You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
In the anterior region, the loss of a tooth raises functional, esthetic, and psychosocial issues for the patient. The general dental practitioner, who often has the first contact with the patient, may collaborate with various clinical specialists to design and execute a comprehensive treatment plan that addresses the patient’s concerns. In recent years, dental implants have become the treatment of choice for replacing a missing tooth. When restoring edentulous spaces in the esthetic zone with dental implants, the adequacy of hard and soft tissues, in terms of height and thickness, are essential for an esthetic and functional implant restoration.1 Hence, this paper aims to discuss dimensional changes of the ridge following tooth removal and methods for ridge preservation and augmentation for implant replacement in the esthetic zone.
Dimensional Changes of the Ridge Following Tooth Removal
The bundle bone is a tooth-dependent structure that consists of collagen fibers inserted from root cementum into alveolar bone. During an extraction, these collagen fibers are severed, leaving a socket defect to heal by secondary intention. Formation of a blood clot, which eventually transforms from granulation tissue to osteoid, occurs with the migration of osteogenic cells and growth factors from the surrounding bony walls. Bone fill starts from the apex of the defect to the coronal portion. At the same time, epithelial cells migrate from the wound edges over the blood clot to seal the entrance of the socket.2 As a result, soft-tissue thickness at an extraction site is increased by 2.1 mm occlusally and 0.4 to 0.5 mm on the buccal and palatal sites.3 However, soft-tissue contour follows the underlying hard-tissue contour. As such, despite the increase in soft-tissue thickness, the contour might not be ideal for an esthetic implant restoration.
Model analysis found that the buccal bone resorbed to a greater extent, thus pushing the center of the ridge palatally or lingually.4 Histological evidence from a canine model showed that after tooth extraction, the bundle bone was resorbed, resulting in greater buccal bone height and width reduction compared to the other surfaces. It was found that at sites with facial bone thickness of ≤1 mm, significant vertical bone resorption of 7.5 mm was measured, as compared to sites with thick facial bone, which had only a 1.1-mm reduction in bone height.5 This phenomenon occurs because the mid-facial buccal bone is generally thinner than the palatal bone,6 has less blood supply, and is thus more prone to resorption.7 A recent systematic review of 20 human clinical trials reported that ridge resorption after tooth extraction occurred mainly in the first 3 months, with horizontal ridge resorption ranging from 29% to 63% (2.46 mm to 4.56 mm) and vertical ridge resorption from 11% to 22% (0.8 mm to 1.5 mm).8 A mid-buccal bone height reduction of 1.67 mm, which could significantly affect the fabrication of an esthetic restoration, was also reported.9 A summary of the features of ridge resorption is provided in Table 1. With this significant amount of bone loss after tooth extraction, the volume of bone available to encase a dental implant in the ideal 3-dimensional (3D), prosthetically driven position is inadequate. Therefore, methods to preserve the ridge dimensions have been proposed.
Methods to Maintain Ridge Dimensions Following Removal of the Tooth
Ridge preservation, defined as maintaining the ridge volume and contour that existed at the time of extraction,10 is important because it allows the implant to be placed in an ideal position with adequate buccal bone thickness and height for an esthetic implant restoration. This can be achieved through several methods, but the first step to prevent excessive bone loss after tooth extraction is to use a minimally traumatic flapless tooth extraction technique. This is because raising a flap separates the periosteum from bone, causing the initiation of a local inflammatory response, which results in increased bone resorption at the extraction site.11 However, a systematic review demonstrated that a flapped surgical procedure for socket augmentation had significantly less horizontal ridge resorption compared to a flapless surgical procedure.12 This was because primary wound closure was achieved.12 Therefore, in sites with severe bone loss, ridge augmentation utilizing bone grafts and membranes can be performed after tooth removal. If primary wound closure is unachievable in these cases, it is preferable to perform ridge augmentation after the soft tissues have healed, thus providing additional soft-tissue coverage over the augmented site. Alternatively, a flapless approach can be used with a nonresorbable polytetrafluoroethylene (PTFE) membrane and bone grafts for socket augmentation. This technique is further elaborated in the next section.
