You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Because of high rates of obesity, and the resultant 5 fold increase in bariatric surgery, it is likely the number of dental patients presenting with a history of bariatric surgery is also rising.1–4 Heling et al found that 34% of patients reported an increase in frequency of dental visits following bariatric surgery, which further increases the likelihood more of these patients will be seen in the dental office.5 This case report is representative of people undergoing bariatric surgery to reduce morbid obesity and manage chronic medical conditions.1 Both before and after surgery, there are implications for dental care requiring careful follow–up. This report provides dental professionals with an overview of dental considerations to enhance their ability to provide bariatric patients with high quality preventive care and non–surgical periodontal therapy (NSPT), as prescribed.
Review of the Literature
Bariatric surgery is not cosmetic surgery. Rather, it is medically necessary for many morbidly obese people to aid in loss of large amounts of weight to assist with risk reduction and management of chronic diseases that increase the risk of morbidity and mortality.6 The implications of bariatric surgery, cardiovascular disease and diabetes for dental care will be briefly reviewed before sharing the details pertaining to the patient in this case report.
Obesity
In the past 25 years, obesity in adults has doubled. The 2005 to 2006 National Health and Nutrition Examination Survey estimated that 34% of adults in the United States are obese as defined by a Body Mass Index (BMI) greater than 30 kg/m2, and 32.7% are overweight (BMI of 25 to 29.9 kg/ m2), with 1.6 billion adults being affected worldwide.2–4 Seventy–two million Americans and 400 million adults worldwide are obese (BMI>30 kg/ m2).3 Obesity is a systemic disease substantially raising the risk for co–morbidities and complications affecting overall health from chronic diseases such as hypertension, type 2 diabetes, coronary heart disease and stroke.7,8 In addition to the link between obesity and chronic diseases, epidemiologic studies suggest an association between obesity and periodontal disease.9–16 The link between periodontal disease and obesity, along with other chronic disease, such as cardiovascular disease, is proposed to be the biologic mediators of the inflammatory process.12,17–20
A meta–analysis supports bariatric surgery as an effective means of long term weight loss, therefore increasing the number of patients who undergo procedures such as gastric bypass and gastric lap band surgery.6 As more patients present in the dental office with a history of bariatric surgery, it becomes crucial that dental professionals be familiar with these types of surgery and the potential impact on dental care.
Bariatric Surgery
The impact of bariatric surgery on weight loss and chronic disease in a recent meta–analysis found diabetes resolved in 60% of cases, hyperlipidemia (high cholesterol and/or triglycerides) improved in 70% of patients and 43% had resolution of hypertension.6 In the meta–analysis, resolution refers to the disappearance of the co–morbid condition or the condition no longer required therapy.1 In addition to improvements in chronic disease, weight loss was significant and sustainable long term.21,22
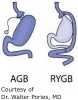
The 2 categories of bariatric surgery include malabsorptive and restrictive. The most common bariatric surgeries are adjustable gastric bands (AGB) and Roux–en–Y gastric bypass (RYGP, Figure 1).23 In malabsorptive–type surgeries such as RYGP, portions of the stomach and small intestine are bypassed, which leads to restriction of food intake along with reduction in the absorption capacity of the intestine. In restrictive–type surgeries, such as AGB, the mechanism of action is primarily a restriction in the amount of food consumed using a bracelet–like band that is placed around the upper part of the stomach and can be adjusted by adding or decreasing the amount of saline solution in the band or balloon.24
Following bariatric surgery, the stomach holds approximately 1 to 2 ounces, which requires the patient to eat frequent, small meals with the intake of fluids spread throughout the day. This frequency of meals puts the patient at increased risk for dental caries. However, the level of risk is dependent upon types of foods selected and other caries risk factors.25 Bariatric surgery patients are encouraged to choose nutrient–dense foods, which reduces cariogenicity of the diet and minimize intake of empty calories, such as high fat and high–sugar type foods.26 Another reason for increased caries risk and tooth erosion is the high prevalence of gastroesophageal reflux (GER) in the morbidly obese (73%) that is not entirely resolved following bariatric surgery.27 GER may improve after RYGP, but it may worsen after AGB, with one–third of patients developing severe reflux.27 In addition to issues with GER, bariatric surgery patients may also experience frequent vomiting.5
