You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
All practitioners performing minor or major surgical procedures want and expect ideal results. It can be frustrating when some patients seem to recover so much faster than others who have the same surgery under the same circumstances. Practitioners strive to decrease the number of complications during surgery. When results are less than ideal, they usually think about local factors that may influence healing, such as surgical technique, adequate blood supply, poor oral hygiene, or noncompliance with postoperative instructions. Although these are all plausible explanations for poor healing, there are several systemic factors that influence the ability to heal, with smoking and diabetes at the top of the list.
One factor receiving a lot of attention in the medical field in the past few years is the nutritional status of a patient. The goal of this article is to provide an update on how nutrition can influence postsurgical healing and present practices dentists can easily implement to enhance their patients’ healing following surgery, especially for dental implants.
Assessing Nutritional Status
Nutritional assessments are rarely performed on people facing surgery in medicine or in dentistry. A medical report called “Fit for Surgery” describes how preoperative malnutrition compromises surgical outcomes, and extreme weight loss can lead to postoperative morbidity and mortality. The authors of that report recommended that everyone on the multidisciplinary team understand that adequate nutrition contributes to successful surgical outcomes.1 This conclusion applies to members of the dental surgery team as well.
Assessing patients’ nutritional status starts with a detailed medical history. Most medical history forms do not include any nutritional information or questions about patients’ eating habits.
An important question to ask patients is whether or not they are on a special diet. For example, gluten intolerance is on the rise; currently about 20% of the population maintains a gluten-free diet.2 Patients who eliminate gluten-containing foods may be deficient in B vitamins, fiber, iron, and trace minerals found in complex carbohydrates, such as wheat-based products.3 Furthermore, there are some dental products that contain gluten, such as prophy paste and toothpaste. These should be avoided in patients with gluten allergy, as they can develop an inflammatory reaction. Vegan or vegetarian diets may also present problems in terms of healing if the patient’s protein and B12 intake are not adequate. A restricted caloric diet may be an issue if the patient is not receiving an adequate amount of nutrients. During healing, there is a 25% increase in total caloric requirements for metabolic function.4
In addition to questions focused on patients’ eating habits, it is also important to ask what kind of dietary supplements they take. In a survey of medical offices to determine how many doctors ask their patients about nutritional supplements, it was discovered that nearly 70% of the doctors do not ask their patients about the supplements they take.5 The majority of dental patients take at least one dietary supplement. Some supplements can cause excessive bleeding or may interact with the antibiotics and pain medication prescribed.
Table 1 includes recommended questions to assess patients’ nutritional status in the dental office. An increasing number of patients are seeing naturopathic doctors, integrative physicians, or nutritionists for supplement prescriptions. It is important to contact these professionals prior to dental implant surgery to review patients’ dietary supplement list as well as associated health conditions.
Prior to surgery, the patients should be assessed for wellness status, not just illness. Certain symptoms, such as hair loss and fatigue, can indicate major deficiency status, for which the patient should be referred to a nutritionist. A personalized nutrition plan can be implemented by assessing nutrients or metabolites via blood testing or urine, respectively.
Vitamin D and Healing
Vitamin D is a fat-soluble vitamin that can be produced endogenously from sun exposure and acquired via food or supplement intake. When ingested, vitamin D is biologically inert and must undergo hydroxylation to be activated for use in cellular function. The first reaction occurs in the liver and converts vitamin D to 25-hydroxyvitamin D3 (25(OH)D3), also called calcidiol. The second reaction occurs in the kidney and forms 1,25-dihydroxyvitamin D3 (1,25(OH)2D3), also known as calcitriol.6
In recent years, the role of vitamin D has been studied in systemic health as well as oral health. Systemically, vitamin D deficiency increases the risk for osteoporosis, high blood pressure, heart problems, allergies, colds and flu, mental health, and it has also been shown to play a vital role in cancer treatment.7 In a recent systematic review and meta-analysis of 9,700 patients, it was concluded that a level less than 50 nmol/L concentration of 25(OH)D was associated with increased rate of infection, sepsis, and mortality.8 Vitamin D modulates cell growth and immune function and it reduces inflammation.9 It can activate certain genes that regulate cell proliferation, division, and turnover.6
Vitamin D has also been shown to play an important role in bone mineral density. It promotes adequate calcium absorption in the intestines and maintains adequate levels of calcium and phosphate in the body for bone mineralization. This is especially important during dental implant osseointegration. Vitamin D is necessary for bone remodeling and the proper functioning of osteoblasts and osteoclasts.10
Since 1997, the recommended level of vitamin D daily supplementation has increased significantly.7 At that time, a maximum of 600 IU of vitamin D daily was recommended. The safe upper limit has been raised several times since then. The Institute of Medicine (IOM) doubled the safe upper limit from 2000 IU to 4000 IU of vitamin D per day.
