This leads to severe attrition compounded by the chemical erosion from the toxic by-products produced from smoking the drug. Increased function further affects the periodontal health and can contribute to premature tooth loss.
Although the most common problems (classic presentation of rampant caries) occur from smoking methamphetamine, signs of oral damage are evident from the other options for intake of the drug. The presentations are similar to those who are addicted to or abuse other drugs such as tobacco, alcohol, marijuana, heroin, prescription medications, etc. These include poor oral hygiene, fractured or missing teeth, severe tooth wear, advancing periodontitis, thick “ropey” saliva, xerostomia, inflamed oral mucosa, etc.
The Scope of the Problem
According to the 2007 National Survey on Drug Use and Health, there has been an 11% increase in the number of methamphetamine-dependent users nationally since 2005.6 In that same period of time, 47% of hospitals report methamphetamine as the top illicit drug involved with emergency room visits. Treatment admissions for methamphetamine dependence more than doubled nationally between 2000 and 2005.7
The US Department of Justice’s National Drug Threat Assessment 2009 continues to report that an overwhelming percentage (68%) of state and local agencies in the 20 Western states perceive methamphetamine as their greatest drug threat.8 Comparatively, 19% perceive cocaine as their top threat.
The Changing Demographics of Meth
Forty-seven percent of county sheriffs surveyed report that methamphetamine is their top drug problem. That is more than cocaine (21%) and marijuana (22%) combined.8,9 The survey found that 60% of the sheriffs reported increased use by women and 49% reported increased use by teens during the last 3 years; 50% report abuse of the drug has stayed the same and 30% report that it has increased.9
The availability of methamphetamine continues to grow. Even with federal precursor legislation, 38% of the sheriffs surveyed reported an increase in the availability of methamphetamine, largely because of importation from across state lines and from Mexico.9
Brief Interventions
The Survey of Current Issues in Dentistry is published periodically by the American Dental Association and covers various topics of interest. The latest survey was conducted in 2007. Its objective was to obtain information on a number of issues currently affecting private practitioners. Twenty-one hundred dentists responded to the questions pertaining to substance abuse.10
From this study, there were several points that were relevant to treatment of a patient who has substance abuse issues. Of note, two in five dentists (39%) have treated at least one patient with “meth mouth” in the last year, and 17.5% of dentists have consulted the “meth mouth” resources on ADA.org. The vast majority (99.7%) thought the information on “meth mouth” found on ADA.org was either somewhat or very helpful.
With regard to dentists asking their patients about alcohol or drug use, more than half (54%) of dentists do not ask their patients about alcohol use. Of those who do not regularly ask, more than half (56.4%) were either somewhat uncomfortable or not at all comfortable about asking patients about their alcohol use. Similarly, 52.4% of dentists do not ask their patients about their use of illegal substances. Of those who do not ask, compared to alcohol use, more dentists (65.6%) feel either somewhat uncomfortable or not at all comfortable asking the question.
Dentists overwhelmingly do not know what to do with a patient who abuses alcohol or drugs. Eighty-seven percent of dentists surveyed agreed that dentists should make a treatment recommendation to a patient who admits to heavy drinking or drug use, but do not know how.
On a more positive note, research shows that healthcare professionals play an important role in their patients’ health decisions. A recent analysis concluded that brief interventions may reduce mortality rates among problem drinkers by an estimated 23% to 26%.11,12 Dentists can be equally effective.
Recommendations for Brief Intervention
Express genuine concern regarding the dental findings and more importantly, the overall well-being of the patient. Reinforce the fact that if the patient chooses to use or continues to use methamphetamine, it could be life-threatening or life-ending. If the patient is receptive to a medical consult, have the phone number of a local physician, clinic, or substance abuse rehabilitation facility available and be familiar with their protocol, so the patient can be told what to expect. Offer personal support while in treatment if appropriate. If the patient is a minor, a judicious discussion with the family may be helpful in getting the patient the help he or she needs.
When conducted in a caring genuine manner, it has been proven that brief interventions conducted by a healthcare professional such as a dentist profoundly affects a patient’s motivation to change and could save his or her life.
Recommendations for Dental Treatment
Commence with a complete and comprehensive oral examination that includes a thorough dental and medical history. It is strongly recommended that the patient receive treatment for the addiction and get medical clearance prior to providing any dental treatment. Long-term drug abuse can lead to liver, kidney, heart, and/or brain damage. An assessment of all major systems should be completed by a physician who knows the patient’s history of addiction and is experienced in treating an addict. These patients are also at an increased risk for HIV, Hepatitis B, and Hepatitis C.
Provide dentistry as needed only if the patient is clean and sober. If the addiction is not addressed, there is a strong inclination that the patient will continue to abuse drugs. Because of the devastating effects on the teeth, any dentistry done on an actively using methamphetamine addict will most likely fail.
