You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
GLOSSARY
abdominal support bar: a bar on an assisting stool that is in front of the operator.
double articulating headrest: headrest on a patient chair that adjusts in multiple planes to optimally support the patient’s head and neck.
flat headrest: flat headrest on a patient chair that only slides in and out.
fulcrum: a point of rest about which an object turns.
ischemia: decreased oxygenation due to a mechanical obstruction of the blood supply.
ligaments: a band of strong tissue-connecting bones.
multi-factorial: having more than one cause.
mechanical stabilization: stabilization provided by a source external to the body.
muscle imbalance: a muscle on one side of a spine or joint becomes stronger and shorter, while the opposing muscle becomes weaker and longer. This condition often results from repeated asymmetrical postures.
microtrauma: structural damage to the musculoskeletal system occurring on a microscopic scale.
occiput: refers to the occipital bone, the back part of the head.
Over-the-Patient (trans-thoracic) delivery system: a type of delivery system that is positioned directly over the patient’s chest.
physical stabilization: stabilization that is provided by the body’s internal postural muscles.
postural stabilizing muscles: muscles located close to the spine that function primarily to stabilize the body in upright posture for long periods of time.
ratcheting arm: bar on an assisting stool that adjusts inward toward the center of the chair, not just around the periphery.
rear-delivery system: a type of delivery system that is located behind the patient’s head.
scoliosis: a lateral curvature of the spine, to the left or right, which may be congenital (from birth) or functional (due to work-related postures).
spinal disc: fibrous discs located between each vertebrae that allow movement of the spine.
tendons: a fibrous cord or band that connects a muscle with its bony attachment.
torso support bar: a bar on an assisting stool that is positioned at the side of the assistant.
transverse abdominal muscles: the deepest group of abdominal muscles, which provide stabilization to the spine.
ERGONOMICS AND THE DENTAL ASSISTANT
Ergonomics is the science of fitting jobs to the people who work them. The goal of an ergonomics program is to reduce work-related pain and injuries when a major part of the worker’s job requires reaching, bending over, awkward positions, continuous force, or repetitive motions. As it applies to dental assisting, ergonomics involves the design of operatory layouts, delivery systems, stools, and procedures that minimize excessive reaching, gripping, twisting, and leaning. Some jobs require workers to intermittently deviate from their optimal posture throughout the workday. Unfortunately, in dental assisting, frequent rotation often occurs repeatedly to one side, which can result in muscle imbalances and pain.4,5
Additionally, assistants are often required to hold one posture for prolonged periods of time, which may cause painful muscle ischemia.6 Therefore, an effective dental ergonomics program requires that the human body also be addressed with frequent chairside stretching and specific exercise to develop balanced musculoskeletal health.
Implementing ergonomic and injury prevention techniques into the workday will mean less likelihood of fatigue, job burnout, musculoskeletal disorders, and better morale.
MSDs IN DENTAL ASSISTING
A musculoskeletal disorder (MSD) may be defined as a disorder of the muscles, tendons, peripheral nerves, or vascular system not directly resulting from an accident (a slip or fall). These disorders are considered to be work-related when the work environment and the performance of work contribute significantly to the development of a multifactorial disease.7
The most frequently reported MSD among assistants is chronic low back pain.1,2 Other common sites of pain include the neck, shoulders (right more than left), legs, arms, and hands. Left untreated, this pain may result in muscle imbalances, ischemia, nerve compression, and joint or disc degeneration. Warning signs and symptoms of an MSD include:
• Decreased strength (example: gripping strength in assistants).
• Decreased range of motion (example: neck rotation in assistants).
• Pain or burning.
• Shooting or stabbing pain into an arm or leg.
• Swelling or inflammation.
Maintaining optimal musculoskeletal health for dental assistants means understanding the unique muscle imbalances to which they are prone and how various working postures, positions, adjustment of ergonomic equipment, and exercise can positively or negatively affect their musculoskeletal health.