Another common problem experienced after bariatric surgery are nutritional deficiencies which have the potential to impact healing following dental treatment. Malnutrition and micronutrient deficiencies tend to be more common after malabsorptive surgical procedures because of loss of intestinal surface for nutrient absorption, but it can occur in restrictive procedures as well.24 A review of nutrition complications following malabsorptive–type bariatric surgery found the following incidence of nutrition issues: protein inadequacy (13 to 18%), vitamin A deficiency (12 to 69%), vitamin B12 deficiency (33%), iron deficiency (13 to 47%) and zinc deficiency (36 to 50%).24,28 One concern for oral health professionals is the risk for calcium and vitamin D metabolic defects leading to issues with bone density following RYGP. Other studies found vitamin D depletion rose significantly beyond existing deficiencies from 57% to 63% in a 4 year span.24 Research is needed to evaluate the long term impact on periodontal health. In restrictive–type surgery, nutrient deficiencies are less common because patients retain function of the entire gastrointestinal tract.28 Therefore, the primary reason for deficiency in restrictive–type surgery is poor food selection.
An additional concern for patients who undergo bariatric surgery is the risk of gastric cancer. According to an article by Collins et al, historical cohorts demonstrate an increased incidence of gastric cancer in patients with gastric and duodenal ulcers after bariatric surgery.29 This is due to inflammation, ulceration and hyperproliferative changes to the squamous epithelium of the esophagus caused by chronic reflux post surgery.29 However, incidence is thought to be less in patients with the RYGP due to the anatomical differences between this surgical procedure and other gastric operations, such as distal gastrectomy.30 Although the risk of developing gastric or esophageal cancer is a concern, overall bariatric surgery has shown an inverse association (reduction) for cancer incidence and mortality for all cancers.31,32
Diabetes
Diabetes is a chronic disease in which the body does not produce or properly use insulin, and type 2 (the most common form) specifically results from insulin resistance. Diabetes requires significant self care by the patient to maintain glycemic control and reduce the incidence of complications.33 Research about the relationship between poorly controlled diabetes and severity of periodontal disease and tooth loss suggests a correlation.18,34–36 Since poorly controlled diabetes increases the risk for more severe periodontitis, periodontal therapy must be part of the comprehensive care of the patient with diabetes.18,35
Despite the connection between uncontrolled diabetes and severity of periodontal disease, inconsistent research findings make it less clear that controlling periodontal disease improves metabolic control of a patient’s diabetes.34,37–43 Regardless of inconsistent research findings, medical and dental practitioners need to encourage patients to manage their periodontal health since it may be one of the factors involved in glycemic control.36 In addition, dental professionals need to be concerned with the patient’s glycemic control prior to beginning dental treatment to maximize healing and to prevent medical emergencies, such as hypoglycemia, in the dental chair (Table I). Ultimately, by taking a few precautionary steps and looking at the overall health of the patient, as well as periodontal health, dental professionals can aid in playing an essential role in the treatment of patients with diabetes.35
Cardiovascular Disease
Although bariatric surgery resolves conditions associated with cardiovascular disease, including hypertension and dyslipidemia (in 43 and 70% of patients respectively), the disease may still be a condition that has to be managed. In order to safely treat patients with a history of cardiovascular disease, the clinician needs to minimize hemodynamic changes.6 If a patient has a history of ischemic heart disease, cardiac arrhythmias, cerebrovascular accident or anti–coagulant therapy, the following approaches to minimizing hemodynamic alterations should be implemented: shorter appointments in the morning so the patient is more rested and able to withstand stress, profound local anesthesia for pain control, possible conscious sedation and adequate pain control post–operatively.44
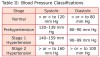
Hypertension blood pressure is a parameter that should be routinely monitored to identify those patients at risk for hypertension and/or medical emergency during dental care. Hypertension affects 1 in 3 people in the United States.45 Stage 1 hypertension is defined as a common, often asymptomatic disorder characterized by elevated blood pressure persistently exceeding 140/90 mmHg.45 The National Institutes of Health’s joint commission defined 4 levels of classification for blood pressure in adults (Table II).
