You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The American Dental Association Principles of Ethics and Code of Professional Conduct (ADA Code) lists five fundamental principles that are aspirational goals for the dental profession: patient autonomy, nonmaleficence, beneficence, justice, and veracity.1 The principle of patient autonomy ("self-governance") states that dentists have to respect a patient's right to confidentiality and self-determination. It means that patients must be treated according to their desires, needs, and abilities, within the boundaries of accepted treatment. Also, they should be actively involved in treatment decisions. The principle of nonmaleficence expresses that dentists must "do no harm." The principle of beneficence says that dentists have the duty to promote patients' welfare, delivering competent dental care and taking into consideration patients' needs, desires, and values. The principle of justice means that dentists must treat people fairly, while the principle of veracity means that dentists have an obligation to communicate truthfully and be honest and trustworthy. Although each principle is considered a guidepost, the ADA Code recognizes that these principles might overlap and compete for priority, sometimes needing to be balanced against each other.1
In regard to patient autonomy, dentists are required to obtain informed consent before providing any kind of treatment. Adequate consent can only be obtained if the patient is introduced to all reasonable treatment alternatives, including no treatment, with explanation of risks and benefits. The dentist must not be paternalistic, meaning that there should be no bias in driving the patient to choose any of the alternatives.1 Thus, it is not uncommon for a patient to choose a different plan than the one the dentist deems best.
To obtain better insight into a patient's decision-making process, it is important for clinicians to try to evaluate the conditions that might guide the patient, such as financial issues, dental care phobia, and expectancy of tooth longevity.2 However, underlying behavioral and historical factors might also play a role in this process. Take, for example, the association between dental care and tooth extraction. It is not uncommon for patients to express a desire to have an extraction, believing it to be the best and most definitive solution to their dental problems.3
Although extractions are still indicated, such as in cases of severely compromised teeth due to periodontal disease, caries, impaction, or as an orthodontic treatment option, to name just a few, they should be seen as a last resource and not as a first option when tooth restoration is achievable.2 The development of new techniques and materials makes it possible for dentists to rehabilitate challenging oral health conditions with great success rates. While extraction might solve the pain and restore health temporarily, it fails to restore function and esthetics. Without posterior rehabilitation, removal of a tooth will further compromise patients' oral health, having a negative impact on the stability of adjacent teeth and periodontal status.4 Moreover, Gupta et al have shown that there is an association between tooth loss without rehabilitation and higher mortality.5
When dentists offer extraction as a treatment alternative among more conservative options, presenting it as a conclusive treatment without consideration for rehabilitation, this may reinforce patients' misconception that it is a treatment plan as good as any other. Even though health communication skills are developed in dental school, dentists may still find it hard to fully convey to a layperson the advantages and disadvantages of each treatment plan, even when thoroughly explaining it to obtain informed consent.6
In their Dental Registry and DNA Repository (DRDR) project,7-10 the present authors observed that there was a high number of patients who chose teeth extraction instead of rehabilitation or restoration as a solution to their chief complaint. The factors described in the health records affecting patients' decisions ranged from financial concerns and the desire to expedite and rapidly complete care. In the present report, a case is described of a patient who chose an extraction alternative as a treatment for his oral conditions, but many complications developed that resulted in poorer quality of life. This case, found in the DRDR database, is reported for the purpose of exemplifying a situation where extractions were not the ideal treatment plan, but the treatment was nonetheless carried out in respect to the patient's autonomy.
Case Report
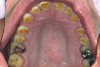
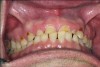
A 53-year-old man sought care at the University of Pittsburgh School of Dental Medicine for a routine oral evaluation and prophylaxis on August 12, 2016. After a full periodontal examination, the patient was reported having moderate to severe periodontitis. Probing depths ranged from 1 mm to 7 mm and several teeth had class I mobility. Severe attrition and lingual erosion were found on all maxillary teeth, except the molars (Figure 1 and Figure 2).
The patient's medical history was positive for tobacco use (half to one pack per day), seasonal allergies, and hepatitis C. He reported the use of ibuprofen (Advil®) for hip pain and recreational marijuana. The blood pressure was documented as 155/98 millimeters of mercury, pulse of 72, unlabored respiration, and body mass index of 23.0.
After consultation at the School's Prosthodontics department, the patient was presented with possible treatment options. Alternatives ranged from full-mouth rehabilitation, ie, periodontal and restorative treatment that included scaling, root planing, composite restoration, and/or crown placement, to no treatment at all. Due to financial reasons, the patient selected the least expensive treatment, which was extraction of all maxillary teeth and fabrication of a maxillary complete denture. The patient made this decision despite being informed that at his age these procedures could be considered overly aggressive in light of his oral health conditions.
Respecting the patient's autonomy, surgical extraction of the maxillary teeth and an alveoloplasty were performed on May 11, 2017, with no complications, and oral and written postoperative instructions were provided. The interim denture was delivered on the same day. The patient complained of ill fit, gagging, and pain, so, even though the prosthodontist verified that the denture fit well, adjustments were made for the patient's comfort.
