You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Mastering Direct Restorations: How to Navigate Critical Advancements in Composites and Adhesives
Dentistry is constantly evolving, especially in regard to new restorative materials. Each year, manufacturers conduct extensive research before putting products on the market that improve the materials dentists are using. Restorative materials in particular have gone through immense change to provide better-quality restorations and improved longevity for patients. Dentists also reap benefits in that the materials are becoming less technique-sensitive. The new materials allow results to be achieved more easily and have overall better handling properties. However, the advancements also result in dentists increasingly experiencing the paradox of choice between different composites and dentin adhesives. It is difficult to know whether one should remain with the materials already in use or transition to the next generation of materials. This article provides an overview of advancements in direct restorative materials such as composites and adhesives as a guide for dentists to explore all options.
Critical Aspects of Composite Materials
In the full scope of direct restorative materials available today, the main material for most dentists is composite. All composite resin materials, at their essence, are similar. They consist of organic resin matrix, filler particles, and coupling agent. The physical properties are determined by the characteristics and mix of the matrix and filler particles.1-6 The chemistry may depend on the photoinitiator, or it may depend on the add-ins that are designed to delay the setting in room light so the composite only responds to light from curing units.7,8 The chemical composition could also result from the coupling agents that hold everything together or components that add color or esthetics to the material.
A composite material should ideally wear as closely to natural enamel as possible. It should not wear down faster than the surrounding tooth structure or contribute to wear in the opposing tooth structure. In the oral environment, how materials will fare in a moist setting is of primary concern. As filler content decreases, negative factors begin to emerge. The material must not have a high level of water absorption that could lead to breaking down and changing physical properties in the oral environment. Additionally, shrinkage stress is critical. For many years, the terminology used to describe this phenomenon was polymerization shrinkage.9,10
With newer composite materials, many improvements and advancements have occurred. In assessing the flexural strength of the material, how it bends, flexes, and moves in response to the forces placed on teeth are integral. These qualities also make the bond to the tooth more durable. If the flexural strength of the materials is similar to the tooth, there is no stress that accumulates at the adhesive interface and marginal breakdown does not occur as quickly. Composites are less likely than ceramic materials to fracture or break in the oral environment.11 Polishability is another essential factor.
A composite is, at its core, an esthetic restorative material. Dentistry has transitioned to relying on composites more heavily for two main reasons. First, because composites are adhesively placed, preparations can be more conservative; more natural tooth structure can be conserved while esthetics are maximized. Second, because the color of the composite is similar to the tooth, restorations can more closely mimic natural esthetics. Nevertheless, some particular types of composites are more esthetic than others. Because composites share an emphasis on esthetics, it can be challenging to determine superiority between the different materials.
The Evolution of Composite Materials
The evolution of composite materials goes back to materials that were basically toothpaste. A base and catalyst were mixed together. Those materials can still be found today, although they are rarely used because there are now other options, such as nanohybrid, nanofill, nanocluster, and bulk fill. These options were developed over many decades of scientific research into optimizing composite physical properties, handling properties, and the balance between resin and filler. All these improvements are closely tied to the percentage of filler compared with resin.
As the filler content decreases, the material absorbs more water and is less durable in the oral environment. The bulk amount of polymerization shrinkage and the amount of that shrinkage that stresses the bonded interface then increases. This means there will be more strain on the adhesive interface, and therefore there is much faster marginal breakdown, leakage, secondary caries, and need to replace the restoration. The flexural strength also decreases, which means that the material will be less bendable and capable of taking flexural load. Stress accumulates at the bonded surface and breaks down the seal of the restoration to the tooth.12
At the same time, the material's ability to resist fracturing decreases, and it becomes more prone to fracture.13,14 The viscosity also decreases; however, lower viscosity is a handling property that dentists may prefer. Materials that have low viscosity demonstrate a runny, liquidlike consistency. Flowables are an example of a type of composite that fits into the lower-viscosity category. This handling property is one of the bonuses of having less filler, but as the filler content decreases, valuable physical properties that make materials more durable in the oral environment are lost.12
Conversely, as the filler content increases, water absorption and shrinkage stress decrease while the flexural strength and fracture toughness increase.12 Arbitrarily, the viscosity increases as well, and there is a limit to how viscous the composite can be and still be usable. Most of the evolution of composites has occurred with filler particles. Finding the right blend of sizes, shapes, and types of particles to create a combination with ideal high filler content has been the primary aim. The main challenge has been maximizing and improving the physical properties of the material without making it so viscous that it cannot be used.