CONTRIBUTING FACTORS TO MSDs
The causes of work-related musculoskeletal pain can be attributed to numerous risk factors, including prolonged static postures, repetitive movements, poor seating, suboptimal lighting, poor positioning, genetic predisposition, mental stress, physical conditioning, and age.8-10 Each dental team member is predisposed to pain or injury in slightly different areas of the body depending on his or her tasks and positioning in relation to the patient. For example, assistants are predisposed to a higher incidence of low back pain, largely due to holding one position for a prolonged period in repeated forward and sideleaning postures. Over time, these postures can lead to microtrauma, or damage that is occurring on such a small scale, the assistant does not feel it until the cumulative structural damage results in pain. The body is constantly repairing this microtrauma; however if breaks are infrequent, the rate of damage can exceed the rate of repair. Pain or an MSD may result.
Three primary types of microtrauma inherent to dental assisting are muscle imbalances, muscle ischemia, and increased disc pressures. To better understand the microtrauma, we will briefly review spinal anatomy.
SPINAL ANATOMY AND MICROTRAUMA
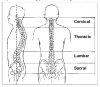
The spine has three movable curves when viewed from the side (Figure 1). When the curves of the spine are present and balanced against the center of gravity, and the spine is straight from a posterior view, the spine is supported mostly by the bony structure of the vertebrae resting on top of one another. In this position there is less stress on the surrounding muscles, ligaments, and discs, and microtrauma is lessened.
Muscle Ischemia
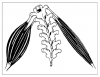
When these curves become flattened (Figure 2) or the spine is bent to one side (Figure 3), the spine depends increasingly on muscles, ligaments, disks, and soft tissue to remain erect. As posture deviates from neutral, the muscles must contract harder to maintain working posture. This increased stress can cause muscle ischemia. When a muscle is constantly contracted for a prolonged period, the pressure inside the muscle rises and can occlude blood flow to the muscle. When muscles do not receive the needed oxygen and nutrients, and lactic acid cannot be removed, painful muscle ischemia can occur.11 This oxygen deficiency also lowers the effective working level of the muscle. Even in optimal seated posture, more than 50% of the body’s muscles must contract to hold the body motionless while resisting gravity.12
MUSCLE IMBALANCES
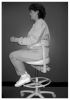
Prolonged leaning postures (Figure 3) can lead to muscle imbalances. Muscles on one side of a spine or joint become tighter and stronger, while muscles on the other side become longer and weaker (Figure 4). Over time, these imbalances may hold the spine in improper alignment not only in the operatory, but outside as well. In assistants, a functional scoliosis may develop, where the spine is curved to one side as a result of constant leaning in the operatory.13 These asymmetrical forces on the spine can cause misalignment of the spinal column and loss of range of motion in one direction over the other. Nerve compression and spinal disc degeneration can result.
Increased Disc Pressure
Microtrauma can also result from the increased disc pressuresin seated postures. When seated, pressure in the low back spinal discs increases by 40% over pressure from standing. When sitting, leaning forward, and rotating, a position often assumed by dental assistants, the pressure increases to 400%,14 making the structure vulnerable to injury. Over time, repeated forward bending can weaken the wall of the disc, resulting in a bulging, or herniated, disc, which can cause low back, buttock, or leg pain.
NEUTRAL POSTURE
One goal of an ergonomics program is to maintain neutral postures. To minimize musculoskeletal strain, the assistant should know the neutral postures of the back, neck, wrist, and shoulder. The more the body deviates from these neutral postures, the more strain is placed on muscles, tendons, ligaments, joints, and spinal discs.
When seated in neutral posture, the assistant’s ear, shoulder, and hip should be vertically aligned (Figure 5). This is often difficult while delivering dental care because there is always some degree of forward head posture, which is why stretching and exercise are imperative to the health of the assistant. Viewed from the back, posture of the neutral spine is straight (Figure 6). The elbows should be held at the sides, and shoulders should be relaxed, not elevated. Wrists should be as straight as possible when holding handpieces, neither flexed nor extended.
ASSISTANT SEATING OPTIONS
Perhaps the most controversial area of ergonomics in dental assisting is use of the dental assisting stool. However, when we consider how microtrauma occurs among dental assistants, recommendations for better seating options become clearer.
Features of dental assisting stools are varied: backrests only, torso support bars only, and those that have both a backrest and a torso support bar. It is probably due to this variety of assistant stools and the positioning challenges faced chairside that assistants have adopted such a wide array of seated postures. Unfortunately, many of these postures contribute to microtrauma that can lead to MSDs. Table 1 lists the most common seating errors and their impact on musculoskeletal health.
