You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The term dental insertion torque refers to the moment of force used to insert an implant into bone.1 This force affects primary stability (mechanical stabilization of the implant), which helps achieve osseointegration.2 Primary stability denotes a lack of implant micromotion (detected with the naked eye). Movement of 100 µm to 150 µm is deleterious to implant osseointegration,3,4 because it induces peri-implant bone remodeling, fibro-encapsulation, and implant loss.3 Thus, selecting an amount of insertion torque to enhance implant stability is an important factor pertaining to achieving predictable osseointegration. However, questions persist related to the effect of insertion torque on various facets of wound healing. Specifically, what is the minimum insertion force needed to attain primary implant stability if the implant is placed into a healed ridge or inserted into a fresh extraction socket prior to immediate loading? What forces do clinicians routinely use in these situations? Does increasing the insertion torque reduce micromotion and enhance an implant’s primary stability? What level of increased force during implant placement is detrimental to bone? Does the magnitude of initial insertion torque make a difference concerning implant stability several months after insertion? This article addresses these questions and provides background information relevant to this subject.
Search Method
The literature was searched via PubMed using the following terms: insertion torque, implant insertion torque, minimum insertion torque, primary stability of an implant, implant stability, immediate loading, bone-to-implant contact, and implant surface modifications; reference lists of articles were searched for pertinent studies. Clinical trials were excluded that did not clearly state research protocols. The search was completed on January 5, 2016.
Primary vs Secondary Stability of Implants
Primary stability (mechanical stabilization) is attained when an implant is seated in bone and demonstrates no visible movement when forces are applied to it.2,5,6 Factors affecting firmness include bone density (quality), percentage of initial bone–implant interface, bone quality and dimensions, implant geometry, surface micromorphology, magnitude of insertion torque, and surgical technique used when creating an osteotomy.7-15 In contrast, secondary stability (biological stability) occurs when new bone is formed along the implant interface.7 Bone deposition results in biological anchorage of the implant, and this is synonymous with osseointegration.16
Negative Effect of Micromotion
The strain theory indicates that fractured bones should be fixated to ensure there is no shifting between secured sections.17 Displacement of osseous segments could destroy new cells and blood vessels that form in the gap between bones.17 Subsequently, osteoclasts resorb the adjacent bone and micromotion increases, resulting in failed fracture healing.18 This failure pattern can occur after dental implants are inserted if primary stability is not attained.7 From another perspective, Sivolella et al19 demonstrated that insertion torque is not the critical determinant in obtaining osseointegration; rather, it is the absence of micromotion. They placed implants into created osteotomies (in dogs) that were larger than the implants. Passive fixation plates were used to stabilize the implants, ensuring they did not touch bone. All implants integrated successfully. These findings underscore the importance of achieving primary stability to preclude micromotion.
Devices to Assess Primary Stability of Implants
Two instruments are frequently used in studies to evaluate implant stability: Periotest® (Medizintechnik Gulden, med-gulden.com) and Osstell® (Osstell, osstell.com) devices.20,21 The Periotest instrument contains an electronically driven tapping head that percusses the healing abutment on its buccal aspect. The handpiece utilizes a microcomputer to detect the time it takes for the tapping head to return to its original position. It records findings ranging from -8 to +50 (least stable).20 The Osstell unit functions differently. A sensor is positioned on an implant and stimulated to vibrate with magnetic pulses provided by an Osstell handpiece, which also evaluates the frequency at which the implant vibrates. A high level of vibration correlates with a firmer implant (resonance frequency is measured between 3500 Hz to 8500 Hz). This technique is referred to as resonance frequency analysis (RFA), and recorded frequencies are translated into a user-friendly implant stability quotient (ISQ), in which units range from 1 to 100 (most stable).20 Investigators often employ a threshold score of 65.5 ISQ to indicate whether adequate primary implant stability was achieved.22 Other thresholds have also been used (eg, 56 ISQ).23 However, the European Academy of Osseointegration consensus conference in 2006 concluded there is no justification for normal use of these devices, because their recorded range of values pertaining to success or implant failure is unclear.24
From a practical standpoint, at the time of implant placement, insertion torque can be measured by the drilling unit or manual mechanical torque measuring instruments (Figure 1 and Figure 2). When the implant “locks in,” it is interpreted to indicate primary stability has been attained.
