You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Many studies have been conducted to determine the ideal technique when using adhesive dentistry in the permanent adult dentition. Multiple in vitro and some in vivo investigations have been and are still being conducted to enumerate this technique. Among the topics currently being investigated is a definitive stepwise technique with both total-etch and selective-etch, as well as one-step techniques utilized by practitioners performing adhesive direct restorations.1-3
Dentin Versus Enamel
Understanding the factors that drive the ultimate success of dentin adhesion prompts a review of the histology, steps, and terminology of these procedures. The histological compositions of enamel and dentin, although similar in some ways to bone, have several unique characteristics. Enamel is both acellular and avascular. Developmentally, ameloblasts form a matrix of enamel in columns, which are referred to as enamel rods. Subsequent to the formation of enamel, its final composition is observed to be 95% mineralized tissue (mineral extracellular matrix calcium hydroxyapatite) and 4% protein extracellular matrix composed of amelogenins and enamelin, along with water (1%).4
As noted by Fuentes et al, a consensus exists regarding enamel adhesion.5 It has been well established that phosphoric acid-etching of enamel produces the most successful clinical outcomes.6-8 Fuentes et al noted that a phosphoric etch-and-rinse technique facilitates micromechanical interlocking of the adhesive and enhances the chemical bonding potential of the functional acid monomer, which in the case of their study was MDP (10-methacryloyloxydecyl dihydrogen phosphate). Han and colleagues further demonstrated the advantages of phosphoric etchant on enamel, as their study enumerated that the chemical bonding potential starts with a formation of MDP-calcium (MDP-Ca) salts and an increase in the negative charge of the enamel surface.9-11 They showed that an increase in MDP-Ca formation resulted in two significant advantages. First, this salt formation improved MDP-hydroxyapatite chemical affinity, and secondly, it significantly increased surface wettability, which allows for an improved etch pattern and penetration of the adhesive.12 Finally, it was shown via scanning electron microscope data that not only did phosphoric acid-etching form a honeycomb structure on the enamel surface upon etching, but also a corresponding increase in the contact area between the enamel prisms and bonding resin (and the resultant benefit of increased wettability of the enamel by the resin).9 Given the research and clinical consensus that enamel etching with phosphoric acid produces the highest bond strengths, this step in adhesive dentistry should be considered a requisite.
From a histological perspective, dentin differs significantly from enamel. While ameloblasts are responsible for the formation of enamel, odontoblasts serve the same function in the formation of dentin. These odontoblasts act to secrete dentin as well as to secrete dentinal fluid into dentin tubules. Within each dentin tubule exists an odontoblastic process (an extension of an odontoblast that runs from the pulp to the dentinoenamel junction) and dentinal fluid, which has a mix of proteoglycans, albumin, transferrin, and tenascin. Dentin, when formed, is composed of 50% mineralized tissue (again, extracellular mineralized calcium hydroxyapatite) with 30% protein extracellular matrix (mostly collagen) and 20% water.7,13-15 Notably, while dentin is also avascular and acellular, dentin is immediately adjacent to odontoblastic cell bodies within the pulp with their associated odontoblastic processes extending into dentin.
Iatrogenic cavity preparations that extend into dentin cause the deposition of a smear layer (a zone of preparation debris), which needs to be altered or removed in order to expose dentinal collagen. Smear layer removal can be accomplished in several ways, including using self-etch adhesive systems and systems that rely on phosphoric etchants prior to application of an adhesive agent. Phosphoric acid etchants have been widely demonstrated to remove the smear layer, particularly etchants of 30% to 40% acid concentration.16 This etchant is very effective in removing the entire smear layer as it is demineralized and washed away in an etch-and-rinse technique. Drawbacks to this technique, however, are pronounced. Long-term degradation of dentinal collagen was shown to be more significant in an etch-and-rinse technique.14 It is postulated that the demineralization subsequent to this technique exposes more collagen than in other techniques. Subsequent to more collagen exposure is increased activity of matrix metalloproteinases (MMPs), which are endogenous collagenolytic proteins responsible for the degradation of the collagen component of the hybrid layer over time.17 A reduction in etching time by 50% has been shown to exhibit a dramatic increase in bond strength.16 Hu and colleagues demonstrated that aging-induced reductions in bond strength can be explained by the degradation of dentinal collagen, and this reduction in etching time (and exposure to acid etchant) reduces the activity of MMPs.3,14,18-20 Once exposed, this collagen is infiltrated with resin monomer to form a hybrid layer. Consisting of both dentin and resin, this collagen-resin layer forms the foundation for and is the most critical step in ensuring optimized bond strengths to dentin.21
Selective Enamel Etching
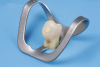
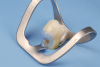
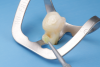
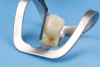
Given the preference to minimize degradation of dentinal collagen and to maintain a more viable hybrid layer, a selective enamel etching technique (Figure 1 through Figure 5) has been suggested. Ma and colleagues recently conducted a meta-analysis and after a review of 981 articles found that when a selective enamel etch protocol was used in addition to utilizing a self-etch system the outcomes were superior to a self-etch protocol alone.22 The authors found a higher incidence of marginal discoloration, unfavorable adaption and retention, and a higher incidence of fractures in a self-etch protocol alone (no phosphoric etch utilized) in 16 randomized controlled trials.
