You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Stability is a necessary part of existence. For societies to function, a stable government must be in place. For a bridge to span a river, the foundations at each shore must be solid if the structure is to handle a load. The examples are numerous, but one cannot escape the need for stability in every aspect of life.
The same can be said for restorative dentistry. Success in dentistry can be broken down into esthetic success and biologic or functional success. Patients are acutely aware of esthetics and are quick to determine whether or not esthetic success has been achieved. Functional success may be more difficult for the patient and the dentist to assess, for in making this determination, time is often the critical factor. The longer a restoration lasts, one can often say the better it was able to function in a harmonious manner.
Teeth fail from two primary reasons: bacterial assault or excessive or misdirected forces. This could be in the form of coronal tooth caries, or from loss of the supporting periodontal structures, ie, periodontal disease. Teeth can also fail from excessive or misdirected forces. Teeth that are weakened from wear, or are loaded in non-axial vectors, often fail which, in turn, results in loss of tooth structure.
Adequate diagnosis often depends on the ability to determine the weak link of the masticatory system. People can have teeth largely unscathed from decay and still lose their teeth to periodontal disease. Likewise, this author has seen people suffering temporomandibular joint breakdown with little to show in regards to tooth wear, while in other instances a person can destroy their teeth through parafunction and complain little of muscle or joint issues. Every patient may have various combinations of clinically relevant issues. The difference between healthy and failing dentition is often reflected in how the body handles bacteria and functional instability.
This article presents insights on the importance of anterior guidance, which can often be the variable to allow control of forces influencing the teeth and restorations. Natural teeth and restorations will last longer if they are placed into a stable relationship. Dr. Peter Dawson describes the five requirements for occlusal stability,1 as follows:
1. Stable holding contacts on all teeth when the condyles are in centric relation.
Centric relation is a stable, anatomically dictated position. This position describes the fully seated position of the condyles in the glenoid fossa. It is described as a stable axial position when the condyle-disk assemblies are in their most superior position. The assemblies are braced medially in the glenoid fossa and are capable of being loaded without discomfort.2 A tripod of stability is formed when both condyles are in centric relation and anterior contact is established. From this position an interference-free occlusion can be developed, derived from a stable and repeatable anatomic position.3
2. Anterior guidance in harmony with the envelope of function.
The mandibular and maxillary teeth interact and must do so in a passive manner. A tooth’s inclination, position, and shape (lingual contour of the maxillary anteriors) will affect the envelope of function. The anterior guidance must accept the boundaries dictated by the envelope of motion of the condyles and the lower incisors. The proper position of the anterior teeth and, thus, the envelope of function varies from patient to patient. The anterior teeth are balanced by opposing forces applied by the muscles of the lips and the tongue; therefore, the position and inclination of the anterior teeth will be variable. One must be sure to allow an incisal edge position that does not interfere with the pathway of the lower incisors, and to allow lingual contours that to not constrict or retrude the mandible. These violations could result in excessive wear, chipping of teeth or porcelain, or unwanted tooth movement.
3. Immediate disclusion of all posterior teeth the moment the mandible moves forward of centric relation (protrusive guidance).
4. Immediate disclusion of all posterior teeth on the non-working side.
5. Non-interference of all posterior teeth on the working side with either the lateral anterior guidance or the border movements of the condyles.
Various opinions exist on the best form of anterior guidance. In decades past, it was thought that balanced and group function offered the best way to distribute forces. Teeth could, in essence, share the load from the musculature in an excursive movement. As time progressed and the ability to measure the activity of muscles increased, opinions have shifted. It was found that, in many cases, canine guidance offered the best choice. Canine guidance immediately discludes the posterior teeth in excursive movement on the working and non-working sides. Studies have shown that this relationship offers the better management of muscular forces. Disclusion of the posterior teeth decreases muscular activity, which in turn decreases the loads on the teeth.4-7 When pure anterior guidance exists, the main elevator muscles are neurologically shut down, thus decreasing the force on the anterior teeth.4-7
The bite forces between the anterior teeth and posterior teeth vary by a factor of 9. This is because when the posterior teeth are in contact (proprioceptive/mechanoreceptive neuromuscular reflex), the major elevator muscles are in use.8 The posterior teeth are designed to be loaded along their long axis. Lateral forces applied to the posterior teeth can cause signs of instability in the occlusion. These would include excessive mobility of one or numerous teeth, excessive wear, or migration of one or more teeth.
