You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Minimally invasive dentistry (MID) has become a buzz phrase in dentistry within the past decade. We hear the term and would all like to think that MID is what we’re doing in our own practices. But what exactly is MID? It is a broad term that can encompass all areas of general and specialty dental practices. Concisely, it is the practice of treating dental disease in a conservative fashion based on the best scientific evidence available. Whether it is caries, loss of tooth structure, pulpal or periodontal disease, or tooth alignment, MID refers to the practice of providing dental therapies in the most conservative, least invasive fashion.
Christensen recently discussed MID and the many possible dental therapy alternatives available using a conservative practice theory.1 He presented an extensive, yet incomplete list of MID alternatives for different dental therapies; an all-inclusive list would require a textbook, not a journal article.He did mention many common examples of MID therapy, however, that can be used daily in a general practice in place of “typical” therapies currently provided, and the article should be recommended reading.
One of the reasons MID has become so popular is the dramatic improvement in how we find disease, and the materials/techniques we can use to treat dental disease. Nowhere in dentistry is this more evident than in the treatment of dental caries. Murdoch-Kinch and McLean recently published an in-depth article that addresses the use of MID concepts for the treatment of dental decay.2 Advances in digital radiography, laser detection, and caries detecting dyes all provide dentists with an opportunity to better visualize decay earlier and more efficiently. Early detection allows dentists to attempt to use remineralization therapies,2 or if slightly more advanced, very precise surgical methods can be used to remove the decay. The use of microscopes, air-abrasion, lasers, and/or extremely small burs allow the dentist to minimize the amount of healthy tooth removed and focus only on removal of the diseased tissue. The mainstream acceptance of the clinical success of adhesive dentistry certainly has impacted MID restorative dentistry. Because of the proven success of adhesive dental procedures, no longer do we need to create cavity preparations that need to have required mechanical retention built into the preparation design. This alone has allowed the dental profession to become more conservative in nature.
A common dental treatment that all dentists focusing on MID should revisit is the posterior crown. Christensen,1,3,4 Jackson,5 and many others have promoted the use of onlay restorations in place of the more traditional full-coverage crown. All too often in the dental practice a full-coverage crown is placed on a posterior tooth that has had a single cusp compromised or fractured. Although a crown is an appropriate treatment option, it often may not be the most conservative treatment option for a particular tooth. A dentist with an MID mindset needs to look at each tooth individually and determine if adequate function can be restored by placing onlays on the cusps that are compromised. The advent of adhesive dentistry has provided the profession with the opportunity to provide a tooth-colored solution with onlay restorations. Dentists can bond to place a ceramic or indirect composite restoration which will return not only the function of the tooth, but the esthetics as well. However, dentists should always remember to provide the patient with the option of gold for an onlay as well, because even today gold is still a superior restorative material.4,5
An MID approach is even more important in esthetic dentistry. Patients who present with healthy teeth but are looking for esthetic therapies are even more of an esthetic challenge, especially in today’s cosmetically aware dental population. Drs Christensen,6 Heymann, Swift,7 and many others have published concerns over the dramatic removal of healthy tooth structure for the sole purpose of cosmetic enhancement.
Within the realm of MID, orthodontic treatment is often an excellent alternative for the correction of many esthetic issues. Unfortunately, many adults will not accept this treatment choice. Even so, the MID-minded dentist will certainly provide this treatment alternative, discuss the risks/benefits, and document that it was presented as an option.
There are often times, however, when orthodontic treatment cannot provide the desired results. Additionally, we do need to provide options for patients who do not choose the orthodontic option. Modern dentistry is again benefitting greatly with the success of adhesive dentistry. The use of bonded composites and ceramics provide today’s practitioner with many conservative options for esthetic change.
Many small, minor esthetic changes can be made using direct composite resin. Although a veneer is a conservative treatment option in some situations, too often dentists will immediately recommend a porcelain veneer when a direct resin restoration would provide the esthetic and/or functional solution. Recent advances in composite resin esthetics and physical properties have made composites esthetically competitive to porcelain in many clinical situations. So a dentist with an MID mindset should always look to see if a direct resin alternative will meet a patient’s needs.
Certainly in our cosmetically aware society, porcelain veneers have gained a lot of popularity. But there does exist the potential for abuse with this dental restoration.6,7 However, for many patients it can be an esthetic solution that addresses their concerns and it can be provided in a very conservative fashion.8-10 When properly designed and using the appropriate materials, porcelain veneers can be a minimally invasive option for the esthetically driven patient.