It is also dangerous to the patient’s overall health if he or she is actively using methamphetamine. Injections of local anesthetic with vasoconstrictors such as epinephrine can push the patient toward stroke, heart attack, etc. Also, because of increased liver function, rapid breakdown of local anesthetic usually occurs, causing decreased efficacy and difficult patient management. An active user will behave very erratically, especially under duress. It is recommended that emergency dental treatment be provided on a sober patient as needed, but only after medical clearance.
Use caution when providing complicated dental treatment. Dentistry is a partnership between the dentist and the patient. The dentist’s job is to provide dentistry at the standard of care as defined by the state. The patient’s job is to maintain their teeth as directed by the dental professional. The patient must consent to meticulous oral care and continued sobriety. Poor oral hygiene and relapse behavior are devastating to the teeth and to dental work. Do not guarantee your dental work under these conditions.
Encourage proper nutrition. Discuss how nutrition can help the overall health and success of the treatment that you will provide. Also discuss how poor nutrition can be deleterious to the success of the dentition/dental work provided. A patient that is clean from methamphetamine and still ingesting large amounts of soda will continue to have a high rate of caries. Reinforce and encourage proper nutrition often as you would with any patient.
When it is determined that the patient is cleared for dental treatment, establish a foundation of health first by treating infections as necessary. This will usually include extractions, root canals, periodontal scaling and root planing. Restore teeth as necessary; the use of a removable prosthesis is usually indicated to restore esthetic and functional concerns.
It is recommended to provisionalize teeth with direct restorations and monitor the patient’s compliance for a period of time. Predicted success will be determined by the patient’s level of commitment to their daily home care and by their continued commitment to their recovery.
When a level of confidence has been established that the patient can move forward with more definitive treatment, reiterate your support to him/her. Also, maintain a firm message of compliance. Remember that addiction is a treatable disease with the possibility of long-term remission with proper treatment and diligent discipline to maintain recovery.
Closely monitor oral hygiene and suspicious behaviors. Immediately express concern to the patient if you notice changes in either. Document all findings in detail both good and bad. Meticulous notes of normal behavior may prove useful in the future if relapse behavior is suspected.
Be cautious when prescribing narcotics, sedatives, general anesthesia, or nitrous oxide. They could trigger euphoric recall that could either lead to a relapse of the addiction to their primary drug of choice or possibly initiate a substitute addiction. Administration of local anesthetics with epinephrine can also trigger a euphoric recall. An accidental venous puncture leading to an increased heart rate can trigger the process, although to a much lesser extent.
Case Report
Joe presented to the primary author’s office when he was 24 years old. He had started using methamphetamine when he was 16. His peers used it and he wanted to fit in with his friends. His initial intake method was nasal (snorting the powder) but he quickly progressed to smoking the drug. There was an instant feeling of euphoria, followed by an intense crash. To combat the crash, Joe used more and more, often leading to illegal activities such as minor thefts and subsequent misdemeanor arrests. His diet included many sweets, alcohol, and his drink of choice was split between Mountain Dew and Red Bull. Meth users crave sugar and caffeine to keep the buzz going.
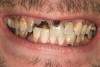
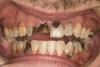
Joe soon learned how to manufacture the drug. His need for meth soon consumed his every thought. He basically lived to do more meth. He admitted that he had made some poor choices. Unfortunately once the addiction kicked in, he no longer had a choice, he had to use. This was his end result (Figure 4 through Figure 6). From these photographs, one might think that he had used the drugs his entire life; however, this progression happened over the course of only about 1 year of smoking the drug. Because of the caustic chemicals (muriatic acid, hydrochloric acid, lithium, etc) his teeth started to blacken, then break.
Through all of this, there were no trips to the dentist. He knew his teeth were a mess, but he did not care. His addiction had such a hold on him that the only thing that he had to do every day was to get high. The addicted mind lowers a person’s values. It “hijacks” the brain to justify and rationalize why doing more meth is the most important reason for existence.
When Joe was finally arrested, his teeth were in the state seen in Figure 4 through Figure 6. He entered rehab, then served his time in prison. He received no dental treatment in prison. Once he was released on probation, he found it quite difficult to find a job. He was hired as a mechanic but only allowed to work in the garage. He was to have no contact with the customers because his appearance was hideous. His self-esteem was at the lowest point it could be. He felt better in prison. At least there, his prison mates understood why his teeth looked the way they did; many people in prison are there as a result of a chemical dependency issue.
