You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Splint therapy can be a major source of frustration. Many dentists question how something so seemingly simple can be so difficult and unpredictable. Oftentimes, dentists feel conflicted about what type of appliance to prescribe. They are unsure if they are making a night guard, a testing device, or just something to give a patient when they are uncertain about what to do but know that they need to do something. There are questions about how it should be designed and fabricated as well as the issues of patient comfort and compliance. Factor in the potential for confusion regarding the goals of splint therapy and the length of treatment required, and it can become even more frustrating. Peter E. Dawson, DDS, the founder of the Dawson Academy, suggests that "in spite of its popularity as the most common treatment for orofacial pain related to temporomandibular joint (TMJ) disorders, splint therapy is still considered by many as a ‘mysterious treatment' that no one really understands."
The reality is that appropriate splints do work. A properly fabricated splint can reduce clicking and popping in the TMJs, decrease joint and muscle pain, and increase the range of motion.1 Unfortunately, splints can also make a patient's condition worse when the wrong appliance is prescribed or when it is improperly designed.2 In order to prescribe the correct type of orthotic splint, it is incumbent upon the clinician to perform a complete examination, including the following3-5:
• Oral, medical, and dental history (focused on joint, muscle, and occlusal history)
• Palpation and evaluation of the muscles of mastication6
• Evaluation of range of motion
• Centric relation load test
• Doppler auscultation
• Evaluation of the dentition for wear, migration, and mobility
• Cone-beam computed tomography or magnetic resonance imaging (if deemed clinically necessary)
This complete examination will help the clinician make a differential diagnosis regarding the TMJ, which could be affected by an intracapsular issue, occluso-muscular issue, or other issue (eg, trigeminal neuralgia, medical/systemic, other pathosis, psychologic, etc). The diagnostic flow must follow the appropriate path of a complete examination in order to lead to a differential diagnosis. This diagnosis will then lead to the appropriate splint therapy. And the results of the splint therapy will then lead to a definitive occlusal and restorative treatment plan. For most patients, splint therapy is the beginning of treatment, not the end of treatment. Splint therapy is not a treatment plan; it is a part of a treatment plan. Making a patient dependent on a piece of plastic should not be the goal.
Splints fall into two basic categories. Per-missive splints allow the unrestricted movement of the mandible against the appliance. Most splint therapy that is provided falls into this category. Directive splints are appliances that will direct the mandible into a predetermined position. These types of appliances should be used with great caution and only for very limited periods of time. Permanent occlusal changes can occur with the use of improper directive splint therapy. An anterior positioning device, which moves the mandible into a position that is anterior to maximum intercuspation, is an example of a directive splint.
Treating Intracapsular Issues
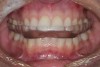
The primary splint used to treat an intracapsular problem is a superior repositioning splint (SRS), which is also known as a centric relation splint (Figure 1). These are full coverage permissive splints that can be made to cover the maxillary or the mandibular teeth. The goal of this appliance is to, in a reversable manner, meet Dawson's five requirements of occlusal stability:
1. Stable holding stops on each tooth in centric relation (With an SRS, this will be as close to centric relation as possible. The goal of SRS therapy is to have TMJs that are capable of full loading with bimanual manipulation without tension or tenderness.)
