You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
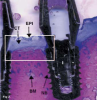
The term bone-to-implant contact (BIC) refers to the amount of bone that touches an implant, and it is a critical component of achieving osseointegration.1 Osseointegration of a dental implant denotes bone-to-metal contact without intervening non-bone tissue. Initially, Bränemark suggested that osseointegration results in bone contacting the implant.2 Subsequently, the term osseointegration was redefined to indicate there was bone-to-implant contact under a light microscope, because under scanning electron microscopy there is always about a 100 angstroms space between bone and a dental implant.3 Figure 1 schematically depicts what can be seen under the light microscope. The implant can touch either bone or other tissues. Figure 2 and Figure 3 are histological representations of high and moderate BIC, respectively.
BIC affects the outcome of clinical procedures, and increased BIC is believed to result in better implant stability.4 The amount of BIC is a microscopic phenomenon and cannot be accurately determined when placing an implant. Furthermore, many factors can influence the percentage of BIC. In this article, the term BIC is used to indicate the percentage of the implant that contacts bone. The authors assessed the literature to determine what is currently known about BIC.
Primary and Secondary Implant Stability
Primary stability (mechanical stabilization) is achieved when an implant is inserted into bone and the implant manifests no visible movement when forces are applied to it.5 Features affecting firmness include bone vertical and horizontal dimensions, surgical technique used to create an osteotomy, bone density, magnitude of insertion torque, percentage of initial bone-implant interface, implant geometry, and surface micromorphology.6-8 Initial implant stability is strongly correlated with 3-dimensional BIC.7
In contrast, secondary stability (biological stability) happens when new bone is deposited along the implant interface. Bone formation results in biological anchorage of the implant, and this is synonymous with osseointegration.9 In the present article, reported BIC percentages are associated with secondary (biologic) stability; if they are related to primary stability, it will be indicated.
Laboratory Assessment to Determine the Percentage of BIC
In 1982, Donath and Breuner developed a technique to study undecalcified sections of bone and teeth, and this method is used to look at 20-µm to 30-µm stained slices of BIC.10 Histomorphometry is another technique commonly used to study BIC.11 However, it is a destructive method and much of the information is lost when processing samples. In contrast, microcomputed tomography is a non-destructive technique that can be employed to assess BIC. It uses absorption of x-rays to identify density differences inside solid matter.12 Bernhardt et al reported that microcomputed tomography can detect BIC and the results are similar to histomorphometric findings.12 BIC assessments can also be done by electron microscopy.13
Clinical Evaluation of Bone Density Prior to
Dental Implantation
Assessing bone density prior to dental implantation provides information that can be used when treatment planning a case. For instance, it may be decided to undersize an osteotomy or place a larger implant if the bone is not sufficiently dense to gain additional frictional retention for an inserted implant. Different methods can be used to evaluate bone density prior to implant placement.
Radiographic evaluation: Computed tomography (CT) is a radiographic technique for assessing bone density. CT provides 3-dimensional images that can be used to accurately assess the volume and density of bone, which is expressed in Hounsfield units (HU).14 In contrast, cone-beam computed tomography (CBCT) scans do not provide accurate HUs and may be inconsistent when recording bone density.15
Clinical assessment: A thin twist drill can be used during osteotomy preparation to initially ascertain the density of bone,16 and an estimation of cortical bone thickness and bone density can be assessed. Bone density is usually recorded as soft, medium, or hard.17,18 Historically, Misch classified bone densities as D1 to D4 (hard to soft, based on resistance to drilling).19 However, Trisi et al found that clinicians could not accurately differentiate between D2 and D318; therefore, only three densities of bone are usually differentiated from each other.17 The method used to evaluate bone density may vary depending on the individual patient's needs or clinician preference.
Site Preparation
A conventional drilling technique to prepare for an implant entails sequential enlargement of the drill diameter to expand the osteotomy. Contrastingly, under-preparation creates the osteotomy narrower than the inserted implant, thereby increasing frictional retention and facilitating increased initial torque values and implant stabilization. Data variance exists regarding the effect of under-drilling and how this technique impacts BIC. BIC values when using standard drilling techniques and under-drilling ranged from 20% to 62.6%.20-24 Most researchers reported no statistical difference in BIC between the two surgical approaches,20-22,24 while others reported significantly higher BIC was obtained with under-drilling.23,24 In general, both drilling techniques produce BIC values that result in successful implantations.
