You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Dentists in North America began placing implants in the early 1980s. At the time, it was suggested that after implant placement, surgical sites should be undisturbed for at least 3 to 6 months to prevent micromotion and, thus, enhance osseointegration between the implant and bone.1 However, this timeframe was established empirically; no evidence supported it. As this discussion is focused on immediate implants, that and related terms are presented according to consensus statements in the International Journal of Oral and Maxillofacial Implants supplement in 2004.2
Consensus Statements Regarding Implant Loading and Restoration After Extraction
Depending on the indication, implants and restorations may be placed immediately or at various intervals after tooth extraction.
In early loading,a restoration is placed in contact with the opposing dentition anywhere between 48 hours and 3 months after implant placement,2 while in delayed loading, the prosthesis is attached—as in the early implant days—in a second procedure to occur sometime later than the conventional healing period of 3 to 6 months.2 With immediate loading, a restoration is placed in occlusion with the opposing dentition within 48 hours of implant placement.2
With an immediate implant, everything—tooth extraction, implant placement, and restoration placement—is completed on the same day.3 This differs from early implant placement, in which implant placement occurs in the early stages of healing—ie, 4 to 8 weeks after extraction3—and delayed placement,when implants are placed after the ridge has healed, between 3 and 6 months after extraction.3
Literature on Immediate Implants
Single Implants
Chaushu et al4 in 2001 compared immediate implant placement and restoration loading was compared to non-immediate implantation in single-tooth implants. They reported that placing a temporary restoration on an implant placed in a fresh extraction socket was associated with a 20% failure rate.4
Multiple Implants Versus Single Implants
In a 2002 study by Cooper et al,5 simultaneous extraction, implant placement, and loading of multiple implants were 100% successful in that all 54 implants had survived after 6 to 18 months, based on independent testing of mobility and radiographic evidence of osseointegration.5 In their discussion, the authors wrote, “Advantages to extraction with simultaneous replacement include the maintenance of vertical dimension, elimination of reline procedures and interim denture therapy, and potential improvement of soft tissue healing.”5
A higher success rate can likely be achieved with multiple implants—compared with single-tooth implants—because when a single tooth is extracted and replaced with an implant, a large gap between the implant surface and bone remains. Not enough bone-to-implant contact is present initially. Making adjustments in this case can be problematic due to the need to retain as much bone height as possible for single teeth—especially in the esthetic areas. This is not an issue with full-arch implants, in which the largest circumference of the socket that is most coronal is reduced prior to implant placement. There is much better adaptation of that implant to the bone. This results in much more bone-to-implant contact and, in most cases, much higher primary stability. The other advantage of immediately placing a large restoration on multiple implants is that the implants are splinted together, which, according to the literature, dramatically enhances implant stability.6
Tilting Implants
Impressive survival rates of multiple implants were also demonstrated in a 2003 study of immediately placed All-on-4® restorations using tilted implants.7 Although previous to this a significant amount of information about nonparallel implants existed, the focus remained on placing the implants parallel. However, in this study, because the distal implants were tilted, the investigators were able to reduce the cantilever slightly, leading this to become a popular restoration for many patients.7
Further, a systematic review of the All-on-4 treatment concept for edentulous jaws in which posterior implants were tilted suggested it to be a cost-effective treatment concept with significant advantages for patients, including improved quality of life, reduction in the number of surgical approaches needed, and elimination of the need for prosthesis removal. This review, which was published in 2014, showed high implant survival rates, a 100% prostheses survival rate, and low marginal bone resorption. The tilting of the posterior implants, reported the authors, “allows the final prostheses to hold as many as 12 teeth with only a short cantilever (one molar) and a favorable inter-implant distance.”8
The advantages of tilting implants can be summarized as follows: 1) the amount of cantilever needed to replace molars is reduced, thus lowering stress on the system; 2) implants can be placed in the densest bone, which improves primary stability; 3) anatomic structures, such as nerves and sinuses, can be avoided; and 4) longer implants are allowed, providing more bone-to-implant contact and better primary stability for loading.
The biomechanic advantages of tilting implants is supported in findings by Bevilacqua et al, who examined the influence of cantilever length and implant inclination on stress distribution in maxillary implant-supported fixed dentures.9 In their study, they placed a load of 150 N on the most distal part of the metal framework cantilever and examined it at 0°—ie, parallel—and tilted at 15°, 30°, and 45°, respectively, which reduced the posterior cantilevers and resulted in decreased stress values for all variables.9
Understanding the reason for tilting implants and optimally handling immediate implant cases sets the stage for a discussion for how individual clinicians can approach these cases, which are best handled collaboratively.