Composites that are dry, crumbly, or too tough cannot be placed properly in the oral environment. Materials first transitioned from macrofills and macrohybrids to microfills and microhybrids and then down to the current realm of nanosized particles. The primary learning during this evolution has been that the smaller the particles are, the higher the filler percentage can be to maintain a viscous, manageable texture. The significantly smaller particles have positively improved other properties as well. Previously, the macro particles would undergo a process called stripping, wherein as filler particles were removed on the occlusal table, a pitted appearance would occur. With nanosized particles, composites avoid stripping and have much better handling properties.12
Composite Fillers and Resin Matrix
Current composite fillers are usually deemed nanofill, meaning that all particles are in the nano range and identical in size. Nanofill can be contrasted with nanohybrid, which means that all particles are in the nano category but that there are a variety of different particle sizes. Occasionally, there are products called nanocluster. These fillers involve a process whereby the material is polymerized, broken up again, and put back in the material.
There are many different types of filler particles. In the majority of cases, these particles fall into the category of glass or silica-based. Today, the phrase ceramic filler is often used, which is basically another term for glass or silica filler. There is interest in zirconia particles as a filler, which is appealing because zirconia is a high-strength ceramic. What is most important in the filler category is the size of the particles rather than the type.
For composite materials, another important component is the resin matrix. In recent years, attention has been placed on the disadvantages of the resin matrix due to fear of exposing patients to bisphenol A (BPA). Patients are becoming increasingly more informed about dental materials and are demonstrating concern about those that contain BPA. It may be accurate to answer that composites do not have BPA in them, but this response leaves out some shades of grey because the resin matrix is often made from a component called bisphenol A-glycidyl methacrylate (bis-GMA) or bisphenol A dimethacrylate (bis-DMA). These resins can break down, producing BPA and leaching it back out.15 For BPA-conscious patients, other materials on the market use a different type of resin. Specifically, urethane dimethacrylate (UDMA) is a popular alternative.
To fully understand the physical makeup of composites, it is useful to dive into the variances between microfill, nanofill/nanohybrid, and flowable. Microfill composites were first brought onto the market in 1974. Since then, they have been quite popular, with many dentists still finding a place for them in their practices today. A microfill has a much larger filler particle size (0.02 to 0.04 μm) than composites in the nano category, along with good, though not excellent, wear resistance.12 Potential disadvantages include a reasonably low flexural strength or modulus of elasticity and high rates of polymerization shrinkage compared with nano materials.12 Nevertheless, microfill products can be beneficial for the 0.5-mm enamel layer, specifically for anterior composites that are on the labial.12
The reason microfills are optimal for this particular situation is their high polishability.16,17 They are easy to polish and maintain a polished surfaced even after toothbrushing and the movement of the patient's lip against the composite. In the author's experience, a microfill is good with enamel shades on the labial surface of a Class III or Class IV restoration. Nothing in any of the other categories of composites is comparable to the esthetic polishability of a microfill. Unfortunately, microfills are not suitable for a posterior, Class I, or Class II scenario. They should not be used to hold an occlusal contact.