Most recently, in cosmetic dental procedures the idea of “no-prep” veneers certainly bridges into the concept of MID. Although a subject of much debate within the profession, Wells, Radz, and several others10-13 have published clinical cases where “no-prep” veneers have produced a highly esthetic outcome with no preparation of tooth structure. Although not appropriate for all clinical situations, the no-prep concept certainly should be in the cosmetic “tool box” of dentists who focus on MID.
The following cases are just a few clinical examples of how MID can be provided for our patients. It is certainly not all-inclusive, but hopefully will stimulate the reader to begin looking closer at how they can better provide and widen the scope of MID procedures that they offer.
Case 1
Modern dental technology has provided us with new diagnostic tools that give us the ability to provide better, more conservative dentistry. The introduction of a laser fluorescence-measuring device, Diagnodent (Kavo, www.kavo.com) allows for the ability to detect small carious lesions in a very early stage. The Diagnodent has demonstrated an ability to find caries that is superior to traditional caries detection methods.14
Early detection of these small lesions has challenged dentists to find more conservative, less invasive techniques to eliminate them with minimal removal of unaffected tooth structure. Some dentists have used hard/soft tissue lasers to remove carious lesions. Other dentists have used specially created small burs to create very small preparations that allow for minimal removal of tooth structure.
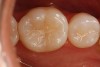
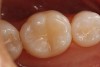
Another preparation technique is the use of air abrasion to remove the area of decay. Figure 1 shows tooth No. 19 with a sealant restoration. Using the Diagnodent, recurrent decay was detected. An air abrasion system was used to remove the old sealant restoration as well as the recurrent decay without the need for local anesthetic (Figure 2). The use of air abrasion allows for the efficient removal of the old resin material as well as the removal of the carious tooth structure.
The tooth was then restored with a flowable composite (Premise™ Flowable, Kerr Corporation, www.kerrdental.com). Care must be taken in the choice of a flowable composite as a restorative material. CRA listed flowable composite as a restorative material option for a Class I restoration,15 yet in 2003 Dr. Christensen stated that care should be taken when issues of occlusal wear may be a concern.16 Flowable composites are basically watered down conventional composites with less filler particles; therefore, they will be less wear resistant. Care and caution should be used when deciding to use a flowable composite as a restorative material for a Class I or II restoration.16
In the clinical case shown, the occlusal contacts were checked before the preparation was started. It was determined that there would be no occlusal contacts in the areas to be prepared, so the restorative flowable material would not be subject to direct occlusal wear. The very narrow and slightly deep nature of the preparation and the absence of occlusal contacts create a situation that is well suited for a flowable composite. Flowable composite, because of its viscosity, allows for it to easily flow and adapt to the narrow preparation, ensuring an absence of voids and excellent adaptation to the preparation. When properly placed, finishing should be minimal.
Figure 3 shows the final conservative, esthetic restoration.
Case 2
Today’s dental practice has seen an increasing number of patients looking for esthetic improvement. Dr. Heymann and others17,18 have expressed concern over the preparation of healthy tooth structure for the sake of purely esthetic change. Certainly this is a valid concern worthy of discussion far beyond the scope of this article.
When dealing with requests from patients for esthetic change, it is important that the dentist looks for the most conservative alternatives. Then the patient should be informed about the risks and benefits associated with these options.
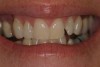
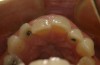
A 45-year-old female presented with a request to improve the appearance of her smile (Figure 4). An occlusal view gives a better perspective of the nature of her esthetic concerns (Figure 5). A discussion of the patient’s expectations and budget led to the presentation of two. The first option was to replace the old Class III composite in tooth No. 10 and engage a course of short-term, limited orthodontics. The second option was to place direct bonded veneers on teeth Nos. 9 and 10. After being instructed in the risks and benefits of each option, the patient chose to resolve her esthetic concerns with direct bonded restorations.
Figure 5 shows that tooth No. 9 is in a lingual version. Because of this position it would be possible to restore this tooth with a noninvasive, no-preparation restoration. Tooth No. 10 would require a minimal amount of preparation. The mesial incisal corner of tooth No. 10 is slightly outside the arch form. Using no anesthetic, an enamelplasty was performed to bring this corner of the tooth back into the arch form.
The teeth were then etched and a fifth-generation bonding agent (OptiBond Solo Plus™, Kerr Corporation) was placed. Current literature demonstrates that etch-and-rinse adhesives provide the strongest bond to an enamel surface.19 Next, a layer of A1 microhybrid composite (Premise) is placed. A final outer layer in a translucent shade was placed. This final layer of clear composite would mimic the optics of natural enamel and allow for a more natural and vital-looking restoration.
