You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
As periodontists and hygienists know, most patients have at least some degree of pseudopocketing distal to the upper second molar. This excess tissue can create a plaque trap, allow calculus accumulation, and be challenging to clean for hygienists and patients alike. If left over time, the pseudopocket may develop true attachment loss and periodontitis. Additionally, tuberosity tissue poses a challenge for restorative dentists, especially on the distal aspect. Be it a pseudopocket or a true pocket (one with attachment loss), the authors will simply refer to either situation collectively as a "pocket" for the purposes of this article.
There are a number of benefits to removing the tuberosity tissue. Doing so helps to eliminate a pocket to assist in treating and preventing periodontal disease while providing improved access for hygienists and patients to maintain periodontal health. Moreover, it allows dentists to restore teeth with greater clinical crown elongation and provides better margins to help prevent recurrent decay. Also, subgingival margins are circumvented, which helps to prevent periodontal infection.
Periodontists commonly perform distal wedge and distal gingivectomy procedures for periodontal disease treatment and for crown lengthening (also now called crown exposure surgery [CES])1 and discard the tuberosity tissue, rendering it as useless. Because removal of this tissue provides numerous benefits as described above, and if the tissue is already going to be removed, the authors propose that the standard of care should be to place this extra tissue in areas of periodontal recession. If a patient presents for a connective tissue graft (CTG) and has pocketing distal to the upper molars, the clinician could utilize the tuberosity tissue for the graft first and also to prevent periodontal disease. Unfortunately, the reverse is what typically occurs.
The tuberosity should be the main source of CTGs. Long term this promotes overall periodontal health (by preventing periodontal disease and recession), enhances the predictability of restorative treatment, and, thus, prevents future complications and expenses for patients.
This, therefore, begs the question of "why do clinicians discard this fine piece of connective tissue without applying its use as a CTG somewhere else in the mouth?" Practitioners rarely use connective tissue (CT) from the tuberosity for CTG procedures perhaps because of misunderstanding how to harvest and modify the graft to use it esthetically without resulting in a keloid-like appearance. This article will suggest techniques to help utilize the tuberosity tissue for CTGs. The assorted techniques are illustrated in Figure 1 through Figure 17.
Overview of Connective Tissue Grafting
Various techniques for root coverage and soft-tissue ridge augmentation for esthetics in restorative dentistry and for dental implants have been developed over the years.2 When referring to CTGs, for purposes of this article, the authors are referring to both root coverage grafting and soft-tissue ridge augmentations. The free gingival graft3 (now with new nomenclature referred to as the epithelialized palatal graft [EPG]1) and the subepithelial CTG use palatal tissue as the graft material.4 Other autograft sources for CTGs include the tuberosity and retromolar areas. Allografts, membranes, and, more recently, xenografts have been used instead of autografts and have proven to be successful.1,3-7 Coronally advanced flaps8 (now referred to as coronally positioned flap [CPF]1) have been utilized with graft material,5 without graft material,8 and with membranes for root coverage.6,7 All techniques require some sort of tissue manipulation and, thus, are susceptible to various levels of swelling, bruising, and discomfort.
The Miller classification describes the amount of expected root coverage needed with various types of periodontal recession.3 Miller Class I and Class II periodontal recession cases have a high degree of success of the graft and the highest chance for complete root coverage.2,3 Miller Class III and Class IV periodontal recession cases have an excellent chance of grafting success to prevent further periodontal recesssion with minimal root coverage.2,3 All classes can have increased attached tissue and CT volume to prevent further periodontal recession.3 Soft-tissue ridge defects have been classified in various manners, with the Seibert classification being used ubiquitously.9 Seibert Class I has a width defect and normal ridge height, Class II has a height defect and normal width, and Class III has a defect in both ridge width and height.9
While the palate has been the most commonly used donor area for CTG procedures, problems with palatal harvested CT include variable types of non-CT tissue (eg, blood vessels, nerves, adipose, and glandular tissue)10 as well as variability in density and amount of fibrous CT.11 Because consistently dense CT is desirable for CTG procedures rather than any other tissue, the palate may not be the best source for CTGs.