Epidemiologic evidence suggests an association between hypertension and periodontal disease in a dose–dependent fashion, meaning that higher blood pressure is associated with more severe periodontitis.46 A dental consideration for hypertensive patients is use of local anesthetic containing a vasoconstrictor, such as epinephrine, since there is a small risk of adverse events.47,48 “Safe and effective periodontal management of such patients requires close medical and dental coordination, an understanding of the potential hazards during dental treatment, knowledge of drugs used in treatment of cardiovascular diseases, and the potential adverse effects of drugs commonly used in periodontal practice.”49 It is important for members of the dental team to have a thorough understanding of cardiovascular disease along with its potential effects on the periodontium in delivery of periodontal therapy.20
Anti–coagulant Therapy
Another medical consideration that must be addressed prior to dental care is patients taking anticoagulants, as this poses a risk for hemorrhage from invasive dental procedures, such as periodontal therapy.20 A medical consultation should precede any invasive dental treatment to determine the patient’s most recent Prothrombin–time (Pro–time), international normalized ratio (INR) and potential need to adjust dosage of anticoagulant.20 This is especially critical if the patient requires dental procedures where bleeding is anticipated, such periodontal surgery, NSPT or extractions.49 A thorough medical history and consultation with the medical provider prior to starting treatment eliminates a potentially life–threatening medical emergency caused by anticoagulant therapy (Table I).
The literature is clear concerning patients with multiple medical conditions – they require careful consideration. Many of these conditions could have dental implications or affect the course of non–surgical periodontal therapy based upon whether or not the conditions are stabilized and controlled. In order to ensure safety of the patient, clinicians must take steps to gather additional information regarding the patient’s current status from the medical practitioner prior to beginning dental treatment. “The ideal management of such individuals should involve the collaborative efforts of health care providers, nurses, dentists and dental hygienists, thus optimizing treatment and minimizing secondary complications derived from the oral cavity.”50
Patient Assessment
N.P., a 54 year old Hispanic male, presented to the dental clinic with a chief complaint of “needing to have his teeth cleaned.” The patient moved to the United States from Mexico 22 years ago, and has had very limited dental treatment. He was 5’7” and weighed 418 pounds with a BMI of 65.5. Initial vital signs included a blood pressure reading of 116/60 and respirations at 20 breaths per minute. N.P. reported a history of hypertension, hyperlipidemia, pulmonary embolism, bariatric surgery (lap band), Type 2 diabetes mellitus and osteoarthritis. The patient lost 60 pounds following bariatric surgery (gastric lap band) in 2002.
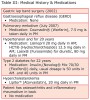
The medical provider was consulted prior to dental treatment due to the medically compromised condition of the patient (Table III). Effective communication between the dental and medical professionals was necessary to ensure that the patient’s needs were met and to monitor Pro–time, INR and hemoglobin A1c (HbA1C) levels during treatment. Table I provides an overview of issues addressed with the medical provider as well as their implications of the information for dental care.
N.P.’s health care provider indicated his most recent HbA1c was 8.2%, which equates to an average blood glucose over 182 mg/dl.27 The goal for HbA1c in non–pregnant adults is less than 7% to prevent microvascular complications.27 Re–evaluation of his HbA1c was scheduled for his next medical visit. In consultation with the medical provider, it was determined N.P. should stop taking Coumadin® 2 days prior to each NSPT appointment.