Today, the workhorse composites in many dental offices are in the nano category (5- to 75-nanometer particles): nanofills and nanohybrids. These products have a much higher filler percentage without being too viscous, which results in outstanding physical and handling properties.18,19 Most also have advantages ranging from a good polish and gloss retention to esthetics and durability in the oral environment. These composites are suited to Class I, Class II, Class V, and Class III anterior restorations that are restricted to the lingual, especially if there is natural tooth structure on the labial. There are also many options for delivery systems of these composites. It is helpful if they can be placed in a composite gun to inject them, but they can still be delivered to a restoration with a syringe and a plastic instrument. In the author's opinion, nanofills and nanohybrids have an ideal balance of esthetics, physical properties, and handling properties.
Most composites in this category are appropriate for anterior and posterior restorations. For example, when using a kit that contains a full range of colors, the clinician can buy a single type of composite for the office. Because the composite is gel-like, it can be used whether it is designed for anterior or posterior. The most common shades for the posterior tend to be A1, A2, and B1, which is why an entire spectrum of shades is not always necessary. There is usually very little need to layer opaque dentin and enamel shades, yet having a system like this available ensures an inventory of basic shades that can be used daily for anterior esthetic results.
One area that has seen considerable advancement in composite science and materials is flowables. What was once a term with a single meaning has now grown to encompass multiple different types of composites. The traditional flowable composite that has been on the market for at least 15 years is still available. It is a low-fill material classically designed for use in very low-stress areas, almost as a liner beneath more traditional composite. It can be married to a temporary material such as bis-acryl for repair of voids or to provide a custom fit for the margins. In addition to traditional flowable materials, there are high-fill flowables. These do not have a filler percentage approaching the amount found in composites that come in a syringe or have to be placed with an instrument or condenser, but they do have a higher percentage than the very low-fill flowable.
The viscosity of flowables is important because if they are too liquid, they will not hold their shape on a mixing pad. Flowables that are more viscous have a texture akin to ice cream that holds its shape, which is a result of the additional filler material. There are also flowable restorative materials that are rated by the manufacturer for standalone restorations such as small Class I and Class V restorations. It is important to clarify whether the flowable has low physical properties that make it ideal as a liner or repair for temporaries or whether it is capable of acting as a standalone in small, conservative preparations. It is likely that clinicians will need more than one type of flowable composite in their office due to the differences in viscosities and physical properties between materials. Classic flowable materials would come in a syringe, but now there is flowable that can be placed in a composite gun.
Bulk-Fill Composites
With bulk-fill flowable materials, the nature of their use requires a greater need to truly understand their clinical indications and how they perform in the oral environment. For years, dentists were told not to bulk fill because when curing composites in more than a 1- to 2-mm layer, the tooth would be compromised and the restoration longevity decreased.20 Different techniques emerged as an attempt to make bulk fill feasible with certain curing processes, such as wave and ramp cure. Then a 1-mm layering technique and angled layers were introduced to overcome polymerization shrinkage. The bigger the bulk of composite cured at one time, the greater the increase of stress accumulation at the adhesive interface or at the margin, the interface between the restorative material and the tooth. A mathematical equation called the C-factor that considered uncured walls versus cured walls and surface area was used to predict the stress accumulation caused by composites.21,22 Counterintuitively, this math indicated that Class I composites would perform the worst with a large bulk. The seal would be compromised and result in premature leakage, secondary caries, or fracture of the enamel rods. This would produce a white shadow around the margins, especially on an occlusal composite.
