You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Communication between a dentist and their technical colleagues is truly an art. The laboratory prescription is the foundation for this communication to take place. There are many complex procedures that are required for a dental team to reach a successful outcome, but they are all dependent on communication between each team member. The humble laboratory prescription, when properly respected, is an essential requirement to achieve this goal. The fundamentals of this respect begin with the dentist's proper attention to writing it and with the laboratory reading and respecting the dentist's requests. The pursuit of achieving a thorough and unencumbered dialogue flow between the clinician and technician will differ according to work styles. As in all aspects of personal and professional life, each person has their own preferences in reference to communication. In the realm of dentist-laboratory teams, the director and leader of the team is the dentist, as they are responsible for care. A dentist will select their laboratory partner for various criteria, all of which have different levels of significance.
Effective Communication
Style of communication may be the most important factor in the prescription-writing process. Some dentists prefer to write short and simplistic prescriptions while others will cover each and every detail in long-form text (Figure 1). Others still prefer to discuss details on a phone call with a bilateral exchange of thoughts (Figure 2). Whichever method of communication is preferred, it must satisfy the main purpose in directing the laboratory to meet the desired goals of the dentist.
Just as the dentist is responsible for providing patient care, the dental laboratory is fully responsible for filling the prescription. Therefore, laboratory technicians need to thoroughly understand the direction the dentist is communicating and be comfortable executing it.
As in all forms of communication, all parties must speak the same language. The terminology used between the dentist and the laboratory must be mutually understood. If a technician or clinician is unfamiliar with technical terminology, they should familiarize themselves with the proper nomenclature in relation to dental prosthetics. Regular review of the glossary of prosthodontic terms can be helpful in this area; however, everyone should be sensitive to the evolution of some terms that may be used between professionals of different generations. Terms that were contemporary 20 years ago may have fallen out of use. Technicians must also be aware that slang terms may be used that are not found in a professional glossary. Since this vernacular is unprofessional and can confuse the communication process, the laboratory should work to correct these terms; the entire team will benefit. The group's goals should be to master communication bilaterally and to be as clear and correct as possible, as well as to request clarity when in doubt. There can be unforeseen questions or variables that arise during the process in the laboratory. In this situation, the technician needs to be expeditious in contacting the dentist to share thoughts and get direction prior to proceeding with the work. It is advantageous to the dentist to prioritize this interchange appropriately, as potential work delays may discourage the laboratory from initiating these discussions in the future.
The dental laboratory is required by law to follow the written specifications contained in the prescription.1 The dentist is ultimately responsible for the restorative treatment design and material selection of any restoration and must direct the laboratory according to their desires. The laboratory is then required to follow the dentist's directions, and it is illegal to shift from those directions for any reason without the consent of the licensed dentist. When verbal instruction strays from the original script, or if it significantly augments the written instructions, it is good practice to document the date and time and indicate exact changes to reflect the discussion and instructions given.
The context of a well-developed laboratory prescription varies with the type of restoration involved and the current relationship with the laboratory. A typical dentist-laboratory relationship is an ongoing endeavor which, in order to run smoothly, should regularly build upon past experiences so that each step does not require constant repetition. Early in the relationship-building process between laboratory technician and dentist, an understanding needs to be in place as to generally accepted basics.
Materials
Certain aspects of the dentist's desires (such as alloy specification and ceramic materials used)can be discussed early in a relationship and considered as a baseline; however, each patient's health history and/or allergies and sensitivities are known only by the clinician; therefore, alloy and/or ceramic materials should be included in the written prescription. There are, however, other aspects which should always be communicated on each laboratory prescription. Certain information such as a patient identifier, tooth numbers, shade, and return expectations are usually provided, but there is much more that should be considered depending on the type of work being requested, such as implants, which can require a variety of specific components (Figure 3). For implant-supported crowns and fixed partial dentures, basic facts such as implant type and size can often be overlooked with the assumption that the impression component will provide that data. This can be disastrous, as an error here may not be discovered until completion and with costly consequences. Also, the method of connection, such as screw retention or cement retention, must also be conveyed on the prescription. Required components should also be mentioned, as well as whether the laboratory or dentist will acquire them. If the laboratory purchases them, are OEM or third-party-manufactured components desired? Lack of appreciation for the importance of all this information, particularly with implant-borne restorations, can be a very costly oversight.
For prescriptions relating to removable prosthodontics, a plethora of details is often missing from the "lab slip." For a partial prosthesis, a major connector design should be drawn, either on a surveyed cast (Figure 4) or at a minimum on paper. This drawing should include major and minor connectors and clasp design. If the prosthetics are in combination with a fixed partial denture, the desired retainer system must be communicated. Here the mutual understanding of terms such as intra-coronal, extra-coronal, semi-precision, and precision, to name a few, are paramount. For both full denture and partial denture prosthetics, technicians need to consider tooth mold selection, border extensions, and posterior palatal seal, as well as occlusal scheme and function. Omission of any of this information by the dentist in essence delegates these decisions to the laboratory. Often an experienced dental technician is knowledgeable in these areas, but the dentist should specifically request their opinion and not delegate by omission; the dentist is ultimately responsible to the patient. These guidelines apply similarly to orthodontic appliances.