Amran et al recently further investigated selective enamel etching via computer-assisted imaging analysis in an in vitro setting to assess the accuracy of selective enamel etching and found no relationship between the application time of etchant and the accuracy of selective enamel etching.23 This suggests that containing the phosphoric acid etchant on enamel is more important than the amount of application time of the etchant if the clinician is faced with the issue of limiting etchant exposure time to prevent dentin exposure to it.
In Fuentes et al's recent research, the authors also investigated the application of an additional hydrophobic bonding resin to a universal adhesive, postulating in their 5-year study that this additional adhesive does not improve clinical performance.5 Their study, however, did show that phosphoric acid-etching was critical to the success of the universal adhesive. To further evaluate the effectiveness of a selective-etch technique, Cuevaz-Suárez and colleagues performed a meta-analysis of whether this technique would improve immediate and long-term bonding performance of universal adhesives.24 Their analysis showed that the selective enamel etch technique can improve the performance of mild universal adhesives. Further, their research indicated that mild universal adhesives seem to foster the optimum bond strength stability with or without acid-etching.
Because recent literature supports the selective etch of enamel, further evaluation has sought to determine whether etching of dentin is warranted or justified. Rosa et al conducted a meta-analysis review of universal adhesives in 10 scientific articles.25 They, as well as others,26,27 found that enamel bond strength was improved with phosphoric acid-etching, but the evidence did not support this effect for dentin in an etch-and-rinse strategy. There was no statistically significant difference between the etch-and-rinse techniques and a self-etch technique with regard to dentin microtensile bond strength. As a result, the use of mild universal adhesives with a selective enamel etch-and-rinse strategy has been advised.
The Push for a Universal Solution
To simplify the steps of adhesive dentistry, the dental profession has sought a universal solution for predictable bonding to enamel and dentin. The challenge, however, lies in the fact that enamel and dentin are markedly different substrates for bonding, as summarized by Perdigão.13 Despite attempts by manufacturers and clinicians to this end, preparing enamel and dentin with the same steps at the same time yields a suboptimal result for one substrate or the other. He further advised selective etching of enamel with phosphoric acid without etching the dentin. Also of interest in his work is the finding that although researchers and manufacturers may cite many in vitro results, these results cannot be directly extrapolated to clinical practice despite the desire of clinicians for a simplified and more versatile adhesive dentistry solution. Manufacturers continue to market novel materials hoping to capitalize on clinicians' yearning for the simplification of this process, but as Perdigão noted, scant evidence has been presented to validate the performance of an ultra-simplified dentin-enamel conditioner. Such adhesive systems have demonstrated insufficient bond strengths to enamel, incompatibility with self-curing resins, and low dentin bond strengths.13,28
Final Recommendations
The current scientific evidence suggests a selective enamel etch technique when preparing the dentition for adhesive dentistry (Figure 6). Enamel etching with phosphoric acid produces a surface with excellent wettability and chemical bonding potential, particularly when an adhesive containing MDP is utilized. Etching of dentin with phosphoric acid is discouraged because of the need for complete smear layer removal and its associated postoperative sensitivity, and most importantly, the potential for MMP activation within the collagen of the hybrid layer and its potential to cause long-term degradation of this layer. The combination of mild universal adhesives used with the selective enamel etch technique should be considered (Figure 7).
Until a technique and material are perfected that can achieve predictable adhesive outcomes for both enamel and dentin, the selective enamel etch technique should be the preferred choice of restorative dentists in the delivery of resin-bonded restorations.
About the Authors
Mark A. Koup, DMD
Clinical Associate Professor, Division of Restorative Dentistry, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania; Fellow, Academy of General Dentistry; Private Practice, Paoli, Pennsylvania
Markus B. Blatz, DMD, PhD
Professor of Restorative Dentistry, Chair, Department of Preventive and Restorative Sciences, and Assistant Dean, Digital Innovation and Professional Development, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania
Queries to the author regarding this course may be submitted to authorqueries@broadcastmed.com.
References
1. Santos MJM, Costa MD, Rêgo HMC, et al. Effect of surface treatments on the bond strength of self-etching adhesive agents to dentin. Gen Dent. 2017;65(4):e1-e6.
2. Huang XQ, Pucci CR, Luo T, et al. No-waiting dentine self-etch concept - merit or hype. J Dent. 2017;62:54-63.
3. Brackett MG, Li N, Brackett WW, et al. The critical barrier to progress in dentine bonding with the etch-and-rinse technique. J Dent. 2011;39
(3):238-248.
4. Lacruz RS, Habelitz S, Wright JT, Paine ML. Dental enamel formation and implications for oral health and disease. Physiol Rev. 2017;97(3):
939-993.