In the flapless approach, it is recommended that the supracrestal fibers first be incised with a 15C scalpel. A periotome is inserted into the periodontal ligament (PDL) space at the proximal surfaces and moved in a bucco-palatal-apical direction to sever the subcrestal fibers and widen the PDL space. To avoid fracturing the buccal bone, the periotome should not be inserted into the buccal surface. A long, narrow, tapered diamond bur on a high-speed handpiece can be used between the bone and root to create space for periotome insertion. When the tooth is significantly mobile, a dental forceps is used with rotational movements to carefully remove the tooth without fracturing the bony walls.
The key factor that determines the need for ridge preservation is the intactness and thickness of the buccal bone after the tooth is removed. As a general principle, well-contained sockets with an intact and thick (≥2 mm) buccal bone do not require additional grafting because the defect has a high regenerative potential.13 Although secondary resorption in the bucco-palatal dimension may occur, as shown in a canine model,7 a recent human study reported no horizontal bone loss and minimal vertical bone loss (1.1 mm) at sites with a thick facial wall of more than 1 mm.5 Therefore, the necessity for socket augmentation at the time of tooth extraction is debatable. In well-contained sockets with an intact and thin (<2 mm) buccal bone, ridge preservation is recommended. This is because of differences in vascularity, leading to greater bone resorption in sites with thin buccal bone compared to sites with thick buccal bone. In the esthetic zone, 90% of the population has an incomplete or thin (<1 mm) buccal bone;6 therefore, most socket defects require ridge preservation.
There are several methods to preserve ridge dimensions following an extraction. The Bio-Col technique was first proposed to preserve ridge anatomy after tooth removal.14 In this technique, the apical two-thirds of the socket was lightly filled with a deproteinized bovine bone matrix that was covered with a collagen plug. The site was sutured with a figure 8 suture and sealed with cyanoacrylate tissue adhesive. It was reported that both hard- and soft-tissue loss was avoided and optimum esthetics was achieved. A similar technique, the mineralized bone allograft-plug augmentation, was later proposed.15 Mineralized human allograft and a collagen plug were used to augment the site. Biopsies of the grafted sites showed 68.5% new bone formation, 3.8% residual graft particles, and 27.7% connective tissue matrix, thus proving the effectiveness of the technique.16
In order to combat resorption of the buccal bone, overbuilding the buccal surface with demineralized freeze-dried bone allograft and bioabsorbable membrane after tooth extraction was proposed.17 However, 39% to 67% of the augmented bone width and 60% to 76% of bone height were lost 4 months later. It was conjectured that additional surgical trauma to the buccal tissues caused the resorption of the augmented bone.18 A modification of this technique, buccal plate augmentation, was designed to prevent alteration of the soft-tissue contour.19 This approach involved placement of bone substitutes in a pouch created between the facial plate and flap, with the site left to heal by secondary intention. The case study reported satisfactory results, but more long-term clinical trials are needed to validate this technique.
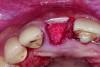
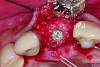
In cases with an incomplete facial plate, the ice cone technique was recommended.20 In this method, a collagen membrane was trimmed to the shape of an ice cone and placed into the socket against the inner aspect of the facial bone. The socket was filled with bone substitutes, and the coronal portion of the membrane was used to cover and protect the underlying bone substitutes. A non-resorbable PTFE membrane can be used for site preservation as well.21 This membrane, if secured to bone, can be left exposed, and epithelialization will occur over it. It was found that sockets grafted with a mineralized bone allograft and PTFE membrane had 47.4% new bone formation and 14.7% residual graft particles. In addition, there was minimum resorption of the buccal bone thickness, as indicated by a 0.3-mm horizontal bone resorption and a 0.25-mm vertical bone resorption.22 A recent systematic review reported that the use of PTFE membranes in ridge preservation shows potential in maintaining ridge dimensions23 and possibly aiding in increasing the zone of keratinized mucosa. Therefore, the use of PTFE membrane may be preferred in ridge preservation of sites in the esthetic zone. Figure 1 and Figure 2 illustrate the use of PTFE membrane in ridge preservation for implant replacement in the esthetic zone. Other authors have also attempted primary closure of the socket or to improve the ridge topography with soft-tissue grafts, but it has not been proven to be effective in increasing bone regeneration.18
The most recent ridge preservation technique, the socket shield technique, involves the removal of most of the tooth, leaving behind a thin buccal fragment of the tooth attached to the buccal bone.24 Subsequently, the implant is placed distal to the root fragment. Histological analysis showed that there is no osteoclastic remodeling of the buccal bone, and new bone was observed between the implant surface and the root fragment. Hence, osseointegration of the implant was not affected by the root fragment.25 Further human clinical trials are needed to validate the long-term effects of this new technique.
