You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
In the last 60 years, composite resin restorations have increased significantly, overtaking amalgam restorations. A variety of reasons account for the increase in composite resin restorations, including less preparation, ease of use, minimal invasive procedures, and more natural appearance.1 Although studies have shown that mercury poisoning is not a concern with amalgam restorations,2,3 anecdotal support has given patients the desire to move away from metal fillings.
This article will describe the types of composite resins. It will also compare posterior amalgam restorations to composite resin restorations and address how to deal with potential postoperative sensitivity and posterior interproximal contacts. It will also explore the option of bulk filling restorations, as well as the advantages and disadvantages of universal adhesives.
Types of Composite Resins
There are currently five types of composite resins: microfills, microhybrids, hybrids, packables, and flowables.4 It is important to select the most appropriate composite resin for the restoration being performed. Each has its own benefit.
Microfills are considered to be the most esthetically pleasing restorations because of their ability to simulate the enamel surface of the tooth and polish to a high luster, which is a result of them having the smallest average particle size of any composite resin on the market. They are also more resistant to stains and plaque, making them more biologically compatible with gingival tissue. Additionally, they produce more translucency due to their high reflective and refractive indices. However, they are less filled than other composite resins, meaning they will not be as strong.5
Microhybrids and hybrids have higher-strength properties than microfills due to their larger particle size. Additionally, they simulate the dentin of natural tooth structure better than other composite resins. Because of these benefits, they are ideal to use in supporting the microfill enamel layer. Additionally, they can be very opaque, allowing for the masking of unwanted color. However, they are not as easy to polish and wear faster than microfill resins. Additionally, they are not as esthetically pleasing on the enamel layer. The main difference between microhybrids and hybrids is their particle size, with hybrids having a larger particle size than microhybrids.6
Packable composite resins were initially introduced as a composite that would handle similarly to amalgams, while helping to resolve the issue of inefficient contacts that occurred when using composite resins. Although packables were considered to result in successful contacts with Class I and II restorations, they fell short with interproximal contacts. They are more viscous than most composite resins and have a large particle size, but they are shown to wear over time.7 Additionally, packable composite resins have similar or higher rates of polymerization shrinkage than non-packables; therefore, they are thought to perform less successfully.8
The last type of composite resin is flowable (Figure 1). Flowables have a lower viscosity than other composite resins.9 Benefits of flowables include penetration into every abnormality due to the low viscosity, ability to form layers of minimum thickness and thereby improve or eliminate air inclusion or entrapment, high flexibility, radiopacity, and a variety of available colors. Disadvantages include high curing shrinkage, which can be attributed to lower filler load, as well as weak mechanical properties.10Taking both their advantages and disadvantages into account, it is recommended that flowables be used as a liner in Class II and V restorations to form a seal, which may help prevent postoperative sensitivity and secondary caries. They also help prevent microleakage when used in conjunction with an additional composite resin.11
Dental Amalgam Versus Composite Resin
Before the 1990s, most dentists chose dental amalgam for fillings. More recently, however, the use of composite resins has exceeded the use of amalgams by a 2-to-1 ratio.12 Studies show that the use of amalgams is continuing to decline.12Although there is debate about whether composite resins are better than amalgams, both seem to perform comparably, with research showing that amalgams may last even longer than composite resin restorations.13 Part of the explanation for the increase in use of composite resins is the esthetic factor. Amalgam fillings are made from mercury, silver, copper, and tin, making them a silver color and, therefore, more obvious to spot in the mouth. Composite resins are made of ceramic and plastic compounds, resulting in a white restoration.14 Patients often prefer the more natural look that composite resins offer.
Additionally, dentists can be more conservative with composite resins by doing smaller fillings or simply targeting the decay. Another benefit of composite resins is that, unlike with amalgams, dentists do not need to perform the added steps of resistance and retention form. Previously, composite resins had only been used in restorations of front teeth because of their limited durability. However, in the last 10 years, composite resins have improved in reliability and durability. The physical properties of hardness, flexural structure, fracture resilience, lower shrinkage rates, and lower wear have since made composite resins a viable option for posterior restorations.15
Yet even with improvements to the material, polymerization shrinkage still poses some issues, particularly with larger posterior restorations. Shrinkage may lead to marginal defects and gaps, regardless of how carefully the composite resin is applied. This, in turn, can lead to microleakage, which may cause secondary caries, pulpal irritation, postoperative sensitivity such as pain when chewing and sensitivity to cold, and marginal discoloration.