When manufacturers made the leap into bulk-fill composites, it required significant improvements in the material science to create efficiency around a process of filling 6-mm deep cavities in 1-mm increments that required 20 seconds of curing each.23-26 They endeavored to reduce this curing time to make bulk fill more efficient and cost-effective. Given that adhesive dentistry must be performed under absolute isolation, technique sensitivity was decreased with bulk fills because the tooth does not need to be kept completely isolated and dry for an extended period.27
The bulk-fill composites that have emerged from advancement in materials science are varied, with differing properties suited to different purposes. Today, the common recommendation for bulk-fill materials is a depth of cure from 4 to 6 mm as opposed to 1- to 2-mm increments.Therefore, they are not called single-increment composites. Many bulk-fill composites on the market do not have appropriate physical properties to be in occlusal contact as the surface cap layer on the occlusal table of the tooth. As a result, it is recommended to use the bulk-fill composite to within 1 or 2 mm of the occlusal preparation and then switch to a more traditional nanofiller/nanohybrid for the 1- to 2-mm cap layer. Certain bulk-fill composites do not require a cap layer due to their physical properties, but nevertheless they may not be appropriate for a single increment because depth of cure is still 4 to 6 mm.28
When a Class I or Class II restoration is performed, a periodontal probe should be used for measuring the floor of the restoration to where the occlusal table will be. This provides an assessment of the occlusal table depth. In a Class II box, it would be rare not to have to do two increments or layers. A depth of 4 to 6 mm is possible, but often a Class II box can be 8, 10, or 12 mm from the floor of the box to the marginal ridge. Most bulk-fill materials are not rated for that great a depth of cure. Additionally, one characteristic that has become popular in bulk-fill composites is a handling property called self-leveling, which means that the material does not require condensation and will automatically fill the preparation by spreading out. Self-leveling minimizes and eliminates voids or porosities in the body of the composites that would normally be seen in a follow-up appointment after taking a bitewing radiographic.29
Bulk-fill composites were primarily improved by reconfiguring composite materials, filler content, and type of fillers to control the direction of shrinkage and what it pulls against. Now, the shrinkage does not pull on the adhesive interface and therefore does not compromise the bond of the material to the tooth. Premature failure of that bond, opening of margins, leakage, and secondary caries can be avoided. Shrinkage stress refers to how much of the polymerization shrinkage stresses the adhesive interface. Modern bulk-fill composites have lower rates of shrinkage stress than traditional nanofill or newer generations of composites that were on the market before bulk fills.30 Photoinitiators have also been improved to achieve greater depths of cure and change the direction of the filler particles as well as other chemical properties. They make materials appear more translucent, which allows greater depth of cure. Overall, this author is of the opinion that bulk-fill composites today are often superior to the composites from the prior generation.
Currently, it is popular to use a bulk-fill composite that falls into the bulk-fill flowable category. These composites are more viscous than a traditional composite. Bulk-fill flowable composites in general have higher filler content than traditional flowables, but not so much that they must be condensed or placed. The lower viscosity enables the material to adapt well to the walls of the preparation of the matrix band. No condenser is needed, and there will not be any voids or porosities. Consequently, they can be used either to fill a Class II box from the floor up to the occlusal table of the preparation or to fill up the entirety, get within 1 to 2 mm of the occlusal, and then switch to a nanofiller/nanohybrid composite as a cap layer. If a bulk-fill is flowable in nature, the odds are good that it requires a cap fill or that the manufacturer requires a cap layer.31
There are also bulk-fill materials that have a viscosity similar to more-traditional composites and adequate physical properties to function as their own cap layer. These materials need to be placed using a plastic instrument and then must be put in the preparation using a condenser. Another option includes materials that have higher viscosity but that are designed to flow or run by the addition of either ultrasonic power, kinetic energy, or heat. Composite heaters can be used to temporarily make traditional composites flow more easily.32
Clinicians will want to find a composite technique that takes advantage of the science and material properties of flowable composites, including their ease, efficiency, and low technique sensitivity. The technique can then be used to fill a solid majority of the preparation before placing a highly esthetic nanofill or nanohybrid as the cap layer.
