You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
With the introduction of a new generation of chairside computer-aided design/computer-aided manufacturing (CAD/CAM) systems, what was once possibly considered a cumbersome toy for a small niche of dental enthusiasts has quickly transformed to become the standard of care. This new generation of systems allows for an ease of use, accuracy, and speed that has never been seen before.
Features such as customized, high-definition black-and-white photographic models designed to specifically highlight the reflectance of enamel and dentin as well as realistic color models that aid in tissue and tooth identification allow for a new level of precision, and offer a great advantage compared with looking at a poured stone model. Not to undermine other improvements, this additional information superimposed on the digital model has propelled chairside impressions and laboratory communication to a new level. Nevertheless, many clinicians still remain reluctant to adopt this technology into their practice, and four often-repeated concerns clinicians have about chairside CAD/CAM dentistry relate to restoration fit, longevity, esthetics, and the perceived difficulty of the software and scanning.
Restoration Fit
One common misconception is that CAD/CAM restorations do not fit as well as conventionally fabricated restorations. First of all, the fit of conventional restorations must be established and defined as presented in the literature. Many studies have evaluated the marginal fit of non-CAD/CAM restorations, with gaps ranging from 0 μm to 313 μm and a mean marginal opening of 155 μm.1,2 In a landmark in vivo study, McLean and Fraunhofer examined more than 1,000 conventionally fabricated crowns after a 5-year period and concluded that a marginal opening of ≤120 μm is clinically acceptable for conventionally cemented restorations. Interestingly, this average is much greater than the once-suggested acceptable marginal gap of 25 μm to 40 μm.3,4 Other studies that agreed with McLean and Fraunhofer’s findings suggested acceptable clinical longevity with marginal gaps of 100 μm to 200 μm.3-9
Research shows that CAD/CAM systems produce in-office milled restorations that fit just as well as laboratory-fabricated restorations. For example:
• One study of ceramic onlay restorations compared CEREC Bluecam (Sirona Dental Systems, www.sironausa.com) restorations to laboratory-pressed restorations and found that the CEREC-produced restorations had better marginal fit,10 and it has been reported that the CEREC system yields reliable internal and marginal fit.11-14
• In another recently published study, Brawek et al compared the fit of restorations made from intraoral scans with both the CEREC AC Bluecam and Lava™ Chairside Oral Scanner COS (3M ESPE, http://solutions.3m.com) and concluded that the mean marginal gap of the Lava COS crowns was 51 μm (±38 μm) while the CEREC AC Bluecam crowns had a mean gap of 83 μm (±51 μm).15
• Yet another study evaluated 37 restorations fabricated using the Lava COS and found excellent marginal fit, with a mean marginal gap of 48.65 μm.16
• Four-unit fixed partial dentures (FPDs) fabricated using the Lava COS were found to have better fit than restorations fabricated in the same cases using conventional impression techniques.17 Clinicians evaluated more than 117 cases where two restorations were made, one by CAD/CAM and another by a laboratory, and were asked to choose which one they thought was better. Blind to which crown was made using digital technology and which crown was made using conventional techniques, the clinicians chose the digitally made crown 68% of the time.18
• In a recent publication, IPS e.max® restorations (Ivoclar Vivadent, www.ivoclarvivadent.us) fabricated using the PlanScan and PlanMill CAD/CAM system (Planmeca E4D Technologies, www.e4d.com) on preparations of varying quality were evaluated. It was found that the mean marginal gap of crowns fabricated on ideal preparations was 38.5 μm, those considered fair had a mean marginal gap of 58.3 μm, while those categorized as poor averaged 90.1 μm.19
• A separate study showed that E4D restorations had a mean marginal gap of 79.32 μm on the buccal and 50.39 μm on the lingual.20
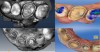
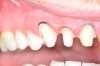
It is clear from the literature that digital dentistry is just as accurate, if not more, than conventional dentistry. Nevertheless, all systems are only capable of producing accurate margins if the margin is identifiable on the digital model. New systems produce models that have additional information that helps the clinician or laboratory technician easily and accurately identify the margin through the incorporation of color or high-definition photographs that are designed to detect enamel and dentin in black and white (Figure 1). Notice how clear the margins are, even in subgingival areas.