Tuberosity for Connective Tissue Grafting
Tuberosity CT has been reported to obtain full root coverage with a good color match.12 It also is easier and quicker to obtain the graft material than using the palatal approach.12 Tuberosity tissue has been utilized in soft-tissue augmentation around implants with high success.13 Tuberosity has been used for CTGs in severe bony defects9 as well as in a block of epithelialized CT and bone for dental implant placement.14 The literature provides only a limited number of case reports on the use of tuberosity tissue for the aforementioned procedures and offers minimal information about the soft-tissue component of the tuberosity. Studer found significantly more soft-tissue thickness in the tuberosity when compared with the hard palate and reported the CTG size is limited by the width of keratinized tissue.15
Macroscopically, the tuberosity has consistentlydense fibrous CT, is less vascular than palatal tissue, and has no adipose or glandular tissue.15 This means that after the tuberosity graft is de-epithelialized, dense CT is all that remains. Because the tissue harvested in the tuberosity is so far posterior, eating and talking are less affected than when a palatal graft is performed. Additionally, the risk of bleeding and discomfort may be decreased due to smaller blood vessels and nerves in the tuberosity.
The thickness of the epithelial layer is consistently thinner in the tuberosity than in the palate, thus a greater percentage of the CTG is comprised of CT. Because the goal of CTG is to add CT, the larger volume of CT (quantity) and denser CT (quality), along with the other benefits mentioned above, may indicate the tuberosity is ideal tissue for CTGs (Table 1).
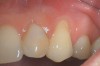
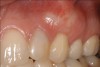
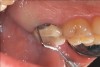
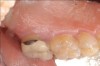
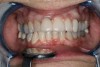
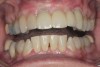
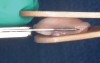
A complication in using CT from the tuberosity reported in the literature is a tendency for clinicians to harvest tissue that is too thick.12 This can result in a keloid-like appearance similar to what may occur with an EPG. This excess thickness can be unesthetic (Figure 1 and Figure 2) and subsequently require a gingivoplasty to remove the superfluous tissue.12 This problem may perhaps be alleviated with proper thinning of the graft prior to insertion into the recipient area.
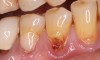
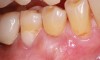
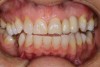
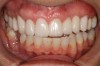
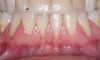
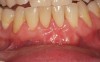
Regarding the avoidance of a gingivoplasty procedure later, there appears to be nothing in the literature describing the ideal thickness of a tuberosity CTG. From palatal and allograft thickness recommendations, one could hypothesize that the thickness be between 0.75 mm and 2 mm. This article will propose a graft thickness between 1 mm to 1.5 mm (Figure 3 and Figure 4) for the optimal functional and esthetic outcome and will discuss various procurement and fileting techniques.
Tuberosity Harvesting and Fileting Techniques: Case Examples
The authors estimate that they have treated more than 1,000 patients with the tuberosity CT technique. The purpose of this initial report is to provide a proof of principle. Further studies are forthcoming. Typically, patients receive a comprehensive periodontal examination with cone-beam computed tomography (CBCT) imaging and photography. The tuberosity is evaluated 3-dimensionally via periodontal probing of the distal tooth and measuring the tuberosity's width and height. The amount of soft tissue coronal to the bony tuberosity is estimated by the outline of the soft tissue on x-rays (panoramic and periapical views). The tuberosity is further evaluated on the day of treatment via bone sounding of the entire tuberosity.
The recipient site surgical techniques include varied approaches, such as the CPF and tunneling techniques.5 The purpose of this article is not to discuss the technique for the recipient site, but instead the techniques for procuring tuberosity CT. Post-treatment medications include methylprednisolone, codeine 30 mg with 325 mg acetaminophen alternated with 600 mg ibuprofen, and chlorhexidine rinse beginning 2 days post-treatment. Patients are provided additional post-treatment instructions.
After the recipient site is prepared, the CTG can be harvested from the tuberosity. Immediately after harvesting the tuberosity tissue, dry gauze should be placed in the tuberosity (similar to an extraction) and the teeth closed on a mouth prop to help apply posterior pressure and hold the gauze in place. The graft can now be placed and sutured in the recipient site. Frequently, bleeding subsides in the tuberosity area after the procedure is completed. To help prevent bleeding recurrence, the patient should leave with gauze applied for 30 minutes.