Results
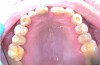
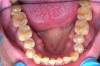
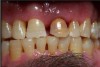
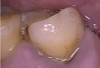
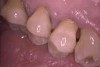
N.P.’s occlusal surfaces exhibited generalized extreme wear and/or erosion, and he complained of dentin hypersensitivity (Figure 2 and Figure 3). A caries risk assessment and diet recall was performed to assess the patient’s diet to determine its impact on the dentin hypersensitivity and caries risk. During the dietary assessment, N.P. reported severe GER problems limited his food selection.
Periodontal assessment revealed (Figure 4 through Figure 9):
- eneralized 4 to 6 mm probing depths on posterior teeth
- Furcation involvement, which included Grade I buccal of the maxillary left first and second molar and ML and Grade II buccal of the maxillary left third molar
- Tooth mobility – Class I maxillary left central incisor
- Bleeding Index: 39.8%
- Plaque Index: 100%
Preventive and Periodontal Treatment
Based on generalized moderate chronic periodontitis as evidenced by clinical attachment loss, radiographic bone loss, furcation involvement, tooth mobility, heavy calculus deposits and bleeding on probing, full mouth NSPT was prescribed along with oral hygiene instruction. Other preventive services to address dentin hypersensitivity and caries risk included fluoride therapy and nutrition counseling.
It is hypothesized that N.P.’s severe GER contributed to generalized occlusal erosion, dentin hypersensitivity and dental caries based on the high incidence of GER in obesity and post–gastric lap band surgery.23,25,45 In addition, his dietary recall demonstrated GER impacted his ability to consume an adequate nutrient–dense diet. This had the potential to impact his immune response and ability to heal. His poor dietary intake was also a significant concern in regard to managing his diabetes.
The patient reported for 4 appointments for quadrant NSPT with local anesthesia over a 5 week period. Ultrasonic and hand instrumentation was utilized for debridement and disruption of plaque biofilm and calculus removal. Fluoride varnish was applied to assist with desensitization and caries prevention.
Periodontal re–evaluation was completed 6 weeks following completion of NSPT. Patient’s bleeding and plaque index improved from 39% and 100%, respectively, at baseline to 4.6% and 40%. Oral self–care was reviewed and reinforced. Periodontal data collection revealed pocket depths improved with all posterior areas measuring 4 mm or less. Monitoring and periodontal maintenance were planned at 3 month intervals. In addition to improvement in periodontal health, N.P.’s patient medical provider reported his HbA1c decreased to 7.7%, an improvement of 0.5% in the 4 months from baseline to re–evaluation. There are many factors that could have contributed to this positive shift in HbA1c levels. However, this is consistent with reductions in HbA1c in research reports following NSPT.33
Discussion
This case was representative of issues dental providers face when providing care for bariatric surgery patients. Students, dentists and dental hygienists often learn about medical conditions in isolation, so cases like this present an opportunity to learn how to manage more complex patients seen routinely in dental offices. The role of the dental professional is increasingly challenging as the population grows more medically complex. In this particular case, significant investigation, consultation and education with the medical provider were required in regard to bariatric surgery and the chronic diseases this patient exhibited prior to providing dental treatment. The medical providers for this case were unaware of the need for the dental professional to be informed about neither glycemic control nor the potential impact that periodontal inflammation might have on diabetes control. Persistence by the dental practitioner was required to gain the necessary information prior to beginning treatment. This case presented the opportunity for educating the medical provider about the oral–systemic link. Even though communication between the dental professional and medical professional is essential to determine the best course of treatment for the medically compromised patient, many medical professionals may have limited knowledge about the oral–systemic connection.
Equally important is the feedback dental professionals can provide to the medical practitioner to help further regulate medical conditions and diseases. This case required follow–up bariatric surgery and surgical replacement of the gastric lap–band with new one, due to the poor weight loss and severe GER. Medical providers were unaware of the impact of uncontrolled GER on oral health and potential for increased risk for esophageal cancer.
