You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
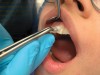
Ironically, practitioners currently use relatively low-tech instruments (eg, cold/hot tests, electric pulp testing [EPT]) for sensibility testing to derive complex pretreatment pulpal diagnoses (Figure 1). By definition, sensibility refers to the ability to respond to a stimulus. Thermal and electric pulp tests are considered sensibility tests because they assess the pulp's nerve response to a stimulus. One problem with our current sensibility testing techniques is that they sometimes provide inaccurate results when assessing the real time status of the pulp tissue's state of health.1
Alternatively, pulp vitality is a direct assessment of pulpal blood flow.1 Pulp vitality testing can be performed using laser Doppler flowmetry (LDF) or pulse oximetry. The difference between LDF and pulse oximetry is that a laser Doppler instrument measures pulpal blood flow, whereas a pulse oximeter measures the oxygen saturation of the blood.2,3 LDF and pulse oximetry are not used in clinical endodontics for pulpal diagnosis because of their limitations.
LDF's limitations for determining pulpal blood flow include its inability to measure blood flow in absolute units and the fact that extraneous noise or movement in or near the unit can affect its performance. Another major clinical problem with adapting LDF for endodontic diagnosis is the limited ability of its laser to penetrate the mineralized tooth tissue.2
Regarding the use of a pulse oximeter, the sensors need to conform to the size, shape, and anatomy of a tooth such that the light-emitting diodes and the photodetector are parallel to each other in order to obtain an accurate blood oxygenation level.3 Similar to LDF, another major clinical limitation of a pulse oximeter is its ability to obtain an accurate reading through the mineralized tissue of a tooth.
Pulpal Nerve Types
The pulpal nerve fibers (eg, A-delta fibers and C fibers) are nociceptors, which are sensory receptors that respond to stimuli by sending nerve signals to the brain. A-delta fibers respond to cold stimuli and EPT, and C fibers respond to hot stimuli. These stimuli can cause the perception of pain in an individual.4
A-delta fibers, which are myelinated nerves that have a fast conduction speed and low stimulation threshold, are located in the pulp-dentin junction. They generate a sharp, stabbing, localized type of pain.5 C fibers, which are unmyelinated nerves with a slow conduction speed and high stimulation threshold, are located throughout the central region of the pulp. They generate a dull aching, burning type of pain.5 A-delta fibers also differ from C fibers in their lack of ability to maintain functionality in a hypoxic (ie, low oxygen) environment. The reason for this is that oxygen consumption is higher in the thicker A-delta fibers when compared with the thinner C fibers.6
Sensibility Testing
Regarding thermal testing and EPT, thermal testing depends on the outward and inward movement of the dentinal fluid within the dentinal tubules, whereas EPT depends on the ionic movement.7 Pulpal nerves do not have thermosensing nerve endings; therefore, the thermal pain response of a patient's tooth is explained by the hydrodynamic theory.8 Based on this theory, when cold is applied to a tooth, there is an outward movement of the dentinal fluid (ie, contraction of fluid), which produces a response from the A-delta fibers. Conversely, when heat is applied to a tooth, there is an inward dentinal fluid movement, which elicits the firing of the C fibers.5 Because thermal tests require the dentinal tubules to be open enough to allow fluid to flow according to the hydrodynamic theory, these tests may not be effective in elderly patients, who are more likely to have teeth with closed tubules and substantial secondary dentin formation.1
When performing EPT, a positive response from the A-delta fibers is due to an ionic shift in the dentinal tubules that causes local depolarization and the subsequent creation of an action potential from an intact A-delta fiber.9 It is important to note that C fibers do not respond to EPT because a higher amount of electrical stimulation is required to activate these pulpal nerve fibers.10
When a dentist performs pulp sensibility tests on a patient's tooth to obtain a pretreatment pulpal diagnosis and the tooth does not respond to cold or electrical stimuli, the clinician should still administer local anesthesia prior to performing endodontic treatment. The reason for this is that, although the A-delta fibers have degenerated, the C fibers may still be responsive, especially if the patient reports sensitivity to hot foods or liquids or has a history of unprovoked (ie, spontaneous) pain from the tooth to be treated.5
Another clinical scenario that merits discussion is when a dentist repeatedly performs cold testing on a tooth during a short period of time, which can reduce the displacement rate of the fluids inside the dentinal tubules, thus causing a less painful response.5 This refractory period following the attempted repeated nerve stimulation with cold could possibly lead a clinician to make an incorrect pretreatment pulpal diagnosis. Therefore, when retesting a tooth's response to a cold stimulus is necessary, it is important for the dentist to wait a few minutes before reapplying the cold stimulus to the tooth.