Proper Seating
First and foremost, neutral spinal alignment must be supported and maintained during dental assisting. To achieve this, the seated assistant must implement both mechanical and physical stabilization.
Physical Stabilization
Clearly, the assistant cannot maintain neutral vertical spinal posture at all times during treatment. Whenever posture deviates from neutral, stabilization must come from within. The deep transverse abdominal muscleswrap horizontally around the trunk and attach in the low back. When they are strong, these muscles help to stabilize and maintain the low back curve and can help reduce low back pain.15,16 Therefore, the assistant should learn how to physically stabilize the trunk with these muscles whenever the body is in an unbalanced posture (ie, leaning forward or reaching). This can be achieved with the following exercise:
Dental Operator Pivot
Sit tall on the stool. Exhale, and actively pull your navel toward your spine. Your transverse abdominal muscles are now helping to maintain your low back curve. (One common mistake is to suck one’s breath in to pull the spine toward the navel. You should still be able to talk, breathe, and move while holding this contraction.) Assume a relaxed working position with your arms, and using your hips as a fulcrum, pivot forward at the hips, maintaining the contraction throughout the exercise. Strive to make this Operator Pivot exercise a habit throughout the workday:
• any time you must leave a balanced sitting posture.
• to stabilize the lumbar spine and help reduce lower back pain.
Mechanical Stabilization
Mechanical means of stabilizing the spine may be accomplished with an ergonomically designed dental assisting stool. Important features of the stool include:
• Height adjustment
• Footring with adjustable height
• Single torso support bar:
◦ Which adjusts toward center of stool
◦ With adjustable height
OR
• Backrest
◦ Which adjusts forward/backward
◦ With adjustable height
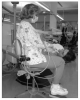
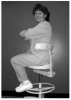
Using a stool with a backrest onlywill allow intermittent periods when the low back muscles can rest and be replenished with oxygen and blood (Figure 7). A second means of mechanical stabilization is using a stool with a single torso supportbar at the side, so the bar is snug under the bottom rib. The end of the bar should be only slightly in front of midline of the torso (Figure 8) and provide enough bar support behind the assistant to rest the back. Both the backrest only and torso support bar designs will allow for easy performance of the operator pivot when needed to gain better visibility into the oral cavity (Figure 9).
To provide effective stabilization, the torso support bar should be adjustable inward toward the side of the assistant (Figure 10). Without this inward adjustment, most assistants must sit toward the edge of their seat to properly use the support bar. In most assisting stool models, this is achieved with a ratcheting support bar.
Support bars that swing around the periphery of the stool cannot be adjusted to snugly provide support at the side of smaller assistants. However, larger-framed assistants may not need this inward adjustment, as the support bars located at the periphery of the stool may already contact their torsos.
ADJUSTING THE ASSISTING STOOL
The assistant’s stool ideally should be used by only one assistant. After the dentist and patient are seated and positioned correctly, adjust the stool as follows. Once the stool is adjusted for the assistant, only the height of the stool should have to be changed, depending on procedures.
For stools with backrest only:
1. Sit with buttocks snugly against the backrest.
2. Adjust the height of the chair so assistant’s eye level is 4 inches to 6 inches above the dentist.
3. Adjust the footring up or down until the assistant’s thighs are parallel to the floor or sloping very slightly downward.
4. Adjust the lumbar support up or down to nestle into the low back curve.
5. Sit tall, with a slight arch in the low back and angle the backrest of the stool forward to snugly support the low back.
For stools with torso support bar only:
1. Sit with buttocks toward back of seat, thighs supported on front of seat.
2. Adjust the height of the chair so assistant’s eye level is 4 inches to 6 inches above the dentist.
3. Adjust the footring of the stool up or down so assistant’s thighs are parallel to the floor or sloping slightly downward.
4. Adjust the height of the torso support bar to just below the bottom rib.
5. Sit tall and adjust the torso support bar inward toward the side of the assistant to fit snugly against the torso under the ribs.
Stools with both backrests and abdominal support bars typically do not adjust inward toward the assistant’s side to provide trunk stabilization. These models may work well for operators with larger torsos; however, they do encourage “bellying over the bar” (Figure 2). Many of these models also have a gap between the backrest and abdominal support bar, where support is needed, but not provided.