Growth factors, such as recombinant human bone morphogenetic protein-2 (rhBMP-2) and platelet-derived growth factor (PDGF), have been used in ridge preservation. In a feasibility study, rhBMP-2 was applied to a collagen sponge and placed into an extraction socket. The regenerated bone was histologically similar to native bone.26 Histological assessment of extraction sockets grafted with a xenograft and 0.3-mg/ml PDGF-BB showed 23% new bone and 9.5% residual grafting material at 4 months post extraction.27 Currently, the evidence supporting the use of growth factors in ridge preservation is limited, and it is necessary to consider the cost-benefit ratio when using these growth factors in clinical practice.
In general, ridge preservation is performed in the esthetic zone to reduce ridge resorption after tooth removal.12 A membrane is used to recreate the facial plate in sites with incomplete facial bone.
Horizontal and Vertical Bone Augmentation
In situations whereby the ridge is deficient in width and height, ridge augmentation is necessary. Several methods were proposed to augment the residual ridge. Due to the complexity of the procedures, clinical scenarios that require block grafts, ridge expansion, and distraction osteogenesis are generally referred to oral surgeons or periodontists. Therefore, this discussion focuses on guided bone augmentation (GBR) as the main method to augment a deficient ridge in the esthetic zone.
Guided Bone Regeneration
The biological mechanism behind GBR is the exclusion of undesirable cells—eg, fibroblasts and epithelial cells—from the wound, in an attempt to facilitate infiltration and colonization of osteoprogenitor cells into the coagulum-filled space beneath the barrier membrane. The “PASS” principle was created as a guideline for clinicians to follow when performing GBR.28 The PASS acronym stands for Primary wound closure, Angiogenesis, Space creation and maintenance, and Stability of the initial blood clot and the implant fixture. Primary wound closure with tension-free sutures provides an enclosed, undisturbed, and stable healing environment away from bacterial and mechanical insults. This greatly enhances the healing capacity of the wound site. Techniques such as flap extensions and cutback incisions can be used to advance a flap so that primary wound closure is attainable,29 in which case angiogenesis would provide an influx of new blood vessels, thus increasing the growth and regeneration of the defect. This can be achieved via decortication, which entails perforating the cortical bone to induce the regional acceleratory phenomenon.30 These perforations also serve as pathways for blood vessels, growth factors, and osteoprogenitor cells to rapidly infiltrate and stabilize the wound site, thus promoting bone regeneration. Space is needed for the osteogenic cells to creep into the wound site, differentiate into osteoblasts, and form woven bone. However, the osteoblasts migrate at a slower pace compared to the epithelial cells. Hence, a bioabsorbable or non-resorbable barrier membrane is used to prevent the unwanted cells from populating the wound site. In addition, bone substitutes are used to maintain the space for bone regeneration. The success of wound healing depends on the stability of initial clot formation. This is because it is a huge reservoir of growth and differentiation factors and also the precursor to granulation tissue, which organizes and remodels to form bone.
This technique can be done prior to or simultaneously with implant placement. It is recommended that staged GBR be performed when the residual ridge width is narrow and primary implant stability is unachievable.31 GBR has been shown to be a predictable method to augment bone horizontally,32-34 and when done simultaneously with implant placement, its success rate was found to range from 79% to 100% after 5 years of function.32 A recent clinical trial evaluating simultaneous GBR with implant placement showed clinically stable peri-implant soft tissues and bone levels, with a mean buccal bone thickness of 1.9 mm. Therefore, esthetically satisfactory treatment outcomes were achieved at the 6-year follow-up visit.35 A recent systematic review reported a vertical bone gain of 2 mm to 8 mm and a complication rate of 45.5%.36 Because of the high complication rate, a meta-analysis found that short implants might be preferable to vertical bone augmentation.37
Soft-Tissue Augmentation
A systematic review demonstrated that implants with an adequate band of peri-implant keratinized mucosa had less mucosal inflammation and recession.38 Therefore, presence of an adequate band of peri-implant keratinized mucosa is beneficial for peri-implant health and ensuring a better long-term, esthetically pleasing treatment outcome. Autogenous, allogenic, or xenogenic grafts can be used for soft-tissue augmentation. To date, autogenous soft tissue grafts yield the most favorable treatment outcomes. Thus, in the highly esthetic region, placement of a subepithelial connective tissue graft is often recommended. Soft-tissue augmentation can be performed before bone augmentation if there is inadequate thickness or width of keratinized mucosa. This is because a thicker flap has greater resistance to incision-line opening39 and thus can provide better coverage and revascularization40 to the underlying bone graft. It can also be performed during the implant uncovering surgery to provide greater soft-tissue thickness, which can be conditioned based on the contours of the implant restoration to provide better esthetics and long-term maintenance of the implant.
