You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Much has been written over the years on the importance of effective communication between patients and the staff of the dental practice. However, despite the extensive literature on the topic, the need for effective communication and the skills necessary for facilitating such communication have generally been discussed in the context of the concerns of the dental practice. Improved communication between patient and dental staff can often be considered a means to an end: sometimes it is discussed in terms of growing the dental practice and increasing revenue, by its direct impact on appointments booked and kept; other times it is considered a vehicle for efficiency, by minimizing misunderstandings; still other times it is seen as a means of building trust and rapport, which enhances the overall patient experience and thus results in greater retention of patients for the practice and increased patient referrals. All of these are important, worthwhile goals and are beneficial to patients and dental professionals alike.
Yet there is another, preeminent reason for improving communication between patients and dental professionals, and in particular, cultivating patient-centered communication: that is the care of the patient, and the moral imperative for providing this care. Although clinicians are inclined to think of patient care as consisting of the alleviation of physical pain and illness, patient care can take many forms, including addressing the socio-emotional needs of the patient, which has been found to improve patient outcomes.1,2According to the Institute of Medicine, patient-centered care is one of the basic elements of high-quality healthcare.3Thus, complete patient care begins with the socio-emotional care that occurs during communication between the patient and the dental professional, as well as between the patient and the dental office staff.
COMMUNICATION BETWEEN THE PATIENT AND THE FRONT OFFICE STAFF
The members of the front office staff are the initial contacts for patients, so the care of the dental patient truly begins with them. The front office staff handle a myriad of tasks that require expert coordination and strict attention to detail, such as chart generation, patient registration, electronic medical records, answering phones, making appointments, basic accounting and handling of copayments and billing, and assisting with the dental practitioners in the completion of orders to keep patients moving through the system. Indeed, on any given day the front office staff may often be "swamped" with tasks that have little to do with communicating with patients. In such situations, patient interactions may be seen by some misguided staff members as "interruptions" in their work, or as simply another task that must be "fit in" with the others and performed in a quick and efficient manner.4
Given that front office staff face these workload challenges, how does the dental practice promote a change in staff outlook on and approach toward patient-staff communication? Clearly, the approach cannot depend solely on the personal attributes of the employee, eg, whether or not he or she happens to have good manners or a friendly personality. It also cannot be based on the subjective mood of the front desk personnel at any given time, or how busy they may happen to be at the time that the patient walks through the door. Instead, patient-centered communication must be established as a system. Prompt, courteous, and kindly interaction with the patient must be codified as an unbending, non-negotiable policy that every member of the team understands and agrees to abide by. Failure to adhere to this system should be considered equivalent to failing to report to work on time or a failing to take an appropriate radiograph. It should be considered a mandatory duty for front office staff to treat every new patient who enters the office with the utmost kindness and respect.
Research supports the notion that the patients' opinion about a dental office is largely determined by how they are treated by the front desk staff when they first arrive for their appointment.5,6 Front office staff should therefore be coached to develop the ability to greet new patients in a timely fashion while making them feel both welcome and cared for. The following are some simple steps that staff can take to treat new patients in a personable and welcoming manner:
1. Stand up, make eye contact, address the patient by name, and shake their hand (or, as an infection control precaution, wave). Ideally, this ought to be done for all patients, but it must be a requirement for greeting new patients.
2. When appropriate, pay the patient a compliment or thank them for their promptness to the appointment (or their readi- ness in supplying their insurance information, etc).
3. Step out of the front desk domain, and enter the reception area domain. This means that front desk personnel must exit their "comfort zone," walk around the counter, and stand next to the patient, side by side (or if the patient is sitting, take the seat next to him or her). Only while sitting next to the patient should the front desk staff member begin asking about paperwork, insurance cards, and so on.
4. While sitting next to the patient, offer to bring them water, coffee, or tea, provide them with directions to the restroom, or make available any other little comfort item that your office provides.