Dentin exposure is not normal and is indicative of occlusal instability. The serious nature of this problem is highlighted when considering the rate of wear difference between enamel and dentin. Exposed dentin wears at a much faster rate than enamel, and this difference is compounded when loading of the dentin is occurring and the pH levels are more acidic.9
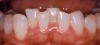
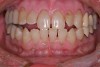
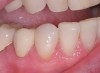
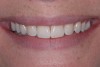
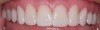
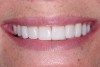
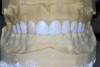
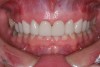
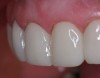
For canine guidance to be achieved, the canine teeth themselves must be in a position to function. Instability causes wear, and as this wear progresses, teeth loose their natural contour. Teeth may also not be in the proper position within the alveolar ridge to allow proper contact in canine guidance (Figure 1 and Figure 2). In these cases, Dr. Dawson describes five choices for correcting occlusal disharmonies.10 They are:
- Reductive reshaping or coronoplasty (equilibration).
- Repositioning teeth within the alveolar bone with orthodontics.
- Additive reshaping through restorative dentistry.
- Repositioning segments of the alveolar ridge without changing the skeletal base.
- Repositioning of skeletal segments in relation to the cranial base.
When restoration becomes necessary, it is also important to recognize functional patterns. A person who often moves their mandible horizontally and can protrude with little difficulty will exhibit flat, worn anterior teeth. And as the anterior wear continues, the posterior teeth will also begin to lose their anatomy. The other spectrum would include patients who wear their teeth with a vertical bias. These patients would have the wear confined to just their anterior teeth. The anterior incisors are often greatly affected, with little wear beyond the canine teeth. Vertical-pattern patients will often have difficulty moving their mandible laterally, while horizontal-pattern patients can freely move in any direction.
It is important to recognize these patterns. The main reason is that you do not want to “trap” a horizontal-functioning patient. The guidance of the anterior teeth should allow easy disclusion of the posterior teeth once they are leaving intercuspation. If the new anterior guidance is too steep, the horizontal patient will be always placing force on the teeth to seek the freedom of movement. The main point is to recognize that the mandible will have a favored functional pattern, and to not place dental restorations in the way. By having a stable occlusal set-up, with proper anterior guidance, one cannot wear that which cannot be rubbed together.
The reality is that many clinical situations involve the need to use various combinations of the aforementioned five choices. The treatment then becomes interdisciplinary in nature and proper coordination of information becomes critical. All members of a restorative team must understand the end point of the functional relationship. Completion of treatment must meet the requirements outlined in the requirements for occlusal stability.
Case One
This patient presented with a distal-incisal fracture on tooth No. 7. Upon review of the patient’s dental history, it was discovered that fracture of this tooth had become a chronic issue. It had broken and been restored numerous times over the past few years. Frustration with lack of the restoration longevity had led her to seek another care provider.
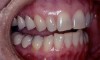
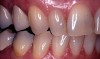
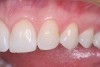
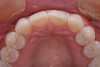
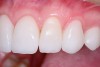
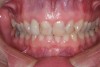
On examination, it was discovered that tooth No. 27 was severely worn and that this lack of contour was causing occlusal instability (Figure 3). In a lateral excursive movement (right working side movement) the lateral incisor was becoming the guiding anterior tooth (Figure 4). Tooth No. 7, however, does not have the proper lingual contour to allow posterior disclusion in an excursive movement. This lack of posterior disclusion allows the continuous posterior tooth contact that leads to activation of the elevator muscles. Excessive occlusal forces on tooth No. 7 led to repeated fracturing of the composite restorations.
At this point, patient education became critical. Success in dentistry can only occur when a patient takes ownership of their situation and is committed to an outcome. At the initial visit, the broken incisal edge of the lateral was restored. However, it was clearly explained to the patient that the underlying cause of the failures was still present and that this deficiency would result in another restorative failure if it was not properly addressed.
Treatment for this patient began with evaluation of the patient’s joint position. It was determined that the patient had a centric relation/maximum intercuspation discrepancy. Occlusal equilibration (coronoplasty) allowed establishment of stable, even holding contacts with the condyles in centric relation.
To allow immediate disclusion and non-interference of posterior teeth in lateral movements, the worn canine had to be restored to normal physiologic contours (additive reshaping). This was accomplished by preparing the tooth to be restored for a thin veneer. This restoration could be fabricated from porcelain or a resin material. To minimize the wear on the opposing tooth, the material that was selected in this case was Belleglass (now marketed as Premise Indirect) (Kerr Dental Corporation, www.kerrdental.com), a laboratory-processed indirect resin material (Figure 5). This material offered the advantages of low abrasiveness against the opposing dentition and excellent esthetics. NX3 Nexus Third Generation (Kerr) resin cement was used in combination with a total-etch technique and fourth-generation bonding agent.
The end result was an esthetic and functionally contoured restoration in harmony with the patient’s envelope of function. And, most importantly, this functional solution has lasted the test of time. Figure 5 is a 90-month follow-up, which shows no loss of contour or de-bonding and no failure of the bonding of tooth No. 7 during this period.
