You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Dental patients may seek answers to challenges they experience while they sleep. It is now more common for patients to present to the dental office feeling tired, experiencing headaches, or stating that they were diagnosed with sleep apnea but could not tolerate the use of a continuous positive airway pressure (CPAP) machine. This growing desire to learn more about sleep disorders is in line with trend analysis from Google showing that general public interest on the topic of sleep has peaked in recent months.1
Consistent with these trends, position statements have been published by organized dentistry. For instance, the American Dental Association (ADA) published an 11-point position statement on the role of dentists in sleep-related breathing disorders (SRBDs) in October 2017.2 The primary message from the ADA is for practices to actively screen patients and treat patients for sleep disorders with an oral appliance as may be indicated. More recently, in March 2019, the American Academy of Orthodontists published a 53-page white paper to address patients with obstructive sleep apnea (OSA).3
Non-discriminatory screening for this potentially life-threatening condition must be conducted to identify the more than 80% of patients who are estimated to remain undiagnosed and untreated.4Current research estimates that there are more than 1.3 billion individuals with sleep apnea worldwide.5
Prevalence and Screening for Sleep Disorders
According to the Centers for Disease Control and Prevention, at least 28.5% and as much as 44.1% of the adult American population suffers from insufficient sleep.6 Moreover, it is estimated that approximately 50 to 70 million Americans suffer from sleep apnea,7one of several types of SRBDs that increase the likelihood of early death and several other medical comorbidities, including cardiovascular disease, type 2 diabetes, and renal disease, among others.8
To identify the large number of persons with SRBDs, dental practices need to screen their entire patient base, regardless of size, gender, or age, because sleep disorders impact patients of all types. Furthermore, proper screening protocols ensure that dental practices are compliant with the ADA position statement that encourages all practices to screen for SRBD.2 To screen for these conditions, practices should deploy validated screening tools, such as the Epworth Sleepiness Scale, the STOP-Bang questionnaire, or an appropriate sleep disorders assessment form that seeks to identify patients with sleep disorders beyond mild sleep apnea (Figure 1).
Physical Signs and Symptoms of Sleep Disorders
In addition to using self-assessment forms, clinicians and back-office team members should be trained to quickly identify and document known dental comorbidities of patients with SRBD. According to various peer-reviewed articles, these signs and symptoms include the following9,10:
• Narrow dental arch, high-vaulted palate
• Tooth crowding
• Class II malocclusion
• Occlusal wear (bruxing, grinding, and/or abfractions)
• Gastroesophageal reflux disease (GERD)
• Tongue-tie (ankyloglossia)
• Headaches
• Upper-jaw displacement
• Elongated uvula
• Dental tori
• Edentulism
• Overjet discrepancies
• Retrognathia or micrognathia
The Role of Digital Photographs in Sleep Dentistry
Most patients with sleep disorders are unaware of their condition. Therefore, if patients are found to be at risk after completing self-assessment forms or, if on examination, clinicians determine that patients may be at risk, the dental team should take the time to educate these patients on the reasons why they are suspected to be at risk and why a diagnostic evaluation of their sleep is necessary.
The author has found that incorporating a medical-grade digital photographic camera allows practices to take diagnostic photographs that document and identify the primary point of mid-facial collapsibility and oropharyngeal constriction for patients with sleep disorders. Moreover, the digital images serve as part of the medical record and assist patients in understanding why they may have these conditions. Digital images also allow for patient self-discovery within the oral cavity-for instance, tongue position and its effects on the airway, graded as Mallampati score. A high Mallampati score (class 3 or 4) is associated with a higher incidence of sleep apnea.11
The photographs that are taken chairside should be captured in a relatively small frame of time, legible so that soft and hard structures are properly documented, and available for access to a nearby computer for patient education or simply within the camera screen (Figure 2 and Figure 3).