It is important for the dental practitioner to understand how a patient’s level of vitamin D affects treatment, especially when it comes to surgery—whether it is dental implants or simply soft-tissue procedures. More and more studies are being published about vitamin D’s involvement in oral health. Because of the anti-inflammatory and antimicrobial properties of vitamin D, studies in recent years have focused on its impact on periodontal health and caries. One such study looked at 25(OH)D concentration in 920 postmenopausal women when assessing their periodontal status. Their vitamin D level was found to be inversely associated with gingival bleeding and level of periodontal disease.11 Other studies have confirmed this finding.
An in vitro study of osteoblasts in the presence of vitamin C and 1,25(OH)2D3 produced an extracellular matrix composed of collagen type 1 as well as osteocalcin and other proteins.12 Animal models (rats) have shown that the bone-to-implant contact ratio was significantly decreased in the group that was vitamin D insufficient.13
Assessing Vitamin D
The best indicator of an individual’s vitamin D status is serum concentration of 25(OH)D, because it has a half-life of 15 days. An IOM committee report addresses adequate levels of 25(OH)D.6 A serum concentration of less than 30 nmol/L is designated as a deficiency (Table 2). Ideally, serum concentration of 25(OH)D should be above 50 nmol/L. Certain studies have determined that a level of 80 to 100 nmol/L may be better, and in the near future, this level is likely to be increased.
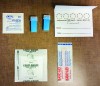
Vitamin D testing is easily accessible today. Several laboratories offer testing via dry blood spot, which is very accurate. A few drops of blood from a quick nick of the finger are placed on a filter paper to dry. Blood from a surgical site, such as a dental implant or extraction, can also be placed on the filter paper to be tested. Patients can also order a kit directly from the laboratory, and perform this test in the comfort of their home (Figure 1). Once the blood-spot sample is received by the laboratory, results are usually available in 1 week.
Micronutrient Deficiency Testing
In recent years, there has been a growing movement toward personalized medicine and nutrition to restore health. Many of those who claim to be healthy may in fact not be well; they may be suffering from poor vitamin/mineral intake or absorption, putting their bodies into suboptimal function. In the past 5 years, more than 17,000 articles published in medical journals have connected nutritional deficiency to high blood pressure, diabetes, immune problems, fibromyalgia, and even cancer.14 People’s individual nutritional requirements are based on genetics; age; level of activity; and intestinal absorption, transport, and storage of nutrients. This variability may help explain why it is very difficult to isolate single nutrients in a human study.
Multiple nutrients are involved in healing. Soft-tissue healing requirements vary slightly when compared to bone healing (Table 3 and Table 4).
The best way to determine an individual’s nutritional status today is via blood testing, such as that developed by Dr. William Shive, available through Spectracell Laboratories. A patented process measures long-term nutritional status by testing biochemical function rather than measuring serum concentrations. The test currently includes vitamins A, B1, B2, B3, B6, B12, C, D, E, K2, biotin, inositol, folate, pantothenate, asparagine, calcium, carnitine, choline, chromium, coenzyme Q10, copper, cysteine, fructose/glucose sensitivity, glutamine, glutathione, lip politic acid, magnesium, oleic acid, selenium, serine, total antioxidant function, and zinc.
It is ideal to encourage the patients to receive adequate nutrients from their diet rather than from supplements. Hippocrates once said, “Let food be thy medicine and medicine be thy food.” This still holds true today, and the nutritional community encourages patients to adopt a healthy, well-balanced diet first, and then supplement as needed. However, the reality is that most patients do not get enough nutrients from their food. The lab report from the micronutrient testing contains food groups that will replenish a specific nutrient deficiency uncovered during their testing. This makes it easy for the practitioner to give a recommendation.
Several companies make formulations for postsurgical recovery. A word of caution regarding the recommendation that patients take multivitamins: Patients on blood thinners should avoid vitamin K supplements, as these may counteract the effects of the blood thinner.
Enzymes and Healing
Enzymes, which are involved in healing as in nearly all processes in the body, decrease in number and functional ability with age. Their ability to function depends on vitamins and minerals, which serve as coenzymes. The use of enzymes as an aid for digestion is well known, but in recent years, research on enzymes has proven their importance in decreasing inflammation.
