You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Since Charles H. Land patented the first all-porcelain "jacket" crown in 1889,1 various porcelains have been introduced to dentistry. Today, there are many different classifications,2 and these classifications make it easier for both the dentist and the laboratory technician to understand the types of dental porcelain available and their applications. Not having a thorough understanding of the indications and contraindications as well as the selection criteria for the material and design can lead to unpredictable results. It can also ultimately lead to technical complications, such as chipping, crown fracture, framework fracture, chipping of the veneered porcelain, unesthetic results, and other failures.
Classification by Microstructure
Dental ceramics consist of two phases, the glassy phase and the crystalline phase. According to the literature, one way that dental ceramics are classified is based on their microstructure. Regarding microstructure, Giordano and McLaren categorized ceramics into four groups: glass-based ceramics; glass-based ceramics with fillers, usually crystalline; crystalline-based ceramics with glass fillers, and polycrystalline solids (See Table 1).3
Glass-Based Ceramics
Glass-based ceramics, which contain mainly silica, primarily consist of the glassy phase aluminosilicate. Although their mechanical properties (eg, flexural strength of 60 MPa to 70 MPa) are the weakest when compared with the other categories, they have the highest esthetic properties.3 This type of porcelain can be used in porcelain laminate veneers, metal-ceramic (eg, porcelain-fused-to-metal, porcelain-pressed-to-metal) restorations, and porcelain jacket crowns (ie, monolithic glass-based crowns). Due to the presence of the glassy phase in glass-based ceramics, they are etchable and must be bonded with resin cements in order to reinforce their weak mechanical properties. Glass-based ceramics have the weakest masking properties; therefore, it has been recommended to have 0.2 mm to 0.3 mm of thickness for every change in shade from the stump shade.4
Glass-Based Ceramics With Crystalline Fillers
Unlike glass ceramics, this category has a glassy phase as well as a crystalline phase. The percentage of the crystalline phase differs among the various porcelains in this category. The flexural strength of glass-based ceramics with crystalline fillers depends on the nature of the crystalline phase, but in general, the ceramics in this category exhibit higher flexural strength than glass ceramics. Like glass ceramics, however, glass-based ceramics with crystalline fillers are also etchable and must be bonded to teeth with resin cements in order to achieve optimal results. This category can be further broken down into subcategories, including the following3:
• Low-to-Moderate (10% to 25%5) Leucite-Containing Feldspathic Glass.The incorporation of leucite into the glass structure may benefit the ceramic's strength by inhibiting crack propagation as well as altering the coefficient of thermal expansion (CTE).3 The first generation of leucite materials had large crystals with average sizes of more than 100 μm; however, newer leucite materials have thinner crystals with average sizes of 10 μm to 20 μm, which are less abrasive and possess greater flexural strength.6 This category is mainly used as veneering porcelains for metal-ceramic restorations.