5. Finally, make it a point to learn something about the pa- tient. When doing so, be careful to devote your atten- tion and interest to the patient, and do not inject yourself (ie, talking about yourself) into the conversation. In order to fight the tendency to talk about yourself, focus on questions you can ask the patient, and ask open-ended questions. These are questions that cannot be answered with a "yes" or a "no." To learn where the patient lives, you might ask if he or she had a short drive to the dental office and ask what town they live in, and how long they have lived there. In the course of these questions, you may end up learn- ing some additional "facts" about the patient, such as where they lived before they moved to the area. So, if a patient says that they grew up in New Mexico, for example, to keep your questions open-ended, avoid asking, "Did you like living there?" and instead ask, "What was it like living there?" Or "How would you compare living there to where you're living now?"
In addition, front office personnel can be instrumental in calming patients who are experiencing dental anxiety. According to one published report,7 for a person prone to dental phobia, anxiety can be triggered even by the encounter with the receptionist or by the clinic's ambience; conversely, staff members who are positive and caring and who elicit information from patients in an unhurried and concerned tone can help allay anxiety.7
At this point, the front office team has made the patient feel welcome, respected, valued, and cared for. It will now be easier for the clinical staff to "pick up where the front office staff left off" and continue the positive and caring interaction with the patient after he or she has been ushered into the examination room or dental operatory (the clinical domain). The patient will also be able to enter the clinical domain with a greater sense of trust.
COMMUNICATION BETWEEN THE PATIENT AND THE CLINICAL STAFF
Once the patient has entered the clinical domain, the first interaction between the patient and the dental healthcare professional should again include learning about the patient with open-ended questions. Patient-centered communication (in contrast to disease-focused communication) includes eliciting the patient's agenda with open-ended questions, particularly during the clini- cian's initial interactions with the patient.3 Thus, open-ended questions should in fact begin the interaction with the patient. Many dental assistants, dental hygienists, and dentists might begin the conversation with the patient by asking, "So, what brings you here today?" or "Are you having any problems I can help you with?" However, the problem with beginning the interaction in this manner is its impersonal quality; in failing to show an interest in the patient as a person and to learn a little about the patient's life beyond the problem that has brought them to the dental office, the clinical staff has missed a valuable opportunity for helping build trust. By attempting to learn something about the patient beyond their oral health status, the clinical staff can help the patient feel cared for and validated as a person.
Obtaining Photographs
While in dental school, students are trained that the only imaging to be provided to patients prior to their comprehensive examination is a full mouth series of radiographs or a panoramic radiograph. However, extra-oral and intra-oral photography are other necessary features of dental imaging, and at the same time are aspects of patient care that demonstrate that extra measures are being undertaken for that patient.
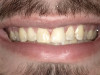
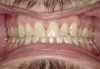
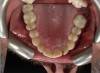
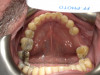
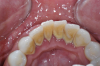
Extra-oral photography. Extra-oral photography is essential for giving patients a full picture of their smile and oral health status. This has been a challenge for most dentists over the past two decades because many cameras that have the capability of taking high-quality, fully focused images of the dental arch have been difficult to use and program and awkward to sterilize. Other dentists have limited their use of such cameras to the occasional cosmetic case. However, extra-oral photography should be provided for every patient. The use of such photography and the type of photographs taken can vary from office to office, depending on the patient flow and the availability and training of personnel at that particular office. Regardless of these variations, however, all dental practices should take the following four extra-oral photos: the close-up smile, the retracted smile, the upper arch, and the lower arch (Figure 1 through Figure 4).
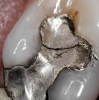
Intra-oral photography. Many dental conditions involve the margins between the natural tooth and the old restoration, which can be difficult to adequately capture with either traditional radi- ography or extra-oral photography. Every operatory should therefore be equipped with a high-quality intra-oral camera; sharing such photographs with the patient during the consultation is quite helpful in explaining the need for longer-term restorations. A well-trained dental hygienist or assistant can quickly and seamlessly integrate several intraoral photographs during the new patient interview (Figure 5 and Figure 6), discussed below.