Enzymes are classified into six groups, based on their function: hydrolases, lysases, oxidoreductases, transferases, isomerases, and ligases. Among these, proteases, amylases, and lipases play an important role in postsurgical repair. Postsurgically or post–acute trauma, proteins must be replaced. An inflammatory reaction sets in and the synthesis for fibrin, thrombin, kinin, and plasmin increases. Enzymes are used for this synthesis. Deficiencies in enzymes can result in a longer period of inflammation in pain. Oral use of proteolytic enzymes can accelerate healing by up to 50%.15
Several studies have shown that enzymes can have similar effects to nonsteroidal anti-inflammatory drugs (NSAIDs). Although NSAIDs relieve pain, they also slow tissue repair by suppressing the inflammatory response, which is essential to the wound healing process.16
Bromelain is a protease enzyme derived from the pineapple stem, which has been getting a lot of attention due to its anti-inflammatory properties. Several studies examined its effectiveness after wisdom tooth extraction, and it was determined to have similar results in decreasing pain and inflammation as NSAIDs but without the gastrointestinal side effects.17,18 The recommended dose is 500 mg three times a day taken on an empty stomach. Doctors should avoid prescribing bromelain for patients who are allergic to pineapple.
Other formulations of enzymes on the market are specifically designed for inflammation reduction and healing. Their benefit in relation to oral surgery has not yet been studied. The research in this field continues in the hopes of providing patients a better alternative to medications.
The Postsurgical Diet Plan
The author recommends urging patients to eat specific foods to promote healing postsurgically. Eating nutritious foods after oral surgery—which calls for a softer, not spicy, and less acidic diet—can be difficult. The typical soft diet includes mainly simple carbohydrates such as mashed potatoes or processed foods that are high in sugar, such as gelatin, pudding, and yogurt. A diet high in sugar delays wound healing and increases the risk of infection.19 When blood sugar level is between 100 and 140 mg/dL pre- and postsurgery, faster healing and fewer complications are observed.20
An ideal postoperative diet consists of foods rich in antioxidants and phyto-nutrients to offset the oxidative stress caused by surgery. Good sources of protein, healthy fats, and complex carbohydrates are equally important.16
The Future of Nutrition
With the modern advances in medicine, nutrition received less attention as medical professionals focused more on their area of medical specialty. However, given the limitations and side effect of medication, nutritional advances are proving to be very helpful in postsurgical and post-injury recovery. In the next few years, the need for nutritional testing and individualized supplement plans is likely to grow, and an increasing number of clinicians will be prescribing dietary supplements.
The field of stem cell research is growing at a rapid pace, and an interesting set of supplements is emerging in the field of stem cell nutrition. It has been demonstrated that the number of adult stem cells in the blood can be increased by taking certain dietary supplements. Increasing the number of circulating stem cells accelerates healing of second-degree burns and speeds up bone healing from fractures. Scar formation also depends upon the number of stem cells available for repair.21 Certain factors affect the number and release of stem cells from the bone marrow: adequate sleep, a good diet, and antioxidant nutrition. An algae extract from Aphanizomenon flos-aquae (AFA) is showing promising results in supporting the natural release of stem cells from the bone marrow during healing.22 Compounds such as cats claw, devils claw, ginger, and curcumin are also being studied.
Americans are living longer and they are increasingly interested in how to live a healthier life. As health care costs continued to increase, and patients seek information from the Internet more than ever, it is important to stay up-to-date in the nutrition and dietary supplements field.
About the Author
Dr. Moldovan is an award-winning periodontist and nutritionist. An Ohio State University School of Dentistry graduate, Dr. Moldovan continued her studies at UCLA’s Post Graduate Periodontics Department, where she also received a Masters of Science in Oral Biology. She is a diplomate of the American Academy of Periodontology and a certified nutritionist. Dr. Moldovan is a member of the Academy of Laser Dentistry, American College of Nutrition, and Academy of Anti-Aging Medicine. She serves patients at her office in Los Angeles, California.
Dr. Moldovan frequently lectures on dental implants and nutritional for a healthy mouth at the UCLA School of Dentistry and is a faculty at Global Institute for Dental Education. She stays on top of her field’s latest research and technology, particularly laser techniques, minimally invasive techniques in dental implant surgery, periodontal plastic surgery, and nutritional support.
