You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Although the dental literature confirms that implant-supported prostheses provide beneficial solutions for patients, technical and biological complications from implant treatments can arise.1-3 After a comprehensive literature review, Goodacre et al4 determined that clinical complications with implants and prostheses were more frequently biomechanical in nature. Calderon et al5 also found that the most common complications involving implants were mechanical and related to attachment components of prosthetic mechanisms, complex load with frequent loosening, fractures, and implant-bone anchoring.
The author suggests that poor design remains the greatest underlying cause contributing to complications with implants and prostheses. In order to prevent potential complications, treatment planning should encompass and consider contingency, priority, and risk perspectives (CPR). Effective CPR evaluation examines the patient’s condition in different ways to establish an ideal and thorough treatment plan. Because CPR is also a universally utilized acronym to describe the emergency protocol for assisting a patient who has experienced cardiac arrest (ie, cardio pulmonary resuscitation), it would be metaphorically appropriate to use it when treatment planning a seriously damaged dentition.
Contingency
Contingency addresses a future event or circumstance that is possible but cannot be predicted with certainty. In some instances, radiographic evaluation of a reconstruction demonstrates that no contingency plan was developed at the time the prosthesis was delivered. This can necessitate removal of the entire implant and restoration complex, and development and placement of a newly designed implant-supported restoration.
For patients with periodontal disease, extensive deficiencies of supporting hard and soft tissues, as well as atrophy of the alveolar ridges, are frequent.6 While prosthetic reconstruction of major tissue defects is possible, creating predictable, functional, and esthetic implant-supported prosthetic restorations is challenging.6 Establishing proper implant position and angulation ensures functional and optimal esthetic implant rehabilitation, helping clinicians predict the successful future of the implants/restorations when a contingency is needed.7
A study completed by the author and colleagues addressed the common complaints associated with removable partial dentures (RPD), including lack of stability, minimal retention, and unesthetic retentive clasping.8 Implants were placed in different areas to provide greater retention in patients with implant-assisted RPD. After utilizing alternative implant and prosthesis designs, a clinical evaluation of at least 1-year follow-up occurred.
In patients with implants used as vertical stops for mandibular distal extension prostheses, extra caution was taken to ensure that the implants were not loaded laterally by creating a single-point contact at the center of the modified healing abutment. The results demonstrated increased patient satisfaction, no radiographic evidence of excessive bone loss, minimal component wear, and stable soft tissues. The focus from a planning standpoint was placing the implant in such a position that eventually, if the patient decided on grafting and placement of additional implants, the previous implant could be utilized in a fixed fashion for possible fixed design in the future.
An example of incorporating contingency in treatment planning includes evaluating a partially edentulous patient with a typical implant-supported restoration and several crowns and/or bridges on the remaining teeth that are experiencing mechanical complications. Extensive decay may occur and require conversion into a full-arch reconstruction. Although there might be a cement-retained restoration in one section, evaluating the contingency can suggest a different solution for the patient. Although a patient may be transitioning into full-arch reconstruction, converting the reconstruction into a screw-retained option in a segmented arch design can provide much easier access and/or lower cost to the patient if or when repair of the prostheses is needed. The clinician could move from one design to the other, providing a contingency plan.
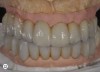
Considering contingency during treatment planning forces clinicians to create a solution for a problem they know will or can occur. It focuses on providing solutions to problems after the implant treatment develops the anticipated complications. For example, a spare set of the implant-supported reconstruction was fabricated utilizing temporary abutments and cold-cure acrylic resin for use if and when a repair of the definitive prosthesis was needed (Figure 1 and Figure 2).
Risk assessment, which is discussed later, has an impact on contingency considerations and, therefore, a patient’s risk must be addressed when determining contingencies in treatment plans. Patients presenting with high functional risk (eg, parafunctional activity, tooth fractures, excessive wear, etc.) will still have parafunctional risk after implant placement, and clinicians must be prepared to properly treat these patients in order to prevent implant damage; they should also be aware that extensive wear and/or fractures may occur to the material used to fabricate the implant-supported restoration. Patients with high biological risk (eg, periodontal disease, systemic compromise, etc.) must also be evaluated and monitored for peri-implant diseases and other health issues after implantation.
One of the most important aspects in evaluating contingency is to share the contingency plan with the patient. This education allows patients to receive an accurate understanding of the reality of their implants and the problems they may or may not encounter after implantation. With a realistic understanding, patients are better prepared to deal with complications associated with their implants.