5. Fuentes MV, Perdigão J, Baracco B, et al. Effect of an additional bonding resin on the 5-year performance of a universal adhesive: a randomized clinical trial. Clin Oral Investig. 2023;27(2):837-848.
6. Alkattan R, Koller G, Banerji S, Deb S. Bis[2-(methacryloyloxy) ethyl] phosphate as a primer for enamel and dentine. J Dent Res. 2021;100
(10):1081-1089.
7. Tsujimoto A, Shimatani Y, Nojiri K, et al. Influence of surface wetness on bonding effectiveness of universal adhesives in etch-and-rinse mode. Eur J Oral Sci. 2019;127(2):162-169.
8. Vermelho PM, Reis AF, Ambrosano GM, Giannini M. Adhesion of multimode adhesives to enamel and dentin after one year of water storage. Clin Oral Investig. 2017;21(5):1707-1715.
9. Han F, Sun Z, Xie H, Chen C. Improved bond performances of self-etch adhesives to enamel through increased MDP-Ca salt formation via phosphoric acid pre-etching. Dent Mater. 2022;38(1):133-146.
10. Kharouf N, Reitzer F, Ashi T, et al. Effectiveness of etching with phosphor-ic acid when associated with rubbing technique. J Stoma. 2021;74(1):16-21.
11. Wang R, Shi Y, Li T, et al. Adhesive interfacial characteristics and the related bonding performance of four self-etching adhesives with different functional monomers applied to dentin. J Dent. 2017;62:72-80.
12. Katyal D, Subramanian AK, Venugopal A, Marya A. Assessment of wettability and contact angle of bonding agent with enamel surface etched by five commercially available etchants: an in vitro study. Int J Dent. 2021;2021:9457553.
13. Perdigão J. Current perspectives on dental adhesion: (1) dentin adhesion - not there yet. Jpn Dent Sci Rev. 2020;56(1):190-207.
14. Tjäderhane L. Dentin bonding: can we make it last? Oper Dent. 2015;40
(1):4-18.
15. Ricci HA, Scheffel DL, Mariusso MR, et al. Exposed collagen in resin bonds to caries-affected dentin after dentin treatment with aqueous and alcoholic chlorhexidine solutions. J Adhes Dent. 2014;16(1):21-28.
16. Saikaew P, Sattabanasuk V, Harnirattisai C, et al. Role of the smear layer in adhesive dentistry and the clinical applications to improve bonding performance. Jpn Dent Sci Rev. 2022;58:59-66.
17. Breschi L, Martin P, Mazzoni A, et al. Use of a specific MMP-inhibitor (galardin) for preservation of hybrid layer. Dent Mater. 2010;26(6):571-578.
18. Hu L, Xiao YH, Fang M, et al. Effects of type I collagen degradation on the durability of three adhesive systems in the early phase of dentin bonding. PLoS One. 2015;10(2):e0116790.
19. Burrer P, Dang H, Par M, et al. Effect of over-etching and prolonged application time of a universal adhesive on dentin bond strength. Polymers (Basel). 2020;12(12):2902.
20. Scheffel DL, Hebling J, Scheffel RH, et al. Inactivation of matrix-bound matrix metalloproteinases by cross-linking agents in acid-etched dentin. Oper Dent. 2014;39(2):152-158.
21. Jin X, Han F, Wang Q, et al. The roles of 10-methacryloyloxydecyl dihydrogen phosphate and its calcium salt in preserving the adhesive-dentin hybrid layer. Dent Mater. 2022;38(7):1194-1205.
22. Ma KS, Wang LT, Blatz MB. Efficacy of adhesive strategies for restorative dentistry: a systematic review and network meta-analysis of double-blind randomized controlled trials over 12 months of follow-up. J Prosthodont Res. 2023;67(1):35-44.
23. Amran T, Meier D, Amato J, et al. Accuracy of selective enamel etching: a computer-assisted imaging analysis. Oper Dent. 2023;48(5):538-545.
24. Cuevas-Suárez CE, da Rosa WLO, Lund RG, et al. Bonding performance of universal adhesives: an updated systematic review and meta-analysis. J Adhes Dent. 2019;21(1):7-26.
25. Rosa WL, Piva E, Silva AF. Bond strength of universal adhesives: a systematic review and meta-analysis. J Dent. 2015;43(7):765-776.
26. Josic U, Mazzitelli C, Maravic T, et al. The influence of selective enamel etch and self-etch mode of universal adhesives' application on clinical behavior of composite restorations placed on non-carious cervical lesions: a systematic review and meta-analysis. Dent Mater. 2022;38(3):472-488.
27. Park KJ, Pfeffer M, Näke T, et al. Evaluation of low-viscosity bulk-fill composites regarding marginal and internal adaptation. Odontology. 2021;109(1):139-148.
28. Pucci CR, Gu LS, Zeng C, et al. Susceptibility of contemporary single-bottle self-etch dentine adhesives to intrinsic water permeation. J Dent. 2017;66:52-61.