Bone Grafting's Impact on Bone Density
Bone grafting is commonly used to increase bone volume in areas where there is insufficient bone to support a dental implant.25 However, bone grafted sites that demonstrate increased bone volume do not manifest a greater bone density or percentage vitality than bone adjacent to the grafted site.26 Bone grafts become integrated and fuse with adjacent native bone.27 On the other hand, bone grafted sites will continue to mineralize up to 1 year, thereby demonstrating greater bone density.28 Bone density can be increased at sites manifesting reduced bone density by using osteotomes or osseo-densification burs (eg, at sites with D4 bone).29,30 In this regard, osseo-densification was demonstrated to result in increased initial BIC,31,32 and this value was greater than that achieved with osteotomes (62.5% vs 31.4%).33
Relationship Between Bone Density and BIC
Bone density affects the quality of bone available to support dental implants and influences the degree of BIC.34,35 Misch reported the following levels of BIC adjacent to implants related to different bone densities: D1, 85%; D2, 65% to 70%; D3, 40% to 50%; and D4, 30% (D1 to D4 reflect decreasing bone densities).35
Similarly, Hao et al reported that bone density affects the percentage of BIC adjacent to implants at different positions in the mouth.34 They used CBCT scans and found bone density was greater in the anterior mandible > anterior maxilla > posterior mandible > posterior maxilla. A systematic review by Sağirkaya et al also related BIC to different regions in the mouth.36 They reported that mean maxillary and mandibular BICs after several months were 53.84% and 70.97%, respectively. The higher percentage BIC in the mandible may be attributed to the fact that the bone is 1.8 times denser in the mandible than in the maxilla.37 The amount of BIC was higher in the anterior mandibular regions (79.92%) than the posterior mandibular areas (69.14%). Similarly, in the maxilla, the anterior segment had a 74.19% BIC and the posteriors were 36.68%.36
Studies reported a moderate association between bone density and primary implant stability.38,39 In addition, a systematic review by Marquezan et al noted a moderate association between HUs and implant stability quotient (ISQ).40
In general, higher bone density is associated with better implant stability and a higher degree of BIC. This is due to the fact that denser bone has a greater capacity to support an implant. In contrast, lower bone density can result in reduced implant stability and a lower degree of BIC, which may increase the risk of implant failure. Other influences such as implant design, surface roughness, surgical technique, and healing time can influence BIC; thus, bone density is not the only factor that determines implant success.
Correlation Between BIC and Insertion Torque
Insertion torque is the amount of rotational force required to place an implant into the bone.41 Several studies demonstrated a positive correlation between insertion torque and initial BIC, suggesting that higher insertion torque is associated with greater BIC and implant stability.42,43 For example, Park et al evaluated the relationship between initial implant stability and BIC in a rabbit tibia model and found a significant correlation between insertion torque and BIC.43 Similarly, Liu et al reported a strong positive correlation between insertion torque and BIC recorded using 3D micro-CT images around implants inserted into artificial cortical and cancellous bone.42
From a different perspective, several animal studies failed to show a correlation between the degree of BIC and RFA (resonance frequency amplitude, used to measure implant stability) after osseointegration.44,45 In this regard, Manresa et al surmised that the lack of association between BIC and ISQ underscores that ISQ values determined by RFA are not able to provide insight regarding the percentage of BIC.46
Overall, most studies support the notion that higher insertion torque is associated with greater BIC and implant stability. However, as mentioned previously, other factors, such as bone quality and implant design, can also affect BIC and implant stability.
Implant Diameter, Length, and Geometry
The geometry of an implant may have an effect on the percentage of BIC. When the BIC of standard-diameter (3.5-mm diameter) and wide (5-mm diameter) implants was compared, the BIC (secondary stability) reportedly was 71% and 73%, respectively. These results were not statistically different.47 Similarly, Hsu et al reported BIC values for different diameter implants, and the BIC (primary stability) was 56.4% for a 6-mm diameter implant and 53.9% for a 3.75-mm diameter implant.48 Thus, while a wider implant provides more surface area, it does not mean that the BIC increases with greater implant diameters.