Correlations of Insertion Torque to Other Parameters
Insertion torque assessments have been correlated to various parameters pertaining to implant stability. Trisi et al2 found that RFA (ISQ) was not related to the amount of bone–implant contact (BIC) or removal torque values. Others also noted that ISQ did not correspond to insertion torque5 or BIC.25 In contrast, some investigators reported that ISQ values reflected insertion torque forces.26,27 However, Norton28 cautioned there could be a poor correlation between ISQ and insertion stability. For instance, implants inserted with either 30 Ncm or 100 Ncm could be extremely stable and have the same ISQ. Regarding bone density, researchers observed there was a relationship between insertion torque and bone quality and concluded that greater primary stability can be achieved in denser bone with increased insertion torque.29-33 It also was suggested that because there was a positive correlation between bone density (assessed on a computed tomography scan and measured in Hounsfield units) and torque values that initial bone density assessments could help predict required initial torque values to achieve primary stability.34
Chronologic Fluctuations of Stability
The degree of primary stability usually decreases several weeks after implant placement due to bone remodeling; this is referred to as a dip in stability35,36 and is caused by injury to bone when an osteotomy is developed.37 Subsequently, implant stability will increase because of bone apposition and maturation (osseointegration).38 The concept that stability is reduced several weeks after implant insertion and then increases is supported by reports that demonstrate a reduction of ISQ several weeks after implant placement followed by an increase of ISQ.9,36-38 Additional corroboration for this phenomenon was provided by investigators who found that reduced reverse torque values were needed to remove implants after their placement, followed by the need for increased forces after further healing.1,39 For instance, Wilke et al39 reported that after inserting implants into sheep tibia with an insertion force of 100 Ncm, their removal force after 2 weeks was 84 Ncm to 88 Ncm and increased to 200 Ncm after 2 months. Therefore, during the transition period from primary to secondary stability, activities such as changing a healing abutment should be approached with caution.
Notably, some study results did not demonstrate a dip in stability several weeks after implant placement.35,38,40 This was attributed to differences in implant surface properties (such as fluoride- or alkali-treated surfaces).35,41 A dip may not have been observed because of accelerated development of biologic stability that compensated for a reduction of mechanical stability.38 Numerous papers have addressed the finding that implant-surface modifications may accelerate healing events such as those noted above.42 However, bioactive surfaces do not appear to provide superior final osseointegration when compared with textured implants.43
Amount of Force Needed to Attain Stability
Insertion torque is considered an objective surrogate measure for primary implant stability.44 Therefore, clarification regarding what torque force should be used in various scenarios (eg, healed ridges, immediate loading of implants in fresh extraction sockets) would be beneficial.
The lowest insertion torque that could be used to attain primary stability of an implant in a healed ridge has never been established.22,45 In that regard, when Trisi et al1 compared the effect of low (10 Ncm) versus high (110 Ncm) insertion torques in sheep mandibles, implants inserted with low insertion torque demonstrated increased stability after 6 weeks compared with implants inserted with high insertion torque. At that time point, biologic findings for the respective two insertion torques (10 Ncm versus 110 Ncm) were reported as follows: ISQ – 69.25 versus 68.25; torque removal values – 40 Ncm versus 61.33 Ncm; and percentage of BIC – 44.9% versus 50.29%.
The insertion torque used to place implants into healed ridges varies depending on the quality of the bone, implant shape, implant surface, and method of osteotomy preparation.7-15 Relevantly, a recent systematic review by Benic et al46 found that the usual insertion torque clinicians use varies between 20 Ncm to 45 Ncm. Different initial torque forces used successfully in healed ridges are listed in Table 1.5,27,46-50 In summary, a precise torque force that should be routinely used to insert an implant into a healed ridge has never been defined. Nevertheless, the literature indicates that clinicians successfully use insertion torques of ≥30 Ncm.5,27,46-49 This, however, may vary among individuals and sites within the same mouth.
Torque Levels Required for Immediate Loading
The term immediate loading denotes that a prosthesis is connected to an implant within 1 week of implant placement.51 Conceptually, a strong insertion force is desired to stabilize an implant that is placed into a fresh extraction socket. This is particularly true if the implant is going to be immediately loaded, because an osteotomy may not provide osseous support circumferentially around the implant, and in function it may need additional stability to avoid micromotion.
Several systematic reviews stated that the minimum force used to place implants in preparation for immediate provisionalization or loading of implants in edentulous patients was ≥30 Ncm51 or ≥35 Ncm,52 and in partially edentulous patients ≥30 Ncm (range of 15 Ncm to 45 Ncm).53 In another study that related insertion torque to implant failure rates conducted by Ottoni et al,54 the authors demonstrated successful integration of implants that were immediately loaded after using an initial insertion torque of ≥32 Ncm, whereas implants placed with a reduced insertion force (20 Ncm) often failed (9 of 10 patients). In contrast, other clinical trials indicated that immediately loaded implants had relatively high survival rates despite low insertion torques used to place the implants.50,55-58 Several authors suggested that if low insertion forces are used to insert implants, the implants should be splinted together to provide greater stability.50,55,56
Does Raising Insertion Torque Increase Primary Implant Stability?