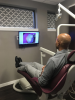
Finally, when taking oral photographs of the patient, make certain that the imaging is always displayed in front of the patient (Figure 7). A common problem with the conventional approach to taking photographs in the examination room or operatory is the tendency to have the viewing box positioned behind the patient. Having the imaging shown directly in front of the patient (a large flat-screen HDMI TV and wall-mount are well-suited to this purpose) assures him or her that they play a major role in the decision making surrounding the comprehensive examination.
The New Patient Interview
In dental school, students are advised to ask patients, early in the course of the clinical interview, about their "chief complaint." While this recommendation may seem entirely pragmatic, it is not necessarily patient-centered, in the sense that it does not assess the patient's feelings about his or her oral health condition. The patient interview is in fact the core clinical interaction in which the value of caring, patient-centered communication is perhaps most evident. Motivational interviewing, a style of counseling originally used in the treatment of individuals with addictions, has increasingly been employed across a broad range of healthcare settings,8,9 and many of its principles and techniques can be adapted to the dental care setting. Motivational interviewing is focused on identifying and mobilizing the patient's intrinsic values and goals to stimulate behavior change, and as such, it has been found to outperform traditional advice-giving in the treatment of a wide variety of diseases, according to a systematic review report.9
The dental practitioner can use this interviewing method to identify an appropriate and mutually agreed upon dental treatment plan with the patient.8,9 The following is an example of how an interview with a new patient can be handled when utilizing the techniques of this method.
First, with select images displayed in front of the patient (eg, a retracted smile photo, some intraoral photos, and the panoramic x-ray), the dental clinician may ask:
"On a scale of 1 to 10, how would you rate your teeth?"
Almost without exception, the patient will answer with a number less than 10. Next, that clinician may ask (question 2):
"So, using the photos in front of you, what do you feel would need to happen in order to make your rating a 10?"
The patient's answer may seem to present a good opportun- ity for the clinician to begin explaining how dentistry can help. Although it may surprise most clinicians-and may even strike many as counterintuitive-this is not how the practitioner should respond to the patient. For example, if the patient replies, "I feel that to rate my teeth a 10, they should be whiter. I do wish they were just a bit whiter," the clinician should not respond by discussing whitening options. Instead, he or she should move on to question 3:
"Why do you feel that way?" or "Why is that important to you?"
This question might seem unnecessary, but it is very possibly the most pivotal question of the patient interview. By asking this question, the clinician has transformed the conversation from one that is "clinical" to one that is "emotional" or "emotionally driven." By offering the patient an opportunity to express their feelings about their teeth, the dental clinician has acknowledged and enhanced the patient's psychological ownership of the problem. The patient now feels vested in their own oral health. The clinician should now move on to question 4:
"What do you think can be done to help [with the problem]?" or "What do you think is the best option moving forward?"
Dental hygienists can also apply these techniques to their role in caring for the patient. At the end of the periodontal examination, for example, at which point the hygienist explains the pocket depths to the patient, the hygienist should ask, "How do you feel about what you just heard?"
It must be emphasized that, throughout the new patient interview, the practitioner should keep his or her focus on a communication style that is thoughtful, empathetic, and caring, and on asking open-ended questions that elicit the patient's feelings and values. The interview technique should also actively avoid "coaching" or "leading" the patient to say what the clinician believes will allow him or her to usher in their treatment advice. Rather, the patient interview is an opportunity for the dental professional to learn what the patient feels are his or her needs and treatment expectations, and is a time for allowing the patient to take command of their own dental future.
COMMUNICATION AT THE HANDOFF
The handoff, a critical transfer point during the patient's visit to the dental office, is essentially the point at which information about and responsibility for the patient are transferred from one staff member to another. As such, the handoff includes communication between care providers about patient care and information tools to assist in the communication.10 Handoffs occur in other areas of ordinary human experience, as well; when "handing off" children to a babysitter, parents will often pass along a verbal (or literal) list of instructions that the babysitter will need to know about the child's traits or needs (eg, "he hasn't eaten lunch yet, so he will be hungry soon"), and it is very seldom that a parent hands off their child without providing any of this information. Unfortunately, patients are often handed off with minimal transfer of information to the next care provider.11 Furthermore, patients today are likely to experience more handoffs than in the past, while poorly managed handoffs can contribute to gaps in patient care and even jeopardize patient safety.10
In the following example of a poorly managed handoff, a patient calls the dental office to schedule an appointment for a broken tooth. She talks to a front desk team member for 5 minutes, describing how unhappy she is that her former dentist has retired, how her tooth does not hurt, but that the remaining cusps feel sharp to her tongue, and so on. When the patient arrives for her appointment, each of the staff members who greet her-the hygienist, the dental assistant, and the dentist-asks, "So what brings you in?" or "How can we help you?" and makes her repeat the same information. Improperly managed handoffs not only cause inefficiencies and potential treatment concerns for the patient, they cause the patient to feel dissatisfied and experience a loss of trust, believing that their dental problem is not being taken seriously.
