You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
In the field of dental medicine and laboratory technology, photography has long been an essential means of documenting, diagnosing, and communicating clinical findings.1-4 The most prevalent devices currently utilized by dentists to achieve these ends are the compact digital camera and digital single lens reflex (DSLR) camera.1,5 Despite the obvious utility of a digital camera as an integral part of the dental practitioner's armamentarium, several surveys within the literature have consistently demonstrated that the majority of dentists do not use photography as a tool in their daily practice. A few of the most relevant reasons cited for not using photography are the high cost of the equipment, the additional training required, and the poor return on investment.1,5,6 These factors, coupled with the integration of digital photography into the cellular phone during the last two decades, have led to an increased prevalence of mobile camera technology within the operatory.7
Smartphone dental photography is inherently convenient, easy to use, and facilitates real-time collaboration with colleagues-all features that make the routine protocols of photographic record keeping less of a hurdle to overcome when compared with the use of a DSLR camera system. However, these advantages are not without technical drawbacks. The most salient disadvantage of smartphone dental photography is the lack of sufficient and appropriate native light output, which is a shortcoming that renders many of the images obtained from contemporary mobile devices inadequate for accurate and effective case documentation.
Ingredients for Good Dental Photography
At the high end of professional dental photography, the images produced by DSLR cameras represent the benchmark for dentists and laboratory technicians alike. Most DSLR cameras possess a modular component system, allowing for a wide variety of interchangeable lenses (Figure 1) and dedicated lighting setups (Figure 2). The flexible nature of DSLR cameras allows for greater creative freedom regarding object illumination and varied focal lengths that are tailored to the desired depth of field.8 In addition, the larger sensors built into DSLR cameras impart improved fidelity to the colors rendered and an increased resolution of the subject being photographed. In combination, these features ultimately produce exceptional results.3,9
Achieving a properly exposed photograph requires mastering the dynamic interplay of various camera settings and lens parameters because small adjustments to any one single factor will affect the others. These factors, which include shutter speed, ISO (Short for the Greek word isos, ISO is an International Organization for Standardization measure of how sensitive a camera's digital sensor is to light), and aperture, are collectively referred to as the "exposure triangle" and have been discussed in great detail elsewhere.10,11 When endeavoring to photograph the human dentition, the well-established principle of the exposure triangle fails due to the dearth of ambient light present in the narrow and restricted confines of the oral cavity. In 1952, Lester Dine recognized and addressed this limitation by developing an external light source that attached to a macro lens on the clinician's camera and was specifically designed to provide sufficient illumination throughout the mouth. Dine's invention, which he called the "ring flash" (Figure 3), allowed clinicians to produce consistent and predictable intraoral photographs for the first time.12
The Exposure Diamond
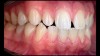
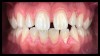
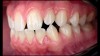
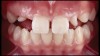
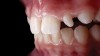
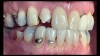
For most dental clinicians and technicians, the acquisition of professional-level photographs with a DSLR camera requires a steep economic investment and possesses a shallow learning curve. The time commitment and nebulous return on investment are certainly potent deterrents to the incorporation of these systems into daily practice. While remaining cognizant of the need for photographic documentation, the dental field has witnessed an increase at the low end of the dental photography continuum through the use of the ubiquitous smartphone as a proxy for the larger and more expensive DSLR camera setups. Most smartphones will allow the user to customize and control the elements of the exposure triangle via the internal camera settings or by means of a third-party application (Figure 4); however, the diminutive nature of the lenses, apertures, and sensors of these devices makes the necessary attainment of light problematic. When this is coupled with low-capacity native light output on the subject being photographed, the resulting images are often distorted, low-resolution, and possess inconsistent reproduction of color and detail, which renders them unacceptable for documenting patient treatment and collaborating with the laboratory (Figure 5 and Figure 6).