Poor initial stability is a significant cause of implant failure.59 Therefore, numerous investigators recommended using increased insertion torque to enhance primary stability.7,14,54,60 To test this hypothesis, Trisi et al7 placed 120 implants in bovine bone that was described as soft, normal, and hard. Forces of 20 Ncm, 35 Ncm, 45 Ncm, 70 Ncm, and 100 Ncm were used to insert implants. The authors demonstrated that increasing the peak insertion force reduced micromotion and there was more micromovement in soft than in dense bone. However, after a force of 45 Ncm was reached, variations in the amount of micromotion regarding dissimilar forces were not significantly different.
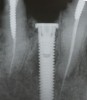
Subsequently, Trisi et al2 confirmed that increased insertion torque reduced implant micromotion when the implants were subjected to lateral forces in vitro (bovine bone). However, it was noted that this relationship may not always be true for all implant designs (Figure 3) and drilling techniques.61 For instance, compared with soft bone, there may be no benefit in increasing insertion torque in dense bone after stability is attained. One can surmise that a moderate increase of insertion torque may provide some benefits with respect to reducing micromotion, especially in less dense bone. However, the amount of increased force that is beneficial is unclear. Another technique to enhance initial stability is to use tapered implants, which develop elevated insertion torque forces. 14,62
Consequences of Excessive Insertion Torque
Historically, it has been presumed that high insertion torques (40 Ncm to 45 Ncm) distort and compress bone, thereby reducing microcirculation.1 Conceptually, this induced bone necrosis and precluded implant osseointegration.14,63 However, this concept has not been validated. To elucidate the association between excessive bone compression and osseous resorption, Trisi et al1 evaluated the bone’s reaction to low and high insertion torques in sheep mandibles. They concluded that high insertion torque (up to 150 Ncm) did not induce bone necrosis or implant failure. Similarly, Consolo et al60 compared the effects of inserting implants into two groups of sheep using a mean torque of 24 Ncm in one group and 105.6 Ncm in the other and reported that high insertion torque did not induce osseous resorption or loss of implants. However, elevated insertion forces did create more microcracks, though these usually repaired within 4 weeks after implant insertion. These investigations were conducted in animals, and the data cannot be extrapolated directly to humans. However, when Khayat et al45 placed dental implants in patients using a high insertion torque of ≥70 Ncm (up to 176 Ncm), they found it did not prevent osseointegration or cause greater bone loss when matched to a control group whose insertion torque ranged from 30 Ncm to 50 Ncm.
Recently, a systematic review compared the amount of bone loss that took place after patients experienced ≥50 Ncm insertion torque versus 35-Ncm to 45-Ncm force; the review stated that no significant difference occurred in the amount of bone resorption at different force levels.64 It can be concluded that insertion torque ≥50 Ncm can be used and doing so does not often result in osseous resorption beyond what normally occurs after implant insertion with lesser force.
Causes of Decreased Implant Stability and Corrective Measures
When implants are placed, several factors can contribute to poor implant stability, including poor bone quality, fresh extraction socket morphology, and over-preparation of osteotomies.58 Relevantly, implants inserted with low initial torque values may be “spinners.” This term refers to an implant that fails to engage the lateral walls and rotates when it is fully seated in an osteotomy. Spinners may have lower rates of osseointegration; however, not all spinners are necessarily doomed to failure.58 For example, Walker et al58 reported spinners that failed to lock in at 15 Ncm had a cumulative survival rate of 86%, whereas implants that locked in at 30 Ncm had a survival rate of 96% (mean 3-year follow-up). Rodrigo et al65 also observed that implants initially denoted as stable had survival rates of 99.1% (after 6 to 42 months) versus unstable (spinners), which had survival rates of 94.1%.