In a properly executed handoff, each member of the team, in their new interaction with this patient at the point of handoff, is given thorough verbal instructions about the patient and their oral condition, and importantly, this information is given in the presence of the patient.
The following is an example of a properly managed handoff:
Front Desk Team to First Clinical Contact
The front desk team, after having their initial conversation with the patient, summarizes that conversation onto the practice management scheduling software.
The first clinical contact (hygienist or assistant), reads that summary, and begins his or her conversation with the patient as though this information were verbally handed off:
"Hi Mary. I talked to Alyssa, and she told me that you broke your tooth eating popcorn. She also mentioned that it feels kind of sharp to your tongue. Tell me more about this. Were you eating the popcorn at home, or were you at the movies when this happened?"
First Clinical Contact to Dentist
When the dentist enters the operatory, instead of beginning the oral examination, he or she should sit down in a nearby chair, welcome Mary to the office, and ask the first clinical contact:
"So, what did you two talk about?"
Dentist to Financial Coordinator
This last handoff is the one that many offices fail to execute. The handoff of the patient to the financial team should be handled as follows:
"Mary, I want to introduce you to Alyssa. You may have met her when you first called or came in. She is the expert here at making these treatment decisions fit with your schedule and financially. Alyssa, Mary and I have decided to_________ [provide details on the treatment plan]. Could you break this down further for her?"
At the end of every handoff, whether it is from the hygienist to the dentist, or the dentist to the financial coordinator, the handoff should end by addressing the patient with:
"Mary, did I cover all the information? Was there anything that I might have missed?"
There are two major hurdles that most offices encounter when they try to implement consistent handoffs in the presence of the patient:
The first is deciding on the point at which the financial coordinator should be brought back to the operatory. Complex, difficult treatment plans require a great deal of time for the financial coordinator, and the dentist is usually too busy to wait for the financial coordinator to complete his or her assessment of the treatment plan. For this reason, the handoff should be done before the treatment financial details are established. In this scenario, the dentist should introduce the financial coordinator immediately after the examination occurs and the treatment recommendations have been made. After the handoff is established, the financial coordinator can choose where the patient should wait for the treatment plan. Sometimes this can be the operatory, if it is available, a consultation office, or the waiting room.
The second hurdle is ensuring that the conversations take place physically in front of the patient; this can be a challenge when several people are involved and the actual physical space is limited. The log tends to be handled in an area behind the patient, while the charting and storing of instruments and supplies are also located physically behind the patient. As a result, it may seem easiest to talk about or to the patient while standing or sitting behind him or her, forcing the patient to twist back and forth as the conversation progresses. However, this is a distinctly inappropriate way to interact during a handoff. Instead, the clinical team should adopt an interaction style championed by the late Peter Dawson (founder of the The Dawson Academy, a provider of dental continuing education): Eye to Eye, Knee to Knee, Heart to Heart.The patient should be sitting comfortably, facing forward, as the hygienist shares their conversation and findings with the dentist (Figure 8), and the same should occur between the dentist and the financial coordinator. If necessary, a couple of stools should be kept in both corners of every operatory in order to accommodate this approach.