2. Anterior guidance in harmony with the envelope of function
3. Immediate disclusion of the posterior teeth in protrusion
4. Immediate disclusion of the balancing side during excursion toward the midline
5. Disclusion of all teeth on the working side with the anterior guidance7
Centric relation is the only condylar position that allows an interference-free occlusion. When the condyle disc assembly is in its most superior and axial braced position in the glenoid fossa, the mandible and the maxilla are in centric relation. In this position, the center of force is on the medial pole of the condyle.8
Fabricating an SRS
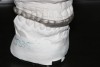
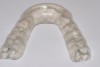
An SRS must be fabricated utilizing facebow-mounted high-quality impressions or digital scans. For the splint to fit the occlusion correctly, the 3D orientation of the maxilla and the condylar axis of rotation must be recorded (Figure 2). The lower model should be mounted as close to centric relation as possible. To provide separation of the posterior teeth in excursive movements, an SRS should be as thin as possible and created with anterior contour. It should also be smooth, fit passively, and not rock on the dentition.9
Expectations and Goals
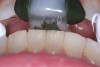
At the delivery appointment, the splint must be equilibrated to allow for even, stable contacts and to ensure that there are no posterior interferences in excursive movements. As the joints stabilize and the condyles seat into the adapted centric posture, the splint will need to be further equilibrated. This will be evident when the patient begins to occlude first with the distal aspects of the splint (Figure 3). This is normal and a sign of positive treatment progress. Some patients will also experience the formation of a pseudo-disc over the head of the condyle. A pseudo-disc forms when undifferentiated mesenchymal cells in the joint space differentiate into chondrogenic and adipogenic cells and create a "callus" over the condylar head.10
Patients can expect to wear an SRS for 20 or more hours a day. Although the treatment takes an average of 3 to 6 months to complete, it is also not uncommon to see improvement in less time or for improvement to take longer than 6 months. In addition to maintaining compliance with wearing the orthotic splint, patients should be encouraged to maintain a softer diet to reduce inflammation in the TMJs, drink plenty of water and eat healthy food, get 8 hours of sleep each night, increase exercise, reduce or eliminate smoking and alcohol consumption, and engage in positive self-talk. Following these guidelines will promote a healing environment for the body to allow adaptation in the TMJs.
The goals of SRS treatment include the following11,12:
• Relief of joint and muscle symptoms, including headache
• Reduction of inflammation in the joints
• Formation of a pseudo-disc
• Decrease in loading of the joints
• Increase in synovial fluid production
• Evaluation of a reversible perfected occlusion
• Reduction of bruxism and parafunction
• Alteration of patient behavior
• Increase in range of motion
Once the joints have been stabilized, which means that the symptoms have resolved and they can be load tested, it is time to correct the underlying issues that ultimately resulted in the need for splint therapy. "Splint therapy is not a cure for occlusal disharmony," emphasizes Dawson. "The common practice of removing the splint without correcting the occlusion is counterproductive because the original cause of the problem is still present. In time, the uncorrected occlusal interferences will reactivate the problems. The next proper step is to correct the occlusion."
Treating Occluso-Muscular Issues
The most effective way to treat occluso-muscular issues is with a permissive splint that is designed to be a segmental deprogramming device (eg, Lucia Jig, Great Lakes Dental Technologies [Figure 4]; NTI-tss™, National Dentex Labs; QuickSplint®, Orofacial Thera-peutics [Figure 5]). Segmental deprogrammers are short-term or intraoffice devices. Because they are segmental, they cannot be worn for more than 6 to 8 hours a day without the risk of tooth drifting or eruption; however, these devices are excellent tools to help make a differential diagnosis of intracapsular or occluso-muscular issues.
Deprogrammers are highly effective because they separate the posterior dentition. When the posterior teeth are not touching, the elevator muscles shut down by approximately 70% to 80%.13 These periods of relaxation can greatly reduce inflammation and lactic acid buildup in overused/hypertrophic muscles.14
For long-term deprogramming, a different device must be prescribed that permits usage for more than 8 hours a day without creating the potential for tooth drifting or eruption. A dual arch B-splint (Figure 6) is the full-coverage permissive device that is recommended for long-term deprogramming. With a B-splint, both arches are covered with what are essentially rigid orthodontic retainers. The anterior segments have opposing flat plane tables, so when the patient closes his or her mouth, the back teeth stay separated. And because the back teeth stay separated and the only contact is on the flat planes, when the patient slides into excursive movements, there is little resistance. This is why the dual arch B-splint is also an excellent appliance for bruxers.
Patients should discontinue usage if they experience any discomfort and report this to the clinician. Temporary bite changes are to be expected in the mornings, and practitioners should exercise caution when using a deprogramming device in patients with large centric relation/maximum intercuspation interferences.
Fabricating and Delivering a B-Splint
High-quality impressions or scans are all that is required for the laboratory to fabricate a B-splint. Because the occlusion will be open, there is no need for facebow records.At delivery, the clinician should ensure a passive fit of both arches. The patient must move his or her mandible into extreme protrusive and lateral excursive movements to ensure that there is no contact of the splint on the molars. This is a critical step that should not be overlooked. If the patient's second molars experience contact in the B-splint, then the muscles of mastication will still be active (Figure 7).
