You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Oral pathology encompasses diseases of the mouth, jaw, and related structures, such as the temporomandibular joint (TMJ), salivary glands, periorbital skin, and facial muscles. There are hundreds of oral pathologies. When patients have a suspicious growth or condition of the mouth, it is essential to determine the cause, accurately diagnose, and speedily give any necessary care.
Every year, there are about 500,000 new cases of oral cancer worldwide, accounting for approximately 3% of all malignancies.1 Oral cancer has a tendency to be detected at a late stage, which is detrimental to patients.2 Although the oral cavity is a potentially accessible site for examination, up to 50% of oral cancers are not detected until the disease is well advanced.3 The most common form of oral cancer is squamous cell carcinoma, which accounts for 96% of all cancers of the oral cavity.4 Despite significant advances in cancer treatment, early detection of oral cancer and its curable precursors remains the best way to ensure patient survival and improved quality of life.5,6 Clinicians can improve patients' survival rates if a cancerous lesion is detected at an early stage or if a precursor lesion (dysplasia) is discovered and treated before malignant progression.7 As the emphasis shifts from damage mitigation to disease prevention or reversal of early disease in the oral cavity, the need for sensitive and accurate detection and diagnostic tools becomes more important.8
The goal of this article is to build confidence and competence in the identification, screening, and differential diagnoses of common oral pathologies as well as the detection of oral abnormalities. Building this knowledge will take collaboration between dental providers, physicians, and specialists, including oral and maxillofacial surgeons, radiologists, and pathologists.
Identifying and Differentiating Between Common Abnormalities
The development of a reasonable differential diagnosis is of prime importance in determining whether biopsy is indicated. The differential diagnosis aids the clinician in selecting the appropriate technique if a biopsy is necessary.9 There are three steps to achieving the first learning objective of this article, identifying and differentiating between common abnormalities of the mouth and surrounding area. One is to take a comprehensive medical history. Another is to understand the anatomy of the oral cavity and surrounding structures. The third is to be familiar with the terminology associated with what is being visualized or palpated.
Medical History
Medical history should be collected at every appointment. Patients should be asked about their social history, including dietary habits, oral hygiene habits, smoking, and alcohol and drug use. A comprehensive understanding of each patient's medical history enables dentists to understand the psychosocial components and general habits of a patient, thus enabling an accurate assessment of risk factors and pathologies.
Physical Assessment
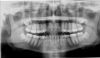
A physical assessment of the oral cavity and surrounding landmarks has three components: the extraoral assessment, the intraoral assessment, and radiographs. The extraoral assessment involves palpation of the submandibular and sublingual glands, cervical lymph nodes, pre- and post-auricular lymph nodes, TMJ, any asymmetries, lips, skin and facial structures, thyroid gland, and muscles of mastication. An intraoral assessment includes visualizing all landmarks in the oral cavity and gingival and buccal mucosa, along with the dentition. Radiographic assessments may involve a panoramic image (Figure 1) or cone-beam computed tomography (CBCT) as required, which must be read by someone trained to do so.
A thorough understanding of anatomy includes an awareness of nerves and vasculature. This knowledge will enable a more comprehensive assessment of complex pathologies. Furthermore, when taking a biopsy of an area of the mouth, an understanding of the vital structures in those areas is crucial in order to prevent damage to the vasculature and nerves.
Terminology
When describing a lesion, terminology is key. Critical components in the description of a lesion include, but are not limited to, location, size, shape, color, consistency, mobility, and radiographic properties. A history of the lesion, including whether it causes pain and any other curiosities, is also important. Some of the most common terminology in diagnosis is listed in Table 1. It is also important to take medication histories, not only to prevent prescription errors and consequent risks to patients but also to detect drug-related clinical or pathologic changes.10
Screening Methods
After the medical history and physical assessment, anatomy, landmarks, and descriptive terminology are understood, the next objective is to define screening methods and tools to help detect oral pathologies. Screening methods fall into four categories: visual, tools, laboratory studies, and biopsy.