Longevity
Some practitioners are reluctant to adopt CAD/CAM technology based on a common misconception that chairside-milled restorations do not last in function. Millable ceramic technology has made remarkable advances in strength over the past few years. One distinct advantage of chairside CAD/CAM is having the ability to make restorations in a single visit from a solid, and essentially flawless, premanufactured block. The block is made in ideal conditions so, as a result, it has an ideal density with none of the residual porosity found in many layered or pressed porcelains. Porosities may act as a weak point and lead to the buildup of internal tensile stress in the ceramic, eventually causing a catastrophic failure.
Monolithic chairside-milled restorations have several distinct advantages over layered restorations when it comes to mechanical properties. Layered restorations are often veneered with weak feldspathic glasses that can chip or break, especially if they are not properly supported by the framework.21 Furthermore, there is no concern about delamination and microchipping of the veneering porcelain, which has been reported to be as high as 25% percent for porcelain-fused-to-zirconium restorations.21
One unique material, lithium disilicate (ie, IPS e.max) has changed how dentistry thinks about chairside millable materials because of its impressive strength. After the restoration is milled and tried in, it is crystalized and characterized in a short 15-minute oven cycle. During this cycle, the lithium metasilicate crystals are transformed into lithium disilicate crystals, and the flexural strength significantly increases from approximately 160 MPa to 360 MPa, according to the manufacturer.
IPS e.max was introduced to the dental market in 2006 and well-done clinical studies are now being published. Gehrt and colleagues followed 104 e.max crowns in 44 patients and found the corresponding survival rate for all restorations was 97.4% after 5 years and 94.8% after 8 years of clinical service, with location not significantly impacting survival rate.22 In a 10-year study, Kern et al found that 3-unit FPDs made from monolithic lithium disilicate showed 5- and 10-year survival and success rates that were similar to those of conventional metal–ceramic FPDs. They concluded that the calculated survival rate for the monolithic lithium-disilicate FPDs was 100% after 5 years and dropped to 90.8% (when considering only catastrophic ceramic fractures) and 87.9% (when considering catastrophic ceramic fractures and biological failures) after 10 years.23 Because of this flexural strength, some clinicians were concerned that IPS e.max may be aggressive on the opposing dentition, but in a clinical study, Silva et al found it to be more gentle on the opposing enamel than feldspathic ceramics, with a wear rate on enamel similar to natural dentition.24
Esthetics
Many clinicians are concerned that monolithic chairside-milled restorations are not esthetic enough for their patients, especially for anterior restorations. With poor design software and cumbersome tools, in the past it was difficult and time-consuming to achieve nice anterior restorations. Now, however, with recent advances in software it is simple and fast to do multiple units.
In the first case example, the patient presented with fractured teeth Nos. 8 and 9 from a car accident (Figure 2). Minimum tooth preparation was required and digital models were rapidly made using PlanScan (E4D Technologies) (Figure 3). The restorations were quickly designed using the software’s proposals and intuitive tools (Figure 4). Monolithic milled veneers were characterized (Figure 5) and delivered (Figure 6). It is worth noting that the service to the patient is remarkable, when they can come in and in a short appointment leave with an entirely brand-new smile, not temporaries.
When designing more than 4 units, it is more predictable to have a diagnostic wax-up on properly mounted models. The wax-up can be scanned into the software and used as a template for restoration design. Alternatively, if temporary restorations are placed, such as in larger cases where vertical dimension is altered, the clinician can scan the temporaries after they have been in function and use them as a guide for the fabrication of the final restorations. This makes large cases extremely predictable.