Tuberosity tissue can be harvested using either a distal gingivectomy (DGV) technique12 or distal wedge (DW) technique for CTGs.Calculus is commonly found on the tooth surface (either enamel or root) after the tuberosity harvest. This area must be inspected and scaled and root planed judiciously.
The clinician must determine which of these two harvest techniques should be utilized. Each has its advantages in different situations. For non-wide (buccal-palatal dimension) tuberosities, the DGV technique offers less tissue loss. For wide tuberosities, which are greater than 4 mm in width buccal-lingually and have more CT, the DW technique may be advantageous, as the flap can be approximated and closed with sutures, and this potentially may be more comfortable for the patient. Either technique adequately removes the excess tissue and reduces the pocket. The DGV approach provides a faster tissue harvest and a greater amount of tissue (Figure 5 and Figure 6).
For the DW technique, a #15 or #15C blade is used. For the DGV technique, the graft is harvested with a #12 blade.12 A single-blade scalpel can be used, or the graft can be harvested and partly trimmed with a double-blade scalpel with a 1.5 mm separation. A split-thickness approach with a blade is suggested, because this prevents removing the periosteum and possible tori formation as has been reported with the EPG,2 which could be unesthetic. Because the DW technique is a full-thickness procedure, it is more likely to include periosteal tissue and result in the formation of a tori under the soft-tissue graft.
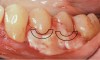
Depending on the 3-dimensional aspect of the graft, it can be adjusted in a myriad of ways for thickness and for the number of teeth receiving root coverage. If the CT is being used for a soft-tissue ridge-augmentation procedure, the tissue, of course, can be left thicker (Figure 7 through Figure 10). This prevents the need to suture multiple pieces of graft material together, which is commonly needed with other graft materials.
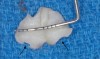
After the graft has been harvested it can be further adjusted with a single- or double-blade scalpel. In the authors' experience, it appears to be easier to obtain the graft with a #12 blade and then adjust the graft after the harvest with a single or double #15 or #15C blade (Figure 11 through Figure 15). Note in Figure 11 through Figure 15 the lack of adipose or glandular tissue in the CTG from the tuberosity; once the CTG is de-epithelialized all that is present is CT.
Because the tuberosity tissue has denser CT than the palate tissue, it is easier to filet into multiple grafts. Additionally, the epithelial layer is very thin. This poses a distinct advantage for the DGV technique over the DW. If the DW technique is used, more CT will be left with the flap and less CT will be available for the graft. Some or all of the epithelial layer may be retained if it is desired to keep keratinized tissue retained in the graft. From the ease of harvesting to maximizing the amount of CT, the authors prefer the DGV technique over the DW; however, in some circumstances, such as with wide tuberosities, the DW approach may be more advantageous.
Fileting can be accomplished freehand either on moistened gauze laid on a moistened sharpening stone for support, a moistened surgical towel, or a moistened tongue blade. If necessary, two tongue blades can be utilized with a "tong"-like grip to secure the CTG for fileting (Figure 13). The importance of preventing desiccation of the graft cannot be overemphasized.
The techniques for de-epithelialization and graft trimming with what the authors call the "book" or "butterfly" technique can be visualized in Figure 11 and Figure 12. When the initially harvested CTG is more than 7 mm thick it can be sliced further into one connected CTG in a "snake" or "trifold" configuration or separated into multiple individual CTGs to a 1 mm to 1.5 mm thickness (Figure 13 through Figure 15). In some instances when the tuberosity tissue forms a "c" shape distal to the molar, the CTG can be fileted and then placed around the buccal or lingual aspect of teeth to conform to the shape of the cementoenamel junction (CEJ) around single or multiple adjacent teeth (Figure 11 and Figure 12).