• High (≈ 50%) Leucite-Containing Glass, Glass-Ceramics. In this category, the leucite crystals undergo a secondary heat treatment, which enhances their mechanical and physical properties and resistance to fracture, heat, and erosion. These crystals help to inhibit crack propagation.3
• Lithium Disilicate Glass-Ceramics. This category has a glass matrix that is made of lithium silicate with lithium disilicate crystals in between. Lithium disilicate glass-ceramics possess flexural strengths of 360 MPa to 400 MPa, which is approximately 3 times stronger than the previous category.7 They are highly translucent, which allows them to be used for veneers to achieve results with excellent esthetics. Another filler that can be added to the glass structure is fluoroapatite. Fluoroapatite crystals, which contain fluoride, enhance the material's optical properties and have an effect on thermal expansion.8
Crystalline-Based Ceramics With Infiltrated Glass
These ceramics consist of a porous crystalline matrix with glass infiltrated among the porosities. Primarily fabricated using a method called slip casting, crystalline-based ceramics with infiltrated glass are mainly comprised of an alumina matrix that can be augmented with other fillers, such as magnesia and zirconia.3 Crystalline-based ceramics require preparations with at least 1.2 mm of space, but 1.5 mm of space is preferred when masking or changing shade. The preparations should be designed to permit a 0.5-mm core as well as 1 mm of porcelain to achieve optimal esthetic results.4
Polycrystalline Solids
Polycrystalline solids consist entirely of crystalline phase material with no glassy phase. The crystals can be either zirconia or alumina. Not having a glassy phase makes these ceramics unetchable, too opaque for esthetic cases, and the strongest among all of the other categories with flexural strengths of above 1,000 MPa.9 The mechanical properties of polycrystalline solids make them suitable for multiunit restorations in posterior, high-stress areas; however, due to their opacity, they are not recommended for use in the anterior region.6
Zirconia has three different phases, each of which occur at different temperatures. Zirconia is in the monoclinic phase from room temperature to 1,170°C, the tetragonal phase from 1,170°C to 2,370°C, and the cubic phase from 2,370°C to 2,716°C. The tetragonal phase is the strongest phase of all, and the addition of yttria to zirconia stabilizes this phase, allowing it to occur at room temperature.10 During the past few years, translucent zirconia has also become available for esthetic cases. Translucent zirconia is fabricated by adjusting the grain size or increasing the yttria content to stabilize the cubic phase at room temperature; therefore, translucent zirconia has weaker mechanical properties when compared with traditional zirconia.11
Classification by Fabrication Method
Ceramics can also be classified based on the technique used to fabricate them. There are a variety of processing techniques that can be used, including the following3:
• Powder/liquid (Powder Condensation) systems. In the conventional method, ceramic is created by adding porcelain paste manually and sintering it in the furnace. During this process, the ceramic is condensed because of the fusion of the powder, and this is accompanied by an approximately 25% loss of volume of the whole material.2 In the slip casting method, a slurry of ceramic powder is first applied to a refractory die and then condensed. Next, the refractory die is sent to the furnace for the ceramic powder to be sintered, and the result is a sponge-like, porous matrix of ceramic. Lastly, lanthanum glass is infiltrated into this matrix, and it is sent back to the furnace for a second firing.
• Pressable systems. For pressable restorations, a wax-up is performed, and then a phosphate-bonded investment mold is produced using the lost-wax technique. Ceramic ingots are brought to high temperatures, then the softened ceramic is injected into the mold under pressure.
• CAD/CAM systems.This technique involves either the removal of excess material to fabricate a restoration (ie, subtractive process) or the addition of material to fabricate a restoration (ie, additive process). After the restoration is designed using software, the subtractive process entails milling it out of a block of porcelain in a milling machine, whereas the additive process, electrodeposition, involves the application of an electric current to a conductive die onto which the powder particles are dispersed.
Monolithic or Layered?
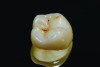
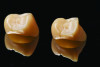
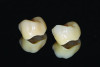
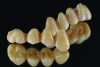
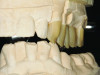
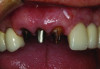
A prosthesis fabricated from one ceramic material, such as feldspathic porcelain, leucite-reinforced ceramic, lithium disilicate, or zirconia (Figure 1), is referred to as a monolithic restoration. However, similar to metal-ceramic restorations, bilayered all-ceramic restorations often consist of a material with stronger mechanical properties as the substructure, which is veneered with more esthetic porcelain to enhance the optical properties of the restoration. In one method of fabricating a bilayered all-ceramic prosthesis, a monolithic restoration is created with a facial cutback design, then glass-ceramics or feldspathic porcelains are veneered onto the facial aspect in order to improve the esthetics (Figure 2 and Figure 3). Another method involves creating a framework or coping from high-strength ceramic, overlaying a ceramic with better optical properties (eg, glass-based ceramic or feldspathic porcelain), then fusing them together. When the framework/coping is made of zirconia, this design is sometimes referred to as porcelain-fused-to-zirconia.12
Factors Affecting Ceramic Fracture
Predictable and successful results in dentistry require a thorough understanding of every step in the course of restoration, from diagnosis and treatment planning to insertion, cementation, and the maintenance phase. For all-ceramic restorations, one of these steps is the material and design selection, which, with inadequate knowledge, can lead to unsatisfactory results.
