You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Dental professionals acknowledge that oral health is essential for overall health and well-being.1-3 Periods of pregnancy are no exception. Yet many dental and medical professionals, including prenatal care providers, struggle with interpreting the safety and appropriateness of dental treatment during pregnancy despite a series of consensus reports and guidelines that indicate preventive and restorative dental care are both safe and essential.4,5 Not surprising, therefore, this uncertainty also seems to exist among expectant mothers. Few pregnant women seek or receive routine dental care, and as many as one in two with obvious dental problems do not seek care.6
Good oral health and dental hygiene are critical components of a healthy pregnancy and may reduce the burden of bacterial load and inflammatory mediators, enable dental interventions to be avoided, and help the mother-to-be and her fetus maintain overall well-being.6,7 Additionally, pregnancy may provide a teachable moment when the mother-to-be may have a heightened interest in oral health, thereby presenting the dental team with an opportunity to discuss optimal self-care and appropriate use of dental services for both herself and her infant.1 Further, the multidisciplinary array of prenatal healthcare professionals allows for interprofessional collaboration and the chance to achieve better health outcomes as well as referral opportunities.
Deferral of dental care until after delivery often results from fear and caution by patients and the dental team. The complex molecular and cellular interactions of the systemic-oral relationships are challenging to discuss as concrete clinical recommendations. Many patients and their prenatal care providers are not always aware of these relationships.8 To avoid any misunderstanding and to build skills and confidence in caring for pregnant women, dental professionals should familiarize themselves with the current consensus statements and guidelines to provide appropriate dental services.9
The dental management of the pregnant patient with comorbidities such as diabetes, valvular conditions, hypertension, bleeding disorders, and so on, as well as pregnancy complications and/or marked risk factors for adverse outcomes are beyond the scope of this review. The emphasis is the healthy patient with a non-complicated pregnancy.
Consensus Statements and Practice Guidelines
Multidisciplinary panels representing social care and healthcare for women and neonates have evaluated the evidence with regard to the delivery of dental care during pregnancy, with the objective to help ensure optimal outcomes for all pregnant women. Oral Health Care During Pregnancy: A National Consensus Statement was published in 2012 by the National Maternal and Child Oral Health Resource Center at Georgetown University to establish guidelines to enable pregnant women to receive optimal oral health services.9 The statement provides detailed guidance for both prenatal and oral health professionals, advising that preventive, diagnostic, and restorative dental treatment is safe throughout pregnancy and is effective in improving and maintaining oral health. It also offers guidance for health professionals to share with pregnant women that includes the practice of good oral hygiene and healthy eating. Pharmacological considerations are also presented and include indications and contraindications for analgesics, antibiotics, anesthetics, and antimicrobial agents.6,10
State health departments, including California, New York, South Carolina, and Washington, and other state and national professional organizations have also published consensus statements and practice guidelines.4,9,11-17 Typically, these publications have included consensus contributions from professional organizations representing OB/GYN, primary care, pediatrics, nurse-midwives, pediatric dentistry, public health dentistry, and periodontology.
Reports of dental care utilization during pregnancy range from 23% to 35%. Up to a quarter of pregnant women surveyed reported having a dental problem, and of these, only about half sought dental care.6 However, a recent (2016) survey by the Delta Dental Plans Association indicated that 63% of expectant mothers reported visiting a dentist during their pregnancy.18 Underutilization of dental care may be influenced by lack of, or inadequate, dental insurance coverage for lower-income women, other life stressors (eg, unemployment, housing, intimate partner violence, substance abuse), and/or an unwillingness of dental care professionals to render treatment due to reliance on previous recommendations that lacked current evidence-based knowledge.4
For some women, pregnancy is the only time they have medical and dental insurance, providing a unique chance for access to dental care and increased opportunities for oral health.16 Pregnancy also allows the prospect for improved self-care. For example, pregnant women are nearly twice as likely to quit smoking and stay quit than their non-pregnant counterparts.19,20 Furthermore, improved maternal oral health and hygiene has been shown to decrease caries rates in children up to 5 years old.18,21 This may represent a critical time point to allow for intervention that has a long-lasting effect on both maternal and childhood oral health.
Physiologic Changes in the Pregnant Dental Patient
Pregnancy is marked by complex physiologic changes. During pregnancy many temporary shifts occur in the normal mechanisms of a healthy female body, and adaptations occur to accommodate the growing fetus. The most commonly occurring changes and their significance to oral health and dental care are summarized as follows1,2,10:
Cardiovascular system—Blood volume, heart rate, and cardiac output all increase. Smooth muscle relaxation may lead to vasodilation and a reduction in diastolic blood pressure. In the second and third trimesters, supine hypotension syndrome may occur due to the weight of the fetus and uterus compressing the inferior vena cava. Dental significance: Blood pressure monitoring will be useful and should ideally be referenced against that reported by other prenatal healthcare providers. In the second and third trimesters, the patient should be tilted to her left side to relieve pressure on the inferior vena cava.