The effect of implant length on BIC was assessed using micro-computed tomography.49 With increased length there is more surface area, but with additional depth the implant only contacts cancellous bone, which is porous. Hsu et al reported that implants with different lengths in porous trabecular bone demonstrated significant differences for ISQ values between implants with lengths of 8.5 mm and 13 mm and 8.5 mm and 11.5 mm, but there were no significant increases for BIC (primary stability).49 This occurred despite the fact that the potential BIC area was larger with longer implants.
Implant macroscopic features can affect BIC. Threaded implants provide more BIC than non-threaded implants.50 Decreasing thread pitch provides greater surface area, which can increase BIC and primary stability.51 Deeper implant threads also provide more surface area for BIC.52 Studies demonstrated that screw-type implants had a higher BIC than cylinder implants53 and that square-threaded implants had a higher BIC than v-shaped thread shapes.54 Numerous investigations indicated that tapered implants initially provide greater primary stability than cylindrical implants based on ISQ and insertion torque values.53,55,56 Many of these features have been incorporated into contemporary implants.
Implant Positioning
Dental implants can be positioned coronal to the crest of bone, at the crest, or subcrestally. This can affect the amount of bone resorption that occurs. Some authors noted that the position of the implant platform did not interfere with osseointegration or the amount of BIC (which ranged from 51.1% to 69.4%).57,58
BIC Changes Over Time and Function
The percentage of BIC has the capacity to change over time due to a variety of factors. After an implant is initially placed, the BIC can increase over time due to healing and function.59-61 It was noted that healing of unloaded conventional implants resulted in a mean increase of BIC at <3 months to >3months (44.35% vs 66.31%).36 It was demonstrated that conventionally loaded implants manifest an increased BIC when compared to unloaded implants (75.7% vs 54.07%).36 In this regard, Tumedei et al also reported that loaded implants presented 10% to12% higher BIC values when compared to submerged, unloaded implants.62
In contrast, Lian et al suggested that initial findings of high BIC may be reversed.63 Using finite element analysis, they proposed that BIC percentages ranging from 25% to 100% have little influence on the final BIC, which is around 58% to 60%. This reduction in the percentage of BIC was attributed to remodeling of bone to achieve a bone equilibrium state. An analogous situation was noted when implants were placed with high torque values. The bone remodels over time and decreases the torque values to ones that are in equilibrium with the existing bone.64,65 This was confirmed with reverse torque testing to remove the implants. De-osseointegration and peri-implantitis also can reduce the percentage of BIC.
Minimum BIC to Provide Implant Stability
The minimum BIC required to provide implant stability depends on several factors, including implant design, implant location, and patient-specific characteristics such as bone density. Overall, implants are unlikely to achieve 100% contact with surrounding bone (Figure 3).66 Furthermore, Sağirkaya et al reported there was a large range of mean BIC associated with commercially inserted implants (54% to 87%).36 Nevertheless, the BIC can vary for a single implant, spanning widely from 2.82% to 100%.36 At present, the minimum BIC necessary for a successful implant outcome is undetermined. In this regard, Bolind et al stated that the amount of BIC in successful oral implants varied between 60% and 99% with no evidence that implants with 99% BIC fared better than those with 60% BIC.67
Relationship Between BIC and De-osseointegration
De-osseointegration is the loss of dental implant osseointegration.68 It is synonymous with loss or rupture of BIC. It is often attributed to occlusal overload, and the stable implant becomes movable. Usually, in such cases the implant can be rotated and may not be movable horizontally unless there was previous bone loss due to peri-implantitis. Occlusal overload can occur when chewing forces exceed the capacity of the BIC to stabilize the implant. De-osseointegration also may happen when a component such as a healing abutment is torqued and the force exceeds the resistance provided by BIC. A cracking sound may be heard. If this happens, it may be possible to anesthetize the patient and re-torque the implant into place so that it can re-osseointegrate over time (eg, 3 months).69 Another method of treatment is to remove the implant and place a larger one into the osteotomy to re-engage the socket walls.