Pjetursson and colleagues demonstrated in a systematic review that the survival rate of an all-ceramic restoration is around 95%.13 Studies have shown that the most common complications include ceramic fracture, porcelain chipping, and framework fracture.14 In order to achieve high survival rates in our day-to-day practices and to prevent any complications, it is beneficial to understand the factors affecting ceramic fracture when choosing materials. Numerous factors can contribute to ceramic fractures in dentistry, and they can be classified into the following four categories.15
Factors Related to Material Properties
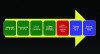
Figure 4 illustrates the order of dental ceramics in terms of flexural strength.3 Although some studies have shown that flexural strength is not as clinically relevant as other material properties,9 it still provides the dentist and the laboratory technician with an idea about the strength of the ceramic, which informs selection of the proper materials. Although zirconia has the highest flexural strength, it cannot always be used monolithically because of its poor optical properties, especially in anterior cases. The other factor that is crucial to consider is CTE. Studies have shown that CTE mismatch in bilayered all-ceramic restorations can lead to technical complications such as chipping or fracture.16
Factors Related to Restoration Design
Regarding the design of the framework and core of all-ceramic restorations, studies have recommended the following:
• The core should be anatomical and at least 0.3 mm to 0.5 mm in thickness.16
• The veneering porcelain should be uniform and 0.5 mm to 0.7 mm in thickness in order to harmonize the cooling rates in the furnace.17,18
• For multiunit all-ceramic fixed dental prostheses, the minimum dimensions of the connector surface area should be 3 mm2 to 4 mm2 x 3 mm2 to 4 mm2 (Figure 5).19
• Dentists should avoid any sharp angles in their tooth preparations, which should have an anatomical, reduced occlusal aspect to make it possible for the laboratory technician to fabricate a uniform anatomical coping/core.
Factors Related to Fabrication
All fabrication techniques for dental ceramics are technique sensitive. Every single step outlined in manufacturers' manuals should be followed to eliminate the potential for errors and defects in the prosthesis, such as porosities.
Miscellaneous Factors
Other factors affecting the potential fracture of all-ceramic restorations include those involving occlusion, internal fit, and parafunction. A thorough understanding and diagnosis of patients' occlusion and occlusal scheme can lead to a more durable prosthesis. Regarding internal fit, studies have shown the importance of having less than 70 μm in all-ceramic crowns in order to increase their fracture resistance.20 In addition, parafunctional habits such as bruxism or clenching are risk factors for fracture, and monolithic all-ceramic prostheses are recommended for these patients.4
Selection Criteria
Considering the variety of materials and designs, dentists now have many options for all-ceramic restorations. In order to achieve a predictable, durable result, several factors need to be considered when selecting ceramic materials, including the following:
• Occlusion. Evaluating the patient's occlusion and the occlusal scheme is important in both restorative dentistry and prosthodontics. Eliminating any occlusal interferences in excursive movements and adjusting the occlusion with the design of new prostheses can lead to more durable outcomes. When fabricating monolithic prostheses with facial cutbacks, no occlusal contact should be designed at the interface between porcelains for maximum intercuspation position and excursive movements (Figure 6).21
•
Substrate. The nature of the substrate that remains after tooth preparation is an important factor for veneers. Dentin has a lower flexural strength than enamel; therefore, cementing glass ceramics or feldspathic veneers is riskier on dentin.4 Because of this, it cannot act as a solid infrastructure for the ceramic, and ceramic with a higher crystalline phase content is recommended in these cases. Furthermore, the bond strength that can be achieved with dentin is weaker than that of enamel, making enamel a better substrate for veneers.