Collaborating to Maximize Benefits of Immediate Implants
The main players involved in planning and executing immediate implant treatment generally include the restorative dentist, implant surgeon, laboratory technician, and dental hygienist. Each has an important role.
The leader of this implant team is the restorative dentist, who dictates the restorative treatment. However, the “pilot” who implements the treatment plan of the restorative dentist is the implant surgeon, and it is up to the dental technician to predictably deliver the esthetic outcome desired. The role of the dental hygienist is to follow up with these patients to maintain their restorations. Given that the average complete denture patient returns to the dentist after 10 years, patients with implants need to know that their journeys with dentistry do not end with the placement of an implant-supported denture.
Although, thanks to technology, distance is no longer a factor in collaboration between the dentists and laboratory technicians; excellent communication among them as well as with the patient is paramount.
Issues to Discuss: CALM
The acronym used by the author to represent the main issues that must be handled and effectively communicated to all team members is CALM and for good reason—addressing these often overlapping issues in advance reduces stress and helps treatment go smoothly and predictably. The acronym stands for Cost, Aims of treatment, Liability, and Maintenance, as discussed below.
Cost
The cost of treatment for the patient is based on numerous factors, including fees for the time, materials, and other expenses of the clinician, surgeon, and laboratory. These costs should be assessed and a fee agreed upon by the individuals involved, so a single established total cost of treatment can be presented to the patient with no hidden costs.
A discussion of the cost of treatment with the patient may include how payment will be made. This can involve devising a payment plan or recommending a financing service.
Aims of Treatment
The cost of treatment, of course, will be significantly impacted by the extent and complexity of the procedures and restoration recommended based on team-member collaboration. Together they will need to determine the number of implants, where they will be positioned based on available bone, whether they can be loaded immediately, and the amount of osseous reduction needed to meet prosthetic space requirements.
Although this discussion is about immediate implants and that is often the goal, if implants are not stable, they cannot be loaded; it may not be possible to send the patient home with a fixed restoration.
Liabilities
Planning treatment also involves assessing patient risk based on a review of the medical history at the first patient appointment. Patients at high risk may not be candidates for an extensive surgical procedure. However, this determination—as well as the entire treatment plan—should be collaborative based on the input of all team members, which may include a surgeon, a prosthodontist, and a laboratory technician, reviewing the case together electronically or by phone.
Another important aspect of liability is managing patient expectations. Patients who have failing dentitions need to understand that clinicians do not have the luxury of the try-in and that the esthetic outcome might not be ideal. The full-arch provisional restoration is an excellent communication tool for the final esthetic result.
Maintenance and Complications
The purpose of proper maintenance is the prevention of problems. The dental hygienist plays an important part in the maintenance chain, providing patients with guidance on the tools and techniques they need for home care, providing strict oral hygiene instruction, and stressing the importance of regular recall visits such as were not required for traditional dentures.
However, problems can happen. Sometimes an implant fixture fractures or an implant fails to integrate. Therefore, the team needs to be prepared to deal with such scenarios and perhaps revisit decisions such as whether to load an implant that is not as stable as would be desired or how to deal with fractures that occur at different times—eg, during treatment, during the temporary phase, or 5 years after the final restoration. Every effort should be made to prevent the number-one prosthetic complication—denture teeth popping off the final restorations or the temporary restoration—by ensuring that occlusion has been set up properly and that alveolar reduction is sufficient to provide enough prosthetic space for good support of the denture teeth.
Denture Techniques
Immediate implants with four tilted implants has become a common procedure at least partly because it is more affordable relative to procedures with more implants. Its success requires that the practitioner have a strong understanding of denture techniques, such as tooth position, vertical dimension, and closest speaking space, to be able to handle cases with different complexities.
Case 1
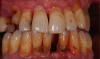
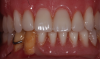
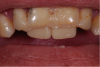
Although the teeth are not esthetic, in this case, the vertical dimension is correct, the incisal position of the maxilla is in the proper position, and the amount of teeth showing is proper (Figure 1). Therefore, all that is required is to take an impression and send it to the laboratory, where the technicians can use the teeth as a guide to set up the final or temporary restoration (Figure 2).