ADJUSTMENTS TO PATIENT INTERACTIONS IN A POST-CORONAVIRUS WORLD
The COVID-19 pandemic has necessitated a variety of adjustments to dental practice operations. Infection control measures have included the use of air purifiers, extra-oral suction equipment, aerosol-reduction controls, and more stringent adherence to air-borne and blood-borne pathogen control standards. Clear plastic barriers have also been put up at the front desk, and masks are used during all patient interactions. To accommodate infection control, additional adjustments to your interactions with the patient may include the following:
1. When a new patient first walks in, the hand shake can be replaced with a simple wave.
2. Because masks obscure face-to-face interaction and inter- fere with the warmth of the interaction, have buttons made with headshots of each of your team members. Those buttons can be attached to the clinical gown.
3. For photography, cameras are available that are specially made to withstand being wiped down with harsh dental disinfectants (eg, the EyeSpecial digital dental camera [Shofu], smartCam [FutuDent], and Rebel T6 with dental kit [Canon]). All intraoral cameras can be used with a physical transparent shield.
REHEARSING PATIENT INTERACTIONS
These communication practices will work best if they are rehearsed by the dental office team members. Staff can try role-playing all stages of these patient interactions: for example, an assistant could pretend that she just broke a tooth, and start the process with the phone call. A dental hygienist could pretend that the patient is frustrated with the gap between his teeth, and start the process with photography. In this way, the entire staff of the dental office-both the front office employees and the clinical staff-can discover potential awkward situations and possible road blocks, and can brainstorm on ways to maneuver through these.
CONCLUSION
Communication between staff and patients should be consistently patient-centered, with a focus on serving as an extension of excellent overall patient care. With this in mind, patient-centered communication cannot be simply a matter of approaching the patient in a friendly and kindly manner. Effective and caring patient interactions must be undertaken in a systematic way by all staff members of the dental office, and the different steps of the system should be codified as policies of the dental practice. All stages of the patient experience during a dental office visit-beginning with interactions with the front office staff, through handoffs between team members, the patient interview, and conversations with and about the patient in his or her presence-should be managed as parts of an overall system that every member of the team adheres to as a matter of course. When all team members are committed to this system, complete patient care that begins with addressing socio-emotional needs of the patient is ensured.
About the Author
Ankur Gupta, DDS
North Ridgeville Family Dentistry
North Ridgeville, OH
References
1. Pehrson C, Baerjee SM, Mnna R, et al. Responding empathically to patients: development, implementation, and evaluation of a communication skills training module for oncology nurses. Patient Educ Couns. 2016;99(4):610-616.
2. Sinclair S, Beamer K, Hack TF, et al. Sympathy, empathy, and compassion: a grounded theory study of palliative care patient's understandings, experiences, and preferences. Palliat Med. 2017;31(5):437-447.
3. Hashim MJ. Patient-centered communication: basic skills. Am Fam Physician. 2017;95(1):29-34.
4. Hewitt H, McCloughan L. Front desk talk: discourse analysis of receptionist-patient interaction. Br J Gen Pract.2009;59(565):e260-e266.
5. Premack P. Science says people decide these 12 things within seconds of meeting you. Business Insider.Updated April 24, 2019.
6. Bastemeijer CM, Boosman H, van Ewijk H, Vrweij LM, Voogt L, Hazelzet JA. Patient experiences: a systematic review of quality improvement interventions in a hospital setting. Patient Related Outcome Measures. 2019;10:157-169.
7. Appukuttan DP. Strategies to manage patients with dental anxiety and dental phobia: literature review. Clin Cosmet Investig Dent. 2016;8:35-50.
8. Resnicow K, McMaster F. Motivational Interviewing: moving from why to how with autonomy support. Int J Behav Nutr Phys Act. 2012;9:19.
9. Rubak S. Motivational Interviewing: a systemic review and meta analysis. Br J Gen Pract.2005;55(515):305-312.
10. Friesen M, White SV, Byers JF. Handoffs: implications for nurses. In: Hughes RG, Ed. Patient Safety and Quality: An Evidence-Based Handbook for Nurses. Rockville, MD: Agency for Healthcare Research and Quality; 2008.
11. Rattray N, Flanagan ME, Militello LG, Barach P, Frankel RN. The art of effective handoff communication among medical and surgery residents. Journal of Cognitive Engineering and Decision Making.2021. doi: 10.1177/15553434211018296.