Visual Examination
Visual examination involves what was covered in the previous section of this article: radiographic interpretation, along with extraoral and intraoral assessments. Some oral pathologies are easily diagnosed based on history and appearance; however, others are not. In addition, although diagnosis may appear to be self-evident by visual inspection alone, coexisting diseases could be present that may go undetected and untreated.11 Nevertheless, a thorough history-taking ensures a good doctor-patient relationship and can prevent the need for expensive laboratory procedures in some cases.12
Tools
A variety of screening tools can be implemented to detect oral pathologies. Some use fluorescent visualization to detect oral disease. Others use three wavelengths of light to reveal mucosal abnormalities. Still others use light-emitting diode (LED) beam technology and a high-contract fluorescence viewer to enable both intraoral and extraoral access. Depending on the type of light and the imaging approaches used, optical imaging of the oral tissues can detect slight changes within the tissues, such as alterations in tissue architecture and composition; expression of specific biomarkers, vascularity/angiogenesis, and perfusion; and microanatomy and tissue boundary integrity.13,14 These tools can be used to identify oral cancer, but when abnormalities are found, it is important to remember that not all abnormal tissue will be cancer. Each tool has its individual benefits; choosing a tool ultimately comes down to personal preference.
Laboratory Studies
The next set of diagnostics involves collection of cultures or tissues for laboratory studies. Cultures can be taken to assess bacterial, fungal, and viral infections that may be contributory to the pathologies. Bacterial and fungal culturing is not routinely performed for oral lesions. The cultures can be obtained by swabbing a patient's draining abscess to determine which type of bacteria or fungus is present in order to best treat with antibiotics or antifungal therapy. Viral cultures can be obtained similarly. Other tests include direct fluorescence, an antibody test, and polymerase chain reaction.
Biopsy
To diagnose oral lesions, a tissue biopsy is considered the gold standard.15 An oral biopsy is essential for a definitive diagnosis of the diseases that occur in the oral mucosa.16 Initially, the accuracy of the history-taking and clinical examination can have an influence on the accuracy of a biopsy. Thereafter, the biopsy's accuracy is dependent on the administration of local anesthesia, the method adopted to remove the tissue, adequate size and depth of the tissue from the representative site, and the subsequent fixation method.17
The four biopsy techniques that can be used orally include a punch biopsy, a brush or exfoliative cytology, an incisional or excisional biopsy, or an aspiration. An incisional biopsy is typically obtained to get a small representative sample, while an excisional biopsy is usually used to surgically remove and evaluate an entire lesion. The area can be numbed with topical or local anesthetic, or a block may be used instead in an effort to reduce the risk of distorting the lesion.
Biopsy punches come in a variety of sizes and in both reusable and disposable forms (Figure 2). Disposable biopsy punches are lighter and more easily manipulated than their metal counterparts. Most incisional intraoral biopsies can be performed with a 3- or 4-mm punch, whereas larger punches can be used for small excisional biopsies.
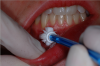
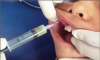
An excisional biopsy removes the entire lesion and a border around the lesion. An incisional biopsy removes part of the lesion for diagnostic purposes. In a brush biopsy (Figure 3), a small brush is used on the lesion to collect material for the biopsy that may provide helpful information on infectious and noninfectious oral diseases. Fine-needle aspiration biopsy technique (Figure 4) is used on salivary gland masses and enlarged lymph nodes. Fine-needle aspiration involves a thin hollow needle being inserted into a mass to extract cells or fluids. The patient rinses the mouth with chlorhexidine for about 60 seconds, and the area is then numbed with local anesthetic. A 22-gauge needle is normally used to collect a sample, which is then fixated to a slide for examination by an oral pathologist.