Since clinicians began photographing teeth, it has been well-established that the application of the exposure triangle is ill-suited to this particular form of image capture. Alternatively, an "exposure diamond" (Figure 7), in which an external artificial light source (EALS) represents the apex, provides a more appropriate conceptual framework that takes into account the prioritization of focused light output over the other three factors in the exposure triangle.
The Dental Industry Responds to a Need
Paralleling the obstacles that Lester Dine faced nearly 70 years ago, there exists a need within the dental community today for a cost-effective, easy-to-use technology that is specifically tailored to address the limitations of intraoral smartphone photography. In recognition of these shortcomings, several dental companies have developed economical and user-friendly smartphone light attachments that produce consistent and uniform illumination of subjects. These attachments allow the user to overcome the physical limitations of the small internal camera and sensor-rendering the extensive manual modification of shutter speed, ISO, and aperture unnecessary. The addition of a dental specific EALS to a contemporary smartphone ultimately simplifies the operator experience, resulting in a heightened focus on patient care and an elevation of the smartphone dental photography to a level that exceeds the current threshold for acceptable standards of clinical documentation.
Application of Smartphone Dental Photography
Today, the myriad uses for dental photography span the gamut from academia to art. The following examples do not represent an exhaustive list of the possible applications for smartphone dental photography, but rather, they serve to illustrate how smartphones are rapidly becoming an indispensable part of the armamentarium for the most common and practical day-to-day clinical and laboratory protocols.
Diagnosis and Routine Treatment Planning
One of the main advantages that smartphone cameras have over DSLR cameras is that nearly everyone is already very familiar with the technology; therefore, the incorporation of these devices into everyday practice does not require learning a new and unfamiliar skill set. The task of producing a series of high-quality clinical photographs for routine examinations (Figure 8), esthetic treatment planning (Figure 9 through Figure 11), or specialty care (Figure 12 and Figure 13) can be delegated with confidence to any staff member during the patient's initial office visit and will generally require less than 5 minutes of time to complete. When a DSLR camera is used, evaluation of the intraoral images either takes place on the small viewfinder built into the camera or necessitates the physical removal of the memory card from the camera to downloaded the images onto a computer for review. An added bonus of smartphone dental photography is that the phone's screen now replaces the much smaller viewfinder of a DSLR camera and provides the clinician with the ability to view and zoom into the patient images on a 5- to 6-inch, high-definition display.
Emergency Care and Referral to Specialists
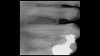
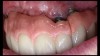
Emergency visits are a common and unpredictable occurrence at nearly all dental practices (Figure 14 and Figure 15). When an emergency occurs, the patient's provider may not always be available to evaluate and initiate treatment. In a similar manner, new patients of record frequently present with oral conditions that require the attention of a dental specialist who may only be available at another clinic (Figure 16 and Figure 17). For many of these patients, immediate access to care may be limited, and if a patient is experiencing discomfort, time will be a critical factor in regard to initiating a proposed plan of action. The use of a smartphone with an EALS can allow the clinical staff to rapidly acquire intraoral photographs or a video and transmit these images and other information via encrypted text message or secure e-mail to anywhere in the world for immediate consultation. The combination of telecommunications and dentistry is known as teledentistry,13which has been shown to impart significant benefits to patients and providers in the fields of oral medicine,14 oral and maxillofacial surgery,15 endodontics,16 prosthodontics,17 periodontics,18 pediatrics,19 orthodontics,20 and oral hygiene.21
Shade Selection and Laboratory Communication
The most utilized intraoral photographs in the field of dentistry are perhaps those that capture shade information (Figure 18 and Figure 19). The analysis of color (ie, value, chroma, hue) in dentistry is a critical step in the fabrication of esthetic indirect restorations, such as all-ceramic crowns and porcelain laminate veneers. The ability to properly communicate this information with the dental laboratory is essential to ensure an appropriate shade match, a reduction in chairtime and overhead, and most importantly, a satisfactory patient experience and treatment outcome. In recent years, the use of polarized light photography as an aid in the shade selection process has become extremely popular. For some EALS devices, special polarizing filters have been specifically designed to fit over the light-emitting portion of the device (Figure 20 and Figure 21). The images produced using polarized light photography demonstrate an elimination or reduction in the specular reflection of hard and soft tissue, resulting in a matte-finish appearance of the dentition and gingiva. These types of photographs aid the ceramist in identifying areas of opacity and translucency, crack lines, hypo- or hypercalcification, and other internal features of the dentition that may not be readily visible without such a filter (Figure 22).