Conclusion
The medically compromised dental patient requires extra precaution to ensure the patient’s well–being and safety while providing dental hygiene care. Bariatric surgery patients seen in the dental office are at risk for a number of oral health related issues requiring management. The interprofessional health care team must work together to develop a comprehensive care plan to address all the patient’s short and long–term medical and dental needs. The collaboration between the dental professional and medical professional is a vital component to determining the best course of treatment for the medically compromised patient. By working together, a comprehensive care plan can be created with all the patient’s needs taken into consideration and met by the recommended dental treatment.
Recommendations
Dental professionals need to become more aware of the dental implications that bariatric surgery patients may present with at the dental office. Careful review of the patient’s medical, medication, dental and psychosocial history is essential to determine the extent of consultations needed with other health care providers to ensure safe and effective prevention and management of oral disease. Because the literature suggests chronic diseases such as hypertension and diabetes mellitus may improve or resolve following bariatric surgery, close collaboration with medical providers will be necessary in order to monitor the patient’s status in regard to blood glucose, INR and blood pressure.
The areas of particular interest for the bariatric patient include an understanding of the side effects the patient may be experiencing, such as vomiting, GER and possible challenges obtaining adequate nutrient intakes. These issues may impact oral health in a number of ways by increasing the risk of dental caries, tooth erosion, esophageal cancer and poor healing following NSPT, surgery or extractions as result of nutrient deficiencies. These conditions present opportunities to collaborate with other health care providers to ensure the patients overall well–being.
References
1. Smoot TM, Xu P, Hilsenrath 1. P, Kuppersmith NC, Singh KP. Gastric bypass surgery in the United States, 1998–2002. Am J Public Health. 2006;96(7):1187–1189.
2. National Center for Health Statistics. Prevalence of overweight, obesity and extreme obesity among adults: United States, trends 1976–80 through 2005–2006. NCHS [Internet]. 2008 [cited 2010 January 12]. Available from: http://www.cdc.gov/nchs/data/hestat/overweight/overweight_adult.pdf.
3. Ogden CL, Carroll MD, McDowell MA, Flegal KM. Obesity among adults in the United States – no change since 2003–2004. NCHS [Internet]. 2007 [cited 2010 March 17]. Available from: http://www.cdc.gov/nchs/data/databriefs/db01.pdf.
4. World Health Organization. Obesity and overweight. WHO [Internet]. 2006 September [cited 2010 January 12]. Available from: http://www.who.int/mediacentre/factsheets/fs311/en/.
5. Heling I, Sgan–Cohen HD, Itzhaki M, Beglaibter N, Avrutis O, Gimmon Z. Dental complications following gastric restrictive bariatric surgery. Obes Surg. 2006;16(9):1131–1134.
6. Cunneen SA. Review of meta–analytic comparisons of bariatric surgery with a focus on laparoscopic adjustable gastric banding. Surg Obes Relat Dis. 2008;4(3 Suppl):S47–55.
7. National Heart, Lung, and Blood Institute, National Institute of Diabetes and Digestive and Kidney Diseases. The Practical Guide: Identification, Evaluation, and Treatment of Overweight and Obesity in Adults: The Evidence Report. U.S. Department of Health & Human Services [Internet]. 1998 September [cited 2010 January 12]. Available from: http://www.nhlbi.nih.gov/guidelines/obesity/ob_gdlns.htm.
8. Pischon T, Nöthlings U, Boeing H. Obesity and cancer. Proc Nutr Soc. 2008;67(2):128–145.
9. Al–Zahrani MS, Bissada NF, Borawskit EA. Obesity and periodontal disease in young, middle–aged, and older adults. J Periodontol. 2003;74(5):610–615.
10. Alabdulkarim M, Bissada N, Al–Zahrani M, Ficara A, Siegel B. Alveolar bone loss in obese subjects. J Int Acad Periodontol. 2005;7(2):34–38.
11. Chapper A, Munch A, Schermann C, Piacentini CC, Fasolo MT. Obesity and periodontal disease in diabetic pregnant women. Braz Oral Res. 2005;19(2):83–87.
12. Pischon N, Heng N, Bernimoulin JP, Kleber BM, Willich SN, Pischon T. Obesity, inflammation, and periodontal disease. J Dent Res. 2007;86(5):400–409.
