You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The fundamental concepts of applying occlusion to practice involve the ability to identify common occlusion problems, accurately and thoroughly examine the occlusion as well as the temporomandibular joint (TMJ), and treat patients who are having pain. Patients experiencing muscle pain can be treated with a full or partial coverage flat-plane appliance. Knowing when and when not to use specific appliances is valuable. This article explores the methodology for approaching the separate aspects of occlusion and incorporating them in the practice.
Introductory Occlusion Concepts
When applying occlusion to restorative dentistry, one of the concepts is the degree of difference between centric occlusion and maximum intercuspal position (MIP). In some instances a significant shift could indicate the presence of a keystone tooth. The author defines a keystone tooth as a tooth that gives the body an awareness of where the bite should be, which happens when the patient touches on that tooth in centric occlusion. If work is performed on that tooth, the occlusion can be fundamentally changed accidentally, making recovery difficult. In dentistry, it is prudent to avoid working on a tooth that can change the way the other teeth fit together until the consequences of a change can be anticipated; the result could be joint position change or recapture of a disc. More information must be gathered.
Defining Centric Relation
Centric relation is where the joint is in the most superior and anterior position within the fossa.1It should not be confused with related terminology such as centric occlusion, maximum intercuspation, adaptive centric posture, long centric, centric slides, or centric stops. The Glossary of Prosthodontic Terms defines centric relation as the maxillomandibular relationship in which the condyles articulate with the thinnest avascular portion of their respective discs with the complex in the anterosuperior position against the shapes of the articular eminence.1,2 This position is independent of tooth contact. Essentially, the joint is in the anterosuperior place, independent of tooth contact.
Educator Frank Spear, DDS, defines centric relation as the position of the condyle when the lateral pterygoid is relaxed and elevator muscles contract with the disc properly aligned.3 The muscles pull everything up to the center, which is fine if the muscles are not irritated and protecting the joint somehow, or if there is damage to the disc. Centric relation is a position that self-centers. As an example, if a marble ball is dropped anywhere inside a bowl, eventually it will rest in the center of the bowl. If the pterygoid muscle is inflamed, hot, and protecting the position of that condyle from seating, it would be like having a magnet and a metal marble in the bowl; the magnet will pull the marble to one side or position. That is what can happen with an inflamed lateral pterygoid.
Finding Centric Relation
Centric relation can be determined by several different means.4,5 The simplest but least accurate method is to have the patient put the tongue to the back of the roof of the mouth and bite down, which is helpful for a quick analysis but in the author's opinion not especially accurate. Another method is bilateral manipulation (bilateral guidance), which is technique sensitive. It involves creating a "C" shape with the fingers and thumb and placing the fingers on the mandible and chin; then the patient is asked to gently open and close in order to get the patient used to the motion. After a few cycles of opening and closing in rotation, the dentist asks the patient to relax and takes over using caution not to overpower the patient and activate the patient's musculature to resist the motion. Care must also be taken that the condyle is not pushed backward; it should be guided into the anterior and superior medial position.
A third method is to use an anterior deprogrammer. A tool such as a Lucia jig or quicksplint is placed in the mouth with bite registration material. It is affixed to the central incisors. The patient moves forward and backward on the Lucia jig, relaxing the muscles. After the muscles are relaxed, the patient is directed to bite back on the flat plane. When the patient is back at that point and squeezes, the condyle should seat into the fossa.5 Another simple technique is the leaf gauge, which is similar to an anterior deprogrammer.4 A leaf gauge can be opened to different verticals by removing or inserting leaves. Whether a leaf gauge can distalize the condyle is questionable, but it will get the dentist in the right area. If the joint is healthy, the disc is not displaced and the muscles are not holding it out of place. Consequently, the muscles can self-center the joint. A well-adjusted bite splint that has relaxed the muscles will also assist in finding centric relation.