• Stump shade. In the aforementioned classification by microstructure, the translucency of the material decreases as the percentage of the crystalline phase increases. The stump shade should always be considered during material selection for all-ceramic restorations and should always be selected using a stump shade guide. Knowing the stump shade helps the dental technician mask it for better shade matching (Figure 7).
• Esthetics. In esthetic cases, selecting ceramics from among the polycrystalline solids is not recommended. The lack of a glassy phase in these ceramics makes them look unnatural; therefore, selecting a material with greater translucency or using a bilayered design is more suitable.
• Axial reduction and abutment height. When preparing short teeth for any dental prostheses, ceramics with thinner optimum thicknesses (eg, high strength ceramics) should be selected. This is done in order to preserve tooth structure for retention and resistance of the prosthesis. Designing boxes/grooves on these teeth is indicated to enhance these features.22
• Tooth position. Because the mandible acts as a class 3 lever, the posterior teeth are under higher occlusal forces than the anterior teeth.23 Therefore, selecting stronger ceramics in cases involving posterior teeth is recommended.4
• Opposing material. When selecting materials for all-ceramic restorations, the material opposing the prosthesis should always be considered. Having an opposing removable prosthesis will reduce the risk of any complications for an all-ceramic restoration. Alternatively, for cases involving a fixed prosthesis in the opposing jaw, dental ceramics with higher flexural strengths should be considered. In addition to the strength of the material, the surface roughness should also be taken into account. Studies have shown that polished ceramics result in less wear to the opposing material when compared with glazed ceramics and that polished zirconia is the most wear-friendly of all of the ceramics.24
• Parafunctional habits. Diagnosing parafunctional habits should always be a part of the treatment planning process, and in these cases, selecting monolithic lithium disilicate or zirconia restorations is recommended over bilayered restorations.4 Fabricating an occlusal guard for patients with parafunctional habits also helps to significantly reduce the risk of fracture in all-ceramic restorations.25
Conclusion
Having a complete knowledge of the various ways that dental ceramics can be classified helps technicians and dentists to fully understand the differences in the properties of these materials, their benefits and drawbacks, and when one is better indicated for a case than another. When the most appropriate ceramic restorative material is selected in each case, patients experience optimal outcomes that demonstrate long-term function and ideal esthetics.
About the Authors
Siamak Najafi-Abrandabadi, DDS
Clinical Assistant Professor
Department of Prosthodontics
New York University
College of Dentistry
New York, NY
Asim Abdul Quader, BDS
Clinical Fellow
Advanced Programs for International Dentists in Comprehensive Dentistry
New York University
College of Dentistry
New York, NY
Yasmin Raslan Ojjeh, BDS
Student
Advanced Programs for International Dentists in Comprehensive Dentistry
New York University
College of Dentistry
New York, NY
References
1. Taylor JA. History of Dentistry: A Practical Treatise for the Use of Dental Students and Practitioners. Philadelphia, PA: Lea & Febiger; 1922: 148.
2. Helvey GA. Classifying dental ceramics: numerous materials and formulations available for indirect restorations. Compend Contin Educ Dent. 2014;35(1):38-43.
3. Giordano R, McLaren EA. Ceramics overview: classification by microstructure and processing methods. Compend Contin Educ Dent. 2010;31(9):682-684, 686, 688 passim; quiz 698, 700.
4. McLaren EA, Whiteman YY. Ceramics: rationale for material selection. Compend Contin Educ Dent. 2010;31(9):666-668, 670, 672 passim; quiz 680, 700.
5. Lee B, Gadow R, Mitic V. Proceedings of the IV Advanced Ceramics and Applications Conference. Paris, France: Atlantis Press; 2017:100.
