You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Partial or complete edentulism adversely affects quality of life and can have a derogatory effect on the maintenance of an individual's overall health.1,2 Nearly 1 in 5 Americans 65 years or older have lost all their teeth.3 Anyone with tooth loss may be a candidate for implants; therefore, incorporating digital workflow technology for implant treatment may be a useful plan for any dental office.
The field of digital dental workflow has made great technological advancements due to improvements in tools such as intraoral scanners, CAD/CAM, cone-beam computed tomography (CBCT), and software programs. These technologies have improved the communication between clinician, technician, and patient. The digital workflow streamlines processes, reducing treatment times and costs.4 As a result, clinical practices are shifting to virtual-based workflows, and digital dentistry is becoming an increasingly substantial discipline.5 This article will discuss how to achieve the goal of using technology to make dental workflows more accurate and predictable, ultimately saving time and money.
An implant workflow or restorative workload begins with a diagnostic workup, which will include a complete medical and dental history, hard- and soft-tissue charting, radiographs, and camera images. Digital technology such as intraoral cameras, extraoral cameras, radiographic sensors, panoramic images, intraoral scanners, and CBCT machines all contribute to developing a data set for each patient. The data set will help with communication between everyone involved in the treatment plan. Overall, the introduction of digital systems into the diagnostic routine, and their application together with 3-dimensional (3D) data of bone topography, have made it possible to reconcile the two central aspects of oral implant surgery: (1) planning an ideal prosthetic solution with (2) the given anatomic situation.6
Cone-Beam Computed Tomography
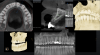
The introduction of CBCT in the late 1990s represented an unparalleled advancement in dentistry, especially in the field of implant surgery, in part because it greatly reduced radiation exposure to patients compared with multislice CT.7-9 The information generated by CBCT offers the potential of improved diagnosis and treatment planning for a wide range of clinical applications in implant dentistry.10 Originally, CBCT scans were obtained with the patient wearing a radiographic template with fiducial markers.11 However, now there is also a radiographic template-free computer-guided implant surgery workflow that can be used for partially edentulous patients.12 If there are enough remaining teeth, image fusion of the intraoral scan data and the CBCT data can be performed by matching resin markers placed in the patient's mouth.6 A CBCT scan obtains the patient's bone height, thickness, and angulation (Figure 1). This information is important for treatment planning because the next step is for the CBCT data to be imported into virtual implant planning software to formulate a prosthetically driven implant surgical plan.13 These planning data are then transferred to a surgical template that can be physically fabricated in a variety of ways, either in or out of the office, and using a variety of materials, including ceramic, lithium disilicate, and zirconia.14
Studies support the use of CBCT in dental implant treatment planning particularly in regard to linear measurements, 3D evaluation of alveolar ridge topography, proximity to vital anatomical structures, and fabrication of surgical guides.15 The International Congress of Oral Implantologists recommends that all CBCT examinations, as well as other radiographic examinations, must be justified on an individualized needs basis.15 The benefits to the patient must outweigh the potential risks. This is again why it is critical to obtain a thorough medical and dental history, in addition to performing comprehensive clinical examinations.
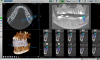
In addition to its use in diagnostics and treatment planning, a CBCT scan can be used for postsurgical evaluations (Figure 2). A postsurgical scan can be taken and placed over the image of the treatment plan to evaluate how close the implant is to the original plan. The practitioner may want to implement the cotton roll technique, in which a cotton roll is placed on areas to highlight the area on the CBCT.16 The cotton roll works by keeping the soft tissue pushed down to better visualize the bone. Similarly, cotton rolls can be used before a CBCT scan involving a denture: lingual cotton rolls can be used to keep the tongue away from the lingual slope of the complete denture; occlusal cotton rolls permit visualization of the occlusal surface details; and buccal cotton rolls can keep the cheeks and lips away from the denture surface.17 Thus, apart from radio-diagnostic possibilities, CBCT may offer a huge therapeutic potential related to surgical guides and further prosthetic rehabilitation.18 A CBCT scan can provide dentists with more precise diagnostic information than traditional radiography and impressions, especially when combined with intraoral scanning.