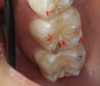
After centric relation is found, the point of first contact must be determined. The point of first contact may be a keystone tooth, but not everyone has a keystone tooth. The point of first contact needs to be marked, but not necessarily physically. In Figure 1, showing teeth Nos. 2 and 3, the point of first contact is on the mesiolingual cusp of No. 2, which has the strongest blue mark. There is also a slight mark on the distal buccal cusp of tooth No. 3. When the jaw is in centric relation, the point or coincident points of first contact are called centric occlusion. Centric relation is a joint position and is found independent of tooth contact; the joint is centered and teeth do not need to touch if centric relation is in the joint space. When the opposing teeth come together in the joint space, the term is centric occlusion.1
Locating Centric Occlusion
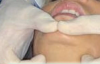
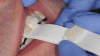
MIP is the term for the habitual bite, when the patient squeezes together and the maximum number of teeth touch. Centric occlusion can be determined with bilateral manipulation, bilateral guidance (Figure 2), or a leaf gauge (Figure 3).6 The position may or may not coincide with MIP.7,8 If the dentist is planning to restore the tooth that has the point of first contact, the existence or absence of a slide must be determined. The author's preferred technique to identify the slide is by having the patient squeeze the teeth together in MIP to determine whether the jaw shifts in any substantial way when going into that position.
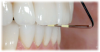
Before the slide is determined, the dentist must measure the overbite and the overjet, which can be done with a periodontal probe. If the change in overjet (horizontal) is greater than the change in overbite (vertical), the dentist must use more caution (Figure 4). It is common for patients who have a slide in centric occlusion to have more change in the vertical than the horizontal position.9 Most patients will slide either to the right, left, vertical, back, or front.9 A slide greater than about 1.5 to 2 mm and that changes more horizontally than vertically indicates the presence of the potential problem that can be referred to as the keystone tooth. The term keystone tooth is used because just as the presence of a keystone in an arc is key to the stability of the arc, so too can the presence of a keystone tooth be a patient's existing occlusal function. If a keystone tooth is present, restoratively altering this tooth can lead to unanticipated consequences.
The only way to understand these consequences is to mount the case in centric relation to see what happens to the rest of the bite after the occlusion on the keystone tooth is eliminated.10 Due to the unique qualities of physiology, as soon as memories are erased of (1) what was partially holding the occlusion together, (2) the way the patient would eventually bite together, and (3) what kept the disc in place, the feedback loop of the teeth to the muscles and the muscles to the teeth is interrupted. If the feedback loop is interrupted, the patient may never be able to return to the habitual bite. It is essential to determine whether this problem will occur before the tooth is cut down and a crown is placed on it.11Tooth structure should not be removed before a thorough evaluation of that tooth's role in the occlusion. If the teeth continue to fit well together after mounting the case and evaluating to occlusion in centric, there is little to be concerned with. If, however, new points of first contact are discovered that do not articulate well or if there is a significant lack of occlusal space between the keystone tooth and the opposing tooth, it is prudent to explain the potential consequences to the patient. It is impossible to know with certainty that the restorative dentistry will create a problem that the patient cannot tolerate; however, if a conversation about this potential is had prior to restoring the tooth, the patient will be better prepared if this unfortunate circumstance comes to pass.
Performing a Thorough Pretreatment Evaluation
Before a clinician treats a patient, a complete evaluation must be performed. The clinician must devote time to understanding the patient's occlusion, bite, muscles, and TMJ. Ideally, any red flags that could lead to future concerns should be eliminated. The goal is not to become a pain doctor but to understand the difference between patients who are safe for restorative work and those who necessitate more caution. A comprehensive examination begins with a history, including talking to the patient and uncovering any past trauma or pain. The patient's overall medical history should be ascertained, along with eliminating or confirming the existence of obstructive sleep apnea, snoring, gastroesophageal reflux disease, antianxiety/antidepressant medications, and headaches. Patients with sleep apnea may not be aware of it, so an Epworth Sleepiness Scale or similar classification algorithm should be used to determine probability of risk.12
Moderating Degree of Invasiveness
During an Evaluation
After the history is gathered, the examination becomes more mindset-based. The dentist should ask patients about their level of awareness and general attitude toward their occlusion; for example, patients may have flattened teeth but claim they don't clench or grind. The examination should be considered as proceeding from outside the mouth to inside the mouth, transitioning slowly from the less personal to the more personal; touching a patient's temporal region is not the same level of invasiveness as an oral cancer screening.