13. Rech RL, Nurkin N, da Cruz I, et al. Association between periodontal disease and acute coronary syndrome. Arq Bras Cardiol. 2007;88(2):185–190.
14. Saito T, Shimazaki Y, Kiyohara Y, et al. Relationship between obesity, glucose tolerance, and periodontal disease in Japanese women: the Hisayama study. J Periodontal Res. 2005;40(4):346–353.
15. Sarlati F, Akhondi N, Ettehad T, Neyestani T, Kamali Z. Relationship between obesity and periodontal status in a sample of young Iranian adults. Int Dent J. 2008;58(1):36–40.
16. Wood N, Johnson RB, Streckfus CF. Comparison of body composition and periodontal disease using nutritional assessment techniques: Third National Health and Nutrition Examination Survey (NHANES III). J Clin Periodontol. 2003;30(4):321–327.
17. Boesing F, Patiño JS, da Silva VR, Moreira EA. The interface between obesity and periodontitis with emphasis on oxidative stress and inflammatory response. Obes Rev. 2009;10(3):290–297.
18. Mealey BL, Oates TW, American Academy of Periodontology. Diabetes mellitus and periodontal diseases. J Periodontol. 2006;77(8):1289–1303.
19. Nishimura F, Murayama Y. Periodontal inflammation and insulin resistance––lessons from obesity. J Dent Res. 2001;80(8):1690–1694.
20. Seymour RA, Preshaw PM, Thomason JM, Ellis JS, Steele JG. Cardiovascular diseases and periodontology. J Clin Periodontol. 2003;30(4):279–292.
21. Anwar M, Collins J, Kow L, Toouli J. Long–term efficacy of a low–pressure adjustable gastric band in the treatment of morbid obesity. Ann Surg. 2008;247(5):771–778.
22. Garb J, Welch G, Zagarins S, 22. Kuhn J, Romanelli J. Bariatric surgery for the treatment of morbid obesity: a meta–analysis of weight loss outcomes for laparoscopic adjustable gastric banding and laparoscopic gastric bypass. Obes Surg. 2009;19(10):1447–1455.
23. Meneghini LF. Impact of bariatric surgery on type 2 diabetes. Cell Biochem Biophys. 2007;48(2–3):97–102.
24. Davies DJ, Baxter JM, Baxter JN. Nutritional deficiencies after bariatric surgery. Obes Surg. 2007;17(9):1150–1158.
25. Hague AL, Baechle M. Advanced caries in a patient with a history of bariatric surgery. J Dent Hyg. 2008;82(2):22.
26. University of Wisconsin Health Bariatric Surgery Program. Nutrition After Bariatric Surgery. University of Wisconsin [Internet]. 2008 April 20 [cited 2010 January 12]. Available from: http://www.uwhealth.org/files/uwhealth/docs/pdf/bariatric_surgery_nutrition.pdf.
27. Merrouche M, Sabaté JM, Jouet P, et al. Gastroesophageal reflux and esophageal motility disorders in morbidly obese patients before and after bariatric surgery. Obes Surg. 2007;17(7):894–900.
28. Miller AD, Smith KM. Medication and nutrient administration considerations after bariatric surgery. Am J Health Syst Pharm. 2006;63(19):1852–1857.
29. Collins BJ, Miyashita T, Schweitzer M, Magnuson T, Harmon JW. Gastric bypass: why Roux–en–Y? A review of experimental data. Arch Surg. 2007;142(10):1000–1003.
30. Inoue H, Rubino F, Shimada Y, et al. Risk of gastric cancer after Roux–en–Y gastric bypass. Arch Surg. 2007;142(10):947–953.
31. Adams TD, Stroup AM, Gress RE, et al. Cancer incidence and mortality after gastric bypass surgery. Obesity (Silver Spring). 2009;17(4):796–802.