The Adhesive Process
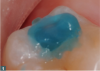
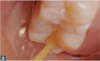
Dentin adhesive is the next consideration that should be understood fully from a standpoint of how to connect composite resin to the tooth surface. The main purpose of the adhesive process is to prepare the tooth, remove the smear layer from the preparation (Figure 1), and demineralize the enamel. The dentinal tubules will be opened and demineralize some of the dentin. Then the open dentinal tubules, enamel, and demineralized dentin will be infiltrated with a very low-fill, highly flowable unfilled resin dentin adhesive (Figure 2). Next, the hybrid zone can be created, which is the connection between the composite and the tooth structure.
Traditionally, this process was accomplished using phosphoric acid in the form of the infamous blue gel that contained somewhere between 30% and 40% phosphoric acid.33 The challenge with phosphoric acid is its technique sensitivity-the enamel needs 25 seconds or so in contact with the phosphoric acid, but the dentin can only handle 10 to 15 seconds.34 This discrepancy poses a significant challenge. If the enamel is under-etched, the margins open prematurely; if the dentin is over-etched, sensitivity increases along with lower bond strengths, compromising the longevity of the restoration.35
Another challenge applies to rinsing away the phosphoric acid and drying the tooth without drying it too much because the primer and the adhesive are hydrophilic. In the past, getting around the challenges of total etch was accomplished using rewetting agents or desensitizers. For years, the addition of a solution containing 5% glutaraldehyde and 35% hydroxyethyl methacrylate (HEMA) in water allowed clinicians to open dentinal tubules and rewet after using phosphoric acid, then rinse and dry.36
In addition to total etch and self-etch, there is also selective etching. Selective etching is still a phosphoric acid technique, but the phosphoric acid is placed on the enamel without covering the dentin for 10 to 15 seconds. Then the dentin is covered with phosphoric acid and 10 more seconds pass before rinsing and drying. A fourth technique is hybrid etching, where the phosphoric acid is placed.35 The clinician completes the process by switching to an adhesive that has self-etching capability and uses it to finish etching the enamel and the dentin. Finally, there is the true self-etching technique that bypasses use of phosphoric acid: universal adhesives. This enables the flexibility to etch in any way desired with one material and very low inventory control.
In discussions of commonly used rewetting agents, it is important to mention materials that fall into the category of desensitizers. A main component of the chemistry of these agents, HEMA, is a powerful desensitizer. It goes down into the dentinal tubules and spurs a coagulant to block the fluid movement in the tubules.37,38 This prevents sensitivity that comes from fluid moving back and forth, which accounts for the largest portion of tooth sensitivity. At the same time, these materials act as a wetting agent, allowing clinicians to rinse and dry phosphoric acid without worrying about leaving the tooth too wet or too dry. In the last 5 to 10 years, additional advantages to these materials have emerged. One of the big advantages is the component glutaraldehyde, which is an antimicrobial agent. It gets rid of bacteria that have been introduced by decay and the restorative procedure. These bacteria are responsible for both reversible and irreversible pulpitis. Thus, glutaraldehyde not only reduces postoperative sensitivity by decreasing the incidence of pulpitis but also decreases the incidence of postoperative pulpal necrosis that can lead to a root canal.39
The 5% glutaraldehyde and 35% HEMA solution has another benefit inherent to matrix metalloproteinases (MMPs).40,41 Bond degradation is a phenomenon involving the breakdown of adhesive connections, more specifically between the adhesive and the dentin. Part of that breakdown is a process initiated in the tooth that is a response from the collagen that produces MMPs. Glutaraldehyde minimizes the production of MMPs, thereby significantly slowing the rate of bond degradation. This maximizes the longevity of the restoration through a minimal amount of material. A 5% glutaraldehyde and 35% HEMA solution can do everything from sealing the dentinal tubules with HEMA and adding the antimicrobial effect of the glutaraldehyde to minimizing the production of MMPs, managing bone degradation, and acting as a rewetting agent for those who still use phosphoric acid.39
Universal Etch
Universal etching, a new category of adhesives, ensures a similar level of flexibility for clinicians who prefer to use different etching techniques in their practice. In the past, that would mean needing more than one material in the office. Universal dentin adhesives eliminate this problem, but it is still important to be familiar with individual brands because not all universal adhesives have the same clinical applications and broad applicability to different restorative procedures. However, they all will allow clinicians to choose their etching technique. Universal etching can be used along with a total-etch technique, so phosphoric acid can be placed on both the enamel and dentin. Alternately, it can be used with a self-etch, hybrid, or selective etching while maintaining high-quality bond strengths and results. Many universal-etching materials are compatible with dual-cure materials.