ASSISTANT POSITIONING
Once again, our goal in positioning the assistant is maintaining as neutral a posture as possible. For most assistants, sitting with their hip next to the patient’s shoulder is a good guideline (Figure 11). The assistant’s knees should be angled inward toward the head of the patient. Most patient chairs are tapered toward the head of the chair and accommodate this position. If the assistant’s thighs are parallel with the long axis of the patient, more twisting of the trunk is required of the assistant.
If the stool will not raise high enough, consider asking the manufacturer for a taller cylinder. Standard assistant chair height is about 27 inches, however some manufacturers make models 31 inches tall.
It is a good idea for the assistant to alternate between standing and sitting whenever possible. Opportunities should be taken between procedures to stand. This moves the workload from one group of low back muscles to another and may help reduce low back pain.17,18 When working while standing, always remember to perform the dental operator pivot before pivoting forward at the hips to gain better visibility. This helps to stabilize the low back both in standing and sitting.
OPERATORY LAYOUTS
The proximity of the handpieces and instrument tray is an important consideration. The instrument tray should be directly in front of the assistant (Figure 12), preferably with knees underneath the tray. Too far of a reach will result in repeated extended reaching or forward leaning toward the area. All handpieces and instruments should be within a fingertip’s reach when the arm is comfortably extended, without leaning. Hoses on handpieces should be long enough so that excessive force is not necessary while working. One common mistake seen in the operatory is placing the instrument tray to the right of the assistant, necessitating repeated twisting to retrieve instruments.
Rear-delivery-countertop systems are of concern to assistants, especially when they are not adjustable. If, after the assistant is properly positioned chairside, (hip next to patient shoulder) any instruments are out of comfortable reach, try swiveling the patient chair 10° to 20° counter-clockwise (Figure 12). There is usually a lever at the base of the patient chair that will lock and unlock the swivel feature of the patient chair. This may also place the assistant closer to the rear-delivery and instruments.
Over-the-patient delivery systems should be placed as close to the chest of the patient as possible (Figure 13). If positioned over the abdomen, this will encourage twisting of the assistant to retrieve handpieces.
Mobile assisting carts are often a good solution to positioning. They can be moved to the desired position in the operatory, and have storage underneath a sliding assisting tray. Assistants should be able to position their knees easily under the instrument tray of a mobile assisting cart.
LIGHTING
In an efficient team, the assistant should adjust the lighting for the dentist. If the light is difficult to pull along a track or to adjust, contact the manufacturer. Constant pulling on a stiff light can cause shoulder problems.
HANDS AND GLOVES
Assistants may alternate between palm and pen grasps to move the workload over a larger group of hand muscles. Gloves should be loosely fitted across the palm and around the wrist, and snug in the fingers. Fitted gloves are best. Gloves that are too snug across the palm may cause pain at the base of the thumb.
POSITIONING THE PATIENT
It is frequently the job of the assistant to position the patient for the dentist prior to the procedure. Regardless, the assistant should be aware of how the patient chair and headrest operate. For maxillary procedures, it is generally recommended the patient be in a full supine position; for mandibular procedures, the semi-supine position.
The position of the headrest can have a significant impact on visibility into the oral cavity and, therefore, on team member postures. For maxillary procedures, a double articulating headrest should be angled up into the patient’s occiput. This relaxes the patient’s cervical muscles and places the oral cavity in better view. For headrests without an articulation, have the patient move all the way to the end of the headrest. This usually helps the dentist gain closer proximity. Place a towel roll or cervical cushion under the patient’s neck for support. For mandibular procedures, the double articulating headrest should be approximately flat.
THE ASSISTANT AS OPERATOR
The assistant that alternates between assistant and operator positions has the advantage of varying their working positions and is, therefore, less prone to overstressing one part of the body.
Seating considerations for the assistant in the operator position are somewhat different than those in assisting. Close proximity to the patient is an important and often difficult factor for the operator. Tilting the operator seat forward 10° to 15° places the hips higher than the knees and can help gain closer positioning to the patient by opening the hip angle. It also reduces low back disc pressure, helps maintain the lumbar curve, and may help prevent low back pain.19,20 The patient should be positioned low enough so that the assistant can work with neutral shoulder posture—that is, without abducting the arms away from the sides of the body. Forearms should be approximately parallel with the floor, the elbows relaxed at the sides. To operate in this optimal position, the patient will usually have to be placed at lap level, which may increase the visual distance. For this reason, assistants who frequently work in the operator position should consider purchasing magnification (Figure 14).