Discussion
One popular trend is the fabrication of soft and hard/soft splints. Soft splints are popular because they can be easily and economically fabricated right in the office. Hard/soft splints utilize a soft material on the intaglio surface and a hard material on the occluding surface. These splints are popular because they rarely demonstrate issues with fitting over the teeth; however, clinicians should not be fooled into thinking that they can produce beneficial results for patients. In fact, research has shown that compressible splints will often increase muscle function, having the exact opposite effect of the intended result.15,16
In conclusion, the astute clinician will administer a complete examination to ensure that the appropriate splint appliance is being prescribed in each case. He or she must understand the goals of appliance therapy as well as the long-term treatment to restore the occlusal harmony that will follow. In addition, the clinician should not lose sight of the presence of other nondental issues, such as neuropathoses, central nervous system issues, soft- or hard-tissue pathoses, psychologic factors, and pain disorders, to name a few. When a complete examination is performed and a differential diagnosis is made, splint therapy can become a predictable and efficacious form of treatment.
Queries regarding this course may be submitted to authorqueries@aegiscomm.com
About the Author
Leonard A. Hess, DDS
Senior Faculty
The Dawson Academy
St. Petersburg, Florida
Private Practice
Monroe, North Carolina
References
1. Sletten WO, Taylor LP, Goodacre CJ, Dumont TD. The effect of specially designed and managed occlusal devices on patient symptoms and pain: a cohort study. Gen Dent. 2015;63(2):46-52.
2. Fricton J, Look JO, Wright E, et al. Systematic review and meta-analysis of randomized controlled trials evaluating intraoral orthopedic appliances for temporomandibular disorders. J Orofac Pain. 2010;24(3):237-254.
3. Dawson PE. Differential diagnosis of temporomandibular disorders. In: Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007:259-264.
4. Dawson PE. Occluso-muscle disorders. In: Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007:265-276.
5. Dawson PE. Intracapsular disorders of the TMJ. In: Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007:277-306.
6. Haley D, Schiffman E, Baker C, Belgrade M. The comparison of patients suffering from temporomandibular disorders and a general headache population. Headache. 1993;33(4):210-213.
7. Williamson EH, Lundquist DO. Anterior guidance: its effect on electromyographic activity of the temporal and masseter muscles. J Prosthet Dent. 1983;49(6):816-823.
8. Dawson PE. Occlusal disease. In: Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007:17-26.
9. Conti PC, dos Santos CN, Kogawa EM, et al. The treatment of painful temporomandibular joint clicking with oral splints: a randomized clinical trial. J Am Dent Assoc. 2006;137(8):1108-1114.
10. Lavi A, Pelled G, Tawackoli W, et al. Isolation and characterization of mesenchymal stromal progenitors from the temporomandibular joint disc. J Tissue Eng Regen Med. 2017;11(5):1553-1561.
11. Tsuga K, Akagawa Y, Sakaguchi R, Tsuru H. A short-term evaluation of the effectiveness of stabilization-type occlusal splint therapy for specific symptoms of temporomandibular joint dysfunction syndrome. J Prosthet Dent. 1989;61(5):610-613.
12. Kreiner M, Betancor E, Clark GT. Occlusal stabilization appliances. Evidence of their efficacy. J Am Dent Assoc. 2001;132(6):770-777.
13. Mansour RM, Reynik RJ. In vivo occlusal forces and moments: I. Forces measured in terminal hinge position and associated moments. J Dent Res. 1975;54(1):114-120.
14. Shinogaya T, Kimura M, Matsumoto M. Effects of occlusal contact on the level of mandibular elevator muscle activity during maximal clenching in lateral positions. J Med Dent Sci. 1997;44(4):105-112.
15. Fricton J, Look JO, Wright E, et al. Systematic review and meta-analysis of randomized controlled trials evaluating intraoral orthopedic appliances for temporomandibular disorders. J Orofac Pain. 2010;24(3):237-254.
16. Okeson JP. The effects of hard and soft occlusal splints on nocturnal bruxism. J Am Dent Assoc. 1987;114(6):788-791.