If poor primary stability exists after implant placement, several options can be used to improve the situation. The osteotomy can be deepened if apical bone is available, or a wider implant may be used if bone and space are present.66,67 Clinicians can also consider removing an implant and adding bone to the osteotomy with an amalgam carrier, condensing the bone, and then placing the implant.68 However, an osteotome or drill (not moving) one size smaller than the implant needs to be placed into the osteotomy to condense bone laterally and create an orienting space for implant insertion. When dealing with a spinner, it is prudent to submerge the implant and allow it to osseointegrate for 3 to 6 months before loading it.69-71
Concerning unstable implants, another facet of therapy that may affect results is implant surface topography. Orenstein et al72 described improved survival rates of mobile implants that were coated with hydroxyapatite compared to unstable implants without a coating (91.8% vs 53.6%, respectively, after 3 years). With spinners, Balshi et al69 also achieved better survival rates with textured implants compared to machined surfaces (91.7% vs 70.0%, respectively). Pertinently, several authors suggested there is an improved initial stability with rough-surfaced implants compared to machined implants after evaluations were done in an artificial bone.73,74 However, in a review article, Javed et al75 concluded that it is unclear if surface morphology improves primary stability.
High Insertion Torque: No Significant Residual Benefit
It appears that initial benefits of high insertion torque may not be maintained. If initial stability of an implant is defined with an Osstell unit as low (eg, ISQ 55) and there is no visible mobility, osseointegration can increase ISQ.76 Conversely, if the initial stability is high (eg, ≥ISQ 75), osseointegration does not enhance stability.76,77 Actually, a high initial primary stability achieved with high insertion torque will be supplanted by a developed biological stability that has a lower ISQ.23,38,78,79 Evidence supporting this concept has been demonstrated in numerous studies using different ISQ values to represent low and high insertion torques (eg, ISQ <56 vs >56,23 ISQ <68 vs >7238). Similarly, Olsson et al80 demonstrated that stability of implants with initially low ISQ values increased with time, and implants with high ISQ values decreased from the time of placement to permanent bridge insertion (ISQ values ranged initially from 45 to 75). In general, implants tended to have an ISQ of 60 to 65.
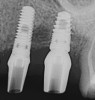
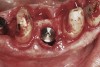
Apparently with time, stable implants placed with low initial torque develop bone characteristics around them that are similar to sites where implants were placed with a high initial torque (Figure 4 and Figure 5). Conversely, for implants placed with a high initial torque, the healing process, despite the high initial torque, provides a level of biologic stability that is not necessarily influenced by the initial insertion torque value.
Potential Errors Due to Overreliance on Insertion Torque
Using the console of a contemporary implant motor, a clinician can select the amount of insertion torque to use for implantation. When the programmed torque is reached (eg, 30 Ncm), the implant usually binds on some aspects of the osteotomy’s walls and ceases rotation into bone. However, the clinician is unable to discern precisely where binding occurred and cannot know if bony contact exists throughout the osteotomy’s length or only in the area of cortical bone.81 Several scenarios may be encountered with respect to the various types of bone density, ie, dense, medium, and soft. To help clarify appropriate drilling protocols and selection of insertion torques for diverse situations, clinicians can ascertain information concerning bone density during initial osteotomy preparation with a 2-mm twist drill.67,82 They can tactilely determine the quality of bone with which they are engaging, ie, dense, medium, or soft.67,83 Dense bone provides frictional resistance to drill penetration for most of the osteotomy’s length. This finding will translate into resistance to implant insertion and result in intimate contact between an implant and bone at the programmed insertion torque.67,84
Regarding medium-quality bone, which consists of 1 mm to 2 mm of dense cortical bone and a poorly trabecularized marrow compartment, decision-making is more problematic.67 For example, the cortical bone in this situation often provides all the resistance to implant insertion.81 Thus, if the clinician uses insertion torque as the sole parameter for clinical decision-making, an immediate load protocol may be selected to complete the procedure. This could create a problem with respect to maintaining primary stability, because the biologic width may form during early wound healing around a nonsubmerged, functionally utilized implant, thereby reducing the amount of cortical bone support. The implant may then be subjected to micromotion above the critical threshold and fail to achieve osseointegration.
On the other hand, when encountering soft bone, it is less likely that the desired insertion torque will be reached and the implant ceases to rotate. Lack of drilling resistance will be obvious to the implant surgeon and will dictate the need to adjust clinical procedures to accommodate this finding (eg, undersize the osteotomy and/or submerge the implants for protected and possibly prolonged healing).67 In summary, tactile information furnished by the first surgical drill can be employed in conjunction with insertion torque to achieve predictable primary stability of inserted implants.
Summary and Conclusions
Initial insertion torque should provide primary stability when an implant is inserted. In general, insertion torques of ≥30 Ncm can be used to insert dental implants in healed ridges or fresh extraction sockets. For implants that are to be immediately loaded the insertion torque is also ≥30 Ncm (ie, 30 Ncm to 40 Ncm). The data support the concept that high insertion torques (≥50 Ncm) attain greater initial stability and do not induce bone resorption. Spinners are associated with low insertion torque; nevertheless, their submergence can result in a high osseointegration rate. It also seems that implants placed with a low insertion torque can achieve biologic stability, while implants placed with a high insertion force develop a biologic stability similar to those placed with a lower insertion torque. Finally, from a practical perspective, tactile information furnished by the first surgical drill can be used to aid selection of insertion torques that can achieve desired primary stability of inserted dental implants.