Respiratory system—Hyper-ventilation, dyspnea, and hypoxia may occur due to increased maternal-fetal oxygen requirements, upward displacement of the diaphragm by the developing fetus, and airway edema. Dental significance:These effects may be exacerbated when in the supine position.
Gastrointestinal system—Nausea and vomiting are the most commonly occurring changes. Gastroesophageal reflux and symptoms of heartburn are common in the later stages and are thought to be the effect of physical changes of the enlarging fetus. Dental significance:Reflux and vomiting increase the risk for acid erosion. For patients suffering morning sickness and nausea, it may be helpful to allow some flexibility in scheduling dental appointments.
Endocrine system—Many alterations occur with significant increases in progesterone and estrogens. For example, sensitivity to insulin may diminish, increasing the risk of gestational diabetes. Dental significance: Food cravings and increased intake are believed to be of hormonal origin and may increase risk for caries and acid erosion. Elevated estrogen may lead to vascular permeability manifesting as increased gingival inflammation, combined with an increased level of periodontal pathogens, specifically Porphyromonas gingivalisand Prevotella intermedia.
Renal system—An increased glomerular filtration rate may lead to a greater need to urinate, which may be exacerbated by pressure of the developing fetus. Dental significance: Consideration of the patient's need for frequent urination should be given during lengthy dental appointments.
Immune system—The immune system adapts to accommodate the fetus and its genetic differences with the mother. Dental significance:Changes in the immune system may also be responsible for an increased response to plaque manifested as pregnancy gingivitis or pyogenic granuloma.
Metabolic system—Daily nutritional requirements increase to support fetal growth. The enlarging uterus, placenta, and developing fetus together with increased body fluids and deposition of fat all contribute to an increase in body weight. Dental significance: Increased appetite may be satisfied by greater amounts and more frequent intake of sugar-containing foods and beverages, leading to an increased risk of dental caries.
Changes in the Oral Cavity During Pregnancy
Soft Tissues
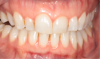
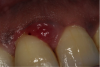
Increased gingival inflammation during pregnancy is due to elevated pathogenicity and/or a higher response by the host to the plaque biofilm.8 Plaque-induced gingivitis is the most common form of periodontal disease, affecting 36% to 100% of pregnant women.22-24 Common conditions present clinically as gingivitis (Figure 1), gingival enlargement, or pyogenic granuloma (Figure 2).
Pregnancy does not cause periodontal disease, but it may exacerbate any current inflammatory condition or predispose the pregnant woman to increased inflammation. If the mother has been diagnosed with periodontitis, the condition might affect the development and overall health of the fetus as a result of plaque microbes or inflammatory mediators released by the host tissues entering the circulation and reaching the placenta.25 Worldwide, 15 million babies are born prematurely each year, and preterm birth ranks as the second-most common cause of death for children less than 5 years old.26 In the United States in 2015, preterm birth affected about one in every 10 infants.27
Pregnant patients should be evaluated to determine their periodontal condition, and those who exhibit signs of gingivitis or pregnancy granuloma or are periodontally compromised should be recalled and reviewed more frequently and given prophylaxis or scaling and root planing as necessary. If these conditions do not resolve after delivery, referral to a periodontist should be considered. Further, the clinician can re-evaluate the need for more frequent maintenance visits and make appropriate recommendations with regard to future at-home self-care and in-office professional care.
An emphasis should be placed on meticulous oral hygiene when gingivitis and/or periodontal conditions such as pregnancy granuloma are present during pregnancy. These conditions may improve with intensive instructions and the use of advanced oral hygiene aids.28 After delivery, resolution occurs in most cases as the body returns to its non-pregnant state.29,30 If complete resolution is not achieved, periodontal referral should be considered.
Hard Tissues
Tooth enamel and exposed dentin may be indirectly affected during pregnancy either by the vomiting associated with early morning sickness or by food cravings. The presence of stomach acid in the mouth causes demineralization and surface softening of both enamel and dentin, which may lead to erosion. Cravings for acidic foods and beverages, such as citrus fruits and juices, or carbonated beverages may also result in erosion.31,32
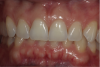
Erosion may initially manifest itself by the symptom of sensitivity and the clinical signs of a smooth, dull enamel surface (Figure 3). Later stages of erosion will appear as cratering of the cervical areas, yellowing as enamel thins, reductions in incisal height, and loss of anatomical features such as grooves and cusps. Erosion due to vomiting most commonly occurs on the palatal surfaces of upper molars and incisors, while erosion due to acidic foods and beverages is less distinct and varies widely.
