You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The esthetics of a single-tooth, implant-supported restoration is most often attributable to the soft-tissue architecture that frames the clinical crown.1 In order for an implant-supported restoration to accurately mimic its adjacent natural counterpart, the restorative complex must traverse the peri-implant mucosal tissues and transition from a flat cylindrical implant interface to a scalloped architectural configuration determined by the patient’s gingival attachment level and clinical crown’s cross-sectional anatomy.2
As a result of the inherent disconnect between cylindrical implant interfaces and morphologically derived prosthetic crowns, the clinician and laboratory technician often must collaboratively design a custom, patient-specific transmucosal abutment to unite these different components. Recently, CAD/CAM technology has enabled the production of site- or patient-specific abutments made from various biomaterials.3 An optimally designed and milled custom abutment provides both the clinician and laboratory technician with the opportunity to establish proper prosthetic emergence characteristics, flexibility in biomaterial selection, core and porcelain support, prosthetic draw, and finish-line parameters to enable excess cement removal. When CAD/CAM abutments were compared with stock abutments in anterior sites retrospectively after 2 years of service, CAD/CAM custom abutments resulted in significantly improved soft-tissue stability.4
However, such collaborative design and manufacture of a custom abutment is primarily dependent on the technician receiving an accurate representation of the mature, supported peri-implant mucosal tissue architecture. This transfer of information regarding the soft tissues can be facilitated by implant provisionalization for a period prior to impressioning.5 Subsequently, analog or digital protocols to statically index and transmit the mature peri-implant mucosal architecture to the laboratory can be leveraged to enhance communication and facilitate optimal abutment design.6-9
Once both the implant fixture and surrounding supported soft-tissue complex are simultaneously represented, the clinician-technician collaborative design process can begin. Contemporary digital abutment workflows such as ATLANTIS™ Abutments (DENTSPLY Implants, dentsplyimplants.com) enable the team members to have varying degrees of design control, depending on their respective preferences and comfort level. Initial prescription protocols allow the clinician to demarcate parameters such as the specific implant manufacturer being indexed, abutment material selection (eg, titanium, gold-hue titanium, shaded zirconia), fixation preference (eg, cement-retained, screw-retained), emergence profile design and contour, and marginal finish-line position relative to the mucosal margin. Through use of the Web-based ATLANTIS 3D Editor software, a virtual rendering of the proposed abutment to suit the needs of the restorative team and patient can be viewed before manufacturing without the need to purchase special software. The authors have found such a workflow to be extremely beneficial for enhancing communication during restoration design and fabrication, regardless of the case’s complexity.
Case Presentation
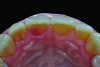
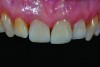
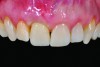
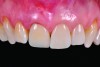
A 57-year-old female was referred to the author’s intramural practice at the University of Iowa College of Dentistry for evaluation of a visually evident, pink lesion associated with the lingual aspect of tooth No. 8 (Figure 1). The patient had no symptoms at the time of the examination. The periodontal status was normal, with isolated areas of facial mucogingival recession (Figure 2). Percussion testing of the maxillary sextant revealed ankylosis of tooth No. 8 based on auditory sounding. A diagnostic cone-beam computed tomography (CBCT) scan was performed. The findings pointed to confirmation of a large external cervical resorption lesion (Heithersay Class IV lesion10) associated with tooth No. 8 (Figure 3), leading to a hopeless long-term prognosis.
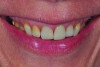
After consultation with the patient regarding these findings, an implant strategy was chosen. The patient was made aware of several esthetic challenges related to her case, including a high smile line (Figure 4), ankylosis of the tooth to be extracted, and long-term maintenance of the alveolar process and associated mucosal topography post-extraction due to a very thin facial cortex of bone labial to tooth No. 8.
After diagnostic models were obtained, the tooth was extracted using an atraumatic extraction kit (Easy X-Trac System, A. Titan Instruments, atitan.com). Despite a successful extraction, an apical fenestration was visualized at the extraction socket apex, and a tunnel approach apical to the mucogingival junction was performed to enable guided bone regeneration simultaneous with site preservation of the extraction socket using a demineralized freeze-dried bone allograft (Puros Cortical Particulate Allograft #8271R, Zimmer Dental, zimmerdental.com) and a collagen plug (CollaPlug, Zimmer Dental). The patient was given an interim Essix appliance to use during the healing phase.