Marketing and Creative Photography
Dentistry is a highly visual healthcare specialty. Annual symposiums, office websites, and peer-reviewed publications are all inundated with gorgeous before and after case photographs as well as images of materials and techniques. The ability of a smartphone equipped with an EALS to document the workflow of relevant patient treatment does not necessarily have to end at the dental chair. Another use for smartphone image capture aided by an EALS is small object product photography (Figure 23 through Figure 25). Some EALS devices also have the ability to facilitate the addition of third-party add-on lenses (Figure 26) to add further innovation to smartphone photography and video recordings. Creative photographs have extraordinary potential for developing a marketable and recognizable brand, attracting new clients, and providing a deeper sense of career-related personal satisfaction.
Smartphone Usage and Patient Privacy Concerns
In 1996, the adoption of the Health Insurance Portability and Accountability Act (HIPAA) placed a mandate on all healthcare providers, including dentists and dental laboratories, to create and implement policies to protect patients' personal health information.22 As the use of smartphones for capturing, storing, and sharing images in clinical dentistry has increased, so too has the potential for the violation of HIPAA guidelines via unencrypted e-mail, text messaging, and social media platforms.23 In order to remain HIPAA compliant, dental offices and laboratories are encouraged to incorporate any of the widely available smartphone applications that address the aforementioned vulnerabilities in the routine dissemination of patient images (Figure 27). Features to look for when selecting an application include consent forms, integration with the electronic health record, user authentication, an audit trail that logs user access to patient information, nonpermanent data storage, an application time-out feature, integrated image and video capture, image annotation, and secure wireless transmission.24 Additional best practice guidelines to minimize the risk of a breach include the use of password protection and data encryption as well as the removal of identifiable information, such as distinguishing facial features, birthmarks, and tattoos from all images.25
Discussion
Clinical and laboratory photographic documentation in dentistry is a well-established practice that informs case documentation, patient education, staff training, medicolegal reporting, marketing, collaboration with colleagues, communication with the laboratory, didactic lessons in academia, and, of course, self-improvement. The DSLR camera currently represents the most common tool that practitioners and technicians use to achieve this end; however, the continued advancement of smartphone cameras and dental-specific EALS devices is causing a sea change in this trend. The potential applications of this emerging shift toward smartphone dental photography present the field of dentistry with a myriad of novel and exciting ways in which to capture, share, and utilize patient images. As the fundamental nature of small object photography requires both substantial ambient light and a large sensor to collect that light in order to be effective, the images produced with smartphone cameras and dental-specific EALS devices will always be challenged to match the images produced by DSLR cameras. For this reason, smartphone dental photography should not be viewed as an absolute replacement for the DSLR camera. Instead, it should be viewed as a unique adjunct and, perhaps, a preferred tool for certain individuals in particular circumstances. Creativity is the only limit.
About the Authors
Miles Reed Cone, DMD, MS, CDT
Fellow
American College of Prosthodontists
Nuance Dental Specialists
Portland, Maine
Cornelia Cone, MA
CEO
Nuance Dental Specialists
Portland, Maine
References
1.Morse GA, Haque MS, Sharland MR, et al. The use of clinical photography by UK general dental practitioners. Br Dent J. 2010;208(1):E1; discussion 14-15.
2.Yoo A. Ten reasons why dental photography should be an essential part of your practice. Dental Economics. 2014(104)9:86-94.
