You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Dental implants continue to amass widespread acceptance as their success becomes increasingly more predictable. As a result of tremendous advancements in bone grafting materials and ridge preservation and augmentation procedures, implants are progressively easier to place, with ever-growing success rates.
However, despite advancements in materials and techniques that facilitate stable osseointegration, an ample amount of good-quality, natural bone—particularly buccal bone—remains the most significant factor contributing to long-term implant treatment esthetics, functionality, and overall success.1,2 Sufficient bone and the natural bony architecture (ie, ridge density, width, etc) facilitate osseointegration, soft-tissue support, and prosthodontic harmony (eg, full-coverage crown, fixed partial denture, removable prosthesis).3 Therefore, preserving the natural bone during tooth extraction procedures is critically important.
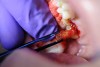
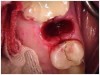
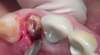
Tooth extractions are usually performed under two circumstances: when teeth are damaged (eg, broken, abscessed) or otherwise nonrestorable due to clinical or financial reasons; and when teeth are healthy and nonsymptomatic (eg, third molars, premolars for orthodontics) (Figure 1).4 Approximately 20 million teeth are extracted annually in the United States, half of which are wisdom teeth.5
Regardless of the circumstances necessitating tooth extraction, an atraumatic versus traumatic approach is best. Unfortunately, conventional extraction techniques have traditionally involved using instruments that are inefficient (eg, forceps that cannot grip deep down on the root), break teeth (eg, elevators that cannot reach deep into the periodontal ligament [PDL]), or otherwise preclude noninvasive extraction techniques (eg, instruments that cannot navigate the PDL space and/or that require a flap).6
For example, conventional extraction practices have dictated using an elevator to work on the crown of the tooth and forceps to grasp that crown and roll it to the buccal. Many forceps are large and cannot grip below the crown, which may fracture when rolled. Additionally, the traditional technique of rolling the tooth to the buccal breaks the buccal bone, while fractures at the tooth crown often require drilling into the bone to remove the root.6,7
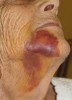
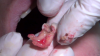
The effects of such traumatic extractions include bone loss that leads to ridge collapse; increased postoperative pain, bruising, and swelling for the patient (Figure 2); greater chance for postoperative infections; and extended healing time. The compromised socket and collapsed ridge present a more difficult site for future implant placement, one that will affect the esthetics and stability of fixed crown-and-bridge restorations, as well as the stability of implant-supported dentures.
Atraumatic Tooth Extraction
Therefore, atraumatically extracting teeth is becoming increasingly important to satisfy patient demands and ensure long-term implant function and esthetics. By avoiding injury to the bone when removing a tooth, the socket and natural bony architecture are preserved and ridge integrity is more likely to be maintained.8 Regardless of whether or not bone grafting will be performed, a sufficient ridge remains for implant placement, better esthetics for crown-and-bridge restorations, and improved stability for partial dentures.
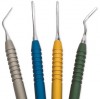
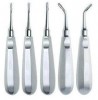
Contributing to clinicians’ abilities to perform atraumatic extractions has been the introduction of new instruments and techniques designed to loosen the tooth in the socket, remove the tooth up and out of the socket without destroying the bone, and ultimately preserve the bony and gingival architecture.9 Among the instruments available for atraumatic extractions are thin and sharp PDL knives, periotomes (Figure 3), mechanically designed forceps (Figure 4), and twisting elevators (Figure 5), among others (Figure 6).6,9,10 These instruments enable navigation deep into the PDL space to sever the PDL, expansion of the bone and dislodging of the tooth, and work on and extraction of the tooth from the root.
Whereas conventional extraction techniques have rolled the tooth to the buccal, atraumatic techniques employ new instruments to extract a tooth in a more apical direction. Rather than push the tooth, in atraumatic techniques the tooth is essentially separated from the bone through a series of steps involving cutting the PDL, pushing away the bone (but not drilling or destroying it), and nudging the root to dislodge it as the socket is expanded, thereby establishing a path of extraction.