Diagnostic Terminology
When using the current sensibility testing methods (eg, cold/hot tests, EPT) on a tooth, the following pulpal diagnoses can be obtained11:
Normal pulp. These pulps test within normal limits to cold. Clinically, a patient with normal pulp will respond to a cold stimulus; however, after this stimulus is removed, the cold sensation will dissipate immediately. It should be noted that the time it takes for a patient to respond to cold has no correlation to the diagnosis and therefore does not need to be recorded.
Reversible pulpitis. This diagnosis refers to pain from an inflamed pulp that can be treated without the removal of the pulp tissue. This is not a state of disease but a symptom. A classic clinical sign of reversible pulpitis is a sharp, quick pain that subsides as soon as the stimulus is removed. Reversible pulpitis does not elicit an unprovoked response.
Symptomatic irreversible pulpitis. Pulps with symptomatic irreversible pulpitis are inflamed and cannot be treated except by the removal of the pulp tissue. Classic clinical symptoms include lingering sensations from cold/hot stimuli that last longer than 5 seconds and patient reports of spontaneous or referred (ie, occurring at a site that is different from its origin) tooth pain.
Asymptomatic irreversible pulpitis. This diagnosis refers to a vital pulp that is incapable of healing but for which endodontic treatment is indicated. Clinically, this presents as a carious tooth that is asymptomatic and responds within normal limits to cold.
Pulp necrosis. A necrotic pulp can result from untreated irreversible pulpitis or immediately follow a traumatic injury that disrupts the pulpal vasculature. A necrotic pulp does not respond to cold and heat testing or EPT.
The last time pulpal diagnostic terminology was updated was at the American Association of Endodontists (AAE) Consensus Conference in 2008.12 At the time that this terminology was published, there was not as good of an understanding of the correlation between pulp histology and clinical diagnosis being reported in the endodontic literature as there is today. During the last 5 years, the scientific and material advancements in the field of endodontics have led to a better understanding of the histologic and diagnostic assessment of inflamed pulp tissue.
A recent study by Ricucci and colleagues13 found that 96.6% of the clinical pulpal diagnoses of normal pulp or reversible pulpitis matched the histologic diagnoses of the pulp tissue of the teeth, as compared with the clinical pulpal diagnoses of irreversible pulpitis, which only had an 84.4% correlation to the histologic diagnoses of the pulp tissue. This study noted that bacterial invasion of the pulp tissue was common in teeth diagnosed with irreversible pulpitis but absent in teeth diagnosed with normal pulps or reversible pulpitis.
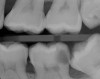
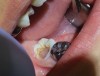
These findings demonstrate that the pulpal diagnostic term asymptomatic irreversible pulpitis needs to be updated. This diagnosis represents a tooth that presents with clinical and radiographic evidence of caries (Figure 2) and responds normally to clinical sensibility testing to cold. The AAE Consensus Conference Recommended Diagnostic Terminology defines asymptomatic irreversible pulpitis as "a clinical diagnosis based on subjective and objective findings indicating that the vital inflamed pulp is incapable of healing. Additional descriptors: no clinical symptoms but inflammation produced by caries, caries excavation, trauma."12 In reality, this diagnosis can technically only be confirmed histologically. But, according to the results of the study conducted by Ricucci and colleagues13, teeth that responded normally to cold testing demonstrated only a mild to moderate accumulation of chronic inflammatory cells beneath the tubules that were affected by caries, and the inflammation did not extend through the entire portion of the pulpal tissue. Therefore, the pulp of a carious tooth that responds normally to cold testing should be diagnosed as normal pulp, not asymptomatic irreversible pulpitis. A more pertinent use of the diagnostic term asymptomatic irreversible pulpitis would be for cases involving a pulp polyp or internal resorption of a vital tooth (Figure 3).
A New Paradigm
In a recent article by Wolters and colleagues, the authors recommended changing the pulpal diagnostic terminology to use the terms initial, mild, moderate, and severe pulpitis.14 This article also noted that in cases involving a diagnosis of irreversible pulpitis, the diagnosis may not necessarily correspond to an irreversible state of inflammation of the entire pulp and is limited only to the pulp chamber. In further support of the need for updated diagnoses and definitions, a study on vital pulp therapy by Awawdeh and colleagues concluded that a better understanding of the healing potential of the dental pulp has created the necessity for revision of the current pulpal disease terminology.15
With today's better understanding of the clinical correlation between pretreatment pulpal diagnosis and actual pulpal status, the endodontic treatment methodology has changed. Depending on the extent of inflammation and infection, pulp tissue can now be treated with vital pulp cryotherapy or regenerative endodontics.16,17 It is this updated didactic and clinical knowledge that has become the catalyst driving the movement to change the current endodontic diagnosis and treatment terminologies to best reflect the current understanding of pulp biology.
An updated system of pulpal diagnostic terminology could include the following terms:
Normal pulp. No hyper-response or lingering pain to hot or cold sensibility tests.