MAGNIFICATION
Properly adjusted scopes can reduce muscle strain in the neck and upper back by promoting proper neck and shoulder posture.21 Two general styles of scopes are available: through-the-lens and flip-up styles. The TTL, or through-the-lens, style is mounted directly in the lens, is generally lighter weight, and non-adjustable. Flip-up style scopes are heavier in weight, can be flipped up for unmagnified viewing, and are adjustable. For assistants, a magnification of 2X – 2.5X is recommended. Two of the most critical factors to consider when purchasing scopes are working distance and declination angle.
The working distance is the distance from the operator’s eye to the working area. Measure the working distance in your own operatory, if possible, with your arms relaxed at your sides and forearms approximately parallel to the floor.
From an ergonomic and musculoskeletal standpoint, the declination angle of the scopes is your most important consideration. The declination angle is the steepness of the downward viewing angle the scopes allow. A good declination angle will allow you to work with a more upright, neutral head and neck posture (Figure 15). Selecting a larger frame size will allow the manufacturer to place the scope lower in the frame, enabling the best declination angle and, hence, the best neck posture. Although generic magnifying reading glasses are less expensive and improve visibility, they have no declination angle and, therefore, frequently result in poor head posture (Figure 16).
CHAIRSIDE STRETCHING
Even with the best assisting stool and techniques, the assistant will intermittently have to leave optimal posture. When this occurs, it is usually toward one side, predisposing the assistant to muscle imbalances. The assistant should regularly perform chairside stretches that reversethese potentially harmful postures (ie, primarily away from the patient). It is important to know how to stretch safely:
• Move into and out of a stretch slowly. This ensures that you will not overstretch and encourages relaxation of the nervous system.
• Assume the starting position, this is where the stretch begins.
• Breathe in and exhale slowly as you increase the stretch to a point of mild tension or discomfort.
• Hold stretch for two to four breathing cycles.
• Never stretch in a painful range.
Three examples of stretches for the trunk are shown in Figure 17 through Figure 19. Stretches that target the neck, shoulder, and hand/wrist are also important for assistants to perform.
EXERCISE
Because assistants are prone to low back injuries, exercises that strengthen the postural trunk muscles (especially the transverse and oblique abdominal muscles) and stabilize the low back are important to incorporate into an exercise routine. There are many ways to strengthen these muscles. The transverse abdominal muscles may be strengthened by lying on the floor, pulling the navel to the spine, and holding it throughout the exercise while alternately lifting one leg, then the other off the floor (Figure 20). The oblique abdominal muscles may be targeted by lying on the back and alternately reaching one hand toward the opposite knee, lifting only the shoulder blade off the floor. Pilates is an excellent exercise program to target the postural muscles of the trunk and shoulder girdle.
The above are guidelines only. As with all exercise, always consult your physician before beginning any strengthening or stretching programs. Work with a trained healthcare professional to develop a safe and well-rounded strengthening program.
SUMMARY
Using equipment properly, paying attention to proper positioning, and learning about balanced musculoskeletal health can all contribute to preventing pain and injuries in dental assisting. Addressing and preventing muscular pain early on can make the difference between a satisfying, lengthy career in dental assisting or painful, early retirement.
SUGGESTED RESOURCES
Craig C. Pilates on the Ball. Healing Arts Press. Rochester, Vermont 2001.
Egoscue P. Painfree: A revolutionary method for stopping chronic pain. Bantam Publishing. 2000.
Finkbeiner B. Four-handed Dentistry: A Handbook of Clinical Application and Ergonomic Concepts. Prentice Hall. New Jersey; 2001.
Murphy D. Ergonomics and the Dental Care Worker. American Public Health Association. 1998.
Novak J. Posture, Get it Straight! The Berkeley Publishing Group. New York, NY; 1999.
Valachi B. Chairside Stretching and On the Ball Exercise Video Programs for Dental Professionals. Portland, Oregon; 2003. Available at: www.posturedontics.com.