Intraoral Scanners
Intraoral scanners allow a dentist to skip creating a physical impression of a tooth meant for restoration, as well as create more accurate and cleaner scans for a laboratory technician to use to create quality restorations. A digital workflow does not mean the dentist must mill in-house; digital data can be sent to a laboratory or milled in-house, depending on preference. The accuracy of a digital impression technique to fabricate the implant restoration and abutment for a dental implant using an intraoral laser scanner may greatly improve the quality of these restorations. Intraoral scanners allow an immediate determination of the quality of an impression and have the capacity to easily send the models to the laboratory using email or a software program, thus reducing expense and time. Compared with physical impressions, intraoral scans are often more comfortable for the patient and faster.
A variety of intraoral scanners and software are on the market. It is important to consider the quality of the data derived from scanning when choosing which device to incorporate into a dental practice.19,20 Intraoral scanners and software are used in one of the most critical first steps in the 2D/3D digital design process: documenting a patient's smile (Figure 3). The use of dynamic smile documentation provides more efficient diagnoses, more consistent treatment plans, and improved final results.21 This design process can be performed in an entirely digital workflow and will help with all rehabilitative procedures. The advantages of using video documentation are that it facilitates and simplifies the documentation process and improves smile design, facial analysis, treatment planning, team communication, and patient education.22
Although intraoral scanners are integral to the digital workflow, they are not without limitations, and there is a learning curve for adopting intraoral scanners into a dental clinic.23-25 Dentists who are more comfortable in the digital technology world will likely find it easier to adopt intraoral scanners into their practice than dentists who are less experienced in technological innovations.23-25Additionally, unlike the conventional impression materials, light cannot physically detach the gum and therefore cannot register nonvisible areas.26 Similarly, commonly cited challenges with intraoral scanners and optical impressions include difficulty in detecting deep margin lines in prepared teeth or in cases of bleeding.27 Practice, proper attention, and strategies for highlighting preparation lines and avoiding bleeding make it possible for clinicians to detect a satisfactory optical impression even in difficult contexts.19
CAD/CAM
Computer-guided surgery has been validated since the introduction of digital technology in the early 2000s as an efficient and reliable technique for obtaining functional and esthetic outcomes (Figure 4).28,29 Computer-guided implant surgery is defined by the use of a surgical template that reproduces a virtual implant position designed from digital data.30 If a dentist is using a static surgical guide, it can be created with the use of 3D printing.31 CAD/CAM software is an essential tool because it is responsible for guiding robotic devices that design objects and assemblies in a virtual environment.32 CAD/CAM machines can be used to manufacture ceramic restorations based on computer-assisted design and produce a restoration at a single dental appointment, an increasingly popular process.33Dentists can directly scan prosthetic preparations or scan bodies, import those scans into a CAD program, design the restoration, and mill them in an esthetic material.34,35 The restorations are then delivered to the patient through what has been a succinct digital workflow.
Dynamic Surgical Navigation
The next step that is possible with fully digital dentistry is dynamically navigated dental implants. Computer-assisted surgery can be either static or dynamic. Static guides are 3D printed from CAD/CAM and 3D data, as described in the previous section. Dynamic navigation combines digital data from CBCT scans and intraoral scanners so the surgeon can virtually plan the ideal implant location and then use that plan to surgically navigate the exact implant placement.
By using these three technologies together, the surgeon can plan and place implants with an optimal restorative goal in mind. Using dynamic navigation to more accurately place the implant can result in a more functional and esthetic outcome. Dynamic navigation tracks the patient position and live movements of the handpiece drill in real time on a computer screen. With dynamic guidance, the surgeon can view the handpiece's position, angle, and depth while drilling as they relate to the planned implant placement.