ABOUT THE AUTHORS
Gary Greenstein, DDS, MS
Clinical Professor, Department of Periodontology, College of Dental Medicine, Columbia University, New York, New York; Private Practice, Surgical Implantology and Periodontics, Freehold, New Jersey
John Cavallaro, DDS
Clinical Professor, Department of Prosthodontics, College of Dental Medicine, Columbia University, New York, New York; Private Practice, Surgical Implantology and Prosthodontics, Brooklyn, New York
Queries to the authors regarding this course may be submitted to authorqueries@aegiscomm.com.
REFERENCES
1. Trisi P, Todisco M, Consolo U, Travaglini D. High versus low implant insertion torque: a histologic, histomorphometric, and biomechanical study in the sheep mandible. Int J Oral Maxillofac Implants. 2011;26(4):837-849.
2. Trisi P, De Benedittis S, Perfetti G, Berardi D. Primary stability, insertion torque and bone density of cylindric implant ad modum Branemark: is there a relationship? An in vitro study. Clin Oral Implants Res. 2011;22(5):567-570.
3. Szmukler-Moncler S, Piattelli A, Favero GA, Dubruille JH. Considerations preliminary to the application of early and immediate loading protocols in dental implantology. Clin Oral Implants Res. 2000;11(1):12-25.
4. Pilliar RM, Lee JM, Maniatopoulos C. Observations on the effect of movement on bone in growth into porous-surfaced implants. Clin Orthop Relat Res. 1986;208:108-313.
5. Rabel A, Köhler SG, Schmidt-Westhausen AM. Clinical study of the primary stability of two dental implant systems with resonance frequency analysis. Clin Oral Investig. 2007;11(3):257-265.
6. Lioubavina-Hack N, Lang NP, Karring T. Significance of primary stability for osseointegration of dental implants. Clin Oral Implant Res. 2006;17(3):244-250.
7. Trisi P, Perfetti G, Baldoni E, et al. Implant micromotion is related to peak insertion torque and bone density. Clin Oral Implants Res. 2009;20(5):467-471.
8. Cochran DL. Report of the American Academy of Periodontology’s Workshop on the Design and Conduct of Clinical Trials for Endosseous Dental Implants. J Periodontol. 1998;69(2):280-284.
9. Barewal RM, Oates TW, Meredith N, Cochran DL. Resonance frequency measurement of implant stability in vivo on implants with a sandblasted and acid-etched surface. Int J Oral Maxillofac Implants. 2003;18(5):641-651.
10. Beer A, Gahleitner A, Holm A, et al. Correlation of insertion torques with bone mineral density from dental quantitative CT in the mandible. Clin Oral Implants Res. 2003;14(5):616-620.
11. Martinez H, Davarpanah M, Missika P, et al. Optimal implant stabilization in low density bone. Clin Oral Implants Res. 2001;12(5):423-432.
12. Meredith N. Assessment of implant stability as a prognostic determinant. Int J Prosthodont. 1998;11(15):491-501.
13. Nkenke E, Hahn M, Weinzierl K, et al. Implant stability and histomorphometry: a correlation study in human cadavers using stepped cylinder implants. Clin Oral Implants Res. 2003;14(5):601-609.
14. O’Sullivan D, Sennerby L, Meredith N. Measurements comparing the initial stability of five designs of dental implants: a human cadaver study. Clin Implant Dent Relat Res. 2000;2(2):85-92.
15. Sennerby L, Roos J. Surgical determinants of clinical success of osseointegrated oral implants: a review of the literature. Int J Prosthodont. 1998;11(5):408-420.
16. Dagher M, Mokbel N, Jabbour G, Naaman N. Resonance frequency analysis, insertion torque, and bone to implant contact of 4 implant surfaces: comparison and correlation study in sheep. Implant Dent. 2014;23(6):672-678.
17. Perren SM. Evolution of the internal fixation of long bone fractures. The scientific basis of biological internal fixation: choosing a new balance between stability and biology. J Bone Joint Surg Br. 2002;84(8):1093-1110.
18. Rahn BA. Bone healing: histologic and physiologic concepts. In: Sumner-Smith G, ed. Bone in Clinical Orthopedics. 2nd ed. New York, NY: Thieme, AO Publishing; 2002:287-326.