Pulpitis. Hyper-response to hot or cold tests, but it is non-lingering.
Acute pulpitis. Hyper-response to hot or cold tests along with lingering (ie, beyond 5 seconds) pain from the hot or cold stimuli and/or reporting of spontaneous pain.
Necrotic pulp. No response to cold, hot, and/or electric sensibility tests.
Proposed new pulpal treatment terminology could include the following:
Pulp cap. No removal of pulp tissue during vital pulp treatment.
Partial pulpectomy. Removal of all or a portion of the coronal pulp during vital pulp treatment.
Full pulpectomy. Removal of the entire pulp tissue (ie, coronal and radicular pulp) during conventional endodontic treatment.
Conclusion
It is important to note that the updated diagnostic and treatment terminologies proposed here are only a recommendation based on the current evidence-based endodontic literature. Until such a time that these or a variation of these diagnosis and treatment terminologies are accepted and reported in the literature by the AAE, readers should continue to use the official AAE Consensus Conference Recommended Diagnostic Terminology12 as presented in this article.
About the Authors
James Bahcall, DMD, MS
Clinical Professor
Department of Endodontics
University of Illinois at Chicago
College of Dentistry
Chicago, Illinois
Qian Xie, DDS, PhD
Assistant Professor
Department of Endodontics
University of Illinois at Chicago
College of Dentistry
Chicago, Illinois
Mark Baker, DDS
Clinical Associate Professor
Department of Endodontics
University of Illinois at Chicago
College of Dentistry
Chicago, Illinois
Steve Weeks, DDS
Clinical Assistant Professor
Department of Endodontics
University of Illinois at Chicago
College of Dentistry
Chicago, Illinois
References
1. Jafarzadeh H, Abbott PV. Review of pulp sensibility tests. Part I: general information and thermal tests. Int Endod J. 2010;43(9):738-762.
2. Jafarzadeh H. Laser Doppler flowmetry in endodontics: a review. Int Endod J. 2009;42(6):476-490.
3. Jafarzadeh H, Rosenburg P. Pulse oximetry: review of a potential aid in endodontic diagnosis. J Endod. 2009;35(3):329-333.
4. Mattscheck D, Law AS, Nixdorf DR. Diagnosis of nonodontogenic toothache. In: Hargreaves KM, Cohen S, eds. Cohen's Pathways of the Pulp. 10th ed. St. Louis, MO: Mosby; 2011:49-70.
5. Jain N, Gupta A, N M. An insight into neurophysiology of pulpal pain: facts and hypotheses. Korean J Pain. 2013;26(4):347-355.
6. Närhi MV. The characteristics of intradental sensory units and their responses to stimulation. J Dent Res. 1985;64 Spec No:564-571.
7. Bender IB. Pulpal pain diagnosis--a review. J Endod. 2000;26(3):175-179.
8. Cohen S, Hargreaves KM. Pathways of the Pulp. 9th ed. St. Louis: Mosby; 2006.
9. Pantera EA Jr, Anderson RW, Pantera CT. Reliability of electric pulp testing after pulpal testing with dichlorodifluoromethane. J Endod. 1993;19(6):312-314.
10. Närhi M, Virtanen A, Kuhta J, Huopaniemi T. Electrical stimulation of teeth with a pulp tester in the cat. Scand J Dent Res. 1979;87(1):32-38.
11. Glickman GN. AAE consensus conference on diagnostic terminology: background and perspectives. J Endod. 2009;35(12):1619-1620.
12. American Association of Endodontists. AAE consensus conference recommended diagnostic terminology. American Association of Endodontists website. https://www.aae.org/specialty/wp-content/uploads/sites/2/2017/07/aaeconsensusconference
recommendeddiagnosticterminology.pdf. Published December 2009. Accessed November 12, 2019.
13. Ricucci D, Loghin S, Siqueira JF Jr. Correlation between clinical and histologic pulp diagnoses. J Endod. 2014;40(12):1932-1939.
14. Wolters WJ, Duncan HF, Tomson PL, et al. Minimally invasive endodontics: a new diagnostic system for assessing pulpitis and subsequent treatment needs. Int Endod J. 2017;50(9):825-829.
15. Awawdeh L, Al-Qudah A, Hamouri H, Chakra RJ. Outcomes of vital pulp therapy using mineral trioxide aggregate or biodentine: a prospective randomized clinical trial. J Endod. 2018;44(11):1603-1609.
16. Bahcall J, Xie Q, Baker M, Weeks S. New approach in endodontics: cryotherapy for vital pulp treatment. Decisions in Dentistry website. https://decisionsindentistry.com/article/cryotherapy-vital-pulp-treatment/. Updated October 16, 2019. Accessed November 12, 2019.
17. Bahcall J, Xie Q, Baker M, et al. Bioactive endodontics for mature permanent teeth. Inside Dentistry. 2019;15(8):43-46.