Clinical studies show that implants placed with dynamic navigation are more accurate than freehand implant placement.36 Static and dynamic image navigation are both highly accurate systems; however, dynamic systems have additional advantages. Patients can be scanned and planned and have surgery in one day, and plans can be altered during surgery as needed based on the clinical situation. Moreover, the entire field can be visualized throughout the process, allowing accuracy to be verified at any time.36
Conclusion
CBCT, intraoral scanners, and other image-acquisition devices are critical parts of the digital dental field. They can be used to create a fully digital workflow for optimal prosthetic results that are easy to obtain and affordable. Another advantage of using a digital workflow is that with the creation of a preoperative mock-up, the patient can see the impact of the new smile before committing to the treatment and irreversible procedures, thereby increasing patient education and case acceptance. Scientific literature shows that a digital workflow is more efficient than the previously common conventional pathway.4 Studies have also found that overall, patient preference was significantly in favor of a digital technique when compared with conventional impression techniques because it often reduces a patient's stress and discomfort.37Digital techniques are therefore not only beneficial for dentists in the time saved and accuracy gained but preferred by patients as well.
About the Author
Robert Pauley, Jr., DMD Private Practice Union City, Georgia
References
1. Ozhayat EB, Stoltze K, Elverdam B, Owall B. A method for assessment of quality of life in relation to prosthodontics. Partial edentulism and removable partial dentures. J Oral Rehabil. 2007;34(5):336-344.
2. Kimura A, Arakawa H, Noda K, et al. Response shift in oral health-related quality of life measurement in patients with partial edentulism. J Oral Rehabil. 2012;39(1):44-54.
3. Dye BA, Thornton-Evans G, Li X, Iafolla TJ. Dental caries and tooth loss in adults in the United States, 2011-2012. NCHS Data Brief. 2015;(197):197.
4. Joda T, Brägger U. Digital vs. conventional implant prosthetic workflows: a cost/time analysis. Clin Oral Implants Res. 2015;26(12):1430-1435.
5.Mangano F, Shibli JA, Fortin T. Digital dentistry: new materials and techniques. Int J Dent. 2016;2016:5261247.
6. De Vico G, Ferraris F, Arcuri L, et al. A novel workflow for computer guided implant surgery matching digital dental casts and CBCT scan. Oral Implantol (Rome). 2016;9(1):33-48.
7. Spinelli D, Ottria L, De Vico G, et al. Full rehabilitation with Nobel Clinician® and Procera Implant Bridge®: case report. Oral Implantol (Rome). 2013;6(2):25-36.
8. Sukovic P. Cone beam computed tomography in craniofacial imaging. Orthod Craniofac Res. 2003;6(suppl 1):31-36.
9. Tsiklakis K, Donta C, Gavala S, et al. Dose reduction in maxillofacial imaging using low dose cone beam CT. Eur J Radiol. 2005;56(3):413-417.
10. Ganz SD. Cone beam computed tomography-assisted treatment planning concepts. Dent Clin North Am. 2011;55(3):515-536.
11. Terzioğlu H, Akkaya M, Ozan O. The use of a computerized tomography-based software program with a flapless surgical technique in implant dentistry: a case report. Int J Oral Maxillofac Implants. 2009;24(1):137-142.
12. Arcuri L, Lorenzi C, Cecchetti F, et al. Full digital workflow for implant-prosthetic rehabilitations: a case report. Oral Implantol (Rome). 2015;8(4):114-121.
13. Orentlicher G, Abboud M. Guided surgery for implant therapy. Dent Clin North Am. 2011;55(4):715-744.
14. D'haese J, Ackhurst J, Wismeijer D, et al. Current state of the art of computer-guided implant surgery. Periodontol 2000. 2017;73(1):121-133.
15. Benavides E, Rios HF, Ganz SD, et al. Use of cone beam computed tomography in implant dentistry: the International Congress of Oral Implantologists consensus report. Implant Dent. 2012;21(2):78-86.
16. Rinaldi M, Ganz S, Mottola A. Computer-Guided Applications for Dental Implants, Bone Grafting, and Reconstructive Surgery. 1st ed. Elsevier; 2015.