In the following months, besides complaints of fit and sore spots, the patient had several postoperative issues, including right canine space infection with swelling of the maxilla and numerous bony spicules. Each complaint was properly addressed, but the resolution involved several surgical procedures that the patient did not anticipate.
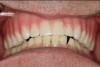
On January 11, 2018, the patient appeared without the maxillary denture in mouth, complaining that it was loose. He stated that he was "very unhappy with the dental procedures." The interim denture was causing discomfort to the point that he could not breathe properly. He suffered with pain, poor function, and subpar esthetics, which were not restored because the patient avoided using the denture. Eleven days later, at the patient's request the acrylic part of the denture was significantly thinned down (Figure 3), even though he was informed that doing so would cause the denture to be more prone to breakage. Since then the patient had numerous subsequent appointments for adjustment of the denture, including several visits to remake it. Eventually, he received a remade denture and has been satisfied with the current resolution.
At the time of this writing, nearly 2 years after the extraction appointment, the patient is assessing the option of having dental implants for an overdenture to be built.
Discussion
Although this case is an extreme example of extractions not working out favorably, all of these risks were properly conveyed to the patient when treatment alternatives were presented. The patient's decision-making process was impacted by financial limitations, but he was optimistic for favorable results due to having sought care in a top-ranked dental teaching facility. Nevertheless, he is now facing a cost as high as the full-mouth rehabilitation alternative, which he discarded due to financial concerns but that would have been a more adequate treatment for his conditions.
A more common and relatable situation in daily dental practice is when a patient chooses extraction instead of endodontic therapy of a tooth with a good or fair prognosis. As mentioned earlier, the reasons for the choice of extraction vary among financial situation, dental care phobia, desire for a "quick fix," and expectancy of tooth longevity, as well as others. In challenging situations like these, a conflict arises between the ethical principles of patient autonomy and nonmaleficence. However, as long as patients are adequately informed of the risks and benefits of all treatment alternatives, they have the right to determine what shall be done to their body, and dentists must respect their decision, as was done in this case. Because dentists must not be paternalistic, a patient cannot be guided to choose the treatment alternative the dentist deems best.
Interestingly enough, Re et al published a study in which they aimed to observe, in a hypothetical scenario, if dentists chose for themselves the same treatment they suggested for their patients. First, 100 volunteer dentists were shown 15 radiographs of compromised teeth and had to decide between extraction, endorestorative recovery, or referral to a specialist to save the tooth. Then, the radiographs where shown again, with the question: "If this was your tooth, what would you do?" Comparing the responses, the authors concluded that dentists were more conservative regarding their own teeth, opting for endorestorative treatment or referral to specialists.11
Hypothetical scenarios do not reproduce feelings such as pain and fatigue, dental care phobia, patient personality, oral health history, and financial issues that influence decision-making. However, the Re et al study shows that dentists chose challenging but more conservative procedures to save their own teeth, indicating that they value tooth retention over tooth extraction. Extraction is left as a last resource for when the prognosis is hopeless and there are no other alternatives to save the tooth.11 This strengthens the argument that extraction is not seen as a gold standard of care by providers.
If dentists, with all of their background knowledge, do not choose this option for themselves, patients should not be choosing it either. Considering that dentists, to the best of their abilities, are fully communicating risks and benefits of each treatment plan to obtain informed consent, patients must not be fully comprehending the implications of their decision. There appears to be a disconnection between the dentist's and patient's understanding of the treatment plans and their outcomes that the dental community must address. This could be done via training for predoctoral students and continuing education for practicing professionals.
Another factor that should be considered when indicating extraction is that, in some cases, this treatment must be followed by proper rehabilitation. For example, extraction by itself is less costly than endodontic treatment plus a full crown, which perhaps may sway patients toward the extraction option. However, failure to rehabilitate the missing tooth could cause further harm to oral health, negatively impacting adjacent teeth stability and periodontal status.4 An adequate treatment plan involving extraction should include a bridge or implants to restore the missing teeth. This would level the cost of the treatment alternatives, perhaps making patients less inclined to choose extraction only for financial reasons. Therefore, it could be argued that treatment plans that do not include rehabilitation after extraction when rehabilitation is needed are not in compliance to the ADA principle of nonmaleficence, because harm to oral health is bound to happen.
With advances in implant dentistry, there is a trend to extract teeth with good or fair prognoses to save bone for placement of implants, which are being considered equal or even superior to natural teeth in regard to survival.12-14 Moshaverinia et al challenged this school of thought as they summarized 10-year follow-up studies that have shown that the longevity of periodontally compromised teeth surpasses implants, especially in well-maintained patients.15 They demonstrated that teeth with good or fair prognoses should not be extracted, because there is a lack of evidence supporting this aggressive approach. They also stated that traditional dental practice should consider extraction as a last resource.
Chandki and Kala also believe that adequate consideration should be given to treatments focusing on preserving and restoring compromised teeth instead of extraction and replacement.12 Considering the expenses necessary for implant placement, Parirokh et al pointed out that this approach might not be a reasonable option for many patients, and this must be taken into account when presenting the treatment plan. Extraction without implant placement would cause greater bone resorption and atrophy of the alveolar ridge than if the tooth was kept, further compromising the possibility of future implant placement.16 As such, although implants have a high success rate, the cost of implant placement is high, and there is a lack of evidence showing they have better survival rates than teeth with good or fair prognoses.