Case 2
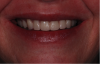
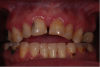
While the vertical dimension is proper in this more complex case, the occlusion and tooth position are not (Figure 3). This case posed the challenge of re-establishing those components and focusing on the additional problem of mobile upper anterior teeth, which made taking the impression difficult and risky. Satisfactorily resolving these issues hinged on the practitioner’s knowledge of denture concepts and where to place the teeth (Figure 4).
Case 3
This case involved a patient with a longstanding tongue-thrusting habit and a large space between the upper and lower teeth (Figure 5). This was corrected in the final restoration, but it required determining where to place the incisal edge of those anterior teeth. Because there was room, it was possible to bond denture teeth to determine whether the position of those teeth was acceptable during the try-in (Figure 6). The laboratory used an impression of this as a guide to set up the case (Figure 7).
Patient Selection
The decision to proceed with any type of dental treatment must consider the current and future needs of the patient. Such is the case when a patient with failing dentition is young and the treatment would require a large amount of bone reduction. It is not yet known how long implants are likely to last, nor whether implant treatment might be detrimental to a young patient’s future treatment needs. With that in mind, the All-on-4 treatment is generally a good option for older patients with failing dentition.
Another aspect of patient selection concerns the patient’s willingness and ability to maintain the restoration properly by complying with recommended hygiene and scheduled recall visits. Intervals can vary; some patients should be seen as often as every 2 months.
The optimal frequency of recall visits can become apparent during the temporary phase—when the provisional prosthesis is removed at different times, including for a final impression and framework try-in. Success and failures of hygiene can be readily observed and discussed in term of the negative impact of poor self-care on the long-term prognosis of the restoration and of the implants. The hygienist is responsible for teaching implant patients how to use the recommended cleaning tools, including manual and electronic flossers and brushes.
Conclusion
Taking a collaborative approach is beneficial for restoring patients’ failing dentitions to offer them the best available treatment. Immediately placing large restorations on multiple tilted implants, as presented above, makes the advantages of implants more affordable and therefore available to more patients than in the past. However, it is important for them to be aware of what is involved. The author recommends that the CALM approach be used by all collaborative team members to maximize the predictability and success of this and other treatments. This means effectively evaluating and communicating aspects of care—Costs, Aims of treatment, Liability, and Maintenance.
References
1. Adell R, Lekholm U, Rockler B, Brånemark PI. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10(6):387-416.
2. Cochran DL, Morton D, Weber HP. Consensus statements and recommended clinical procedures regarding loading protocols for endosseous dental implants. Int J Oral Maxillofac Implants. 2004;19(suppl):109-113.
3. Hämmerle CH, Chen ST, Wilson TG Jr. Consensus statements and recommended clinical procedures regarding the placement of implants in extraction sockets. Int J Oral Maxillofac Implants. 2004;19(suppl):26-28.
4. Chaushu G, Chaushu S, Tzohar A, Dayan D. Immediate loading of single-tooth implants: immediate versus non-immediate implantation. A clinical report. Int J Oral Maxillofac Implants. 2001;16(2):267-272.
5. Cooper LF, Rahman A, Moriarty J, et al. Immediate mandibular rehabilitation with endosseous implants: simultaneous extraction, implant placement, and loading. Int J Oral Maxillofac Implants. 2002;17(4):517-525.
6. Szmukler-Moncler S, Salama H, Reingewirtz Y, Dubruille JH. Timing of loading and effect of micromotion on bone-dental implant interface: review of experimental literature. J Biomed Mater Res. 1998;43(2):192-203.
7. Maló P, Rangert B, Nobre M. “All-on-Four” immediate-function concept with Brånemark System implants for completely edentulous mandibles: a retrospective clinical study. Clin Implant Dent Relat Res. 2003;5(suppl 1):2-9.
8. Patzelt SB, Bahat O, Reynolds MA, Strub JR. The all-on-four treatment concept: a systematic review. Clin Implant Dent Relat Res. 2014;16(6):836-855.
9. Bevilacqua M, Tealdo T, Menini M, et al. The influence of cantilever length and implant inclination on stress distribution in maxillary implant-supported fixed dentures. J Prosthet Dent. 2011;105(1):5-13.