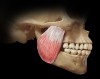
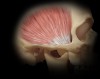
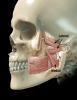
Eight muscles should be in every dentist's frame of reference. The four most significant of these muscles can be evaluated with relative ease: the masseter (Figure 5), temporalis (Figure 6), medial pterygoid, and lateral pterygoid (Figure 7). The digastric muscle, sternocleidomastoid, trapezius, and splenius capitis can be problematic to occlusion and TMJ issues, but they do not need to be examined at the outset unless TMJ dysfunction is discovered.
To examine the four primary muscles, first, the masseter should be palpated with 3 to 5 pounds of pressure. Pressing on a scale in the produce section of a grocery store will give dentists a feel for 3 to 5 pounds of resistance. Then dentists can practice on themselves, applying pressure to different spots. Checking multiple areas on the patient's masseter provides a better idea of whether pressing on the muscles causes pain. The temporalis requires a similar technique.10
Both pterygoid muscles are usually palpated inside the mouth, but the process can be difficult with the lateral pterygoid. An easier method is provocation, in which dentists put their hand in front of the patient's chin and direct the patient to push the chin forward against resistance. The dentist starts protrusively and then tells the patient, "I would like you to move my hand to the right." Patients moving their jaw aids the process considerably.13
Joint Sounds and Range of Motion
It is crucial to also gather information about joint sounds, obtaining a range of motion and joint palpation. To accomplish this, the dentist places his or her finger on the lateral aspect of the joint, directing the patient to open and close until the dentist can feel his or her finger moving somewhat right, in front of the ear. The dentist then applies 3 to 5 pounds of pressure and asks the patient whether it hurts. This move can also be performed behind the joint if the patient has an intact ear with nothing in it. The dentist can put his or her pinky finger behind the joint, having the patient open and close. After joint movement is felt, the dentist can press down and forward against the back of the joint, asking whether it hurts.14 If a patient indicates pain, it is useful to ask the patient to rate the pain on a numeric scale. It is at the discretion of the dentist to determine which scale to use; it is only important to be consistent and to properly explain the scale to the patient.
Range of motion can be measured with a ruler, triangle, or any tool designed specifically for range of motion. Range of motion should be determined in the open and closed position, adding or subtracting the overbite (depending on whether there is an anterior open bite or some overbite). The dentist should also examine the range of motion laterally left and right, which can be more difficult because patients do not always understand side direction cues. Clarity is essential.10
Load Testing and the Jaw Joint
After these steps are completed, the occlusion, centric relation, and centric occlusion should be checked. Load testing determines load on the joint. It is done by placing an object within the mouth, such as a leaf gauge, and having the patient move the jaw forward and backward, followed by biting. If it hurts the patient to move forward, that is not a load issue but a problem associated with the muscles or retrodiscal tissues. After the patient moves back and squeezes on the joint, pain, or the absence of it, gives the dentist a clue about how much of that disc is displaced. The dentist can infer whether there is just lateral pull displacement or also a medial pull displacement, which is more difficult to treat.10
The clinician next transitions from load testing to looking inside the mouth. Attrition, fremitus, and fractures are evaluated intraorally. A comprehensive occlusal examination seeks out the point of first contact as well as interferences. Understanding the patient's excursive and posterior interferences can be useful in determining attrition, fremitus, and fractures. These interferences are revealed with two different colors of articulating ribbon or paper.15,16 The dentist uses the light color first, instructing the patient to move "left, right, forward, back," to "chew it" or "break the paper," and to move "everywhere, further than you think you can." Most patients will clench while they are following these instructions, which limits the normal range of motion they would have in a chewing or bruxing stroke. There is no magic bullet to help a dentist to resolve this other than patience. After having the patient move in all previously stated directions in one color, the patient should tap together two or three times in MIP in the darker color. The lighter color lines and smudges will show where excursive movements and interferences are, and the darker dots will indicate the MIP contacts. This is important for the ultimate comfort of the patient's restoration, but it does not have much to do with TMJ issues. Although the common assumption is that teeth do not have any bearing on what happens with the jaw joint, it is still important to know details related to interferences regarding restorative dentistry and longevity of the periodontium. Another way to do this is with T-scan technology.15,16