32. Adams TD, Hunt SC. Cancer and obesity: Effect of bariatric surgery. World J Surg. 2009;33(10):2028–2033.
33. American Diabetes Association. Standards of medical care in diabetes––2010. Diabetes Care. 2010;33 (Suppl 1):S11–61.
34. Taylor GW. The effects of periodontal treatment on diabetes. J Am Dent Assoc. 2003;134 Spec No:41S–48S.
35. Vernillo AT. Dental considerations for the treatment of patients with diabetes mellitus. J Am Dent Assoc. 2003;134 Spec No:24S–33S.
36. Herring ME, Shah SK. Periodontal disease and control of diabetes mellitus. J Am Osteopath Assoc. 2006;106(7):416–421.
37. Faria–Almeida R, Navarro A, Bascones A. Clinical and metabolic changes after conventional treatment of type 2 diabetic patients with chronic periodontitis. J Periodontol. 2006;77(4):591–598.
38. Grossi SG, Skrepcinski FB, DeCaro T, et al. Treatment of periodontal disease in diabetics reduces glycated hemoglobin. J Periodontol. 1997;68(8):713–719.
39. Janket SJ, Wightman A, Baird AE, Van Dyke TE, Jones JA. Does periodontal treatment improve glycemic control in diabetic patients? A meta–analysis of intervention studies. J Dent Res. 2005;84(12):1154–1159.
40. Jones JA, Miller DR, Wehler CJ, et al. Does periodontal care improve glycemic control? The Department of Veterans Affairs Dental Diabetes Study. J Clin Periodontol. 2007;34(1):46–52.
41. Kiran M, Arpak N, Unsal E, Erdoğan MF. The effect of improved periodontal health on metabolic control in type 2 diabetes mellitus. J Clin Periodontol. 2005;32(3):266–272.
42. Navarro–Sanchez AB, Faria–Almeida R, Bascones–Martinez A. Effect of non–surgical periodontal therapy on clinical and immunological response and glycaemic control in type 2 diabetic patients with moderate periodontitis. J Clin Periodontol. 2007;34(10):835–843.
43. Promsudthi A, Pimapansri S, Deerochanawong C, Kanchanavasita W. The effect of periodontal therapy on uncontrolled type 2 diabetes mellitus in older subjects. Oral Dis. 2005;11(5):293–298.
44. Rose LF, Mealey B, Minsk L, Cohen DW. Oral care for patients with cardiovascular disease and stroke. J Am Dent Assoc. 2002;133 Suppl:37S–44S.
45. National Heart, Lung and Blood 45. Institute. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure – Complete Report. U.S. Department of Health and Human Services [Internet]. 2004 August [cited 2010 January 12]. Available from: http://www.nhlbi.nih.gov/guidelines/hypertension/.
46. Holmlund A, Holm G, Lind L. Severity of periodontal disease and number of remaining teeth are related to the prevalence of myocardial infarction and hypertension in a study based on 4,254 subjects. J Periodontol. 2006;77(7):1173–1178.
47. Herman WW, Konzelman JL Jr, Prisant LM; Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. New national guidelines on hypertension: a summary for dentistry. J Am Dent Assoc. 2004;135(5):576–584.
48. Neves RS, Neves IL, Giorgi DM, et al. Effects of epinephrine in local dental anesthesia in patients with coronary artery disease. Arq Bras Cardiol. 2007;88(5):545–551.
49. Research, Science and Therapy Committee, American Academy of Periodontology. Periodontal management of patients with cardiovascular diseases. J Periodontol. 2002;73(8):954–968.
50. Migliorati CA, Madrid C. The interface between oral and systemic health: the need for more collaboration. Clin Microbiol Infect. 2007;13 Suppl 4:11–16.
About the Author
Lisa J. Moravec, RDH, MSDH Assistant Professor and West Division Site Coordinator University of Nebraska Medical Center College of Dentistry Dental Hygiene Program Gering, Nebraska
Linda D. Boyd, RDH, RD, EdD Dean and Professor Forsyth School of Dental Hygiene Massachusetts College of Pharmacy and Health Sciences Boston, Massachusetts