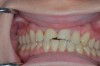
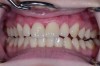
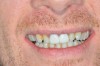
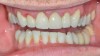
The patient in the next case example presented with existing laboratory-fabricated restorations on teeth Nos. 8 and 9, cervical decay, and large restorations on the other anterior teeth. His chief complaint was that he wanted a nice smile (Figure 7). The existing restorations were removed, and preparations were completed and retraction cord was placed (Figure 8). An intraoral digital impression was made, and the margins were marked using the ICE view (Figure 9). The restorations were designed based on the wax-up (Figure 10). The final milled restorations were delivered and the cord was removed (Figure 11 and Figure 12).
The restorations were made with IPS Empress® (Ivoclar Vivadent). With approximately 45% leucite crystals for dispersion strengthening, Empress is a unique feldspathic glass. According to the manufacturer, the 5-μm leucite crystals improve strength and fracture toughness by acting as “roadblocks” to prevent crack propagation. It is an esthetic material and is available in polychromatic blended shades that give the restoration a layered appearance. Empress Multiblock has a flexural strength around 160 MPa and requires isolation and attention to detail when bonding to ensure long-term success; self-adhesive resin cements should be avoided.
IPS Empress has been on the market for approximately 24 years, and as a result, good clinical research on the longevity of these restorations exists in the literature. A literature review conducted by Brochu and El-Mowafy evaluated and summarized six clinical studies that met their inclusion criteria. They concluded the survival rates for IPS Empress inlays and onlays ranged from 96% at 4.5 years to 91% at 7 years. IPS Empress crowns had a survival rate ranging from 92% to 99% at 3 to 3.5 years. For both crowns and onlays, most failures were a result of bulk fracture.25 In general, IPS Empress has higher failure rates in the posterior than the anterior and higher fracture rates on molars compared with premolars.26-29 Therefore, in the author’s opinion, IPS Empress is a solid material choice in the anterior for esthetically demanding patients.
The introduction of composite resin technology initiated a paradigm shift regarding material thickness and millability. Most ceramic material needs thickness for strength and to avoid chipping in the mill; however, a new generation of resin nanoceramics has been demonstrated to be successful for ultra-conservative preparations with minimum thickness, because of their less brittle nature.30-32 In one in vitro study, Lava™ Ultimate (3M ESPE) 0.3-mm-thick posterior occlusal veneers performed as well as those that were 1-mm thick, demonstrating the forgiving nature of the material.31 Furthermore, the material has a low modulus of elasticity and a less brittle nature that allows for it to be predictably milled 0.2 mm thick. In an experiment by Magne et al involving vertical cyclic loading of 1.2-mm thick CAD/CAM-fabricated occlusal veneers from two ceramic materials and a resin material, Paradigm™ MZ100 composite (3M ESPE), the composite performed drastically better with a 100% survival rate compared with 30% and 0% for the ceramic groups after loading up to 1,400 N.33 Lava Ultimate is the newest generation of resin material and has been shown to perform better than its predecessor Paradigm MZ100.32 In the author’s experience, Lava Ultimate nanoceramic is an excellent choice for no-preparation CAD/CAM veneer in the anterior.