Methods for Examining and Treating the Disc
The gold standard for examining the disc is magnetic resonance imaging (MRI), the only imaging that shows the disc in different positions.17 The dentist can obtain some info-rmation about the disc from tomography, but the possibilities are limited.17 Because MRIs are not an everyday option, the dentist can carry out a simple "open, look, listen, and feel" test. The clinician has the patient open and close, using careful attention to listen and feel with the fingers. The clinician can look to see whether there are deviations or deflections. Deviation is when the disc moves to the side but then centers again, going left or right and ending up back in the middle. Deflection is when the disc moves to one side or the other and stays at that angle. Listening to the jaw joint with a stethoscope is helpful for learning when the disc is either popping on or off the joints and whether the popping is early or late.14 These observations, together with the information collected earlier regarding symptoms, pain, and load testing, enable the dentist to form a working diagnosis.
If the dentist cannot hear with a stethoscope or wants to involve the patient in the process, a Doppler can be used.18 The Doppler allows the dentist to transmit audio noise externally so the patient can hear it also. A downside to this method is the messiness incurred from placing lubricating gel on the tip of the Doppler. Joint vibration analysis (JVA) is another option.19 JVA is a sophisticated measuring device containing a small microphone attached to headphones that go over the jaw joint. It uses frequency and catalogued joint noises for diagnosis, which makes it very useful, but JVA is also expensive. The significant amount of investment required is offset by the necessity of getting accurate joint diagnoses. Correct determination of chronically or acutely displaced discs can prevent harmful effects to later dentistry performed on the patient.11
Naming the Joint Condition
What the dentist has discovered about the jaw joint can be diagnosed and classified using a system created by Mark Piper, MD, DMD. Dr. Piper's system involves five main classifications. Stage I is normal. Stage II is a loose ligament (ligament laxity). The ligament is like a rubber band: it can stretch and become "sloppy" in the joints, sometimes making a noise. In stage III, typically, the lateral pole of the disc will be displaced. The cause could be a recent event that left the patient in acute pain, but that is not always the case. Pain is not necessarily an indication of whether the issue is recent. In stage IV, the disc is medially displaced (acute or chronic). Stage V refers to changes in the anatomy of the disc in retrodiscal tissues (early/acute or chronic perforation). This classification system requires knowledge of the position of the joint.20
Appliances to Treat Muscle-Bracing Pain
The success of treating patients with muscle-bracing pain can depend on the choice of appliance.21 Because the choice of appliance depends on the goal of treatment, it is essential to understand why a certain type of appliance should be chosen. Similarly, the goal of treatment depends on the diagnosis. If the patient presents with slight wear or has new porcelain dentistry and the diagnosis is that the joint is healthy, the purpose of the splint is to protect the teeth from excessive force. Thus, the patient needs a nightguard.22 Nightwear appliances can be used to treat muscle-bracing pain, but they are called splints or orthotics, not nightguards. A splint designed to change the position of the jaw in any dimension and to direct the forces with intention based on the evaluation of the dentist can be appropriate treatment for muscle-bracing pain. A wide variety of splints have been designed and are available to treat this condition.
Full-Coverage Splints
For a problem caused by disc displacement, a patient in pain needs a different type of splint than someone who just grinds their teeth. The standard splint for people who grind and dentists who want to protect teeth is a full-coverage hard splint or some version of a "suck down." This splint protects teeth and may reduce pain in the muscles and joint.23-27 It also can be used to evaluate the severity of grinding and clenching. The upside of a full-coverage suck down is that it can be made quickly and easily in the dental office, requiring no follow-up. The downside is that its use is limited. It treats extra-nocturnal activity but can create an iatrogenic issue.23-27Consequently, some versions of suck down should be avoided in most instances where disc displacement is a possibility.