Diagnostic Wax-Ups
Instructions pertaining to diagnostic wax-ups should communicate the goals of the desired outcome as well as a description of supporting structures visualized on the dental casts. This can be aided by augmenting the prescription with the inclusion of photographs. Communicating any planned adjunctive therapy with the technician is also helpful. Information such as incisal length, labial surface position, and midline cannot be accurately hypothesized on an articulator and therefore should be determined by the dentist and communicated to the laboratory in the prescription. The desired occlusal function should also be determined by the dentist. Hopefully, a dentist undertaking this type of work shares mutual respect and regular dialogue with their technical partner, and discussion on these details can lead to a successful outcome.
Full-coverage restorations and fixed partial dentures-whether natural-abutment-supported or implant-supported-can be some of the most demanding work created in the dental laboratory. The desired outcome, whether in confirmative or non-confirmative dentistry, should always be clear to all at the beginning of the process. The guidelines or template utilized must be clearly understood upon inception and assumptions must be avoided. The dentist should inform the laboratory if they wish to use an approved provisional cast or diagnostic wax-up as a template. Insufficient communication of desired outcomes, even at a substructure stage, can cause less than adequate and unnecessarily costly results. There should be a careful evaluation of all this information by the master dental technician, and any ambiguity should be discussed between dentist and technician as soon as possible.
Color and Shade
In the arena of shade communication, laboratories and dentists are faced with some additional challenges. A simple study of color science will demonstrate how complex and subjective shade evaluation is. When attempting to match a patient's existing tooth shade, the dentist will typically employ shade guides, photographs, and shade map diagrams. The nature of color perception makes this an immensely subjective task largely dependent on environmental conditions. Both the dentist and technician should be using 5500k artificial light sources with a CRI of at least 90. Sample teeth should be clean and hydrated, and any bleaching should be completed prior to sampling. When describing the intricacies of a tooth's shade, everyone needs to understand the qualities of color and use the proper terms. Terms such as hue, value, and chroma are often misused. Both dentist and ceramist must understand the same terms in the same way to accomplish the desired result.
Although photographs will not perfectly communicate base color, they are extremely helpful in visualizing relevant details and effects, along with aiding in comparing and contrasting colors within the same photo. To maximize the benefit of this procedure, the photography must be correctly performed. First, the camera needs to be set to have a maximum depth of field with proper exposure. The resolution should be at the camera's maximum and if possible in RAW. Manual settings are advised, as this will keep control in the hands of the photographer.
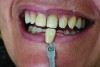
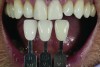
Attention to color temperature is extremely important as well, matching it to the color temperature of the light source. When positioning a shade tab (or multiple tabs), always keep the tab on the same focal plane as the sample tooth (Figure 5 and Figure 6). This positions the tab and the tooth at the same distance from the light source, thus providing the same exposure. It is also best to keep the shade tab identification visible in the photo, for reference purposes.
If communication of subtle details within a tooth's enamel is desired, one must employ a dual polarization filter system to eliminate all reflection (Figure 7). The dentist should describe their perception of the base color as well as the level of detail they wish the ceramist to emulate in the restoration. Photos can easily be shared with Dropbox or other file sharing platforms, and the ceramist should be familiar with photo manipulation programs such as Lightroom.
Conclusion
With current technology, it takes little effort for a dentist to make their technical colleague aware of all the necessary information. It is also just as easy for laboratories to reach out to the dentist-client when information is unclear or not feasible to execute. Oftentimes, details of casts can be communicated with photos taken with a smart device. Video conferencing can be instrumental to virtually bring the patient to the technician and the dentist into the laboratory at a moment's notice. Cloud-based, HIPAA-approved dental laboratory prescriptions make the formation of even the most detailed prescriptions a simple process. Many of these digital prescription solutions are packaged as part of dental laboratory management software and digital impression portal infrastructure.
Whatever technique is utilized, it is incumbent on the laboratory to be aware of local requirements as they pertain to record maintenance. Each state has different laws as to how long the laboratory is required to keep prescriptions; for example, Texas law states that "a dental laboratory owner or manager shall maintain on the premises of a dental laboratory as a part of the laboratory's records a record of each prescription or work order completed at the dental laboratory until the second anniversary of the date the prescription or work order is furnished. The owner or manager shall also maintain the record in an alphabetized file in a separate place."2 If those records are kept digitally, it is important to confirm that that is acceptable in your state; Florida law, for example, specifies that "an original or electronic copy" is sufficient.3 Each state also has its own requirements regarding items that must be included on the prescription; for example, New York law requires "the name of the laboratory to which the prescription is addressed; the date on which it is written; a clear description of the work to be done, with appropriate diagrams if necessary; a clear specification of the character of materials to be used; and the signature and license number of the dentist."4
Aside from the legal ramifications, maintaining records can be beneficial in servicing patients' restorations in the future as well.
It is advantageous for dentists and technicians to work to develop long-term working relationships, since knowing each other's styles and idiosyncrasies can streamline the complexities. As patients become more demanding, it is paramount for dental professionals to accurately communicate in order to prosper in this wonderful profession.
About the Author
Bill Baum, MDT, CDT
Owner
Baum Dental Studio
Instructor
New York University College of Dentistry
Lindenhurst, NY