Figure 6 is a 1-week postoperative photograph of the direct bonded veneers on teeth Nos. 9 and 10. This final result achieves the goals of MID. Virtually no tooth structure was removed and the patient received an esthetic result that met her goals.
Case 3
All too often, dentists look at posterior teeth with large, failing restorations and immediately recommend a crown as the restorative solution. Certainly in many cases this is a good treatment option that will meet the functional requirements for that tooth and that patient. However, there may often be a more conservative option available that will also meet the functional goals but will require less tooth reduction. In the author’s experience, an onlay restoration can frequently be a less invasive than a crown.
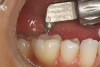
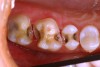
Figure 7 demonstrates a quadrant of old amalgam restorations present on a 32-year-old patient. Clinically, teeth Nos. 2 and 3 tested positive for cuspal fracture. Teeth Nos. 3 through 5 had radiographic evidence of recurrent decay. Each of these teeth had numerous treatment options. A case could be made for all four posterior teeth to be restored with crowns, and this certainly was one treatment option. However, with this young patient every effort was made to minimize the loss of tooth structure while still providing the functional restoration required to provide protection of the tooth and return each tooth to proper health and function while meeting the patient’s esthetic requests.
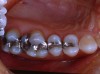
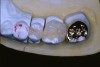
Figure 8 shows the preparations. It was determined that with this quadrant of teeth that No. 5 could be restored with a direct Class II composite (Premise). Tooth No. 4 was a little more involved and because the molars were going to have to be restored indirectly, it was decided to restore this tooth with an inlay. Teeth Nos. 2 and 3 had solid, strong, uninvolved buccal cusps. The functional lingual cusps that tested positive for fracture were the only cusps that required full-coverage protection. Therefore, an onlay design provided the protection required, yet allowed for a dramatic reduction in the amount of healthy tooth structure that needed to be removed.
Tooth No. 2 was restored with a gold onlay. However, the patient’s esthetic requirements dictated the use of tooth-colored material for the indirect restorations on teeth Nos. 3 and 4. Indirect composite has proven to be an excellent restorative material20,21 and was the material chosen for the final restorations. Figure 9 shows the final laboratory work with the gold onlay on tooth No. 2, and the indirect composite (belleGlass HP [now Premise Indirect], Kerr Corporation) inlay and onlay.
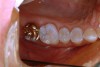
The gold onlay was cemented to place using a self-etching resin cement (Maxcem Elite™, Kerr Corporation). Self-etch cements have demonstrated less postoperative sensitivity, are less technique-sensitive, and will bond to the tooth structure and the restorations.22 The indirect composite inlay and onlay were cemented to place using a total-etch technique and a dual-cure resin cement (NX3 Nexus® Third Generation, Kerr Corporation) using a rubber dam. The final result is functionally durable and esthetic (Figure 10).
Onlay restorations are an excellent option for structurally compromised posterior teeth. Often an onlay can be used to replace a single fractured cusp and conservatively restore strength and function to a posterior tooth. The onlay is a very versatile restoration. Dentists looking for minimally invasive options should consider onlays.
Case 4
Nowhere is minimally invasive dentistry more important than in elective, esthetic dentistry. Removal of healthy tooth structure purely for the improvement of esthetic appearance can be an ethical dilemma for any dentist. The increasing popularity of smile enhancements using porcelain veneers has pushed many dentists to try to find the most minimally invasive techniques and materials possible to provide patients with the esthetic results.
Den-Mat LUMINEERS™ have brought much attention to the concept of “no-prep” veneers. More recently, the work of Wells and Willes and their DURAthin® concept have taken the “no-prep” idea to an even higher artistic level.
The idea of not preparing tooth structure and still being able to achieve the desired esthetic result has a lot of appeal to the conservative dentist. However, doubts exist in the dental industry with concerns for soft-tissue health, proper contours, and overall esthetic quality when it comes to “no-prep” veneers.
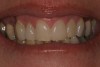
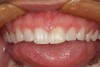
A 24-year-old female presented for esthetic solutions for her smile. Her chief complaints were that her teeth were short, the edges were uneven, and she wanted a whiter overall appearance (Figure 11).
To achieve the patient’s esthetic goals, the following treatment plan was suggested: Gingivectomy to increase the length of the existing maxillary anterior teeth, take-home bleaching, and 10 no-preparation porcelain veneers. Using a diode laser, a gingivectomy procedure was performed on the maxillary anterior teeth. Figure 12 shows the postoperative result at 4 weeks. A subtle, but noticeable increase in clinical crown length was achieved. A full-arch impression was taken using a polyvinylsiloxane impression material (Take 1® Advanced, Kerr Corporation), along with an opposing impression (AlgiNot™, Kerr Corporation), and a bite registration. These, along with digital photographs and the laboratory prescription, were sent to the laboratory.