Priority
Priority in treatment planning culminates in a practical approach to resolving a patient’s problems and providing common-sense treatments. This includes addressing the initial clinical situation, surgical plan, surgical phase, and choice and design of implant and restoration materials.9 It also involves considering the patient’s esthetic, financial, and time constraints, as well as any other limiting factors.
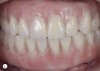
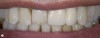
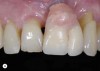
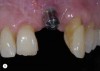
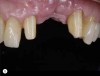
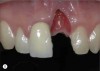
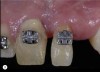
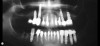
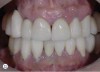
For example, consider the case of a 70+ year-old man who had been inappropriately treated with an implant-supported restoration. Although his lip position and mobility were satisfactory (Figure 3), the dentistry hidden beneath the restoration revealed the extent of poor implant placement and restoration design (Figure 4). Upon removal of the restoration, it was clear the implant was placed in the incorrect position from multiple perspectives—mesial-distal, buccal-lingual, apical-coronal, and angulation (Figure 5). Assessing priorities in this case required consideration of potential alternatives for redesigning the implant-supported restoration.
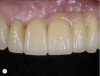
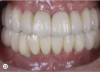
Additional complications and considerations in this case—including removing the implant, grafting, possible multiple implants, orthodontics to optimize the space, and mucogingival correction—were addressed. From a practical perspective, driven partially by the patient’s lip mobility, a traditional tooth-supported restoration with conventional tooth preparation and crown was the approach indicated. While the patient’s mindset influenced the selection of different treatment options (Figure 6 and Figure 7), an essential priority is an understanding of the patient’s risk. By carefully considering the biology of the interaction between the implant-prosthesis complex with the implant site, as well as harmony among the implant-supported restorations and the surrounding hard and soft tissues, clinicians are better prepared to achieve a predictable, esthetic, and practical result.10
Priority also addresses a patient’s finances, desires, and compliance. Costs—both in the time and financial commitment involved—play an important role in determining the type of treatment that is ideal for a given patient; beyond the monetary outlay, they include number of office visits and length of appointments. Today, many treatments are limited to what patients can afford, and finances can determine the type and extent of treatment they receive. A patient’s desires relative to treatment should also be considered as a priority. While esthetics may be the most common, additional considerations regarding a patient’s willingness to undergo extensive and comprehensive therapy should also be considered.
For example, an implant-supported option may become absolutely irrelevant or meaningless if it is suggested to a patient who is a maxillary denture wearer—even if that patient is an excellent candidate for implant therapy in terms of health, anatomy, finances, and time availability—if he or she is happy with a conventional denture. Sometimes clinicians wrongly suggest solutions for problems that patients do not even have, and this, at any given time, may backfire. This is particularly true if a patient is persuaded to undergo therapy without understanding its implications and potential shortcomings; hence, the importance of addressing the patient’s chief concern.
Risk
Risk is the potential that a chosen action or activity, including the choice of inaction, will lead to a loss or undesirable outcome. It includes any threat that the patient or clinician could potentially encounter. In dentistry, it takes seconds to destroy and years to reconstruct (Figure 8 and Figure 9), and this reality can be the greatest threat to reconstruction and implant-supported prostheses. When assessing risks, examining the patient through several different risk filters provides a holistic view of the patient’s condition. A patient’s risk may be present in one or many of these filters.
The biological filter evaluates the patient’s health and condition, including the presence of periodontal disease and the need for treatment. Periodontal disease can lead to bone loss and other complications with surgery, healing, and stability.11 Additionally, patients with periodontal disease prior to treatment may be more susceptible to peri-implant disease after implantation. A health questionnaire can be used, as well as an oral examination, to determine whether patients are at higher risk for biological complications for healing and after-treatment due to underlying health conditions or being systemically compromised—for example, through bisphosphonate use.
The structural filter evaluates the stability of the restorations and oral cavity. A patient with high structural risk demonstrates extensive ill-fitting restorations, numerous endodontically treated teeth, active decay, aggressive preparations/large cast posts and cores, or lack of adequate ferule effect—all of which can also affect the structural integrity of the treatment.12 High structural risk is likely the reason for implantation; eliminating the source of the problem can help to reduce the need for structural contingencies. The structural filter can be affected by material selection,12 occlusion, and wear. Due to the individual nature of occlusion, custom treatment and assessment are necessary for determining ideal occlusion.13
High functional risk can be seen in patients with severe parafunctional activity (eg, extensive abrasion-snapped teeth, tooth fractures, etc.), and while implants may be necessary, many patients’ parafunctional activity returns after implantation. Clinicians are tasked with over-engineering the restorative design (ie, increasing the number of implants) and providing a system that will withstand the patient’s susceptibility to fracture due to parafunctional activity.