Class V fillings are artificial materials that tend to fail at the apical extent and have poor long-term success (Figure 3).1 Conversely, CTGs are natural and attach to the root surface and have high long-term success (Figure 4).1
If insufficient tissue is harvested from the tuberosity for multiple-tooth CTG procedures, the addition of other graft materials may allow multiple teeth to be grafted in one treatment. In these situations, for higher predictability, use of autograft tissue (perhaps from the tuberosity) is suggested in the worst areas of recession and other graft materials (eg, allograft CT or membranes) would be used for augmentation in the less involved areas of periodontal recession (Figure 7 and Figure 8).
Discussion
Dense CT presumably is less susceptible to shrinkage than less-dense CT. One problem with denser CT may be the need for a longer amount of time to blend in with adjacent non-grafted areas. Due to density, a CT graft might never completely blend in and always demonstrate an unesthetic keloid-like appearance. Therefore, with tuberosity tissue, adjusting the tissue thickness prior to placement of the graft is highly clinically relevant. This may be why periodontists have been reluctant to use tuberosity tissue as CT. Palatal tissue has less-dense CT than tuberosity tissue and, therefore, the authors hypothesize and have observed, shrinks more. Because palatal tissue has been the predominant tissue used in CTG, clinicians have become used to the shrinkage associated with the palatal CT and may not realize the need to thin a dense CTG to prevent a keloid-like appearance. Thus, in the past when a tuberosity was used for this purpose, if it was not properly trimmed it would have frequently resulted in an unesthetic keloid-like appearance. The tuberosity CTG should be trimmed to 1 mm to 1.5 mm thick to avoid the need for a future procedure to adjust tissue thickness for esthetics (Figure 3 and Figure 4, Figure 16 and Figure 17).
Studer reported the CTG size is limited by the width of keratinized tissue in the tuberosity.15 However, the present authors believe the amount of dense CT is not limited by the width of the keratinized tissue, because dense CT can be found in the mucosal tissue of the tuberosity as well. Lingual recession is challenging to treat, particularly in the mandibular incisor region. The use of tuberosity CTG for mandibular lingual recession may be highly effective for root coverage and prevention of further recession, because there is minimal graft shrinkage.
While it may sometimes be difficult to estimate the amount of tissue available for harvesting from the tuberosity, the same could be said with regard to the palate. X-rays may be used and correlated with probing and bone sounding to estimate available tissue. In the authors' experience, the amount of tuberosity CT harvested from each tuberosity consistently provides enough tissue for root coverage on two to four teeth.
Having used tuberosity CT for nearly 20 years when performing a CTG for root coverage or soft-tissue ridge augmentation, the authors consider the tuberosity their first choice for the graft material, followed by allograft materials and/or membranes, and, finally, palatal tissue. However, if a palatal flap is elevated for any reason, and a CTG is needed elsewhere, the palate CT should also be considered for grafting. For root coverage on multiple teeth or soft-tissue ridge defects, the tuberosity CTG can be used individually or combined with allograft, xenograft, or autograft (palate or retromolar) tissues (Figure 8). Additionally, the authors have observed that the tuberosity is an excellent source for CTG for pre-adolescent patients and removes excess tissue thickness over unerupted second molars and aids in their eruption.
Few case reports document the use of tuberosity CT,1,2 and future studies should analyze its use further. The density, amount, and type of tissue in the palate and tuberosity should be compared histologically in the same patient. Split-mouth studies could compare the root coverage percentage and esthetics of tuberosity CT with a 1 mm to 1.5 mm thickness when compared to other grafting materials.
Conclusion
This article has described advantages of tuberosity CT over palatal CT. The primary benefit is the ability to harvest a greater volume of denser CT from the tuberosity than from the palate. An added advantage is the elimination of the pocket on the posterior molar, which helps prevent and/or treat periodontal disease and affords a more easily maintainable area for the patient and hygienist. Finally, this approach can provide crown elongation to improve restorative dentistry.
Two techniques have been presented for harvesting tuberosity tissue: the DGV and DW techniques. The former is the faster, easier approach for harvesting the largest amount of CT. A certain thickness-1 mm to 1.5 mm-is proposed to prevent an unesthetic keloid appearance.
When performing removal of tuberosity tissue for periodontal disease treatment or crown elongation, it may be prudent for the clinician to also consider using this CT tissue to treat areas of any periodontal recession that may be present. After all, a periodontist should be inclined to repair all areas of periodontal defects when warranted, whether periodontal recession or ridge defects, and not waste perfectly good tissue. Rather than discard an ideal piece of CT, the clinician may be able to utilize the tuberosity tissue to help the patient achieve optimal oral health.