Another aspect of the universal category is that the same concept applies to the materials against which the adhesive can be used.42-47 Some of these materials contain monomer technology in the form of the material 10-methacryloyloxydecyl dihydrogen phosphate (MDP).48 This monomer has special properties, such as a pH that enables total etch or self-etch. It can also be used against a wide variety of structures, including enamel, dentin, ceramic, metal, and composite. It also acts as a conditioner or primer against restorative materials. If the clinician is trying to do a porcelain repair or bond composite to composite, the same material can be used. Having fewer types of materials can ease stress in a practice from time spent researching and purchasing multiple materials in a singular category and accounting for variable expiration dates, which is not a very cost-effective process.
Another advantage of universal etch is low technique sensitivity because the clinician does not need to refresh knowledge of the material properties and directions due to inconsistent use. The ability to use the same material over and over again ensures a higher likelihood that the clinician is well-versed in its proper use.
Finally, the evolution of materials has extended to the finishing and polishing of all restorations. Diamond polishing paste can be used to finish composites and only necessitates a prophy cup with a handpiece-placed brush. This material aids clinicians in achieving a very smooth, glassy surface texture for patients that feels more like natural tooth structure. There may also be less wear because the patient is not rubbing and trying to smooth the restorations.
Conclusion
The evolution of dental restorative materials has spanned composites, flowables, bulk fill, adhesives, etch, and polish. With these improvements, dentists must adjust to change by thoroughly researching their products of choice and embracing how new properties create more-efficient case procedures. Important considerations include the category of composites, whether they are nanofill or nanohybrid, what kind of bulk-fill regimen is preferred by the clinician, and the advantages of different adhesives. The benefits obtained from deploying these materials include minimizing sensitivity, minimizing challenges in bonding, achieving lower postoperative sensitivity, and achieving greater longevity for restorations. The physical properties of dental materials have a direct influence on enhanced patient care, which is why it is essential to remain updated on advancements related to their appropriate use.
REFERENCES
1. Shinkai K, Taira Y, Suzuki S, et al. Effect of filler size and filler loading on wear of experimental flowable resin composites. J Appl Oral Sci. 2018;26:e20160652.
2. Atai M, Yassini E, Amini M, Watts DC. The effect of a leucite-containing ceramic filler on the abrasive wear of dental composites. Dent Mater. 2007;23(9):1181-1187.
3.Prakki A, Pereira PN, Kalachandra S. Effect of propionaldehyde or 2,3-butanedione additives on the mechanical properties of bis-GMA analog-based composites. Dent Mater. 2009;25(1):26-32.
4. Zimmerli B, Strub M, Jeger F, et al. Composite materials: composition, properties and clinical applications. A literature review. Schweiz Monatsschr Zahnmed. 2010;120(11):972-986.
5. Ilie N, Hickel R. Resin composite restorative materials. Aust Dent J. 2011;56(suppl 1):59-66.
6. Ilie N, Hickel R. Investigations on mechanical behaviour of dental composites. Clin Oral Investig. 2009;13(4):427-438.
7. Park JW, Shim GS, Lee JG, et al. Evaluation of UV curing properties of mixture systems with differently sized monomers. Materials (Basel). 2018;11(4):E509.
8. Santini A, Gallegos IT, Felix CM. Photoinitiators in dentistry: a review. Prim Dent J. 2013;2(4):30-33.
9. Meereis CTW, Münchow EA, de Oliveira da Rosa WL, et al. Polymerization shrinkage stress of resin-based dental materials: a systematic review and meta-analyses of composition strategies. J Mech Behav Biomed Mater. 2018;82:268-281.