Atraumatic Tooth Extraction Technique
Atraumatic tooth extraction techniques are predicated on working on the tooth root deep within the PDL space, which provides the clinician more control throughout the entire procedure. This process is facilitated with the use of forceps that are easy to manage and able to grip deep on the root, which enables control of the extraction and preservation of the socket.
Step 1. Before undertaking an extraction, examining a radiograph is necessary in order to assess the patient’s bony architecture and bony defects, and determine the presence of curved, single, or multiple roots; abscesses or fractures; widened PDL space; and the crown-to-root ratio.11 The clinician should also examine whether the tooth is impacted and if a furcation is involved; determine how the tooth is positioned and whether the gingiva is swollen and infected; and assess the severity of decay and how much tooth structure is visible and/or accessible (ie, Is a flap necessary?). Each of these factors affects the ease or difficulty with which the extraction can be completed. Other considerations include how wide patients can open their mouth, whether they have a large tongue or cheek, and their overall health status. Whether the patient is psychologically ready for an extraction (eg, fearful) can also affect the ease or difficulty of the procedure.
Step 2. Once the radiographic assessment has been completed, the path of extraction is determined to guide the procedure.
Step 3. After determining the path of extraction, the atraumatic extraction can be initiated by slowly entering the socket using very thin instruments (eg, periotome, luxator, PDL knife), working deep within the PDL space and around the tooth. The motion resembles cutting and filing in a manner that pushes and nudges the tooth root. Although this is traditionally accomplished from the mesiobuccal aspect, the instrument used should be thin enough to allow working around all areas, including the buccal aspect. Within the PDL space, the socket is expanded as the PDL is cut, thereby loosening the tooth.
Step 4. Once the tooth is loose, forceps capable of gripping the tooth deep on the root are used to grab at the root and lift the tooth up and out of the socket (Figure 7), rather than rolling it into the buccal bone, as has been conventional practice. With this atraumatic approach, many times the tooth will become so loose that it “pops” right out of the socket, enabling removal with fingers.
Single-Rooted Teeth
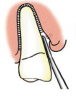
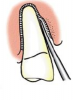
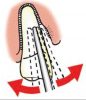
For single-rooted teeth, a PDL knife can be used to “navigate” the PDL space, severing the ligament and displacing the root simultaneously by first cutting and then feeling around the tooth in the PDL space using controlled, apical pressure (Figure 8 and Figure 9). When resistance in the sulcus is encountered, the clinician should “push and nudge” the root with a slight twisting motion (Figure 10). If the root moves, it is then possible to work deeper into the PDL space, causing the root to completely dislodge from the socket for removal.
Additionally, with single-rooted teeth the instrument should be worked along the strongest part of bone. For example, maxillary teeth are usually easiest to remove when worked from the palatal, mesial, distal, and palatal aspect again to loosen the tooth. It is from the palatal aspect that the most leverage can be gained (Figure 11). The buccal aspect should be avoided as much as possible.
Multiple-Rooted Teeth
Extracting multi-rooted teeth begins by first loosening them, expanding the socket in a similar fashion as described earlier, and then sectioning the tooth (if necessary) so that each root can be removed individually.
Curved-Rooted Teeth
If the root is curved (eg, mandibular molars), the path of extraction should follow the direction of the curve. Otherwise, the root/tooth will break. In cases involving first molars, the mesial root is sometimes curved and the distal root is straight. The instrument(s) should be worked deep in the mesial aspect to enable lifting the tooth up and out distally; many times the tooth can be removed completely intact, curved root and all (Figure 12).
Soft, Decayed Root
When the tooth root is soft due to the presence of decay, an abscess, or infection, the decay must be removed first so that instruments can be worked between solid tooth structure and bone. Then, the instruments are worked within the PDL space along the solid root using the previously described cutting, filing, and nudging motion to loosen and dislodge the tooth. Note that sometimes when teeth are infected and/or have an abscess, the PDL space is widened, which can facilitate navigating the instrument(s).