In addition, placing posterior composite resins can be tedious and unpredictable. The process includes achieving the necessary isolation, selecting and placing the appropriate matrix, precise execution of the adhesive steps, the placement of a flowable resin or resin ionomer liner, and the incremental placement, adaptation, and light-curing of two or more layers of composite resin. Additionally, one must sculpt, adjust the occlusion, and finish and polish.12 The numerous steps make composite resin restorations much more technique-sensitive than amalgam restorations. Additionally, composite resin restorations tend to cost more than amalgams.
Postoperative Sensitivity With Composite Resin Restorations
Postoperative sensitivity is one of the main concerns of composite resin fillings. The sharp pain that can be experienced usually occurs only when chewing hard foods. Occasionally, there is a lingering sensitivity to cold as well. Eating soft foods, grinding, or clenching teeth does not generally result in pain. There are few explanations as to why postoperative sensitivity may occur. The type, size, and design of the cavity, as well as material properties and handling techniques, can all contribute to postoperative sensitivity.16
Certain procedures can increase the likelihood the patient will experience postoperative sensitivity, specifically procedures that leave dentinal tubules and collagen exposed during restorations. When tubules are exposed to cold, heat, substances that create an osmotic gradient, or mechanical stimuli, fluid within the dentinal tubules can move and stimulate odontoblasts and nerve fibers located in the tubules near the pulp.17 Additionally, studies have shown that cavity depth can be a strong contributor to postoperative sensitivity.18
Other restoration procedures in which patients most often complain about postoperative sensitivity include Class I, II, and V restorations, particularly large and deep tooth preparations; lithium disilicate crowns, onlays, or inlays cemented with composite resins using a total-etch technique; crowns cemented with self-etch resin cements; and moderate- to large-sized direct or indirect deep restorations placed without a base or liner and with only a bonding agent on the deepest areas.19
According to studies, an application of glutaraldehyde-containing solutions for two 1-minute increments at the appropriate step of the procedure kills organisms on the tooth, which can help prevent postoperative sensitivity. However, it may not be completely eliminated.20,21
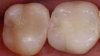
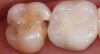
Dental professionals can increase the longevity of composite resin restorations, decrease the chance of postoperative sensitivity in patients, and achieve desired esthetics. Possessing knowledge of scientific evidence and detailed diagnostics, planning correct treatments, and having experience with various techniques, restorative materials, and their clinical indications are essential to achieving successful restorations with minimal postoperative sensitivity (Figure 2).
Posterior Interproximal Contacts With Composite Resin Restorations
Another potential issue of unpredictability in composite restorations is proximal contacts and the placement of matrix bands. Proximal contacts, which support the interproximal papillae, are important both for supportive and protective reasons. They help deflect trauma. An inadequate contact can lead to plaque accumulation and incipient caries, thereby aggravating food impactions and causing damage to the interproximal tissues, drifting of adjacent teeth, and root proximity issues.22
Because of the importance of proximal contacts, it is first imperative to understand characteristics of a successful interproximal contact. The contact should be centered buccolingually below the marginal ridges, highly convex in its middle and occlusal thirds, and flat or concave in the cervical third. Additionally, if there is gingival recession, the tendency is for the cervical third to have a concave form.
Difficulty in creating a good proximal contact can be attributed to the material of the composite resins. They are often viscous and not predictably compactable. In the case of Class II restorations, even the most viscous packable composite resins are unable to adequately and predictably move the matrix band to establish a proper contact form.23
In the past, the most common technique for creating proximal contacts has been applying thin dead-soft stainless-steel matrix bands, which fit circumferentially around teeth. However, using this technique poses additional challenges, such as the time it takes to prepare the matrix band, inconsistent resulting contacts, and occasional instances in which one may not be able to use rubber dam isolation with the circumferential matrix band system.