10. Ernst CP, Brand N, Frommator U, et al. Reduction of polymerization shrinkage stress and marginal microleakage using soft-start polymerization. J Esthet Restor Dent. 2003;15(2):93-103.
11. Morimoto S, Rebello de Sampaio FB, Braga MM, et al. Survival rate of resin and ceramic inlays, onlays, and overlays: a systematic review and meta-analysis. J Dent Res. 2016;95(9):985-994.
12. Kim KH, Ong JL, Okuna O. The effect of filler loading and morphology on the mechanical properties of contemporary composites. J Prosthet Dent. 2002;87(6):642-649.
13. Belli R, Wendler M, Zorzin JI, Lohbauer U. Practical and theoretical considerations on the fracture toughness testing of dental restorative materials. Dent Mater. 2018;34(1):97-119.
14. Soderholm KJ. Review of the fracture toughness approach. Dent Mater. 2010;26(2):e63-e77.
15. Becher R, Wellendorf H, Sakhi AK, et al. Presence and leaching of bisphenol a (BPA) from dental materials. Acta Biomater Odontol Scand. 2018;4(1):56-62.
16. Moda MD, Godas AGL, Fernandes JC, et al. Comparison of different polishing methods on the surface roughness of microhybrid, microfill, and nanofill composite resins. J Investig Clin Dent. 2018;9(1). doi: 10.1111/jicd.12287.
17. Da Costa J, Ferracane J, Paravina RD, et al. The effect of different polishing systems on surface roughness and gloss of various resin composites. J Esthet Restor Dent. 2007;19(4):214-224.
18. Mahmoud SH, El-Embaby AE, AbdAllah AM, Hamama HH. Two-year clinical evaluation of Ormocer, nanohybrid and nanofill composite restorative systems in posterior teeth. J Adhes Dent.2008;10(4):315-322.
19. Saunders SA. Current practicality of nanotechnology in dentistry. Part 1: Focus on nanocomposite restoratives and biomimetics. Clin Cosmet Investig Dent. 2009;1:47-61.
20. Ferracane JL, Hilton TJ. Polymerization stress--is it clinically meaningful? Dent Mater. 2016;32(1):1-10.
21. Fok ASL, Aregawi WA. The two sides of the C-factor. Dent Mater.2018;34(4):649-656.
22. Pabis LV, Xavier TA, Rosa EF, et al. A method to investigate the shrinkage stress developed by resin-composites bonded to a single flat surface. Dent Mater. 2012;28(4):e27-e34.
23. Miletic V, Pongprueksa P, De Munck J, et al. Curing characteristics of flowable and sculptable bulk-fill composites. Clin Oral Investig. 2017;21(4):1201-1212.
24. Leprince JG, Palin WM, Vanacker J, et al. Physico-mechanical characteristics of commercially available bulk-fill composites. J Dent. 2014;42(8):993-1000.
25. Ilie N, Stark K. Curing behaviour of high-viscosity bulk-fill composites. J Dent. 2014;42(8):977-985.
26. Reis AF, Vestphal M, Amaral RCD, et al. Efficiency of polymerization of bulk-fill composite resins: a systematic review. Braz Oral Res. 2017;31(suppl 1):e59.
27. Nair P, Hickel R, Ilie N. Adverse effects of salivary contamination for adhesives in restorative dentistry. A literature review. Am J Dent. 2017;30(3):156-164.
28. Jung JH, Park SH. Comparison of polymerization shrinkage, physical properties, and marginal adaptation of flowable and restorative bulk fill resin-based composites. Oper Dent.2017;42(4):375-386.
29. Soares CJ, Rosatto C, Carvalho VF, et al. Radiopacity and porosity of bulk-fill and conventional composite posterior restorations-digital x-ray analysis. Oper Dent. 2017;42(6):
616-625.