Microscopic Treatments of Implants to Increase BIC
Several implant surface treatments were developed to increase BIC.70-73 Such treatments are designed to modify the implant surface to promote better osseointegration and enhance stability. Studies reported that rough implant surfaces provide better bone apposition and increased BIC than implants with smooth surfaces.70,71 Tumedei et al reported that rougher surfaces had, on average, about a 10% higher BIC than machined surfaces.62 Among the most common implant surface treatments are acid-etching sandblasting, plasma-spraying laser treatment, and nanotexturing.72,73
Issues Associated With Animal Models
Animal models to study BIC provide advantages and disadvantages.74 No single animal model is exactly similar to human bone. For instance, measuring insertion torque in rabbits is flawed, because the tibia of rabbits is hollow and mostly cortical bone. Similarly, rodents have a minimal amount of cancellous bone. Mature sheep have denser trabecular bone than humans, but immature sheep have weaker, low-density trabecular bone. On the other hand, large-bred dogs can often support human-sized implants. Thus, there are limitations to consider when inferring implant outcomes from animals to humans, including differences in bone micro- and macrostructure, rates of growth, and bone sizes.74
Conclusions
BIC provides both primary and secondary (biologic) implant stability. Clinically, the percentage of BIC cannot be determined at the time of implant placement or at subsequent appointments. A range of mean BIC percentages is associated with different commercial implants, typically averaging between 54% to 87%. Yet, when considering individual implants, the percentage of BIC can exhibit a wide span, ranging from as low as 2.82% to as high as 100%.36 Improvements in implant design have resulted in increased amounts of BIC. The minimum BIC to provide dental implant success is unknown.
About the Authors
Sultan Albeshri, BDS, MS
Assistant Professor, Department of Periodontics and Community Dentistry, College of Dentistry, King Saud University, Riyadh, Saudi Arabia
Gary Greenstein, DDS, MS
Former Clinical Professor, Department of Periodontology, College of Dental Medicine, Columbia University, New York, New York; Private Practice, Surgical Implantology and Periodontics, Freehold, New Jersey
Queries to the author regarding this course may be submitted to authorqueries@broadcastmed.com.
References
1. Sennerby L, Wennerberg A, Pasop F. A new microtomographic technique for non-invasive evaluation of the bone structure around implants. Clin Oral Implants Res. 2001;12(1):91-94.
2. Brånemark PI. Osseointegration and its experimental background. J Prosthet Dent. 1983;50(3):399-410.
3. Albrektsson T, Brånemark PI, Hansson HA, Lindström J. Osseointegrated titanium implants. Requirements for ensuring a long-lasting, direct bone-to-implant anchorage in man. Acta Orthop Scand. 1981;52(2):155-170.
4. Park YS, Yi KY, Lee IS, Jung YC. Correlation between microtomography and histomorphometry for assessment of implant osseointegration. Clin Oral Implants Res. 2005;16(2):156-160.
5. Lioubavina-Hack N, Lang NP, Karring T. Significance of primary stability for osseointegration of dental implants. Clin Oral Implants Res. 2006;17(3):244-250.
6. Hsu JT, Huang HL, Chang CH, et al. Relationship of three-dimensional bone-to-implant contact to primary implant stability and peri-implant bone strain in immediate loading: microcomputed tomographic and in vitro analyses. Int J Oral Maxillofac Implants. 2013;28(2):367-374.
7. Huang HL, Tsai MT, Su KC, et al. Relation between initial implant stability quotient and bone-implant contact percentage: an in vitro model study. Oral Surg Oral Med Oral Pathol Oral Radiol. 2013;116(5):e356-e361.
8. Martinez H, Davarpanah M, Missika P, et al. Optimal implant stabilization in low density bone. Clin Oral Implants Res. 2001;12(5):423-432.
9. Monje A, Ravidà A, Wang HL, et al. Relationship between primary/mechanical and secondary/biological implant stability. Int J Oral Maxillofac Implants. 2019;34:s7-s23.
10. Donath K, Breuner G. A method for the study of undecalcified bones and teeth with attached soft tissues. The Säge-Schliff (sawing and grinding) technique. J Oral Pathol. 1982;11(4):318-326.
11. Johansson CB, Hansson HA, Albrektsson T. Qualitative interfacial study between bone and tantalum, niobium or commercially pure titanium. Biomaterials. 1990;11(4):277-280.
12. Bernhardt R, Kuhlisch E, Schulz MC, et al. Comparison of bone-implant contact and bone-implant volume between 2D-histological sections and 3D-SRµCT slices. Eur Cell Mater. 2012;23:237-247.