ACKNOWLEDGMENTS
The authors thank the International Society of Periodontal Plastic Surgeons for selecting this article for this special publication commemorating the Society's 25th anniversary. Dr. Godat especially thanks his mentor and partner Dr. P.D. Miller for his guidance, and Dr. Gruen for his cosmetic restorative treatment of patients in this study.
About the Authors
Mitchel S. Godat, DDS, MS
Clinical Professor, Department of Periodontology, University of Tennessee Memphis Health Science Center, Memphis, Tennessee; Clinical Professor, Department of Periodontics, University of North Carolina, Chapel Hill, North Carolina; Private Practice, Memphis, Tennessee
Todd D. Gruen, DDS
Private Practice, Germantown, Tennessee
Preston D. Miller, DDS
Clinical Professor, Medical University of South Carolina, Charleston, South Carolina; Fellow, International Society of Periodontal Plastic Surgeons
Roger D. Craddock, DDS
Private Practice, Memphis, Tennessee
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Miller PD. Miller classification of marginal tissue recession revisited after 35 years. Compend Contin Educ Dent. 2018;39(8):514-520.
2. Miller PD, Allen EP. The development of periodontal plastic surgery. Periodontol 2000. 1996;11:7-17.
3. Miller PD. A classification of marginal tissue recession. Int J Periodontics Restorative Dent. 1985;5(2):8-13.
4. Langer B, Calagna LJ. The subepithelial connective tissue graft. A new approach to the enhancement of anterior cosmetics. Int J Periodontics Restorative Dent. 1982;2(2):22-33.
5. Allen EP. Subpapillary continuous sling suturing method for soft tissue grafting with tunneling technique. Int J Periodontics Restorative Dent. 2010;30(10):479-485.
6. Chao J. A novel approach to root coverage: the pinhole surgical technique. Int J Periodontics Restorative Dent. 2012;(32):521-530.
7. Harris R. A comparison of 2 root coverage techniques: guided tissue regeneration with a bioabsorbable matrix style membrane versus a connective tissue graft combined with a coronally positioned pedicle graft without vertical incisions. results of a series of consecutive cases. J Periodontol. 1998;69(12):1426-1434.
8. Allen EP, Miller PD. Coronal positioning of existing gingiva: a simple solution for treating shallow marginal tissue recession. J Periodontol. 1989;60(6):316-319.
9. Meltzer JA. Edentulous area tissue graft correction of an esthetic defect. A case report. J Periodontol. 1979;50(6):320-322.
10. Soileau K, Brannon RB. A histologic evaluation of various stages of palatal healing following subepithelial connective tissue grafting procedures: a comparison of eight cases. J Periodontol. 2006;77(7):1267-1273.
11. Bertl K, Pifl M, Hirtler L, et al. Relative composition of fibrous connective- and fatty/glandular tissue in connective tissue grafts depends on the harvesting technique but not on the donor site of the hard palate. J Periodontol. 2015;86(12):1331-1339.
12. Jung UW, Um YJ, Choi SH. Histologic observation of soft tissue acquired from maxillary tuberosity area for root coverage. J Periodontol. 2008;79(5):934-940.
13. Roccuzzo M, Gaudioso L, Bunino M, Dalmasso P. Surgical treatment of buccal soft tissue recessions around single implants: 1-year results from a prospective pilot study. Clin Oral Implants Res. 2014;25(6):641-646.
14. da Rosa JC, Rosa AC, Fadanelli MA, Sotto-Maior BS. Immediate implant placement, reconstruction of compromised sockets, and repair of gingival recession with a triple graft (cancellous and cortical bone and soft tissue graft). from the maxillary tuberosity: a variation of the immediate dentoalveolar restoration technique. J Prosthet Dent. 2014;112(4):717-722.
15. Studer SP, Allen EP, Rees TC, Kouba A. The thickness of masticatory mucosa in the human hard palate and tuberosity as potential donor sites for ridge augmentation procedures. J Periodontol. 1997;68(2):145-151.