Decision Tree
Table 2 shows a decision tree on site preparation for implant replacement in the esthetic zone. An unrestorable tooth in the esthetic zone that will be replaced by an implant-supported restoration should be removed with a minimally invasive technique to preserve the bony contours. After the tooth is removed, a decision to proceed with immediate implant placement or site preservation and early or delayed implant placement must be made. If the socket defect is well contained, with a thick buccal plate (≥2 mm), thick soft tissue (≥2 mm), and primary implant stability can be achieved, immediate implant placement may be attempted. It is important to bear in mind that the implant must be placed in a prosthetically sound 3D position, and it is technically more difficult to do so at an extraction site where the tooth was just removed. This is because implant osteotomy drills tend to shift to the side of least resistance, which in this case, is towards the buccal surface. If the implant is placed buccally, there is an increased risk of mid-facial mucosal recession over time.41 Therefore, due to the technical difficulty in immediate implant placement, it is recommended that the procedure be performed in sites with minimal esthetic concerns.
In sites with an intact and thick (≥2 mm) buccal bone, no grafting is required. A collagen plug may be used for hemostasis at the site of extraction. In sites with an intact and thin (<2 mm) buccal bone, the mineralized bone allograft-plug augmentation technique is preferred because of its effectiveness. For sites with no or incomplete buccal bone, the PTFE membrane can be placed between the bone and buccal soft tissue to form the buccal border. It is subsequently folded over the entrance of the socket, thus serving to contain and protect the bone graft that is placed into the socket. The PTFE membrane is removed 4 weeks after placement,23 and soft tissue will granulate over the site, thus increasing the soft-tissue thickness, which is beneficial for an esthetic implant restoration. Simultaneous or staged GBR, onlay grafts, ridge expansion, or distraction osteogenesis may be used to further augment the residual ridge if necessary. Soft-tissue augmentation can be performed before ridge augmentation or at implant uncovering stage, depending on the soft tissue thickness and width of keratinized mucosa.
Conclusion
As shown in the literature review presented, techniques used to prepare the site for implant replacement in the esthetic zone have yielded favorable outcomes, with GBR being the most promising and best researched. Nonetheless, it is prudent to understand that the key to successful treatment outcomes is to follow biological principles, such as the “PASS” principle, and apply available techniques appropriately. Additionally, augmentation of the soft tissue will aid in achieving a pleasing soft-tissue contour for the implant restoration.
References
1. Belser UC, Schmid B, Higginbottom F, Buser D. Outcome analysis of implant restorations located in the anterior maxilla: a review of the recent literature. Int J Oral Maxillofac Implants. 2004;19 Suppl:30-42.
2. Amler MH. The time sequence of tissue regeneration in human extraction wounds. Oral Surg Oral Med Oral Pathol. 1969;27(3):309-318.
3. Iasella JM, Greenwell H, Miller RL, et al. Ridge preservation with freeze-dried bone allograft and a collagen membrane compared to extraction alone for implant site development: a clinical and histologic study in humans. J Periodontol. 2003;74(7):990-999.
4. Pietrokovski J, Massler M. Alveolar ridge resorption following tooth extraction. J Prosthet Dent. 1967;17(1):21-27.
5. Chappuis V, Engel O, Reyes M, et al. Ridge Alterations Post-extraction in the Esthetic Zone: A 3D Analysis with CBCT. J Dent Res. 2013;92(12 Suppl):195S-201S.