19. Sivolella S, Bressan E, Salata LA, et al. Osteogenesis at implants without primary bone contact - an experimental study in dogs. Clin Oral Implants Res. 2012;23(5):542-549.
20. Atsumi M, Park SH, Wang HL. Methods used to assess implant stability: current status. Int J Oral Maxillofac Implants. 2007;22(5):743-754.
21. Mistry G, Shetty O, Shetty S, Singh RD. Measuring implant stability: A review of different methods. J Dent Implants. 2014;4(2):165-169.
22. Al-Nawas B, Wagner W, Grötz KA. Insertion torque and resonance frequency analysis of dental implant systems in an animal model with loaded implants. Int J Oral Maxillofac Implants. 2006;21(5):726-732.
23. West JD, Oates TW. Identification of stability changes for immediately placed dental implants. Int J Oral Maxillofac Implants. 2007;22(4):623-630.
24. Hämmerle CH, van Steenberghe D. The first EAO Consensus Conference 16-19 February 2006, Pfäffikon, Switzerland. Clin Oral Implants Res. 2006;17(suppl 2):1.
25. Degidi M, Perrotti V, Strocchi R, et al. Is insertion torque correlated to bone-implant contact percentage in the early healing period? A histological and histomorphometrical evaluation of 17 human-retrieved dental implants. Clin Oral Implants Res. 2009;20(8):778-781.
26. Kahraman S, Bal BT, Asar NV, et al. Clinical study on the insertion torque and wireless resonance frequency analysis in the assessment of torque capacity and stability of self-tapping dental implants. J Oral Rehabil. 2009;36(10):755-761.
27. Turkyilmaz I, McGlumphy EA. Influence of bone density on implant stability parameters and implant success: a retrospective clinical study. BMC Oral Health. 2008;8:32.
28. Norton M. Primary stability versus viable constraint—a need to redefine. Int J Oral Maxillofac Implants. 2013;28(1):19-21.
29. Friberg B, Sennerby L, Gröndahl K, et al. On cutting torque measurements during implant placement: a 3-year clinical prospective study. Clin Implant Dent Relat Res. 1999;1(2):75-83.
30. Johansson B, Bäck T, Hirsch JM. Cutting torque measurements in conjunction with implant placement in grafted and nongrafted maxillas as an objective evaluation of bone density: a possible method for identifying early implant failures? Clin Implant Dent Relat Res. 2004;6(1):9-15.
31. Akça K, Chang TL, Tekdemir I, Fanuscu MI. Biomechanical aspects of initial intraosseous stability and implant design: a quantitative micro-morphometric analysis. Clin Oral Implants Res. 2006;17(4):465-472.
32. Farré-Pagés N, Augé-Castro ML, Alaejos-Algarra F, et al. Relation between bone density and primary implant stability. Med Oral Patol Oral Cir Bucal. 2011;16(1):e62-e67.
33. Marquezan M, Osório A, Sant’Anna E, et al. Does bone mineral density influence the primary stability of dental implants? A systematic review. Clin Oral Implants Res. 2012;23(7):767-774.
34. Wada M, Suganami T, Sogo M, Maeda Y. Can we predict the insertion torque using the bone density around the implant? Int J Oral Maxillofac Surg. 2016;45(2):221-225.
35. Geckili O, Bilhan H, Bilgin T. A 24-week prospective study comparing the stability of titanium dioxide grit-blasted dental implants with and without fluoride treatment. Int J Oral Maxillofac Implants. 2009;24(4):684-688.
36. Lai HC, Zhang ZY, Wang F, et al. Resonance frequency analysis of stability on ITI implants with osteotome sinus floor elevation technique without grafting: a 5-month prospective study. Clin Oral Implants Res. 2008;19(5):469-475.
37. Glauser R, Sennerby L, Meredith N, et al. Resonance frequency analysis of implants subjected to immediate or early functional occlusal loading. Successful vs. failing implants. Clin Oral Implants Res. 2004;15(4):428-434.
38. Simunek A, Kopecka D, Brazda T, et al. Development of implant stability during early healing of immediately loaded implants. Int J Oral Maxillofac Implants. 2012;27(3):619-627.
39. Wilke HJ, Claes L, Steinemann SG. The influence of various titanium surfaces on the interface shear strength between implants and bone. In: Heimke G, Soltesz U, Lee AJC, eds. Advances in Biomaterials, Vol 9, Clinical Implant Materials: Proceedings of the Eight European Conference on Biomaterials, Heidelberg, FRG, September 7-9, 1989. Amsterdam: Elsevier Science; 1990.