Case Two
This patient wanted to know more about improving her smile (Figure 6). She had always felt like her smile never looked quite right after she had orthodontics as a teenager. A smile with better proportion, contours, and whiter color was her goal.
The treatment-planning phase began with an examination of her current functional situation and an evaluation of signs of occlusal instability. The patient was suffering from muscular symptoms including temporal tension headaches and elevator muscle soreness and hypertrophy. Doppler auscultation, physical examination, oral history, and joint-loading testing were performed. The patient’s joints proved to be stable and in restorable condition. Examination of the teeth showed numerous signs of occlusal instability, including tooth mobility, excessive wear of the posterior teeth, and development of abfractions.
The origin of the patient’s esthetic concerns and functional issues proved to be the same: the patient was congenitally missing her lateral incisors. The solution for this esthetic deficit during her adolescent years was to move the canines into the position of the lateral incisors and then recontour (flatten the incisal edge) to make it look like a lateral. The premolars were then moved mesially into the canine position (Figure 7). The end result was a solution that closed an edentulous space, yet left a functional deficit. The premolars lacked the proper contour to allow immediate posterior disclusion in an excursive movement (Figure 8). After many years, this functional deficit led to the previously described signs of instability.
Further orthodontic intervention was declined by the patient. Therefore, to meet the patient’s esthetics goals and the necessary functional requirements, a restorative option of stacked porcelain veneers was pursued. During the treatment-planning phase of the restorative process, a diagnostic wax-up was created to allow the buccal cusps of the premolar to mimic the contour of a canine. This allowed immediate posterior disclusion, which decreased the activity of the elevator muscles. Bis-acrylic temporary restorations (Fill-In, Kerr) were created off the diagnostic wax-up, thus allowing a period to test the new anterior guidance (Figure 9). After approximately 6 weeks of the patient testing of the new functional contours, impressions of the provisional restorations were taken. Stents were then made from these models to allow duplication of the provisional contours in the porcelain restorations (Figure 10 and Figure 11).
Case Three
Patients often become concerned about the long-term viably of their teeth due to failing restorations. This patient was unhappy with the esthetics of her smile due to failing restorations and color. Unfortunately the patient’s anterior guidance was less than ideal due to her current tooth position. The axial inclination of her premolars was biased to the lingual. This tipping of the buccal cusps meant that in an excursive movement, the posterior teeth could not disclude. In addition, the canine teeth were rotated, leaving a deficit of needed contour (Figure 12).
The patient’s 10 anterior teeth all had failing restorations and decay discovered during clinical and radiologic examination. During a diagnostic work-up, it was determined that minor contour changes in the final restorations would allow proper canine guidance and idealized lingual anatomy. A wax-up was created to determine ideal incisal positions (Figure 13), which were then transferred to the mouth in provisionals (Fill-in, Kerr) (Figure 14 through Figure 16). The small contour changes in the restorations allowed proper anterior guidance to be established.
Conclusion
In conclusion, the long-term health of our patients must be considered. Many times the focus of care is lopsided toward addressing only bacterial concerns (caries and periodontal disease). However, proper occlusal stability must always be considered. In addition to a repeatable joint position, anterior guidance is a cornerstone of long-term function and success. And, many times, improvements can be made whether one is restoring teeth or moving them into better positions.
References
1. Dawson P. Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2006:347.
2. Dawson P. Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2006:57-69.
3. Hess L. The relevance of occlusion in the golden age of esthetics. Inside Dentistry. 2008;4(2):36-44
4. Okano N, Baba K, Igarashi Y. Influence of altered occlusal guidance on masticatory muscle activity during clenching. J Oral Rehabil. 2007;34(9):679-684.
5. Williamson EH, Ludquist DO. Anterior guidance: its effect on electromyographic activity of the temporal and masseter muscles. J Pros Dent. 1983;49(6):816-823.
6. Manns A, Chan C, Miralles R. Influence of group function and canine guidance on electromyographic activity of elevator muscles. J Prosth Dent. 1987;57(4):494-501.
7. Shinogaya T, Kimura M, Matsumoto M. Effects of occlusal contact on the level of mandibular elevator muscle activity during maximal clenching in lateral positions. J Med Dent Sci. 1997;44(4):105-112.
8. Mansour R, Reynik R. In vivo occlusal forces and moments. J Dent Res. 1975:54(1):114-119.
9. Burak N, Kaidonis JA. Experimental studies of human dentin wear. Arch Oral Biology. 1999; 44(10):885-887.
10. Dawson P. Functional Occlusion: From TMJ to Smile Design. St. Louis, Mo: Mosby; 2006:358-359.
About the Author
Leonard A. Hess, DDS, Private Practice Monroe, North Carolina, Associate Faculty, Dawson Academy