13. Linder L, Albrektsson T, Brånemark PI, et al. Electron microscopic analysis of the bone-titanium interface. Acta Orthop Scand. 1983;54(1):45-52.
14. Aranyarachkul P, Caruso J, Gantes B, et al. Bone density assessments of dental implant sites: 2. Quantitative cone-beam computerized tomography. Int J Oral Maxillofac Implants. 2005;20(3):416-424.
15. Campos MJ, de Souza TS, Mota Júnior SL, et al. Bone mineral density in cone beam computed tomography: only a few shades of gray. World J Radiol. 2014;6(8):607-612.
16. Greenstein G, Cavallaro J, Greenstein B, Tarnow D. Treatment planning implant dentistry with a 2-mm twist drill. Compend Contin Educ Dent. 2010;31(2):126-132.
17. Cavallaro J Jr, Greenstein B, Greenstein G. Clinical methodologies for achieving primary dental implant stability: the effects of alveolar bone density. J Am Dent Assoc. 2009;140(11):1366-1372.
18. Trisi P, Rao W. Bone classification: clinical-histomorphometric comparison. Clin Oral Implants Res. 1999;10(1):1-7.
19. Misch CE. Bone density: a key determinant for clinical success. In: Misch CE, ed. Contemporary Implant Dentistry. 2nd ed. St Louis, MO: Mosby; 1999:109-118.
20. Campos FE, Gomes JB, Marin C, et al. Effect of drilling dimension on implant placement torque and early osseointegration stages: an experimental study in dogs. J Oral Maxillofac Surg. 2012;70(1):43-50.
21. Pantani F, Botticelli D, Garcia IR Jr, et al. Influence of lateral pressure to the implant bed on osseointegration: an experimental study in dogs. Clin Oral Implants Res. 2010;21(11):1264-1270.
22. Shalabi MM, Wolke JG, de Ruijter AJ, Jansen JA. Histological evaluation of oral implants inserted with different surgical techniques into the trabecular bone of goats. Clin Oral Implants Res. 2007;18(4):489-495.
23. Smith A, Hosein YK, Dunning CE, Tassi A. Fracture resistance of commonly used self-drilling orthodontic mini-implants. Angle Orthod. 2015;85(1):26-32.
24. Stocchero M, Toia M, Cecchinato D, et al. Biomechanical, biologic, and clinical outcomes of undersized implant surgical preparation: a systematic review. Int J Oral Maxillofac Implants. 2016;31(6):1247-1263.
25. AlKudmani H, Al Jasser R, Andreana S. Is bone graft or guided bone regeneration needed when placing immediate dental implants? A systematic review. Implant Dent. 2017;26(6):936-944.
26. Froum SJ, Tarnow DP, Wallace SS, et al. The use of a mineralized allograft for sinus augmentation: an interim histological case report from a prospective clinical study. Compend Contin Educ Dent. 2005;26(4):259-260.
27. Einhorn TA. The cell and molecular biology of fracture healing. Clin Orthop Relat Res. 1998(355 suppl):S7-S21.
28. Greenstein G, Greenstein B, Cavallaro Jr J, Carpentieri C. Alveolar bone and implant therapy decisions in dentistry. Decisions in Dentistry. 2018;4(5):26-32.
29. Elsayed MD. Biomechanical factors that influence the bone-implant-interface. Res Rep Oral Maxillofac Surg. 2019;3(1):1-14.
30. Tretto PHW, Fabris V, Cericato GO, et al A. Does the instrument used for the implant site preparation influence the bone-implant interface? A systematic review of clinical and animal studies. Int J Oral Maxillofac Surg. 2019;48(1):97-107.
31. Lahens B, Neiva R, Tovar N, et al. Biomechanical and histologic basis of osseodensification drilling for endosteal implant placement in low density bone. An experimental study in sheep. J Mech Behav Biomed Mater. 2016;63:56-65.
32. Trisi P, Berardini M, Falco A, Podaliri Vulpiani M. New osseodensification implant site preparation method to increase bone density in low-density bone: in vivo evaluation in sheep. Implant Dent. 2016;25(1):24-31.