Overall, it is important that the dental community effectively communicates to patients that tooth extraction is an aggressive, last-resource approach. The difference between patients' and dentists' perceptions of the optimal treatment alternative shows that this message may not be properly understood, jeopardizing informed consent. The present authors suggest that to start changing patients' perceptions, the extraction alternative should not be presented as a final treatment goal, but accompanied by rehabilitation when appropriate. This would help level treatment costs and thereby eliminate financial bias. The hope is that this approach will eventually change patients' misconceptions and enable them to stop considering extraction as a complete treatment option without proper rehabilitation. Nevertheless, patients' autonomy protects their right to choose less-than-optimal treatment plans. Thus, only when the removal of a restorable tooth would cause injury or be below the standard of care may dentists legally and ethically refuse to offer such extraction as a reasonable alternative.
Conclusion
Patients' autonomy must be respected in their decision-making process, even though they might be inclined to choose extraction as a treatment option instead of more conservative approaches. However, indicating extraction alongside other treatment plans may lead patients to believe it to be as good an alternative as any other, and not a last resource. Patients' perception of extraction is not the same as dentists', which is to value teeth retention and proper oral rehabilitation. Dental healthcare providers need to be aware of and address this situation.
Acknowledgment
The University of Pittsburgh Dental Registry and DNA Repository, which is supported by the School of Dental Medicine, provided data for this report. The authors sincerely thank Joseph D. Myers for proofreading and editing the article.
About the Authors
Vicente Telles, DDS
Research Assistant, Department of Oral Biology, School of Dental Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania
Mariana Bezamat, DDS
Graduate Student Researcher, Department of Oral Biology, School of Dental Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania
Alexandre R. Vieira, DDS, PhD
Professor, Department of Oral Biology, School of Dental Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Iovino RP. Revising the American Dental Association Principles of Ethics and Code of Professional Conduct: Adding "Respect for Human Dignity" as the sixth principle of dental ethics to accommodate advances in genetic science. J Am Dent Assoc. 2016;147(12):918-922.
2. Broers DL, Brands WG, Welie JV, de Jongh A. Deciding about patients' requests for extraction: ethical and legal guidelines. J Am Dent Assoc. 2010;141(2):195-203.
3. De Marchi RJ, Leal AF, Padilha DM, Brondani MA. Vulnerability and the psychosocial aspects of tooth loss in old age: A southern Brazilian study. J Cross Cult Gerontol. 2012;27(3):239-258.
4. Aquilino SA, Shugars DA, Bader JD, White BA. Ten-year survival rates of teeth adjacent to treated and untreated posterior bounded edentulous spaces. J Prosthet Dent. 2001;85(5):455-460.
5. Gupta A, Felton DA, Jemt T, Koka S. Rehabilitation of edentulism and mortality: a systematic review. J Prosthodont. 2018. doi: 10.1111/jopr.12792.
6. Seymour B, Yang H, Getman R, et al. Patient-centered communication: exploring the dentist's role in the era of e-patients and health 2.0. J Dent Educ. 2016;80(6):697-704.
7. Ravindramurthy S, Vieira AR. Depression and its effects on the success of resin-based restorations. Spec Care Dentist. 2018;38(4):266-268.
8. Amoo-Achampong F, Vitunac DE, Deeley K, et al. Complex patterns of response to oral hygiene instructions: longitudinal evaluation of periodontal patients. BMC Oral Health. 2018;18(1):72.
9. Vieira AR, Silva MB, Souza KKA, et al. A pragmatic study shows failure of dental composite fillings is genetically determined: a contribution to the discussion on dental amalgams. Front Med (Lausanne). 2017;4:186.
10. Vieira AR, Hilands KM, Braun TW. Saving more teeth-a case for personalized care. J Pers Med. 2015;5(1):30-35.
11. Re D, Cerutti F, Consonni D, Gorni FG. Treatment planning of damaged teeth: to recover or to extract? Minerva Stomatol. 2017;66(5):201-211.
12. Chandki R, Kala M. Natural tooth versus implant: a key to treatment planning. J Oral Implantol. 2012;38(1):95-100.
13. Mordohai N, Reshad M, Jivraj SA. To extract or not to extract? Factors that affect individual tooth prognosis. J Calif Dent Assoc. 2005;33(4):319-328.
14. Anson D. The changing treatment planning paradigm: save the tooth or place an implant. Compend Contin Educ Dent. 2009;30(8):506-517.
15. Moshaverinia A, Kar K, Chee WW. Treatment planning decisions: implant placement versus preserving natural teeth. J Calif Dent Assoc. 2014;42(12):859-868.
16. Parirokh M, Zarifian A, Ghoddusi J. Choice of treatment plan based on root canal therapy versus extraction and implant placement: a mini review. Iran Endod J. 2015;10(3):152-155.