Ease of Use
A number of revolutionary advances have been developed and implemented in this new generation of systems that make the user experience a lot less stressful than it was in the past. Both the CEREC Omnicam and the PlanScan systems allow for video-speed, powder-free imaging. Not only is powder expensive, it also can be difficult to avoid having it clump or become contamined when scanning. Time-saver features allow for a team approach to scanning, where the opposing bite and working quadrants are scanned by the dental assistant while the anesthetic is taking effect, then the tooth that is being prepared is erased from the model. After preparation and isolation, the clinician only has to scan the prepared tooth and the software will automatically stitch the preparation into the prescanned quadrant, eliminating the need for the clinician to capture the entire quadrant or arch. Furthermore, the design software has been transformed from cumbersome to intuitive; no longer are there dots and contour lines on the screen to manipulate. Instead, the clinician simply grabs a cusp and pushes it to the desired location. Rapid manipulation of proposals combined with the option to copy exactly a wax-up or preexisting tooth allows for predictable design in not only simple cases but also larger cases, including up to full-mouth reconstruction. Even in full-mouth reconstruction cases, nothing really changes. Models are made in centric relation and the case is waxed. The patient is temporized and the occlusion, esthetics, and phonetics are verified for 4-6 weeks, and the case is then fabricated a quadrant or sextant at a time. At this point all the clinician has to do is scan an arch of the temporaries, then remove only a quadrant of the temporaries, isolate the preparations, and scan them. The software will copy exactly the occlusion of the temporaries. After milling the quadrant and delivering the final restorations, they usually require no adjustment, as they are an exact replica of the temporaries that have been in function and already approved by the clinician and the patient.
Conclusion
It is clear that the combination of strong and beautiful materials with sophisticated scanning and design software has fueled a new age of chairside digital dentistry. Single-visit, high-quality restorations that look, fit, and function indistinguishably from laboratory restorations are now possible without difficulty. The invaluable service of single-visit dentistry is no longer a compromise in quality; rather it is setting a new standard. Dentistry has never been more exciting than now.
References
1. Adair PJ, Grossmann DG. The castable ceramic crown. Int J Periodontics Restorative Dent. 1984;4:32-46.
2. Pera P, Gilodi S, Bassi F, et al. In vitro marginal adaptation of alumina porcelain ceramic crowns. J Prosthet Dent. 1994;72:585-590.
3. McLean JW, von Fraunhofer JA. The estimation of cement film thickness by an in vivo technique. Br Dent J. 1971;131:107-111.
4. American Dental Association. ANSI/ADA Specification No. 8 for zinc phosphate cement, February 1968. In: Guide to Dental Materials and Devices (ed 5). Chicago, IL: American Dental Association; 1970-1971:87-88.
5. Fransson B, Øilo G, Gjeitanger R. The fit of metal-ceramic crowns, a clinical study. Dent Mater. 1985;1:197-199.
6. Karlsson S. The fit of Procera titanium crowns. An in vitro and clinical study. Acta Odontol Scand. 1993;51:129-134.
7. In-Sung Y, Jae-Ho Y, Jai-Bong L. In vitro marginal fit of three all-ceramic crown systems. J Prosthet Dent. 2003;90:459-464.
8. Boening K, Reppel PD, Walter M. Non-cast titanium restorations in fixed prosthodontics. J Oral Rehabil. 1992;19:281-287.
9. Björn AL, Björn H, Grcovic B. Marginal fit of restorations and its relation to periodontal bone level. II. Crowns. Odontol Revy. 1970;21:337-346.
10. Keshvad A, Hooshmand T, Asefzadeh F, et al. Marginal gap, internal fit, and fracture load of leucite-reinforced ceramic inlays fabricated by CEREC inLab and hot-pressed techniques. J Prosthodont. 2011;20:535-540.
11. Nakamura T, Dei N, Kojima T, Wakabayashi K. Marginal and internal fit of Cerec 3 CAD/CAM all-ceramic crowns. Int J Prosthodont. 2003;16:244-248.
12. Bindl A, Mormann WH. Marginal and internal fit of all-ceramic CAD/CAM crown-copings on chamfer preparations. J Oral Rehabil. 2005;32:441-447.
13. Quintas AF, Oliveira F, Bottino MA. Vertical marginal discrepancy of ceramic copings with different ceramic materials, finish lines, and luting agents: an in vitro evaluation. J Prosthet Dent. 2004;92:250-257.
14. Kyu-Bok L, Charn-Woon P, Kyo-Han K, Tae-Yub K. Marginal and Internal Fit of All-ceramic crowns fabricated with two different CAD/CAM systems. Dent Mater J. 2008;27:422-426.