CBCT and Sleep Disorders
In addition to taking digital images, the use of cone-beam computed tomography (CBCT) is strongly recommended by the author to properly identify the condition of the craniofacial complex and its impact on the entire upper airway. Peer-reviewed articles have found CBCT to provide accurate and reliable analysis of the upper airway.12,13
However, when using CBCT, practices must take caution to use the appropriate field of view (FOV) to capture all the necessary anatomy to obtain a meaningful analysis of the airway. Ideally, the CBCT FOV should be greater than 15 x 13 cm2, width by height.14 The appropriate FOV will capture the entire upper airway (starting from the tip of the nose and ending at the back of the throat, just below the epiglottis), the condyles, and the entire nasal cavity to help identify nasopharyngeal complications that may be keeping the patient from properly breathing through the nose or other contraindications that may prevent patients from being able to wear a sleep appliance (Figure 4).
Case Study
A patient was referred to the author̓s practice for evaluation of SRBD after his general dentist had begun clear aligner therapy. The patient had reported snoring and feeling tired before the aligner treatment; however, the treating dentist did not want to delay the aligner treatment and therefore included an SRBD evaluation as part of the dental treatment, referring the patient to the author's practice for assessment.
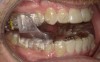
At the initial visit, the patient completed a sleep disorder assessment form, which revealed that he was at high risk of SRBD. Initial digital photographs included an airway Mallampati chairside diagnostic image that recorded an evaluation of visual tongue position (Figure 5); on physical examination, the patient presented with several known dental comorbidities for sleep disorders, such as a narrow upper and lower arch, minor tooth crowding, and mid-craniofacial collapsibility.
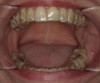
Five photographs documenting the condition of the mandible, jaw discrepancies, periodontal gingival condition, and Mallampati classification were obtained and loaded to the operatory computer. The photographs were then reviewed with the patient to explain why a sleep study was necessary. All images were then uploaded to the patient's chart and made part of the medical record for proper medical billing and reimbursement.
At that time, a sleep study was prescribed to record two nights of sleep behavior to rule in OSA. Home sleep studies have now become part of the diagnostic in the assessment of OSA in which the patient must have a sleep physician interpret the results and recommend treatment options for the referring dentist to review with the patient.
Results from the sleep study revealed that the patient experienced multiple apnea events (events where the patient stops breathing for 10 seconds or more). The interpreting physician diagnosed the patient with OSA with an apnea-hypopnea index (AHI) of 12.7/hr, which translates to a patient not getting any air approximately 13 times in an hour and stopping breathing for a cumulative 15 minutes (Figure 6). Options given by the interpreting sleep physician included CPAP treatment, surgery (soft tissue through removal of the uvula, drooping soft palate, or hard-tissue repositioning), or appliance therapy.
The patient was then recalled and the results of the sleep study were reviewed, and case acceptance was achieved after treatment options were presented to the patient. The patient had chosen to correct his malocclusion with the only custom US Food and Drug Administration (FDA)-cleared sleep appliance that allows for combination treatment of sleep apnea during clear aligner orthodontic movements without having to change the sleep appliance with every aligner change. Although the patient had the option of CPAP or even stopping the aligner wear during sleep and wearing a different OSA appliance, the patient after reviewing the digital images and the treatment modality with the combination treatment chose the option of continuing with the clear aligner and sleep appliance therapy and wearing the sleep appliance during sleep to address his sleep disorders as he underwent clear aligner treatment.
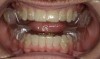
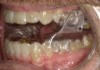
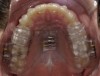
Intraoral scans were taken to document the patient's entire palate and bite registration. Scans were sent to the clinical team for the fabrication of a clear aligner/sleep appliance for the patient to wear; the chosen appliance fits over clear aligners, regardless of the tray number the patient may need (Figure 7 through Figure 11).
After the appliance was delivered, additional photographs were taken with the camera to ensure that the appliance was delivered as intended, to document the case, and to show the patient the ideal fit of the appliance in his mouth as instructions were reviewed with him.