Because of these drawbacks, a newer class of sectional matrix has been introduced (Figure 3). An ultra-thin dead-soft stainless-steel sectional matrix may be used concurrently with a ring designed specifically to create additional tooth separation, allowing the sectional matrix to form a strong contact with the adjacent tooth. Additionally, the ring redesign allows the matrix to be used in restorations of all sizes. Another benefit is that the dentist can place a wedge, which is available in three different sizes, before or after placing the ring. Because of the design, the wedge does not impinge on the interdental papilla, pushing the matrix band against the cervical portion of the box, resulting in a tighter marginal seal. The rings, sectional matrices, and wedges are designed for easy handling, pickup, and better control during placement and removal. They also come with a hole designed specifically to accommodate forceps.
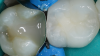
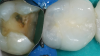
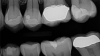
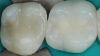
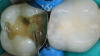
When performing multiple adjacent restorations, preliminary assessments must be made to achieve a successful contact. First, a dental professional must use visual (Figure 4) and radiographic analysis (Figure 5) to establish the location and extent of the caries and assess the adjacent teeth for normal anatomy. Protection of the adjacent teeth during preparation to preserve anatomy and maintain a smooth surface must be ensured, which will help in reducing plaque accumulation. Afterwards, teeth should be prepared with an efficient sequence, and the type and location of matrices should be determined. Next, sequences of steps should be established if adjacent contacts must be restored to ensure that successful anatomic contours are reconstructed. Then a pre-etch technique should be used to optimize the seal of the occlusal portion of the restoration. An adhesive seal of the resin to the tooth structure may be created with a reliable adhesive system, and sectional matrices can be used to form tighter contacts in posterior resin restorations.
Bulk Filling Composite Resin Posterior Restorations
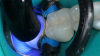
The bulk-filling technique (Figure 6) emerged several years ago as a replacement for more difficult, time-consuming incremental placement techniques. The advantage of bulk filling is that it allows dentists to place large quantities of composite resin at once.24 However, because of the larger quantities being used, it is important to make sure the resin is adequately cured (Figure 7) in order to prevent white lines at the margins and reduce shrinkage, which could lead to gaps, leakage, cracks, or postoperative sensitivity.25
Research shows that proper use of high-intensity lights will cure a range of 4.5 mm to 9.5 mm of resins, according to Gordon J. Christensen, DDS, MSD, PhD.24 He recommends checking the depth of cure in the light being used with the resin being used through the following procedure: place the quantity of resin normally used about 10 mm high and 5 mm in diameter on a piece of paper; place the light tip directly over the resin and cure the resin for the time normally cured; after curing, scrape the bottom part of the resin sample with an instrument, such as a sharp laboratory knife, and remove the soft resin; continue scraping until the process becomes difficult and one seems to be cutting into the cured resin instead of the soft, partially cured resin; measure the depth of cure. Although Christensen warns this is not a precise test, it will provide some indication of the curing ability of the light being used.
Universal Adhesives
Universal adhesives (Figure 8) are designed to work with most procedures, including indirect and direct restorations, desensitization, sealants, and restoration repairs. They allow bonding to any substrate or material, with the exception of high noble metals, without compromising bonds to dentin.26 They can also be used in any etching mode, including total, selective, or no etching, as well as in procedures requiring light-cure, dual-cure, or self-cure. Additionally, they work in wet, dry, or moist environments. They use a quick application method with no rinsing, and they reduce postoperative sensitivity and microleakage.27 However, they also have some disadvantages: they do not bond well to enamel and sclerotic dentin.28
Conclusion
Although there are still potential problems with using composite resins in posterior restorations, these materials continue to increase in popularity due to their ease of use and esthetic advantages. Consequently, manufacturers of composite resins are improving their materials and working to solve issues that may arise. These materials are becoming increasingly predictable and reliable as they are continuously being improved to allow simplification of use.
About the Author
Jason Olitsky, DMD
Private Practice
Ponte Vedra Beach, Florida
References
1. Milnar FJ. The evolution of direct composites. Compend Contin Educ Dent. 2011;32(1):80-81.
2. Rathore M, Singh A, Pant VA. The dental amalgam toxicity fear: a myth or actuality? Toxicol Int. 2012;19(2):81-88.
3. National Institutes of Health. Effects and side effects of dental restorative materials. NIH Technol Assess Statement Online 1991;(9):18. https://consensus.nih.gov/1991/1991DentalRestorativeMaterialsta009html.htm. Accessed August 1, 2018.