33. Tian JH, Neiva R, Coelho PG, et al. Alveolar ridge expansion: comparison of osseodensification and conventional osteotome techniques. J Craniofac Surg. 2019;30(2):607-610.
34. Hao Y, Zhao W, Wang Y, et al. Assessments of jaw bone density at implant sites using 3D cone-beam computed tomography. Eur Rev Med Pharmacol Sci. 2014;18(9):1398-1403.
35. Misch CE. Density of bone: effect on treatment plans, surgical approach, healing, and progressive boen loading. Int J Oral Implantol. 1990;6(2):23-31.
36. Sağirkaya E, Kucukekenci AS, Karasoy D, et al. Comparative assessments, meta-analysis, and recommended guidelines for reporting studies on histomorphometric bone-implant contact in humans. Int J Oral Maxillofac Implants. 2013;28(5):1243-1253.
37. Kim YJ, Henkin J. Micro-computed tomography assessment of human alveolar bone: bone density and three-dimensional micro-architecture. Clin Implant Dent Relat Res. 2015;17(2):307-313.
38. Farré-Pagés N, Augé-Castro ML, Alaejos-Algarra F, et al. Relation between bone density and primary implant stability. Med Oral Patol Oral Cir Bucal. 2011;16(1):e62-e67.
39. Turkyilmaz I, Tumer C, Ozbek EN, Tözüm TF. Relations between the bone density values from computerized tomography, and implant stability parameters: a clinical study of 230 regular platform implants. J Clin Periodontol. 2007;34(8):716-722.
40. Marquezan M, Osório A, Sant'Anna E, et al. Does bone mineral density influence the primary stability of dental implants? A systematic review. Clin Oral Implants Res. 2012;23(7):767-774.
41. Greenstein G, Cavallaro J. Implant insertion torque: its role in achieving primary stability of restorable dental implants. Compend Contin Educ Dent. 2017;38(2):88-95.
42. Liu C, Tsai MT, Huang HL, et al. Relation between insertion torque and bone-implant contact percentage: an artificial bone study. Clin Oral Investig. 2012;16(6):1679-1684.
43. Park IP, Kim SK, Lee SJ, Lee JH. The relationship between initial implant stability quotient values and bone-to-implant contact ratio in the rabbit tibia. J Adv Prosthodont. 2011;3(2):76-80.
44. Ito Y, Sato D, Yoneda S, et al. Relevance of resonance frequency analysis to evaluate dental implant stability: simulation and histomorphometrical animal experiments. Clin Oral Implants Res. 2008;19(1):9-14.
45. Schliephake H, Sewing A, Aref A. Resonance frequency measurements of implant stability in the dog mandible: experimental comparison with histomorphometric data. Int J Oral Maxillofac Surg. 2006;35(10):941-946.
46. Manresa C, Bosch M, Echeverría JJ. The comparison between implant stability quotient and bone-implant contact revisited: an experiment in Beagle dog. Clin Oral Implants Res. 2014;25(11):1213-1221.
47. Brink J, Meraw SJ, Sarment DP. Influence of implant diameter on surrounding bone. Clin Oral Implants Res. 2007;18(5):563-568.
48. Hsu JT, Shen YW, Kuo CW, et al. Impacts of 3D bone-to-implant contact and implant diameter on primary stability of dental implant. J Formos Med Assoc. 2017;116(8):582-590.
49. Hsu JT, Wu AY, Fuh LJ, Huang HL. Effects of implant length and 3D bone-to-implant contact on initial stabilities of dental implant: a microcomputed tomography study. BMC Oral Health. 2017;17(1):132.
50. Tushar SG, Chaudhary A, Aggarwal A. Scientific rationale of implant design: a review article. Saudi J Oral Dent Res. 2022;7(4):101-106.
51. Orsini E, Giavaresi G, Trirè A, et al. Dental implant thread pitch and its influence on the osseointegration process: an in vivo comparison study. Int J Oral Maxillofac Implants. 2012;27(2):383-392.
52. Strong J, Misch C, Bidez M, et al. Functional surface area: thread-form parameter optimization for implant body design. Compend Contin EducDent. 1998;19(3):4-9.
53. Nandini N, Kunusoth R, Alwala AM, et al. Cylindrical implant versus tapered implant: a comparative study. Cureus. 2022;14(9):e29675.