After a few adjustments to the appliance were made and proper fit of the sleep appliance was ensured, the patient was sent home to report back later. The patient was stabilized with a follow-up report of positive sleep and not feeling daily fatigue, along with reduction or elimination of adjunct snoring. A follow-up sleep study confirmed that the patient was no longer experiencing apneic events.
Ten months after the appliance was delivered, the patient remained stable. The patient also completed clear aligner therapy and used retainers along with the clear aligner/sleep appliance during sleep. He remains under long-term care management protocol that monitors his progress for at least 2 years.
Conclusion
This article highlights the necessity to actively screen patients for SRBD, given the large number of patients who remain undiagnosed and may present to the dental practice. Implementing a digital workflow for patients with an SRBD ensures that medical procedures are properly documented using recent advances in digital imaging cameras and CBCT. The case detailed the appropriate sequence to manage patients diagnosed with sleep apnea and the ideal treatment for patients who are being treated with clear aligners and have sleep apnea.
About the Authors
Payam Ataii, DMD
Private Practice
Laguna Hills, California
Sal Rodas, MBA
Chief Product Officer, SleepArchiTx
Executive Director, Foundation for Airway Health
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Google Trends. https://trends.google.com. Accessed September 11, 2019.
2. ADA adopts policy on dentistry's role in treating obstructive sleep apnea, similar disorders [news release]. American Dental Association. https://www.ada.org/en/press-room/news-releases/2017-archives/october/ada-adopts-policy-on-dentistry-role-in-treating-obstructive-sleep-apnea. Published October 23, 2017. Accessed September 9, 2019.
3. Behrents RG, Shelgikar AV, Conley RS, et al. Obstructive sleep apnea and orthodontics: an American Association of Orthodontists white paper. Am J Orthod Dentofacial Orthop. 2019;156(1):13-28.e1.
4. Young T, Evans L, Finn L, Palta M. Estimation of the clinically diagnosed proportion of sleep apnea syndrome in middle-aged men and women. Sleep. 1997;20(9):705-706.
5. Benjafield AC, Ayas NT, Eastwood PR, et al. Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Respir Med. 2019;7(8):687-698.
6. Centers for Disease Control and Prevention. Sleep and sleep disorders. CDC website. https://www.cdc.gov/sleep/data_statistics.html. Updated May 2, 2017. Accessed November 15, 2019.
7. Extent and health consequences of chronic sleep loss and sleep disorders. In: Colten HR, Altevogt BM, eds; Institute of Medicine (US) Committee on Sleep Medicine and Research. Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem. Washington, DC: National Academies Press (US); 2006.
8. Pinto JA, Ribeiro DK, Cavallini AF, et al. Comorbidities associated with obstructive sleep apnea: a retrospective study. Int Arch Otorhinolaryngol. 2016;20(2):145-150.
9. Greenberg H, Lakticova V, Scharf SM. Obstructive sleep apnea: clinical features, evaluation, and principles of management. In: Kryger M, Roth T, Dement WC, eds. Principles and Practice of Sleep Medicine. 6th ed. Philadelphia, PA: Elsevier; 2017.
10. Soo-Lyun A, Ranson C. Obstructive sleep apnea for the dental hygienist: overview and parameters for interprofessional practice. Can J Dent Hyg. 2011;45(4):238-252.
11. Nuckton TJ, Glidden DV, Browner WS, Claman DM. Physical examination: Mallampati score as an independent predictor of obstructive sleep apnea. Sleep. 2006;29(7):903-908.
12. Vizzotto MB, Liedke GS, Delamare EL, et al. A comparative study of lateral cephalograms and cone-beam computed tomographic images in upper airway assessment. Eur J Orthod. 2012;34(3):390-393.
13. Ghoneima A, Kula K. Accuracy and reliability of cone-beam computed tomography for airway volume analysis. Eur J Orthod. 2013;35(2):256-261.
14. Rodas S. Proper use of cone beam imaging for upper airway analysis and management of sleep-related breathing disorders. Australasian Dentist. 2019;80:70-71.