4. Abel MG. Predictable contacts with composite resins. Dent Today. 2004;23(4):72-74.
5. Mopper KW. Let's talk composites! Dent Today. 2008;27(10):118-122.
6. Guilherme S, Strassler H, Webley W. Direct composite resins. Inside Dentistry. 2007;3(7):76-79.
7. Burgess JO, Walker R, Davidson JM. Posterior resin composite restorations. Pediatr Dent. 2002;24(5):465-479.
8. Choi KK, Ferracane JL, Hilton TJ, Charlton D. Properties of packable dental composites. J Esthet Dent.2000;12(4):216-226.
9. Flowable composites. Ivoclar Vivadent. www.ivoclarvivadent.in/zoolu-website/media/document/8648/Flowable+composites. Accessed July 16, 2018.
10. Baroudi K, Rodrigues JC. Flowable resin composites: a systematic review and clinical considerations. J Clin Diagn Res. 2015;9(6):ZE18-ZE24.
11. Margolis FS. Flowable composites: aesthetics for tots and teens. Dent Today. 2011;30(4):132-137.
12. Jackson RD. Placing posterior composites: increasing efficiency. Dent Today. 2011;30(4):126-131.
13. Shenoy A. Is it the end of the road for dental amalgam? A critical review. J Conserv Dent. 2008;11(3):99-107.
14. The facts on fillings: amalgam vs. resin composite. Delta Dental. https://www.deltadentalins.com/oral_health/amalgam.html. Updated January 2017. Accessed July 16, 2018.
15. Ibarra ET, Lien W, Casey J, et al. Physical properties of a new sonically placed composite resin restorative material. Gen Dent. 2015;63(3):51-56.
16. Briso AL, Mestrener SR, Delício G, et al. Clinical assessment of postoperative sensitivity in posterior composite restorations. Oper Dent. 2007;32(5):421-426.
17. Platt JA. Reducing postoperative sensitivity associated with composite dentistry. Dental Economics.2016;106(11):71-73.
18. Auschill TM, Koch CA, Wolkewitz M, et al. Occurrence and causing stimuli of postoperative sensitivity in composite restorations. Oper Dent. 2009;34(1):3-10.
19. Christensen GJ. Preventing postoperative tooth sensitivity. Dental Economics. 2014;104(11):26-29.
20. Porto ICCM, Andrade AKM, Montes MAJR. Diagnosis and treatment of dentinal hypersensitivity. J Oral Sci. 2009;51(3):323-332.
21. Sobral MAP, Garone-Netto N, Luz MAAC, Santos AP. Prevention of postoperative tooth sensitivity: a preliminary clinical trial. J Oral Rehabil. 2005;32(9):661-668.
22. Rosenberg JM. Making contact: a method for restoring adjacent posterior direct resins. Dent Today. 2013;32(3):92-95.
23. Simos S. Making contact just got easier. Making Class II composite restorations more predictable. Dent Today. 2012;31(9):106-109.
24. Christensen GJ. Does "bulk filling" work for composite restorations? Dental Economics. 2017;107(1):55-58.
25. Teel T. Bulk-fill composites: a step-by-step case presentation. Perio-Implant Advisory. https://www.perioimplantadvisory.com/articles/2014/01/bulk-fill-composites-a-step-by-step-case-presentation.html. Published January 7, 2014. Accessed July 16, 2018.
26. Lively T. 7 things you may not know about universal adhesives. Dental Products Report. http://www.dentalproductsreport.com/dental/article/7-things-you-may-not-know-about-universal-adhesives. Published April 12, 2017. Accessed July 16, 2018.
27. Sesemann MR. Efficient posterior restorations with selective etching, universal adhesive, and bulk-fill composite. Dental Economics. https://www.dentaleconomics.com/na/ivovlar-vivadent/efficient-posterior-restorations.html. Published March 20, 2017. Accessed July 16, 2018.
28. Vakay R, Delgado A, Marongiu N. Are universal adhesives really universal? Compend Contin Educ Dent. 2017;38(1):14-15.