6. Braut V, Bornstein MM, Belser U, Buser D. Thickness of the anterior maxillary facial bone wall-a retrospective radiographic study using cone beam computed tomography. Int J Periodontics Restorative Dent. 2011;31(2):125-131.
7. Araújo MG, Lindhe J. Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol. 2005;32(2):212-218.
8. Tan WL, Wong TL, Wong MC, Lang NP. A systematic review of post-extractional alveolar hard and soft tissue dimensional changes in humans. Clin Oral Implants Res. 2012;23 Suppl 5:1-21.
9. Van der Weijden F, Dell’Acqua F, Slot DE. Alveolar bone dimensional changes of post-extraction sockets in humans: a systematic review. J Clin Periodontol. 2009;36(12):1048-1058.
10. Hämmerle CH, Araújo MG, Simion M; Osteology Consensus Group 2011. Evidence-based knowledge on the biology and treatment of extraction sockets. Clin Oral Implants Res. 2012;23 Suppl 5:80-82.
11. Fickl S, Zuhr O, Wachtel H, Bolz W, Huerzeler M. Tissue alterations after tooth extraction with and without surgical trauma: a volumetric study in the beagle dog. J Clin Periodontol. 2008;35(4):356-563.
12. Vignoletti F, Matesanz P, Rodrigo D, et al. Surgical protocols for ridge preservation after tooth extraction. A systematic review. Clin Oral Implants Res. 2012;23 Suppl 5:22-38.
13. Cortellini P, Tonetti MS. Focus on intrabony defects: guided tissue regeneration. Periodontol 2000. 2000;22:104-132.
14. Sclar AG. Preserving alveolar ridge anatomy following tooth removal in conjunction with immediate implant placement. The Bio-Col technique. Atlas Oral Maxillofac Surg Clin North Am. 1999;7(2):39-59.
15. Wang HL, Tsao YP. Mineralized bone allograft-plug socket augmentation: rationale and technique. Implant Dent. 2007;16(1):33-41.
16. Wang HL, Tsao YP. Histologic evaluation of socket augmentation with mineralized human allograft. Int J Periodontics Restorative Dent. 2008;28(3):231-237.
17. Simon BI, Von Hagen S, Deasy MJ, et al. Changes in alveolar bone height and width following ridge augmentation using bone graft and membranes. J Periodontol. 2000;71(11):1774-1791.
18. Fickl S, Schneider D, Zuhr O, et al. Dimensional changes of the ridge contour after socket preservation and buccal overbuilding: an animal study. J Clin Periodontol. 2009;36(5):442-448.
19. Caiazzo A, Brugnami F, Mehra P. Buccal plate augmentation: a new alternative to socket preservation. J Oral Maxillofac Surg. 2010;68(10):2503-2506.
20. Elian N, Cho SC, Froum S, et al. A simplified socket classification and repair technique. Pract Proced Aesthet Dent. 2007;19(2):99-104; quiz 106.
21. Barber HD, Lignelli J, Smith BM, Bartee BK. Using a dense PTFE membrane without primary closure to achieve bone and tissue regeneration. J Oral Maxillofac Surg. 2007;65(4):748-752.
22. Fotek PD, Neiva RF, Wang HL. Comparison of dermal matrix and polytetrafluoroethylene membrane for socket bone augmentation: a clinical and histologic study. J Periodontol. 2009;80(5):776-785.
23. Carbonell JM, Martin IS, Santos A, et al. High-density polytetrafluoroethylene membranes in guided bone and tissue regeneration procedures: a literature review. Int J Oral Maxillofac Surg. 2014;43(1):75-84.
24. Hurzeler MB, Zuhr O, Schupbach P, et al. The socket-shield technique: a proof-of-principle report. J Clin Periodontol. 2010;37(9):855-862.
25. Baumer D, Zuhr O, Rebele S, et al. The socket-shield technique: first histological, clinical, and volumetrical observations after separation of the buccal tooth segment - a pilot study. Clin Implant Dent Relat Res. 2013;Apr 30. doi: 10.1111/cid.12076. [Epub ahead of print]
26. Fiorellini JP, Howell TH, Cochran D, et al. Randomized study evaluating recombinant human bone morphogenetic protein-2 for extraction socket augmentation. J Periodontol. 2005;76(4):605-613.