A full-coverage hard splint performs the same functions as a softer splint/suck down (ie, protecting teeth) but also has joint stability built into the design. It can stabilize a joint, relax muscles, and assist the dentist in locating centric relation.23-27 If a patient has muscle sensitivity without disc displacement and the dentist has difficulty getting the patient into centric relation, a full-coverage hard splint would be a good choice. Full-coverage hard splints can also reduce or create strain on the ligament. Conversely, they have the potential benefit of increasing patient awareness to a point where the dentist is better able to establish trust and confidence. The choice of which splint to use largely depends on the situation; there is no "one size fits all" solution to pain.23-27
There are multiple types of full-coverage hard splints.26,27 The Pankey/Dawson splint is a mandibular flat-plane appliance with no angles that does not displace the disc or the joint posteriorly. The maxillary anterior guidance orthotic (Michigan) splint, commonly taught in dental school, is a hard acrylic splint covering the maxillary teeth, with a ramp on it. The theory here is to keep all guidance away from the posterior teeth. A Tanner appliance has some semblance of occlusion built in. It opens the vertical slightly while the disc and joint position are maintained, allowing the muscles to relax so the dentist can determine where the joint is for diagnosis.
Hybrid Appliances
Hybrid appliances have a multitude of applications; sometimes more than one can be used at a time. The anterior bite plane is popular with some dental educators; this is likely because it is easy to create, is easy to adjust, and has a wide variety of applications. When an anterior bite plane is combined with a lingual ramp behind the teeth, it is referred to as a Farrar appliance and can be extremely useful if the dentist suspects the patient has untreated obstructive sleep apnea. The Farrar appliance does not distalize the joint; it maintains the patient's vertical with the anterior bite plane portion while preventing the patient's jaw from slipping backward with the lingual ramp. The posterior pivot (Gelb) has only posterior occlusion. The Gelb appliance has many uses, but patients must be cautioned against wearing it more than 12 hours per day or more than 3 months because an anterior open bite will develop with excessive wear. A wrap-around Hawley with anterior stops is taught by Kois. A benefit of the Kois splint is that it can be used if the dentist were to equilibrate the occlusion for restoration purposes.26 Instead of needing to repeatedly manipulate the patient or change leaves, the splint can be used as a guide. The dentist can have the patient bite down on the splint and remove it over time. The dentist can begin to pick up on the posterior stops and inferior areas, moving things around until a good spot is found. The difficult part of any type of equilibration is that it can reduce the vertical, an effect that is unhealthy for the joint. The nociceptive trigerminal inhibition (NTI) splint is essentially an anterior bite plane, but smaller, and is also a possibility.
Again, hybrid appliances should not be worn 24 hours a day. This is especially true of a posterior pivot because it changes the bite in a way that can only be resolved through restorative dentistry or orthodontics. If the likelihood of bite change is high, the dentist should have a discussion with the patient ahead of time where the patient is fully informed of the outcomes of treatment. With all hybrid appliances, the primary upside is relieving pain.28
Critical Steps in Delivery of Any Appliance
If the dentist has a diagnosis and has determined treatment, the choice of appliance should not be random. There are critical steps in the delivery of any appliance. The clinician should have two different-colored tapes or ribbon, appropriate burs in place, adequate equipment, a polishing system, and knowledge. An example of the ideal setup begins with drying teeth before putting marks on them. The clinician can place a tissue on articulating ribbon holders for this purpose. Then, the red articulating ribbon is used, followed by the blue. In the author's experience, it is best to have two of everything prepared because patients tend to favor whichever side the articulator and holder are put in. If the clinician puts them only on the right, the patient will try to bite only on that side. Because of this shift, the dentist will not have accurate information. Red normally is used to observe what happens side to side; blue normally is used to check the observations in vertical. Finally, the bur setup should involve differently shaped burs.