To safely store and transport samples, tissue removed from the mouth must typically be placed in a fixative solution. For routine biopsies, 10% neutral buffered formalin is the fixative of choice. The pathology laboratory should be consulted for any anticipated special procedures to ensure that the tissue is handled properly. Sending a biopsy out for analysis should adhere to a standard protocol that includes follow-up with the patient and documentation.
Results can be referred to a specialist: an oral and maxillofacial surgeon, oral pathologist, or periodontist. Referral of these lesions to a specialist will result in an early definitive diagnosis and treatment if needed. Lesions may require special attention and particular management strategies depending on the site, grade of dysplasia, and patient risk.5
Conclusion
Oral pathology is a complex topic that involves continuous education. Determining how to make a differential diagnosis falls into the overall knowledge of oral pathology and describing what is seen. To make a differential diagnosis with confidence, one needs to gather the correct information, including medical history, anatomy, terminology, samples, and images.
References
1. Johnson NW, Warnakulasuriya S, Gupta PC, et al. Global oral health inequalities in incidence and outcomes for oral cancer: causes and solutions. Adv Dent Res. 2011;23(2):237-246.
2. Messadi DV. Diagnostic aids for detection of oral precancerous conditions. Int J Oral Sci. 2013;5(2):59-65.
3.McGurk M, Chan C, Jones J, et al. Delay in diagnosis and its effect on outcome in head and neck cancer. Br J Oral Maxillofac Surg. 2005;43(4):281-284.
4. Siegel R, Naishadham D, Jemal A. Cancer statistics, 2012. CA Cancer J Clin. 2012;62(1):10-29.
5. van der Waal I. Potentially malignant disorders of the oral and oropharyngeal mucosa; terminology, classification and present concepts of management. Oral Oncol. 2009;45(4-5):317-323.
6. Llewellyn CD, Johnson NW, Warnakulasuriya KA. Risk factors for squamous cell carcinoma of the oral cavity in young people-a comprehensive literature review. Oral Oncol. 2001;37(5):401-418.
7.Messadi DV, Wilder-Smith P, Wolinsky L. Improving oral cancer survival: the role of dental providers. J Calif Dent Assoc. 2009;37(11):789-798.
8. Wilder-Smith P, Holtzman J, Epstein J, Le A. Optical diagnostics in the oral cavity: an overview. Oral Dis. 2010;16(8):717-728.
9.Ephros H. Oral tissue biopsy. Medscape. https://emedicine.medscape.com/article/1079770-overview. Updated March 10, 2016. Accessed February 7, 2018.
10.Fitzgerald RJ. Medication errors: the importance of an accurate drug history. Br J Clin Pharmacol. 2009;67(6):671-675.
11.Newsome P, Smales R, Yip K. Oral diagnosis and treatment planning: part 1. Introduction. Br Dent J. 2012;213(1):15-19.
12. Subramanyam RV. Oral pathology in clinical dentistry: a systematic approach. J Int Clin Dent Res Organ. 2014;6(2):72-76.
13.Fedele S. Diagnostic aids in the screening of oral cancer. Head Neck Oncol. 2009;1:5. doi: 10.1186/1758-3284-1-5.
14. Epstein JB, Silverman S Jr, Epstein JD, et al. Analysis of oral lesion biopsies identified and evaluated by visual examination, chemiluminescence and toluidine blue. Oral Oncol. 2008;44(6):538-544.
15.Melrose RJ, Handlers JP, Kerpel S, et al. The use of biopsy in the dental practice. The position of the American Academy of Oral and Maxillofacial Pathology. Gen Dent. 2007;55(5):457-461.
16. Mota-Ramírez A, Silvestre FJ, Simó JM. Oral biopsy in the dental practice. Med Oral Patol Oral Cir Bucal.2007;12(7):E504-E510.
17. Masthan KMK, Sankari SL, Babu NA, Rajguru JP. How to help the oral pathologist in making an accurate diagnosis. J Clin Diagn Res. 2013;7(1):181-184.