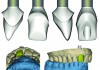
After 12 weeks of healing, a threaded dental implant (OsseoSpeed TX, DENTSPLY Implants, dentsplyimplants.com) measuring 4.5 mm by 11.0 mm was placed in a flapless approach with the aid of a surgical template. The restorative platform of the implant was placed 3.0 mm apical to the planned gingival zenith to provide for adequate transitional contour development with the subsequent interim and definitive abutments. After 6 weeks of healing, a screw-retained, implant-level interim restoration was fabricated in a direct fabrication protocol, using a polyether ether ketone (PEEK) plastic interim abutment (TempDesign 4.5/5.0, DENTSPLY Implants) and bis-acryl provisional material (Protemp Plus, 3M ESPE, 3mespe.com) (Figure 5). After 3 months of healing with the interim restoration and verification of the proper peri-implant mucosal architecture, a customized implant-level impression was made to statically communicate via the master cast the desired contours and finish line of the future patient-specific ATLANTIS abutment.
The maxillary master cast was poured in type IV stone (ResinRock, Whip Mix Corporation, whipmix.com) and scanned with a laboratory-based scanner (Lava™ Scan ST, 3M ESPE) to digitize the master cast. The resulting digital dataset was imported into the ATLANTIS WebOrder software, and a proposed abutment design was sent for review based on the author’s prescription of a zirconia, screw-retained CAD/CAM abutment (ATLANTIS Crown Abutment). Some minor alterations to the initial design of the abutment were made in ATLANTIS 3D Editor, which the technician confirmed prior to milling (Figure 6). Subsequent to milling at the ATLANTIS production facility, the abutment was sent to the technician for application of veneering porcelain (Cerabien ZR, Kuraray Noritake Dental Inc., kuraraynoritake.com) based on a custom shade analysis completed earlier by the technician (Figure 7).
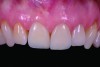
The completed zirconia ATLANTIS Crown Abutment restoration was inserted clinically and evaluated based on several criteria, including mucosal support, coronal form, texture, shade, and occlusion. After all criteria were confirmed, the ATLANTIS Crown Abutment was torqued to 25 Ncm, polytetrafluoroethylene tape was condensed in the screw-access channel, and resin composite (Filtek Supreme Ultra Universal Restorative, 3M ESPE) was used to definitively close the screw-access orifice (Figure 8).
The patient has been followed in the author’s intramural practice for the past 3 years (Figure 9) annually to evaluate prosthetic and mucosal stability, as well as implant marginal bone levels. The bone and mucosa have exhibited excellent stability and lack of inflammation, both due to the ability to screw retain the definitive restoration, the prosthetic connection, and the patient’s excellent oral hygiene. The ability to first shape and support the peri-implant mucosa with an interim restoration during healing and then follow the mucosal outline via an ATLANTIS Crown Abutment has enabled the authors to optimize communication related to the abutment’s design, fabrication, and subsequent customization with porcelain application, leading to an esthetically imperceptible outcome.
Conclusion
Healthcare is increasingly moving toward individualized, patient-centered care to improve outcomes and decrease complications.11 CAD/CAM technologies in dentistry have resulted in an exponential capacity to individualize care, depending on the prosthetic needs of the patient and requirements of the interdisciplinary team. ATLANTIS patient-specific abutments enable both the clinician and laboratory team to individualize each patient’s abutment to meet the unique demands of the case. The capacity to manufacture a single-unit, cement- (ATLANTIS Abutment) or screw-retained (ATLANTIS Crown Abutment) abutment, multiple-unit bar (ATLANTIS ISUS Bar), hybrid framework (ATLANTIS ISUS Hybrid), bridge framework (ATLANTIS ISUS Bridge), or telescopic abutments (ATLANTIS Conus Abutment) to retain an overdenture, enables ATLANTIS to be utilized for a variety of implant prosthetic situations. Coupled with ATLANTIS 3D Editor, such digital workflows enable the clinician and laboratory technician to collaborate and communicate on a higher level and to achieve excellent functional and esthetic outcomes unique to each patient.
Disclosure
This article was supplied by DENTSPLY Implants.
Acknowledgments
The authors thank Derek Borgwardt, DDS, MS, for his surgical expertise and support in the case presented in this article.
References
To view the reference list for this article, go to insidedentaltech.com/idt823
About the Authors
Christopher A. Barwacz, DDS, FAGD
Assist. Professor
The University of Iowa College of Dentistry
Iowa City, Iowa
John Doubet
President
Esthedontics Dental Laboratory
Cedar Rapids, Iowa