Finally, the esthetic risk filter is more subjective. Patient satisfaction, tooth position, extractions, missing teeth, shade, and shape affect esthetics. Lip mobility (ie, smile line) is also a critical parameter when assessing the patient’s esthetic risk. The restorative design, including implant distribution, number of implants, type of retention—eg, splint, screw-retained, cement-retained—and material choice are affected by a combination of esthetic risk and other risk factors.
Treatment Planning and CPR – Contingency, Priority, Risk
After evaluating the contingency, priority, and risk, a clinician can determine the prognosis. Because every patient presents with different risks, priorities, and contingency factors, a standard treatment plan will not work for every patient. Therefore, a customized treatment plan is necessary to develop a plan based on the patient’s CPR. For example, utilizing the CPR protocol, a segmented reconstruction can be planned for a patient—if appropriate—that consists of an implant-supported screw-retained restoration (Figure 10 through Figure 15). By combining these three assessment tools, clinicians are able to create better solutions and treatment plans for their patients.
Conclusion
Poor planning remains the main cause of biomechanical complications with implant-supported restorations. Therefore, clinicians must develop thoughtful solutions for their patients’ long-term benefit. Designing implant-supported restorations utilizing the CPR—ie, contingency, priority, and risk assessment—protocol represents a well-rounded approach for ideal treatment planning. Contingency facilitates planning to resolve problems that may occur in the future. Priority encourages use of the most practical therapeutic approach. Finally, risk addresses what could go wrong. By adopting a CPR philosophy, clinicians are equipped to assess the risks and design successful and long-lasting implant restorations.
Acknowledgment
The author would like to thank the following technicians for the work depicted in this article: Jaro Urbaniski, CDT (Figures 1 and 2); Joel Lopez, CDT (Figure 7); and Arturo Godoy, CDT (Figures 12, 13, and 15).
About The Author
Ricardo Mitrani, DDS, MSD, has a private practice in Mexico City, Mexico.
References
1. Walton JN, MacEntee MI. Problems with prostheses on implants: a retrospective study. J Prosthet Dent. 1994;71(3):283-288.
2. Bozini T, Petridis H, Garefis K, Garefis P. A meta-analysis of prosthodontic complication rates of implant-supported fixed dental prostheses (FDPs) in edentulous patients after an observation period of at least 5 years. Int J Oral Maxillofac Implants. 2011;26(2):304-318.
3. Pjetursson BE, Thoma D, Jung R, et al. A systematic review of the survival and complication rates of implant-supported fixed dental prostheses (FDPs) after a mean observation period of at least 5 years. Clin Oral Implants Res. 2012;23(Suppl 6):22-38.
4. Goodacre CJ, Bernal G, Rungcharassaeng K, Kan JY. Clinical complications with implants and implant prostheses. J Prosthet Dent. 2003;90(2):121-132.
5. Calderon PS, Dantas PM, Montenegro SC, et al. Technical complications with implant-supported dental prostheses. J Oral Sci. 2014;56(2):179-184.
6. Holst S, Blatz MB, Bergler M, et al. Implant-supported treatment in cases with hard- and soft-tissue defects. Quintessence Int. 2005;36(9):671-678.
7. Holst S, Blatz MB, Wichmann M, Eitner S. Clinical application of surgical fixation screws in implant prosthodontics—Part I: positioning of radiographic and surgical templates. J Prosthet Dent. 2004;92(4):395-398.
8. Mitrani R, Brudvik JS, Phillips KM. Posterior implants for distal extension removable prostheses: a retrospective study. Int J Periodontics Restorative Dent. 2003;23(4):353-259.
9. Holst S, Blatz MB, Hegenbarth E, et al. Prosthodontic considerations for predictable single-implant esthetics in the anterior maxilla. J Oral Maxillofac Surg. 2005;63(9 Suppl 2):89-96.
10. Zadeh HH, Daftary F. Implant designs for the spectrum of esthetic and functional requirements. J Calif Dent Assoc. 2004;32(12):1003-1010.
11. Shumaker ND, Metcalf BT, Toscano NT, Holtzclaw DJ. Periodontal and periimplant maintenance: a critical factor in long-term treatment success. Compend Contin Educ Dent. 2009;30(7):388-394.
12. Spear FM. Treatment planning materials, tooth reduction, and margin placement for anterior indirect esthetic restorations. Inside Dent. 2008;4(1):4-13.
13. DiMatteo AM. Pounding on the occlusion pulpit—where in lies all the controversy? Inside Dent. 2008;4(3).