30. Rullman I, Patyna M, Janssen B, Willershausen B. Determination of polymerization shrinkage of different composites using a photoelastic method. Am J Dent. 2017;30(1):16-22.
31. Van Ende A, De Munck J, Lise DP, Van Meerbeek B. Bulk-fill composites: a review of the current literature. J Adhes Dent.2017;19(2):95-109.
32. Nada K, El-Mowafy O. Effect of precuring warming on mechanical properties of restorative composites. Int J Dent. 2011;2011:536212. doi: 10.1155/2011/536212.
33. Mithiborwala SH, Chaugule V, Katge F, et al. A comparative evaluation of the efficacy of etching by the total etch and self-etch dentin bonding systems in the primary teeth: an in vitro study. Int J Clin Pediatr Dent. 2015;8(1):30-36.
34. Cardenas AFM, Siqueira FSF, Bandeca MC, et al. Impact of pH and application time of meta-phosphoric acid on resin-enamel and resin-dentin bonding. J Mech Behav Biomed Mater.2018;78:352-361.
35. Takamizawa T, Barkmeier WW, Tsujimoto A, et al. Influence of different etching modes on bond strength and fatigue strength to dentin using universal adhesive systems. Dent Mater.2016;32(2):e9-e21.
36. Sabatini C, Wu Z. Effect of desensitizing agents on the bond strength of mild and strong self-etching adhesives. Oper Dent.2015;40(5):548-557.
37. Ishihata H, Finger WJ, Kanehira M, et al. In vitro dentin permeability after application of Gluma® desensitizer as aqueous solution or aqueous fumed silica dispersion. J Appl Oral Sci.2011;19(2):147-153.
38. Kolker JL, Vargas MA, Armstrong SR, Dawson DV. Effect of desensitizing agents on dentin permeability and dentin tubule occlusion. J Adhes Dent. 2002;4(3):211-221.
39. Ishihata H, Kanehira M, Finger WJ, et al. Effect of two desensitizing agents on dentin permeability in vitro. J Appl Oral Sci.2017;25(1):34-41.
40. Ou Q, Hu Y, Yao S, et al. Effect of matrix metalloproteinase 8 inhibitor on resin-dentin bonds. Dent Mater. 2018;34(5):756-763.
41. Hass V, Luque-Martinez IV, Gutierrez MF, et al. Collagen cross-linkers on dentin bonding: Stability of the adhesive interfaces, degree of conversion of the adhesive, cytotoxicity and in situ MMP inhibition. Dent Mater. 2016;32(6):732-741.
42. Rosa WL, Piva E, Silva AF. Bond strength of universal adhesives: a systematic review and meta-analysis. J Dent.2015;43(7):
765-776.
43. Muñoz MA, Luque I, Hass V, et al. Immediate bonding properties of universal adhesives to dentine. J Dent. 2013;41(5):404-411.
44. Chen C, Niu LN, Xie H, et al. Bonding of universal adhesives to dentine--old wine in new bottles? J Dent.2015;43(5):525-536.
45. Hanabusa M, Mine A, Kuboki T, et al. Bonding effectiveness of a new "multi-mode" adhesive to enamel and dentine. J Dent.2012;40(6):475-484.
46. Muñoz MA, Luque-Martinez I, Malaquias P, et al. In vitro longevity of bonding properties of universal adhesives to dentin. Oper Dent. 2015;40(3):282-292.
47. Rosa WL, Piva E, Silva AF. Bond strength of universal adhesives: a systematic review and meta-analysis. J Dent.2015;43(7):
765-776.
48. Tsuchiya K, Takamizawa T, Barkmeier WW, et al. Effect of a functional monomer (MDP) on the enamel bond durability of single-step self-etch adhesives. Eur J Oral Sci. 2016;124(1):
96-102.