Delivering Care During Pregnancy
Health history—The standard principles of history-taking, assessment, diagnosis, and treatment planning apply to the pregnant patient as they do for any other dental patient. A variety of additional questions, as listed in Table 1, may be asked when taking the health history of any pregnant patient.
Key advice for oral healthcare—The National Consensus Statement and several other guidelines state that dental professionals should provide reassurance to pregnant patients and those contemplating becoming pregnant that oral healthcare, including radiographs, pain medication, and local anesthesia, is safe throughout pregnancy.9,11-17 This reassurance should include encouragement to continue to seek care, practice effective oral hygiene, eat healthy foods, and attend prenatal classes.
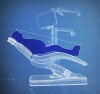
Patient comfort—It can be challenging for the patient to find a comfortable position in the dental chair. However, the National Consensus Statement9 and other reviews1,2 advocate a semi-reclining position in which the head is kept higher than the feet. Frequent position changes should be allowed. In later pregnancy, particularly the third trimester, a small pillow or rolled towel should be placed under the right hip to help the patient avoid dizziness or nausea, as this shifts the weight of the fetus away from the inferior vena cava (Figure 4).
Clinical evaluation—Due to the increased risk of soft- and hard-tissue changes, the clinical evaluation should include emphasis on detecting changes in periodontal, dental caries, and erosion status. Patients who have been seen over many years and have exhibited high levels of plaque control, an absence of gingival inflammation and white spot lesions, and no early signs of erosive tooth wear may suddenly show some or all of these changes. The evaluation should include interview questions regarding morning sickness and the ability to perform early morning oral hygiene, effectiveness of interdental cleaning, and the development of any changes in dietary habits.
Dental health education—Before conception or as early in the pregnancy as opportunity allows, the patient should receive information about the physiologic changes that are commonly encountered, including increased gingival bleeding and enlargement such as pregnancy granuloma, dental caries, and erosion. Topics to discuss with the patient to reduce the risk of these conditions are listed in Table 2.
Provision and scheduling of dental treatment—While necessary procedures can be provided at any stage during pregnancy, it is prudent to avoid scheduling elective dental care in the first trimester and the last half of the third trimester.29 Thus, 14 to 20 weeks of gestation is the ideal time for care.
If scaling and root planing is indicated during pregnancy, local anesthetics in FDA pregnancy category B or C are safe to use. For example, lidocaine and prilocaine are safe as long as they are used at the recommended doses.29 The American Academy of Periodontology has stated that the presence of an acute infection, abscess, or other potentially disseminating sources of sepsis may warrant prompt intervention irrespective of the stage of pregnancy.29 (Authors' note: Pharmacological mechanisms and prescribing suggestions are beyond the scope of this article, which is intended to emphasize the need to provide dental care to women with uncomplicated and healthy pregnancies. More information on the safety and efficacy of pharmacotherapies for pregnant women can be found in the aforementioned National Consensus Statement.) Deferral or refusal of dental care (by either the provider or patient) until after delivery is generally discouraged as the new mother may be preoccupied with the care of her newborn and may find scheduling both her own appointment and a caregiver for her infant a challenge.
After Delivery
Gingival inflammation, including pyogenic granulomas, will generally subside after delivery and the gingival tissues typically will return to their pre-pregnancy state. Likewise, any food cravings that increase risk for caries and acid erosion will likely cease as well, in most cases well before term.1,2,10 If gingival conditions remain, a referral to a periodontist should be considered, especially for the management of any remaining signs of a pyogenic granuloma.
In the case of the first child, the parents will most likely undergo changes in their daily routine and lifestyle and, as such, may neglect their own self-care. They may miss or fail to schedule their own dental appointments due to their natural preoccupation with their new family member. Thus, as one set of risk factors diminishes at delivery, another set emerges that may still compromise the parent's oral health, and these factors must be considered.