6. McLaren EA, Giordano RA. Zirconia-based ceramics: material properties, esthetics, and layering techniques of a new veneering porcelain, VM9. Quintessence Dent Technol. 2005;28:99-111.
7. Fabian Fonzar R, Carrabba M, Sedda M, et al. Flexural resistance of heat-pressed and CAD-CAM lithium disilicate with different translucencies. Dent Mater. 2017;33(1):63-70.
8. Junpoom P, Kukiattrakoon B, Hengtrakool C. Flexural strength of fluorapatite-leucite and fluorapatite porcelains exposed to erosive agents in cyclic immersion. J Appl Oral Sci. 2011;19(2):95-99.
9. McLaren EA, Cao PT. Ceramics in dentistry-part I: classes of materials. Inside Dent. 2009;5(9):94-103.
10. Zhang Y, Lawn BR. Novel zirconia materials in dentistry. J Dent Res. 2018;97(2):140-147.
11. Ghodsi S, Jafarian Z. A review on translucent zirconia. Eur J Prosthodont Restor Dent. 2018;26(2):62-74.
12. Zhang Y, Kelly JR. Dental ceramics for restoration and metal veneering. Dent Clin North Am. 2017;61(4):797-819.
13. Pjetursson BE, Brägger U, Lang NP, Zwahlen M. Comparison of survival and complication rates of tooth-supported fixed dental prostheses (FDPs) and implant-supported FDPs and single crowns (SCs). Clin Oral Implants Res. 2007;18(Suppl 3):97-113.
14. Pieger S, Salman A, Bidra AS. Clinical outcomes of lithium disilicate single crowns and partial fixed dental prostheses: a systematic review. J Prosthet Dent. 2014;112(1):22-30.
15. Zahran MH. Factors Affecting the Fracture Strength and Fatigue Resistance of Molar Crowns Produced Using a Zirconia-based System. [doctoral thesis]. Toronto, Ontario: University of Toronto; 2013.
16. Rekow ED, Silva NR, Coelho PG, et al. Performance of dental ceramics: challenges for improvements. J Dent Res. 2011;90(8):937-952.
17. Guazzato M, Walton TR, Franklin W, et al. Influence of thickness and cooling rate on development of spontaneous cracks in porcelain/zirconia structures. Aust Dent J. 2010;55(3):306-310.
18. Benetti P, Pelogia F, Valandro LF, et al. The effect of porcelain thickness and surface liner application on the fracture behavior of a ceramic system. Dent Mater. 2011;27(9):948-953.
19. Mahmood DJ, Linderoth EH, Vult Von Steyern P. The influence of support properties and complexity on fracture strength and fracture mode of all-ceramic fixed dental prostheses. Acta Odontol Scand. 2011;69(4):229-237.
21. Liu Y, Shen JZ. Advanced Ceramics for Dentistry. 1st ed. Ch. 5: Clinical Failures of Ceramic Dental Prostheses. Oxford, UK: Butterworth-Heinemann; 2013.
22. Sharma A, Rahul GR, Poduval ST, et al. Short clinical crowns (SCC) - treatment considerations and techniques. J Clin Exp Dent. 2012;4(4):e230-e236.
23. Ruiz JL. The three golden rules occlusion. Dent Today. 2010;29(10):92-93.
20. Tuntiprawon M, Wilson PR. The effect of cement thickness on the fracture strength of all-ceramic crowns. Aust Dent J. 1995;40(1):17-21.
24. Sripetchdanond J, Leevailoj C. Wear of human enamel opposing monolithic zirconia, glass ceramic, and composite resin: an in vitro study. J Prosthet Dent. 2014;112(5):1141-1150.
25. Koenig V, Vanheusden AJ, Le Goff SO, Mainjot AK. Clinical risk factors related to failures with zirconia-based restorations: an up to 9-year retrospective study. J Dent. 2013;41(12):1164-1174.