3. Ahmad I. Digital dental photography. Part 2: purposes and uses. Br Dent J. 2009;206(9):459-464.
4. Wander P, Ireland RS. Dental photography in record keeping and litigation. Br Dent J. 2014;217(3):133-137.
5. Uzunov TT, Kosturkov D, Uzunov T, et al. Application of photography in dental practice. J IMAB. 2015:21(1):682-686.
6. Sharland MR, Burke FJ, McHugh S, et al. Use of dental photography by general dental practitioners in Great Britain. Dent Update. 2004;31(4):199-202.
7. Harting MT, DeWees JM, Vela KM, et al. Medical photography: current technology, evolving issues and legal perspectives. Int J Clin Pract. 2015;69(4):401-409.
8. Kalpana D, Rao SJ, Joseph JK, et al. Digital dental photography. Indian J Dent Res. 2018;29(4):507-512.
9. Terry DA, Snow SR, McLaren EA. Contemporary dental photography: selection and application. Compend Contin Educ Dent. 2008;29(8):432-449.
10. Field R. Introduction to clinical digital photography. Int Dent - African Edition. 2017;7(6):70-76.
11. Kozlowski J, Estes M. Getting the perfect photo. Orthodontic Products. 2014;22-25.
12. Glassgold M. How the ring flash changed dental photography. Journal of Cosmetic Dentistry. 2013;29(1):10.
13.Yoshinaga L. The use of teledentistry for remote learning applications. Pract Proced Aesthet Dent. 2001;13(4):327-328.
14. Bradley M, Black P, Nobel S, et al. Application of teledentistry in oral medicine in a community dental service, N. Ireland. Br Dent J. 2010;209(8):399-404.
15. Aziz SR, Ziccardi VB. Telemedicine using smartphones for oral and maxillofacial surgery consultation, communication, and treatment planning. J Oral Maxillofac Surg. 2009;67(11):2505-2509.
16. Brüllmann D, Schmidtmann I, Warzecha K, et al. Recognition of root canal orifices at distance - a preliminary study of teledentistry. J Telemed Telecare. 2011;17(3):154-157.
17. Ignatius E, Perala S, Makela K. Use of videoconferencing for consultation in dental prosthetics and oral rehabilitation. J Telemed Telecare. 2010;16(8):467-470.
18. Rocca MA, Kudryk VL, Pajak JC, et al. The evolution of a teledentistry system within the Department of Defense. Proc AMIA Symp. 1999:921-924.
19. Kopycka-Kedzierawski DT, Bell CH, Billings RJ. Prevalence of dental caries in Early Head Start children as diagnosed using teledentistry. Pediatr Dent. 2008;30(4):329-333.
20. Berndt J, Leone P, King G. Using teledentistry to provide interceptive orthodontic services to disadvantaged children. Am J Orthod Dentofacial Orthop. 2008;134(5):700-706.
21. Summerfelt FF. Teledentistry-assisted, affiliated practice for dental hygienists: an innovative oral health workforce model. J Dent Educ. 2011;75(6):733-742.
22. Pace Brinker S. HIPAA compliance and digital photography with personal mobile devices. Dental Products Report. 2015;49(1):76-80.
23. Dumestre DO, Fraulin FOG. Balancing the need for clinical photography with patient privacy issues: the search for a secure smartphone application to take and store clinical photographs. Plast Surg (Oakv). 2017;25(4):255-260.
24. Landman A, Emani S, Carlile N, et al. A mobile app for securely capturing and transferring clinical images to the electronic health record: description and preliminary usability study. JMIR Mhealth Uhealth. 2015;3(1):e1.
25. Olawoye OA. Clinical photography and video recordings in plastic surgery: beyond patient autonomy and informed consent. Niger J Plastic Surg. 2018;14(1):15-16.
26. Morgan G. Protecting the Patient, Application of HIPAA/PCI in Dentistry. What's in Your Mouth Campaign Website. https://dentallabs.org/protecting-the-patient-application-of-hipaa-pci-in-dentistry/ Published April 5, 2018. Accessed June 3, 2019.