Many parents will seek information about the infant's oral health and the appropriate time to commence dental visits. The American Academy of Pediatric Dentistry encourages parents and other care providers to help every child establish a dental home that provides comprehensive, continuously accessible, coordinated, and compassionate care by 12 months of age.33
Summary
During pregnancy, changes occur in many body systems, including the oral cavity. Most of these changes are hormonal or physical and may lead to further changes in the oral tissues such as gingival inflammation and increase the risk of dental caries and acid erosion. A National Consensus Statement and guidelines from numerous other expert groups indicate that routine dental treatment, including taking radiographs, is considered safe during pregnancy. Many pregnant women, members of the prenatal healthcare team, and some dental professionals may be unsure about the safety and appropriateness of dental care during pregnancy. The ideal time for elective care is early in the second trimester. In the later stages of pregnancy, comfort in and the angle of the dental chair is an important consideration.
Due to increased risk of periodontal diseases, dental caries, and acid erosion, good oral hygiene practices are essential and should include twice-daily brushing with a fluoride toothpaste, daily interdental cleaning, and use of fluoride or antimicrobial mouth rinses as indicated.
Dental professionals should be prepared to collaborate with the patient's prenatal care team and advocate for prenatal care and assist in its arrangement for those patients who do not have a prenatal provider. Only a small number of pregnant patients seek dental care, and fewer than half of those who report dental problems during pregnancy pursue care. Collaboration with the prenatal care team may increase dental referrals, and such a channel of communication between the oral health and prenatal communities can benefit maternal and child oral health outcomes.
About the Authors
Irina F. Dragan, DDS, MS
Assistant Professor, Department of Periodontology
and Faculty Practice Provider
Tufts University School of Dental Medicine
Boston, Massachusetts
Valery Veglia, RDH, MBA
Practice Manager
Tufts University School of Dental Medicine
Boston, Massachusetts
Maria L. Geisinger, DDS, MS
Associate Professor
Director
Advanced Education Program in Periodontology
University of Alabama at Birmingham
Birmingham, Alabama
David C. Alexander, BDS, MSc
Principal
Appolonia Global Health Sciences LLC
Green Brook, New Jersey
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Otomo-Corgel J, Steinberg B. Periodontal medicine and the female patient. In: Rose LF, Genco RJ, Cohen DW, Mealey BL, eds. Periodontal Medicine. Hamilton, ON: B.C. Decker; 2000:151-166.
2. Otomo-Corgel J. Systemic considerations for female patients. In: Newman MG, van Winkelhoff AJ, eds. Antibiotic and Antimicrobial Use in Dental Practice. Chicago, IL: Quintessence Publishing; 2001:636-649.
3. Michalowicz BS, DiAngelis AJ, Novak MJ, et al. Examining the safety of dental treatment in pregnant women. J Am Dent Assoc. 2008;139(6):685-695.
4. California Dental Association. Oral Health During Pregnancy & Early Childhood: Evidence-Based Guidelines for Health Professionals. Sacramento, CA: CDA Foundation; February 2010. https://www.cdafoundation.org/portals/0/pdfs/poh_guidelines.pdf. Accessed December 20, 2017.
5. Silk H, Douglass AB, Douglass JM, Silk L. Oral health during pregnancy. Am Fam Physician. 2008;77(8):1139-1144.
6. Gaffield ML, Gilbert BJ, Malvitz DM, Romaguera R. Oral health during pregnancy: an analysis of information collected by the pregnancy risk assessment monitoring system. J Am Dent Assoc. 2001;132(7):1009-1016.
7. Jeffcoat MK, Hauth JC, Geurs NC, et al. Periodontal disease and preterm birth: results of a pilot intervention study. J Periodontol. 2003;74(8):1214-1218.
8. Carrillo-de-Albornoz A, Figuero E, Herrera D, Bascones-Martınez A. Gingival changes during pregnancy: II. Influence of hormonal variations on the subgingival biofilm. J Clin Periodontol. 2010;37(3):230-240.
9. Oral Health Care During Pregnancy Expert Workgroup. Oral Health Care During Pregnancy: A National Consensus Statement. Washington, DC: National Maternal and Child Oral Health Resource Center; 2012.
10. Steinberg BJ, Hilton IV, Iida H, Samelson R. Oral health and dental care during pregnancy. Dent Clin North Am. 2013;57(2):195-210.
11. New York State Department of Health. Oral Health Care During Pregnancy and Early Childhood. Practice Guidelines. August 2006. https://www.health.ny.gov/publications/0824.pdf. Accessed December 20, 2017.
12. South Carolina Oral Health Coalition. Oral Health Care for Pregnant Women. South Carolina Department of Health and Environmental Control. Updated 2017. http://www.scdhec.gov/library/cr-009437.pdf. Accessed December 20, 2017.
13. Association of State and Territorial Dental Directors. Perinatal Oral Health Policy Statement. Adopted July 26, 2012. http://www.astdd.org/docs/perinatal-oral-health-policy-statement-july-26-2012.pdf. Accessed December 20, 2107.