27. Nevins ML, Camelo M, Schupbach P, et al. Human histologic evaluation of mineralized collagen bone substitute and recombinant platelet-derived growth factor-BB to create bone for implant placement in extraction socket defects at 4 and 6 months: a case series. Int J Periodontics Restorative Dent. 2009;29(2):129-139.
28. Wang HL, Boyapati L. “PASS” principles for predictable bone regeneration. Implant Dent. 2006;15(1):8-17.9. Greenstein G, Greenstein B, Cavallaro J, et al. Flap advancement: practical techniques to attain tension-free primary closure. J Periodontol. 2009;80(1):4-15.
30. Frost HM. The regional acceleratory phenomenon: a review. Henry Ford Hosp Med J. 1983;31(1):3-9.
31. Fu JH, Wang HL. Horizontal bone augmentation: the decision tree. Int J Periodontics Restorative Dent. 2011;31(4):429-436.
32. Hämmerle CH, Jung RE, Feloutzis A. A systematic review of the survival of implants in bone sites augmented with barrier membranes (guided bone regeneration) in partially edentulous patients. J Clin Periodontol. 2002;29 Suppl 3:226-231; discussion 32-33.
33. Park SH, Lee KW, Oh TJ, et al. Effect of absorbable membranes on sandwich bone augmentation. Clin Oral Implants Res. 2008;19(1):32-41.
34. Buser D, Dula K, Belser UC, et al. Localized ridge augmentation using guided bone regeneration. II. Surgical procedure in the mandible. Int J Periodontics Restorative Dent. 1995;15(1):10-29.
35. Buser D, Chappuis V, Kuchler U, et al. Long-term stability of early implant placement with contour augmentation. J Dent Res. 2013;92(12 Suppl):176S-82S.
36. Rocchietta I, Fontana F, Simion M. Clinical outcomes of vertical bone augmentation to enable dental implant placement: a systematic review. J Clin Periodontol. 2008;35(8 Suppl):203-215.
37. Esposito M, Grusovin MG, Felice P, et al. The efficacy of horizontal and vertical bone augmentation procedures for dental implants - a Cochrane systematic review. Eur J Oral Implantol. 2009;2(3):167-184.
38. Lin GH, Chan HL, Wang HL. The significance of keratinized mucosa on implant health: a systematic review. J Periodontol. 2013;84(12):1755-1767.
39. Burkhardt R, Lang NP. Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study. Clin Oral Implants Res. 2010;21(1):50-54.
40. Wilderman MN, Pennel BM, King K, Barron JM. Histogenesis of repair following osseous surgery. J Periodontol. 1970;41(10):551-565.
41. Evans CD, Chen ST. Esthetic outcomes of immediate implant placements. Clin Oral Implants Res. 2008;19(1):73-80.
42. Johnson K. A study of the dimensional changes occurring in the maxilla following tooth extraction. Aust Dent J. 1969;14(4):241-244.
43. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent. 2003;23(4):313-323.
44. Ashman A. Ridge preservation: important buzzwords in dentistry. Gen Dent. 2000;48(3):304-312.
45. Carlsson GE, Bergman B, Hedegård B. Changes in contour of the maxillary alveolar process under immediate dentures. A longitudinal clinical and x-ray cephalometric study covering 5 years. Acta Odontol Scand. 1967;25(1):45-75.
46. Tallgren A. The continuing reduction of the residual alveolar ridges in complete denture wearers: a mixed-longitudinal study covering 25 years. J Prosthet Dent. 1972;27(2):120-132.
47. Pietrokovski J, Massler M. Ridge remodeling after tooth extraction in rats. J Dent Res. 1967;46(1):222-231.
48. Atwood DA, Coy WA. Clinical, cephalometric, and densitometric study of reduction of residual ridges. J Prosthet Dent. 1971;26(3):280-295.
About the Authors
Jia-Hui Fu, BDS, MS
Assistant Professor
Discipline of Periodontology
Faculty of Dentistry
National University of Singapore
Singapore
Hom-Lay Wang, DDS, MSD, PhD
Professor and Director
Graduate Periodontics
Department of Periodontics and Oral Medicine
School of Dentistry
University of Michigan
Ann Arbor, Michigan