54. Steigenga J, Al-Shammari K, Misch C, et al. Effects of implant thread geometry on percentage of osseointegration and resistance to reverse torque in the tibia of rabbits. J Periodontol. 2004;75(9):1233-1241.
55. Barikani H, Rashtak S, Akbari S, et al. The effect of shape, length and diameter of implants on primary stability based on resonance frequency analysis. Dent Res J (Isfahan). 2014;11(1):87-91.
56. Lozano-Carrascal N, Salomó-Coll O, Gilabert-Cerdà M, et al. Effect of implant macro-design on primary stability: a prospective clinical study. Med Oral Patol Oral Cir Bucal. 2016;21(2):e214-e221.
57. Boquete-Castro A, Gómez-Moreno G, Aguilar-Salvatierra A, et al. Influence of the implant design on osseointegration and crestal bone resorption of immediate implants: a histomorphometric study in dogs. Clin Oral Implants Res. 2015;26(8):876-881.
58. Pontes AE, Ribeiro FS, Iezzi G, et al. Bone-implant contact around crestal and subcrestal dental implants submitted to immediate and conventional loading. ScientificWorldJournal. 2014;2014:606947.
59. Kuzyk PR, Schemitsch EH. The basic science of peri-implant bone healing. Indian J Orthop. 2011;45(2):108-115.
60. Mathieu V, Vayron R, Soffer E, et al. Influence of healing time on the ultrasonic response of the bone-implant interface. Ultrasound Med Biol. 2012;38(4):611-618.
61. Rønold HJ, Ellingsen JE. Effect of micro-roughness produced by TiO2 blasting-tensile testing of bone attachment by using coin-shaped implants. Biomaterials. 2002;23(21):4211-4219.
62. Tumedei M, Piattelli A, Degidi M, et al. A narrative review of the histological and histomorphometrical evaluation of the peri-implant bone in loaded and unloaded dental implants. A 30-year experience (1988-2018). Int J Environ Res Public Health. 2020;17(6):2088.
63. Lian Z, Guan H, Ivanovski S, et al. Effect of bone to implant contact percentage on bone remodelling surrounding a dental implant. Int J Oral Maxillofac Surg. 2010;39(7):690-698.
64. Becker W, Sennerby L, Bedrossian E, et al. Implant stability measurements for implants placed at the time of extraction: a cohort, prospective clinical trial. J Periodontol. 2005;76(3):391-397.
65. Nedir R, Bischof M, Szmukler-Moncler S, et al. Predicting osseointegration by means of implant primary stability. Clin Oral Implants Res. 2004;15(5):520-528.
66. Papavasiliou G, Kamposiora P, Bayne SC, Felton DA. 3D-FEA of osseointegration percentages and patterns on implant-bone interfacial stresses. J Dent. 1997;25(6):485-491.
67. Bolind P, Johansson CB, Balshi TJ, et al. A study of 275 retrieved Brånemark oral implants. Int J Periodontics Restorative Dent. 2005;25(5):425-437.
68. International Congress of Oral Implantologists. De-osseointegration. ICOI website. https://www.icoi.org/glossary/de-osseointegration/. Accessed October 2, 2023.
69. Soliman O. Success and survival of re-torquing an early failed dental implant: a 2-year multicenter prospective study. Egyptian Journal of Oral and Maxillofacial Surgery. 2020;11(2):64-69.
70. Hallgren C, Reimers H, Chakarov D, et al. An in vivo study of bone response to implants topographically modified by laser micromachining. Biomaterials. 2003;24(5):701-710.
71. Javed F, Almas K, Crespi R, Romanos GE. Implant surface morphology and primary stability: is there a connection? Implant Dent. 2011;20(1):40-46.
72. Jemat A, Ghazali MJ, Razali M, Otsuka Y. Surface modifications and their effects on titanium dental implants. Biomed Res Int. 2015;2015:791725.
73. Le Guéhennec L, Soueidan A, Layrolle P, Amouriq Y. Surface treatments of titanium dental implants for rapid osseointegration. Dent Mater. 2007;23(7):844-854.
74. Wancket LM. Animal models for evaluation of bone implants and devices: comparative bone structure and common model uses. Vet Pathol. 2015;52(5):842-850.