As a new patient, Joe was instantly likable. He had a great sense of humor. He regretted how his life had turned out. When he finally presented to this author’s practice he was 24 years old. He wanted to remove the evidence of his addiction that were visible to anyone that came in contact with him. His teeth were totally destroyed by his drug use. There was no hope of saving any of them. There were horrible infections in his jaw bones that were spreading through his system. His only option was to remove all of his teeth and have dentures made. Impressions were taken with alginate. A bite was established in maximum intercuspation. We decided that his preoperative incisal edge positions of teeth Nos. 9 and 10 were adequate to recreate the incisal edge position in full dentures.
Full-mouth extraction was performed under local anesthetic (a combination of articaine 4% with 1:100K epinephrine, and marcaine 0.5% with 1:200K epinephrine). After the extractions, the bone was smoothed and sockets were curetted to remove debris and infected tissue. The extraction sites were then irrigated with sterile water. The tissue was then sutured with 3-0 silk. Immediate upper and lower dentures were placed and lined with tissue conditioner. A hard laboratory reline was performed 12 weeks after initial treatment.
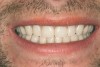
After his treatment was complete (Figure 7 and Figure 8), Joe wrote a letter to convey his gratitude. In part, it said:
I just wanted to say thank you for this opportunity that has really helped me in ways unimaginable. Now I can look in the mirror and see myself as I used to look before my addiction took hold of me. I now hold my head up proudly. I am no longer self-conscious about how I look and I have been clean for almost 2 years. With my new teeth, I now look clean as well. People look at me differently, and they treat me like I am a normal person! I feel whole. Thank you for my smile. You have changed my life!
Conclusion
Never before has the profession of dentistry been offered an opportunity such as this to profoundly affect or even save the lives of our patients and to improve our communities. Patient management is the key issue when dealing with the methamphetamine addict. Properly restoring a smile can greatly improve the self-esteem of a patient, especially in someone who is in the early stages of recovery.
Just like any other chronic disease (diabetes, heart disease, cancer, etc), the disease of addiction holds no prejudice. It affects all demographics with equal intensity. The disease is treatable with the prospect for long-term remission if the patient is motivated to take the responsibility for the daily maintenance of his or her disease. Dentists can partake in helping a recovering addict (methamphetamine or any other drug) return to a normal, healthy life.
Author’s Note
For more information on the various treatment modalities and successful prevention programs available to treat methamphetamine addiction, log on to: www.insidedentistry.net.
References
1. Klasser G, Epstein J. Methamphetamine and its impact on dental care. J Can Dent Assoc. 2005;71(10):759-762.
2. National Institutes of Health: National Institute on Drug Abuse. “Methamphetamine–Abuse and Addiction.” Research Report Series. September 2006.
3. National Institutes of Health: National Institute on Drug Abuse. The Science of Addiction. “Preventing Drug Abuse: The Best Strategy.” May 2007. Available at: www.drugabuse.gov/scienceofaddiction/. Accessed December 17, 2009.
4. National Institutes of Health: National Institute on Drug Abuse. Methamphetamine Abuse Addiction. Research Report Series. 1998:4.
5. Mallat M. Meth mouth, a national scourge. J Indiana Dent Assoc. 2005;84(3):28-29.
6. US Department of Health and Human Services, Substance Abuse & Mental Health Services Administration. 2007 National Survey on Drug Use and Health. Available at: http://www.oas.samhsa.gov/nsduh/2k8nsduh/2k8Results.pdf. Accessed December 17, 2009.
7. Byker C. The Meth Epidemic. A production of Frontline and PBS. Aired February 14, 2006. Available at: http://www.pbs.org/wgbh/pages/frontline/meth/. Accessed December 17, 2009.
8. US Department of Justice: National Drug Intelligence Center. National Drug Threat Assessment 2009. Available at: http://www.justice.gov/ndic/pubs31/31379/index.htm. Accessed December 17, 2009.
9. National Association of Counties. The Methamphetamine Epidemic: The Changing Demographics of Methamphetamine. August 2007.
10. American Dental Association. Survey of Current Issues in Dentistry. Available at: http://www.ada.org/ada/prod/survey/publications_issues.asp#surveyofcurrent. Accessed December 17, 2009.
11. Cuijpers P, Riper H, Lemmers L. The effects on mortality of brief interventions for problem drinking: A meta-analysis. Addiction. 2004;99:839-845.
12. National Institutes of Health: National Institute on Alcohol Abuse and Alcoholism. Alcohol Alert, Number 66, July 2005.
About the Authors
Brett H. Kessler, DDS, Clinical Associate Professor, University of Colorado School of Dental Medicine, Denver, Colorado; Co-Chair, University of Utah School on Alcoholism and Other Drug Dependencies, Salt Lake City, Utah
Michael Dinneen, LCSW, CAC II, Clinical Manager, Center for Dependency, Addiction, and Rehabilitation, University of Colorado Hospital, Aurora, Colorado