15. Brawek PK, Wolfart S, Endres L, et al. The clinical accuracy of single crowns exclusively fabricated by digital workflow—the comparison of two systems. Clin Oral Investig. 2013;17:2119-2125.
16. Scotti R, Cardelli P, Baldissara P, Monaco C. Clinical fitting of CAD/CAM zirconia single crowns generated from digital intraoral impressions based on active wavefront sampling. J Dent. 2011 Oct 17. [Epub ahead of print]
17.Almeida E Silva JS, Erdelt K, Edelhoff D, et al. Marginal and internal fit of four-unit zirconia fixed dental prostheses based on digital and conventional impression techniques. Clin Oral Investig. 2014;18:515-523.
18. Henkel GL. A comparison of fixed prostheses generated from conventional vs digitally scanned dental impressions. Compend Contin Educ Dent. 2007;28(8):422-431.
19. Renne W, McGill ST, Forshee KV, et al. Predicting marginal fit of CAD/CAM crowns based on the presence or absence of common preparation errors. J Prosthet Dent. 2012;108:310-315.
20. Plourde J, Harsono M, Fox L, et al. Marginal and internal fit of E4D CAD/CAM all-ceramic crowns. J Dent Res. 2011;90(Spec Iss A):Abstract #638.
21. Sailer I, Gottnerb J, Kanelb S, Hammerle CH. Randomized controlled clinical trial of zirconia-ceramic and metal-ceramic posterior fixed dental prostheses: a 3-year follow-up. Int J Prosthodont. 2009;22(6):553-560.
22. Maren Gehrt, Stefan Wolfart, Nicole Rafai, et al. Clinical results of lithium-disilicate crowns after up to 9 years of service. Clin Oral Investig. 2013;17:275-284.
23. Kern M, Sasse M, Wolfart S. Ten-year outcome of three-unit fixed dental prostheses made from monolithic lithium disilicate ceramic. J Am Dent Assoc. 2012;143(3):234-240.
24 Esquivel-Upshaw J. Comparative reliability analyses of zirconium oxide and lithium disilicate restorations in vitro and in vivo. J Am Dent Assoc. 2011;142(Suppl 2):4S-9S.
25. Jean-François Brochu, Omar El-Mowafy. Longevity and clinical performance of IPS-Empress ceramic restorations—a literature review. J Can Dent Assoc. 2002;68(4):233-237.
26. Pjetursson BE, Sailer I, Zwahlen M, Hammerle CH. A systematic review of the survival and complication rates of all-ceramic and metal-ceramic reconstructions after an observation period of at least 3 years. Part I: single crowns. Clin Oral Implants Res. 2007;18(Suppl 3):73-85.
27. Della Bona A, Kelly JR. The clinical success of all-ceramic restorations. J Am Dent Assoc. 2008;139(Suppl):8S-13S.
28. Kassem AS, Atta O, El-Mowafy O. Survival rates of porcelain molar crowns—an update. Int J Prosthodont. 2010;23:60-62.
29. Heintze SD, Rousson V. Fracture rates of IPS Empress all-ceramic crowns—a systematic review. Int J Prosthodont. 2010;23:129-133.
30. Pallis K, Griggs JA, Woody RD, et al. Fracture resistance of three all-ceramic restorative systems for posterior applications. J Prosthet Dent. 2004;91:561-569.
31. Skouridou N, Pollington S, Rosentritt M, Tsitrou E. Fracture strength of minimally prepared all-ceramic CEREC crowns after simulating 5 years of service. Dent Mater. 2013;29:e70-e77.
32. Johnson AC, Versluis A, Tantbirojn D, Ahuja S. Fracture strength of CAD/CAM composite and composite-ceramic occlusal veneers. J Prosthodont Res. 2014;58:107-114.
33. Magne P, Schlichting LH, Maia HP, Baratieri LN. In vitro fatigue resistance of CAD/CAM composite resin and ceramic posterior occlusal veneers. J Prosthet Dent. 2010;104:149-157.