40. Oates TW, Valderrama P, Bischof M, et al. Enhanced implant stability with a chemically modified SLA surface: a randomized pilot study. Int J Oral Maxillofac Implants. 2007;22(5):755-760.
41. Strnad J, Urban K, Povysil C, Strnad Z. Secondary stability assessment of titanium implants with an alkali-etched surface: a resonance frequency analysis study in beagle dogs. Int J Oral Maxillofac Implants. 2008;23(3):502-512.
42. Jemat A, Ghazali MJ, Razali M, Otsuka Y. Surface modifications and their effects on titanium dental implants. Biomed Res Int. 2015;2015:791725. doi: 10.1155/2015/791725.
43. Yeo IS. Reality of dental implant surface modification: a short literature review. Open Biomed Eng J. 2014;8:114-119.
44. Cooper LF. Factors influencing primary dental implant stability remain unclear. J Evid Based Dent Pract. 2012;12(3 suppl):185-186.
45. Khayat PG, Arnal HM, Tourbah BI, Sennerby L. Clinical outcome of dental implants placed with high insertion torques (up to 176 Ncm). Clin Implant Dent Relat Res. 2013;15(2):227-233.
46. Benic GI, Mir-Mari J, Hämmerle CH. Loading protocols for single-implant crowns: a systematic review and meta-analysis. Int J Oral Maxillofac Implants. 2014;29(suppl)222-238.
47. Irinakis T, Wiebe C. Initial torque stability of a new bone condensing dental implant. A cohort study of 140 consecutively placed implants. J Oral Implantol. 2009;35(6):277-282.
48. Grandi T, Garuti G, Guazzi P, et al. A longitudinal, multi-centre study on the relationship between insertion torque and peri-implant bone resorption. J Clin Pract Oral Implantol. 2010;1(2):33-40.
49. Alsaadi G, Quirynen M, Michiels K, et al. A biomechanical assessment of the relation between the oral implant stability at insertion and subjective bone quality assessment. J Clin Periodontol. 2007;34(4):359-366.
50. Norton MR. The influence of insertion torque on the survival of immediately placed and restored single-tooth implants. Int J Oral Maxillofac Implants. 2011;26(6):1333-1343.
51. Papaspyridakos P, Chen CJ, Chuang SK, Weber HP. Implant loading protocols for edentulous patients with fixed prostheses: a systematic review and meta-analysis. Int J Oral Maxillofac Implants. 2014;29(suppl):256-270.
52. Schimmel M, Srinivasan M, Herrmann FR, Müller F. Loading protocols for implant-supported overdentures in the edentulous jaw: a systematic review and meta-analysis. Int J Oral Maxillofac Implants. 2014;29(suppl):271-286.
53. Schrott A, Riggi-Heiniger M, Maruo K, Gallucci GO. Implant loading protocols for partially edentulous patients with extended edentulous sites—a systematic review and meta-analysis. Int J Oral Maxillofac Implants. 2014;29(suppl):239-255.
54 Ottoni JM, Oliveira ZF, Mansini R, Cabral AM. Correlation between placement torque and survival of single-tooth implants. Int J Oral Maxillofac Implants. 2005;20(5):769-776.
55. Toljanic JA, Baer RA, Ekstrand K, Thor A. Implant rehabilitation of the atrophic edentulous maxilla including immediate fixed provisional restoration without the use of bone grafting: a review of 1-year outcome data from a long-term prospective clinical trial. Int J Oral Maxillofac Implants. 2009;24(3):518-526.
56. Degidi M, Daprile G, Piattelli A. Implants inserted with low insertion torque values for intraoral welded full-arch prosthesis: 1-year follow-up. Clin Implant Dent Relat Res. 2012;14(suppl 1):e39-e45.
57. Becker CM, Wilson TG Jr, Jensen OT. Minimum criteria for immediate provisionalization of single-tooth dental implants in extraction sites: a 1-year retrospective study of 100 consecutive cases. J Oral Maxillofac Surg. 2011;69(2):491-497.
58. Walker LR, Morris GA, Novotny PJ. Implant insertional torque values predict outcomes. J Oral Maxillofac Surg. 2011;69(5):1344-1349.
59. Romanos GE. Surgical and prosthetic concepts for predictable immediate loading of oral implants. J Calif Dent Assoc. 2004;32(12):991-1001.
60. Consolo U, Travaglini D, Todisco M, et al. Histologic and biomechanical evaluation of the effects of implant insertion torque on peri-implant bone healing. J Craniofac Surg. 2013;24(3):860-865.
61. Akkocaoglu M, Uysal S, Tekdemir I, et al. Implant design and intraosseous stability of immediately placed implants: a human cadaver study. Clin Oral Implants Res. 2005;16(2):202-209.