When the Bite Is Not the Problem
Awareness of sleep bruxism is growing in the dental community. In 2005, the American Academy of Sleep Medicine (AASM) defined sleep-related bruxism as a sleep-related movement disorder, similar to restless leg syndrome or oral parafunctional activity (grinding or clenching during sleeping).29 It is usually associated with sleep arousals. As of 2014, the definition has changed slightly. The AASM now defines sleep bruxism as "a repetitive jaw-muscle activity characterized by clenching or grinding of the teeth and/or by bracing or thrusting of the mandible."30
In a 2014 study, Hosoya et al31 found a correlation between obstructive sleep apnea syndrome and high risk of sleep bruxism. Patients must be screened for the risk factors associated with sleep bruxism. If sleep bruxism is a possibility, a sleep physician should evaluate the patient. A board-certified sleep physician can provide a face-to-face consultation appointment and proper diagnosis. Patients who present with sleep bruxism have hypersensitivity of the teeth, scalloped tongue and cheek indentations, envelope of function issues, masticatory muscle soreness, and TMJ noise and/or locking. Sleep apnea tends to involve tiredness and snoring. Factors indicating sleep apnea and sleep bruxism must be identified during the patient history portion of a pretreatment evaluation.
Conclusion
Employing occlusion effectively in practice nec-essitates identification of common occlusion problems, examination of the occlusion and TMJ, and treatment of patients who experience pain. A thorough understanding of the keystone tooth concept, muscle bracing, and sleep bruxism also should become part of the working knowledge of general dentists. Essential skills to gain awareness of where a patient's bite is and what is potentially a dangerous situation are locating centric relation and centric occlusion and evaluating the muscles of mastication, range of motion, and joint displacement. This information relies on a comprehensive pretreatment evaluation that explores patient history of occlusion, bite, muscles, and TMJ to better understand the difference between patients who are completely safe for restorative work and those who necessitate more caution. The examination should proceed from "outside the mouth" concerns to "inside the mouth," complete with examining the masseter, temporalis, medial pterygoid, and lateral pterygoid. Load testing allows the clinician to determine if load on the joint causes pain, while a classification system should be used to diagnose disc displacement. Treating disc displacement and muscle-bracing pain depends on specific appliances, ranging from full-coverage hard splints to hybrid appliances. Ultimately, it is crucial to recognize the distinction between issues arising from bite versus sleep bruxism. The combination of all these factors is central to successful application of occlusion in general practice.
References
1. Palaskar JN, Bansal S. Centric relation definition: a historical and contemporary prosthodontic perspective. J Indian Prosthodont Soc. 2013;13(3):149-154.
2. Sandhu P. Centric relation to maximum intercuspation. Spear Education. http://www.speareducation.com/spear-review/2017/05/centric-relation-to-maximum-intercuspation-slide-part-1. Accessed November 27, 2017.
3. Bloom DR, Padayachy JN. Increasing occlusal vertical dimension: why, when, and how. Br Dent J. 2006;200(5):251-256.
4. Swenson AL, Oesterle LJ, Shellhart WC, et al. Condylar positions generated by five centric relation recording techniques. Oral Biology and Dentistry. http://www.hoajonline.com/oralbioldent/2053-5775/2/8. Accessed November 27, 2017.
5. Upadya R. When to use an anterior deprogram-mer appliance and why. The Dawson Academy. http://dental.thedawsonacademy.com/bid/117922 When-to-Use-an-Anterior-Deprogramming-Appliance-and-Why. Accessed November 17, 2017.
6. Long JH. Loading centric relation with a leaf gauge. J Prosthet Dent. 1973;29(6):608-610.
7. Klar NA, Kulbersh R, Freeland T, Kaczynski R. Maximum intercuspation-centric relation disharmony in 200 consecutively finished cases in a gnathologically oriented practice. Seminars in Orthodontics. 2003;9(2):109-116.
8. Čimić S, Badel T, Šimunković SK, et al. Centric slide in different Angle's classes of occlusion. Ann Anat. 2016;203(1):47-51.
9. Abraham AP, Veeravalli PT. A positional analyzer for measuring centric slide. J Indian Prosthodont Soc. 2012;12(4):216-221.