14. Association of State and Territorial Dental Directors. Best Practice Approaches for State and Community Oral Health Programs: Perinatal Oral Health. October 25, 2012. http://www.astdd.org/bestpractices/BPAPernatalOralHhealth.pdf. Accessed December 20, 2107.
15. Connecticut State Dental Association. Considerations for the Dental Treatment of Pregnant Women. A Resource for Connecticut Dentists. 2013. http://www.csda.com/docs/default-source/dental-resources/considerations-for-treating-pregnant-patients.pdf?sfvrsn=2. Accessed December 20, 2017.
16. American College of Obstetricians and Gynecologists. Oral Health Care During Pregnancy and Through the Lifespan. Committee Opinion, Number 569. August 2013, Reaffirmed 2017. https://www.acog.org/-/media/Committee-Opinions/Committee-on-Health-Care-for-Underserved-Women/co569.pdf?dmc=1&ts=20161122T1541218879. Accessed December 20, 2017.
17. American Academy of Pediatric Dentistry. Perinatal and Infant Oral Health Care. Revised 2016. http://www.aapd.org/media/Policies_Guidelines/BP_PerinatalOralHealthCare.pdf#xml=http://pr-dtsearch001.americaneagle.com/service/search.asp?cmd=pdfhits&DocId=470&Index=F%3a%5cdtSearch%5caapd%2eorg&HitCount=10&hits=21+5c+95+d5+d6+2fe+347+34d+370+677+&hc=30&req=perinatal. Accessed December 20, 2017.
18. Delta Dental Plans Association. Number of pregnant women in U.S. getting dental care on the rise. Delta Dental website. May 12, 2016. https://www.deltadental.com/Public/NewsMedia/NewsReleasePregnantWomenOnTheRise201605.jsp. Accessed December 20, 2017.
19. Skjöldebrand J, Gahnberg L. Tobacco preventive measures by dental care staff. An attempt to reduce the use of tobacco among adolescents. Swed Dent J. 1997;21(1-2):49-54.
20. Moher M, Hey K, Lancaster T. Workplace interventions for smoking cessation. Cochrane Database Syst Rev. 2005;(2):CD003440.
21. Köhler B, Andréen I. Influence of caries-preventive measures in mothers on cariogenic bacteria and caries experience in their children. Arch Oral Biol. 1994;39(10):907-911.
22. Löe H, Silness J. Periodontal disease in pregnancy I. Prevalence and severity. Acta Odontol Scand. 1963;21:533-551.
23. Maier AW, Orban B. Gingivitis in pregnancy. Oral Surg Oral Med Oral Pathol. 1949;2(3):334-373.
24. Jensen J, Liljemark W, Bloomquist C. The effect of female sex hormones on subgingival plaque. J Periodontol. 1981;52(10):599-602.
25. Timothé P, Eke PI, Presson SM, Malvitz DM. Dental care use among pregnant women in the United States reported in 1999 and 2002. Prev Chronic Dis. 2005;2(1):1-11. https://www.cdc.gov/pcd/issues/2005/jan/pdf/04_0069.pdf. Accessed December 20, 2017.
26. WHO Media Centre. Preterm birth. Fact sheet 363. World Health Organization website. November 2016, updated November 2017. http://www.who.int/mediacentre/factsheets/fs363/en/. Accessed December 20, 2017.
27. Hamilton BE, Martin JA, Osterman MJ. Births: Preliminary data for 2015. Natl Vital Stat Rep. 2016;65(3):1-15.
28. Geisinger ML, Geurs NC, Bain JL, et al. Oral health education and therapy reduces gingivitis during pregnancy. J Clin Periodontol. 2014;41(2):141-148.
29. American Academy of Periodontology statement regarding periodontal management of the pregnant patient. J Periodontol. 2004;75(3):495.
30. Sanz M, Kornman K; working group 3 of the joint EFP/AAP workshop. Periodontitis and adverse pregnancy outcomes: consensus report of the Joint EFP/AAP Workshop on Periodontitis and Systemic Diseases. J Periodontol. 2013;84(4 suppl):S164-S169.
31. Berkowitz RJ. Causes, treatment and prevention of early childhood caries: a microbiologic perspective. J Can Dent Assoc. 2003;69(5):304-307.
32. Bartlett D. Intrinsic causes of erosion. Monogr Oral Sci. 2006;20:119-139.
33. American Academy of Pediatric Dentistry. Policy on the Dental Home. 2015. http://www.aapd.org/media/Policies_Guidelines/P_DentalHome.pdf. Accessed December 20, 2017.