References
1. Windsor A, Braga M, Martindale R, et al. Fit for surgery: an expert panel review on optmising patients prior to surgery, with a particular focus on nutrition. Surgeon. 2004;2(6):315-319.
2. Koch KM. Beyond Gluten Intolerance: GIS - Gluten Inflammatory Syndrome. 1st ed. Ashland, OH: Bookmasters, Inc.; 2012:711.
3. Theethira TG, Dennis M. Celiac disease and the gluten-free diet: consequences and recommendations for improvement. Dig Dis. 2015;33(2):175-182.
4. Sroda R. Nutrition for a Healthy Mouth. 2nd ed. Philadelphia, PA: Lippincott, Williams & Wilkins;2009.
5. Donaldson M, Touger-Decker R. Dietary supplement interactions with medications used commonly in dentistry. J Am Dent Assoc. 2013;144(7):787-794.
6. AC Ross, CL Taylor, AL Yaktine, HB Del Valle, eds. Dietary Reference Intakes for Calcium and Vitamin D. Institute of Medicine website. www.iom.edu/reports/2010/dietary-reference-intakes-for-calcium-and-vitamin-d.aspx. Accessed May 22, 2015.
7. Levine SA. A spoonful of sunshine: the vitamin D picture matures. Optometry Care Santa Barbara website. www.optometrycaresb.com/article/826-a-spoonful-of-sunshine-the-vitamin-d-picture-matures. Accessed May 22, 2015.
8. de Haan K, Groeneveld AB, de Geus HR, et al. Vitamin D deficiency as a risk factor for infection, sepsis and mortality in the critically ill: systematic review and meta-analysis. Crit Care. 2014;18(6):660.
9. Holick MF. Vitamin D. In: Shils ME, Shike M, Ross AC, et al., eds. Modern Nutrition in Health and Disease. 10th ed. Philadelphia, PA: Lippincott, Williams & Wilkins; 2006: 376-395.
10. Vitamin D fact sheet for health professionals. National Institutes of Health Office of Dietary Supplements website. http://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/. Accessed May 22, 2015.
11. Millen AE, Hovey KM, LaMonte MJ, et al. Plasma 25-hydroxyvitamin D concentrations and periodontal disease in postmenopausal women. J Periodontol. 2013;84(9):1243-1256.
12. Doglioli P, Scortecci G. Characterization of endosteal osteoblasts isolated from human maxilla and mandible: an experimental system for biocompatibility tests. Cytotechnology. 1991;7(1):39-48.
13. Kelly J, Lin A, Wang CJ, et al. Vitamin D and bone physiology: demonstration of vitamin D deficiency in an implant osseointegration rat model. J Prosthodont. 2009;18(6):473-478.
14. Fairfield KM, Fletcher RH. Vitamins for chronic disease prevention in adults: scientific review. JAMA. 2002;287(23):3116-3126.
15. Loomis HF Jr. Enzymes: The Key to Health, Vol. 1. Madison, WI: Enzyme Formulations, Inc. 2005.
16. Motyka EG, Motyka TM, Mead MN. The Rapid Recovery Handbook: Your Complete Guide to Faster Healing After Surgery. 1st ed. New York, NY: HarperCollins Publishers; 2006:304.
17. Inchingolo F, Tatullo M, Marrelli M, et al. Clinical trial with bromelain in third molar exodontia. Eur Rev Med Pharmacol Sci. 2010;14(9):771-774.
18. Majid OW, Al-Mashhadani BA. Perioperative bromelain reduces pain and swelling and improves quality of life measures after mandibular third molar surgery: a randomized, double-blind, placebo-controlled clinical trial. J Oral Maxillofac Surg. 2014;72(6):1043-1048.
19. Lioupis C. Effects of diabetes mellitus on wound healing: an update. J Wound Care. 2005;14(2):84-86.
20. Rai NK, Suryabhan, Ansari M, et al. Effect of glycaemic control on apoptosis in diabetic wounds. J Wound Care. 2005;14(6):277-281.
21. Drapeau C. Cracking the Stem Cell Code: Adult Stem Cells Hold the Promise of Miraculous Wellness. Ontario, Canada: The Natural Wellness Group Publishers; 2013:282.
22. Jensen GS, Hart AN, Zaske LA, et al. Mobilization of human CD34+ CD133+ and CD34+ CD133(-) stem cells in vivo by consumption of an extract from Aphanizomenon flos-aquae-- related to modulation of CXCR4 expression by an L-selectin ligand? Cardiovasc Revasc Med. 2007;8(3):189-202.