62. Alves CC, Neves M. Tapered implants: from indications to advantages. Int J Periodontics Restorative Dent. 2009;29(2):161-167.
63. Niimi A, Ozeki K, Ueda M, Nakayama B. A comparative study of removal torque of endosseous implants in the fibula, iliac crest and scapula of cadavers: preliminary report. Clin Oral Implants Res. 1997;8(4):286-289.
64. Li H, Liang Y, Zheng Q. Meta-analysis of correlations between marginal bone resorption and high insertion torque of dental implants. Int J Oral Maxillofac Implants. 2015;30(4):767-772.
65. Rodrigo D, Aracil L, Martin C, Sanz M. Diagnosis of implant stability and its impact on implant survival: a prospective case series study. Clin Oral Implants Res. 2010;21(3):255-261.
66. Greenstein G, Cavallaro JS Jr, Tarnow DP. Clinical pearls for surgical implant dentistry: part 2. Dent Today. 2010;29(8):64-68.
67. Cavallaro J Jr, Greenstein B, Greenstein G. Clinical methodologies for achieving primary dental implant stability: the effects of alveolar bone density. J Am Dent Assoc. 2009;140(11):1366-1372.
68. Hahn J. Clinical uses of osteotomes. J Oral Implantol. 1999;25(1):23-29.
69. Balshi SF, Wolfinger GJ, Balshi TJ. A retrospective analysis of 44 implants with no rotational primary stability used for fixed prosthesis anchorage. Int J Oral Maxillofac Implants. 2007;22(3):467-471.
70. Fugazzotto PA. Treatment options following single-rooted tooth removal: a literature review and proposed hierarchy of treatment selection. J Periodontol. 2005;76(5):821-831.
71. Fugazzotto PA. Implant placement at the time of maxillary molar extraction: technique and report of preliminary results of 83 sites. J Periodontol. 2006;77(2):302-309.
72. Orenstein IH, Tarnow DP, Morris HF, Ochi S. Three-year post-placement survival of implants mobile at placement. Ann Periodontol. 2000;5(1):32-41.
73. Tabassum A, Meijer GJ, Wolke JG, Jansen JA. Influence of surgical technique and surface roughness on the primary stability of an implant in artificial bone with different cortical thickness: a laboratory study. Clin Oral Implants Res. 2010;21(2):213-220.
74. Tabassum A, Meijer GJ, Wolke JG, Jansen JA. Influence of the surgical technique and surface roughness on the primary stability of an implant in artificial bone with a density equivalent to maxillary bone: a laboratory study. Clin Oral Implants Res. 2009;20(4):327-332.
75. Javed F, Almas K, Crespi R, Romanos GE. Implant surface morphology and primary stability: is there a connection? Implant Dent. 2011;20(1):40-46.
76. Sennerby L. Resonance frequency analysis for implant stability measurements. A review. Integration Diagnostics Update. 2015;1:1-11.
77. Osseointegration and The ISQ Scale. Penguin RFA website. http://www.penguinrfa.com/isq-scale/. Accessed November 8, 2016.
78. Becker W, Sennerby L, Bedrossian E, et al. Implant stability measurements for implants placed at the time of extraction: a cohort, prospective clinical trial. J Periodontol. 2005;76(3):391-397.
79. Nedir R, Bischof M, Szmukler-Moncler S, et al. Predicting osseointegration by means of implant primary stability. Clin Oral Implants Res. 2004;15(5):520-528.
80. Olsson M, Urde G, Andersen JB, Sennerby L. Early loading of maxillary fixed cross-arch dental prostheses supported by six or eight oxidized titanium implants: results after 1 year of loading, case series. Clin Implant Dent Relat Res. 2003;5(suppl 1):81-87.
81. Ito Y, Sato D, Yoneda S, et al. Relevance of resonance frequency analysis to evaluate dental implant stability: simulation and histomorphometrical animal experiments. Clin Oral Implants Res. 2008;19(1):9-14.
82. Greenstein G, Cavallaro J, Greenstein B, Tarnow D. Treatment planning implant dentistry with a 2-mm twist drill. Compend Contin Educ Dent. 2010:31(2):126-136.
83. Trisi P, Rao W. Bone classification: clinical-histomorphometric comparison. Clin Oral Implants Res. 1999;10(1):1-7.
84. Misch CE, Qu Z, Bidez MW. Mechanical properties of trabecular bone in the human mandible: implications of dental implant treatment planning and surgical placement. J Oral Maxillofac Surg. 1999;57(6):700-706.