17. Scherer MD. Do we need a radiographic guide? A review of the cone-beam computed tomography (CBCT) visualization and treatment planning for narrow-diameter implant overdentures. Implant Practice. 2014;7(3)34-37.
18. Jacobs R, Salmon B, Codari M, et al. Cone beam computed tomography in implant dentistry: recommendations for clinical use. BMC Oral Health. 2018;18(1):88.
19. Aragón ML, Pontes L, Bichara L, et al. Validity and reliability of intraoral scanners compared to conventional gypsum models measurements: a systematic review. Eur J Orthod. 2016;38(4):429-434.
20. Ender A, Mehl A. Accuracy of complete-arch dental impressions: a new method of measuring trueness and precision. J Prosthet Dent. 2013;109(2):121-128.
21. Tarantili VV, Halazonetis DJ, Spyropoulos MN. The spontaneous smile in dynamic motion. Am J Orthod Dentofacial Orthop. 2005;128(1):8-15.
22. Coachman C, Calamita MA, Sesma N. Dynamic documentation of the smile and the 2D/3D digital smile design process. Int J Periodontics Restorative Dent. 2017;37(2):183-193.
23. Lim JH, Park JM, Kim M, et al. Comparison of digital intraoral scanner reproducibility and image trueness considering repetitive experience. J Prosthet Dent. 2018;119(2):225-232.
24. Mandelli F, Ferrini F, Gastaldi G, et al. Improvement of a digital impression with conventional materials: overcoming intraoral scanner limitations. Int J Prosthodont. 2017;30(4):373-376.
25. Marti AM, Harris BT, Metz MJ, et al. Comparison of digital scanning and polyvinyl siloxane impression techniques by dental students: instructional efficiency and attitudes towards technology. Eur J Dent Educ. 2017;21(3):200-205.
26. Zimmermann M, Mehl A, Mörmann WH, Reich S. Intraoral scanning systems - a current overview. Int J Comput Dent. 2015;18(2):101-129.
27. Mangano F, Gandolfi A, Luongo G, Logozzo S. Intraoral scanners in dentistry: a review of the current literature. BMC Oral Health. 2017;17(1):149.
28. Vercruyssen M, Laleman I, Jacobs R, Quirynen M. Computer-supported implant planning and guided surgery: a narrative review. Clin Oral Implants Res. 2015;26(suppl 11):69-76.
29. D'haese J, Van De Velde T, Komiyama A, et al. Accuracy and complications using computer-designed stereolithographic surgical guides for oral rehabilitation by means of dental implants: a review of the literature. Clin Implant Dent Relat Res. 2012;14(3):321-335.
30. Cassetta M, Stefanelli LV, Giansanti M, Calasso S. Accuracy of implant placement with a stereolithographic surgical template. Int J Oral Maxillofac Implants. 2012;27(3):655-663.
31. Schneider D, Schober F, Grohmann P, et al. In-vitro evaluation of the tolerance of surgical instruments in templates for computer-assisted guided implantology produced by 3-D printing. Clin Oral Implants Res. 2015;26(3):320-325.
32. Chew AA, Esguerra RJ, Teoh KH, et al. Three-dimensional accuracy of digital implant impressions: effects of different scanners and implant level. Int J Oral Maxillofac Implants. 2017;32(1):70-80.
33. Roperto R, Assaf H, Soares-Porto T, et al. Are different generations of CAD/CAM milling machines capable to produce restorations with similar quality? J Clin Exp Dent. 2016;8(4):e423-e428.
34. Imburgia M, Logozzo S, Hauschild U, et al. Accuracy of four intraoral scanners in oral implantology: a comparative in vitro study. BMC Oral Health. 2017;17(1):92.
35. Mangano FG, Veronesi G, Hauschild U, et al. Trueness and precision of four intraoral scanners in oral implantology: a comparative in vitro study. PLoS One. 2016;11(9):e0163107.
36. Emery RW, Merritt SA, Lank K, Gibbs JD. Accuracy of dynamic navigation for dental implant placement-model-based evaluation. J Oral Implantol. 2016;42(5):399-405.