10. McDonald EA. The fundamentals of occlusion and jaw function. Inside Dentistry. 2016;12(11):35-41.
11. Goldstein M. Bite-management considerations for the restorative dentist. Dentistry Today. http://www.dentistrytoday.com/restorative-134/1787--sp-1787181166. Published January 1, 2008. Accessed December 1, 2017.
12. Eiseman NA, Westover MB, Mietus JE, et al. Classification algorithms for predicting sleepiness and sleep apnea severity. J Sleep Res.2012;21(1):101-112.
13. Dupont JS, Brown CE. Provocation testing to assist craniomandibular pain diagnosis. Cranio. 2010;28(2). http://www.freepatentsonline.com/article/CRANIO-Journal-Craniomandibular-Practice/254013126.html. Accessed Dec-ember 1, 2017.
14. Brady LA. Understanding joint sounds. LeeAnnBrady.com. https://leeannbrady.com/occlusion-tmd/understanding-joint-sounds. Accessed December 2, 2017.
15. Solow RA. Clinical protocol for occlusal adjustment: rationale and application. Cranio. 2017. doi: 10.1080/ 08869634.2017.1312199
16. Thanathornwong B, Suebnukarn S. Clinical decision support model to predict occlusal force in bruxism patients. Health Inform Res.2017;23(4):255-261.
17. Bag AK, Gaddikeri S, Singhai A, et al. Imaging of the temporomandibular joint: an update. World J Radiol. 2014;6(8):567-582.
18. Stagnitti A, Marini A, Impara L, et al. Duplex Doppler ultrasound study of the temporomandibular joint. J Ultrasound. 2012;15(2):111-114.
19. Sharma S, Crow HC, Kartha K, et al. Reliability and diagnostic validity of a joint vibration analysis device. BMC Oral Health. 2017;17(1):56.
20. Piper M. Manual for Intermediate to Advanced TMD Treatment. St Petersburg, FL: Center for Advanced Dental Study; 1999:1-17.
21. Bush FM. Occlusal therapy in the management of chronic orofacial pain. Anesth Prog. 1984;31(1):10-16.
22. Lobbezoo F, Brouwers JE, Cune MS, Naeije M. Dental implants in patients with bruxing habits. J Oral Rehabil. 2006;33(2):152-159.
23. Türp JC, Komine F, Hugger A. Efficacy of stabilization splints for the management of patients with masticatory muscle pain: a qualitative systematic review. Clin Oral Investig. 2004;8(4):179-195.
24. Raphael KG, Marbach JJ, Klausner JJ, et al. Is bruxism severity a predictor of oral splint efficacy in patients with myofascial face pain? J Oral Rehabil. 2003;30(1):17-29.
25. Glaros AG, Owais Z, Lausten L. Reduction in parafunctional activity: a potential mechanism for the effectiveness of splint therapy. J Oral Rehabil. 2007;34(2):97-104.
26. Splint Appliance Selection Guide. Great Lakes Orthodontics. https://www.greatlakesortho.com/content/files/resources/SplintApplianceSelectionGuide_S222.pdf. Accessed: December 7, 2017.
27. Dylina T. The basics of occlusal splint therapy. Dentistry Today. http://www.dentistrytoday.com/prosthodontics/prosthetics/1716. Published July 1, 2002. Accessed December 7, 2017.
28. Seedorf H, Scholz A, Kirsch I, et al. Pivot appliances - is there a distractive effect on the temporomandibular joint? J Oral Rehabil.2007;34(1):34-40.
29. Sleep related bruxism. In: International Classification of Sleep Disorders: Diagnosis and Coding Manual. 2nd ed. Westchester, IL: American Academy of Sleep Medicine; 2005:189-192.
30. Sleep related bruxism. In: International Classification of Sleep Disorders.3rd ed. Darien, IL: American Academy of Sleep Medicine; 2014.
31. Hosoya H, Kitaura H, Hashimoto T, et al. Relationship between sleep bruxism and sleep respiratory events in patients with obstructive sleep apnea syndrome. Sleep Breath. 2014;18(4)837-844.