The porcelain restorations were fabricated with a new Lucite-reinforced ceramic (IPS e.max®, Ivoclar Vivadent, www.ivoclarvivadent.com). The newest HT (high translucency) e.max ingots can be pressed to 0.3-mm thick. This allows for the ceramist to fabricate veneers that have a very natural appearance and no negative effect on the soft tissue.
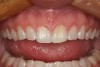
At the delivery appointment, after the veneers were tried in and approved by the patient, they were cemented to place. A total-etch technique (OptiBond Solo Plus) and light-cure resin cement (NX3) were used to place the veneers. Figure 13 shows a 4-month postoperative photograph of the final veneers. The final result demonstrates a very natural appearance. The restorations are not bulky or overcontoured, and the soft tissue has a healthy appearance.
This case demonstrates that with proper case selection and excellent ceramics, it is possible to provide a non-invasive esthetic alternative to the patient seeking elective care.
Conclusion
All dentists should treatment plan their patients using minimally invasive concepts. The preservation of tooth structure is more important now than ever before given that the patient population is living longer and therefore keeping their teeth longer. Any treatment we do today will have long-lasting implications for that patient. Recent advances in dentistry allow us to provide many conservative options. We need to be aware of these options so that we consistently give our patients the best dentistry has to offer.
Acknowledgments
All of the indirect cases shown were created by the ceramists at the Dental Arts Lab Signature division (Peoria, IL).
References
1. Christensen GJ. The advantages of minimally invasive dentistry. J Am Dent Assoc. 2005;136: 1563-1567.
2. Murdoch-Kinch CA, McLean ME. Minimally invasive dentistry. J Am Dent Assoc. 2003;134:87-95.
3. Christensen GJ. Has tooth structure been replaced? J Am Dent Assoc. 2002;133:103-105.
4. Christensen GJ. Considering tooth-colored inlays and onlays versus crowns. J Am Dent Assoc. 2008;139:617-619.
5. Jackson RD. A technique for placing multiple esthetic inlays and onlays. Compend Contin Educ Dent. 1995;17(10):918-924.
6. Christensen GJ. Veneer mania. J Am Dent Assoc. 2006;137:1161-1163.
7. Heymann HO, Swift EJ Jr. Is tooth structure not sacred anymore? J Esthet Restor Dent.2001;13(5):283.
8. Christensen GJ. What is a veneer? J Am Dent Assoc. 2004;135:1574-1576.
9. Nash RW. Extreme dental makeovers without extreme tooth reduction. Dental Products Report. 2005:58-60.
10. Radz GM. Elective veneers: Meeting patient’s expectations while addressing current ethical questions of elective care. Inside Dentistry. 2008;4(3):48-52.
11. Wells DJ. Don’t we all do cosmetic dentistry? Dental Economics. 2007;106-108,138.
12. Radz GM. Enhancing the esthetics through addition: no-prep porcelain veneers, case studies. Oral Health. 2009:23-30.
13. DiMatteo AM. Prep vs. no prep: The evolution of veneers. Inside Dentistry. 2009;5(6):72-79.
14. Ouellet A, Hondrum S, Pietz D. Detection of occlusal carious lesions. Gen Dent. 2002;50(4):346-350.
15. Direct Tooth Restorations, State of the Art. CRA Newsletter. 1999;April:1-2.
16. Christensen G. Direct restorative materials. What goes where? J Am Dent Assoc. 2003;134(10):1395-1397.
17. Heymann HO, Swift EJ Jr. Is tooth structure not sacred anymore? J Esthet Restor Dent. 2001;13(5):283.
18. Radz G. Elective veneers: meeting patients’ expectations while addressing current ethical questions of elective care. Inside Dentistry. 2008;4(3):48-52.
19. Strassler H, Sensi LG. Applications of etch-and-rinse adhesive bonding for esthetic restorative dentistry. Functional Esthetics & Restorative Dentistry. 2008;2(1):26-33.
20. Donly KJ, Jensen M, Triolo PT, et al. A clinical comparison of resin composite inlay and onlay posterior restorations and cast gold restorations at 7 years. Quintessence Int. 1999;30(3):163-168.
21. van Dijken JWV, Horsteadt P. Marginal breakdown of 5 year old composite inlays. J Dent. 1996;24(6):389-394.
22. Powers JM. Self-adhesive resin cements: characteristics, properties, and manipulation. Functional Esthetics & Restorative Dentistry. 2008;2(1):34-36.