ABOUT THE AUTHOR
Bethany Valachi, MS, PT, CEAS, is a physical therapist, certified ergonomic assessment specialist, and owner of Posturedontics, which she co-founded with Keith Valachi, DDS. A member of the National Speaker’s Association, she presents dental ergonomic seminars internationally and provides in-office ergonomic consultations to help dental professionals avoid injuries and extend careers. She is a published author in numerous dental journals, including the Journal of the American Dental Association, and contributing author to a dental hygiene textbook. She has developed home exercise and chairside stretching video programs specifically for dental professionals. She can be reached at bethany@posturedontics.com or via her website at www.posturedontics.com.
ACKNOWLEGMENTS
Special thanks to the dental team educators at OHSU School of Dentistry for their time and contribution: Tammy Stange, CDA, EFDA; Kimberley Cummins, CDA, EFDA; Debra Hãgg, CDA, EFDA; and Debra Sanchez, CDA, EDFA; and to the dental assistants who modeled for this course: Sandra Morris, Jennifer Craig, Raelene Wohlsein, and Kim Barbeau. Also to Pelton & Crane, Orascoptic Research, and Dentech for providing the ergonomic products for this study course.
REFERENCES
1. Lalumandier J, McPhee S, Parrott C, Vendemia M. Musculoskeletal pain: Prevalence, prevention, and differences among dental office personnel. Gen Dent. 2001;49(2):160-166.
2. Murphy D. Ergonomics and the dental care worker. Washington, DC: American Public Health Association; 1998:151-153.
3. Valachi B, Valachi K. Mechanisms contributing to musculoskeletal disorders in dentistry. J Am Dent Assoc. 2003;134;1344-1350.
4. Van Dieen J. Asymmetry of erector spinae muscle activity in twisted postures and consistency of muscle activation patterns across subjects. Spine. 1996;21(22):2651-2661.
5. Torén A. Muscle activity and range of motion during active trunk rotation in a sitting posture. Appl Ergon. 2001;32(6):583-591.
6. Cailliet R. Soft Tissue Pain and Disability. 3rd ed. Philadelphia: F.A. Davis Company; 1996:1-12, 35, 71, 124, 489-501.
7. World Health Organization. WHO identification and control of work-related diseases. Geneva, Switzerland. WHO technical report; 1985:174:7-11.
8. Rundcrantz BL, Johnsson B, Moritz U, Roxendal G. Occupational cervico-brachial disorders among dentists: psychosocial work environment, personal harmony and life-satisfaction. Scand J Soc Med. 1991;19(3):174-180.
9. Westgaard RH. Effects of physical and mental stressors on muscle pain. Scand J Work Environ Health. 1999;25:19-24.
10. Lehto TU, Helnius HY, Alaranta HT. Musculoskeletal symptoms of dentists assessed by a multidisciplinary approach. Community Dent Oral Epidemiol. 1991;19:38-44.
11. Kumar C. Biomechanics in Ergonomics. Philadelphia, PA. Taylor & Francis; 1999:12-15, 250-254.
12. Ratzon NH, Yaros T, Mizlik A, Kanner T. Musculoskeletal symptoms among dentists in relation to work posture. Work. 2000;15;(3):153-158.
13. Hertling D, Kessler R. Management of Common Musculoskeletal Disorders. 3rd ed. Philadelphia, PA: Lippincott Williams & Wilkins; 1996:551-552.
14. Nachemson A. Disc pressure measurements. Spine. 1981;6:93-97.
15. Hodges P, Richardson C. Inefficient muscular stabilization of the lumbar spine associated with low back pain. Spine. 1996;21:2640-2650.
16. Hides J, Richardson C. Multifidus muscle recovery is not automatic after resolution of acute, first-episode low back pain. Spine. 1996;21:2763-2769.
17. Callaghan J, McGill S. Low back joint loading and kinematics during standing and unsupported sitting. Ergonomics. 2001;44:280-294.
18. Ratzon N, Yaros M, Kanner T. Musculoskeletal symptoms among dentists in relation to work posture. Work. 2000;15:153-158.
19. Hedman T, Fernie G. Mechanical response of the lumbar spine to seated postural loads. Spine. 1997;22:734-743.
20. Harrison D, Harrison S, Croft A, et al. Sitting biomechanics part 1: review of the literature. J Manipulative Physiol Ther. 1999;22(9):594-609.
21. Branson B, Bray K, Gadbury-Amyot C, et al. Effect of magnification lenses on student operator posture. J Dent Educ. 2004;68(3):384-389.