Mesially Tilted Teeth
The mesial defects often associated with teeth that are mesially tilted (eg, usually the mandibular second molar) can be used to the clinician’s advantage during extraction. The instrument(s) is placed into the mesial defect, working it deep on the mesial root to begin lifting it. In some instances when extracting a tilting second mandibular molar (ie, impaction), use of a handpiece is required to remove only enough bone to expose a path of extraction and enable instrument access to the PDL. The instrument(s) can then be worked in deep into the sulcus to cut the PDL and slowly nudge the tooth. Repeat handpiece use may be required to facilitate deeper instrument access.
Other Considerations
When performing an atraumatic extraction, supportive hand positioning can make the experience easier for the patient. For example, the patient’s jaw should be supported to protect the temporomandibular joint, and clinicians can place their finger near the buccal aspect of whichever tooth they are working on to protect the patient; if an instrument slips, the clinician’s finger will be hit and not the patient. This hand positioning also provides patients with a sense of security.
Example of Atraumatic Extraction
In a case involving the extraction of a tooth with severely curved roots (ie, tooth No. 31 with a 90-degree angle of both the mesial and distal roots) and large decay on the crown, the instrument was worked deep into the mesiobuccal aspect of the sulcus. The instrument was worked slowly with pushing, nudging, cutting, and filing motions until engagement on a root surface was felt. At that point, the clinician began to slowly twist and elevate along the direction of the root.
The tooth began lifting up and back, at which point the instrument was worked deeper onto the root, engaged further, and slightly twisted, continuing to work the tooth up and out. This was repeated until the tooth could be completely removed with fingers.
Had this extraction been performed according to traditional methods, a flap would most likely have been made and most of the buccal bone drilled away to enable pushing and grabbing of the tooth to remove it. Such a procedure would have been much more traumatic and caused greater injury to the patient.
Conclusion
Every case requiring extraction is different, but the procedure can be a positive experience for the clinician and the patient when good atraumatic techniques are followed and advanced instruments and armamentarium are used. Each situation should be thoroughly assessed. The clinician’s degree of confidence and skill will affect the approach undertaken when performing an atraumatic extraction. This includes selecting instruments from among the many new options that are designed to work deep into the PDL space to push, cut, loosen, and lift the tooth from the socket. By atraumatically extracting teeth, bone loss and ridge collapse can be prevented, and a site more conducive to implant stability preserved.
ABOUT THE AUTHOR
Eric Schuetz, DMD
Private Practice, North Miami Beach, Florida
REFERENCES
1. Sakka S, Coulthard P. Bone quality: a reality for the process of osseointegration. Implant Dent. 2009;18(6):480-485.
2. Tatum OH Jr, Lebowitz MS. Anatomic considerations for dental implants. J Oral Implantol. 1991;17(1):16-21.
3. Block MS. Dental extractions and preservation of space for implant placement in molar sites. Oral Maxillofac Surg Clin North Am. 2015;27(3):353-362.
4. Jamghili H, Greenwood WJ, Guevara PH, Dunn WJ. Reasons for non-third molar extractions in a military population. US Army Med Dep J. 2016 Jan-Mar:85-92.
5. Friedman JW. Prophylactic extraction of third molars: a public health hazard. Am J Public Health. 2007;97(9)1554-1559.
6. El-Kenawy MH, Ahmed WM. Comparison between physics and conventional forceps in simple dental extraction. J Maxillofac Oral Surg. 2015;14(4):949-955.
7. Macgregor AJ. Factors affecting fracture of teeth during extraction. Br J Oral Surg. 1969;7(1):55-62.
8. Leblebicioglu B, Hedge R, Yildiz VO, Tatakis DN. Immediate effects of tooth extraction on ridge integrity and dimensions. Clin Oral Investig. 2015;19(8):1777-1784.
9. Misch CE, Perez HM. Atraumatic extractions: a biomechanical rationale. Dent Today. 2008;27(8):98-101.
10. Sharma SD, Vidya B, Alexander M, Deshmukh S. Periotome as an aid to atraumatic extraction: a comparative double blind randomized controlled trial. J Maxillofac Oral Surg. 2015;14(3):611-615.
11. de Oliveira RC, Leies CR, Lindh C, Ribeiro-Rotta RF. Bone tissue microarchitectural characteristics at dental implant sites. Part 1: identification of clinical-related parameters. Clin Oral Implants Res. 2012;23(8):981-986.