You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Gingival recession (GR) is defined as the displacement of the gingival margin from its normal position to a position apical to the cemento-enamel junction (CEJ).1
Multiple etiological factors are associated with GR; however, vigorous toothbrushing and periodontal disease are considered to be the main ones. In addition, tooth malposition, frenum pull, thin labial bone or bony dehiscence, shallow vestibular depth, occlusal trauma, habits such as nail biting and pen chewing, tongue piercing, iatrogenic factors related to the location of restorative margins, and periodontal procedures have been described as potential causative factors.2
Another factor associated with GR that has been reported in an increasing number of studies in recent years is orthodontic tooth movement. Although most orthodontic treatments do not cause GR or attachment loss, some 10% to 15% of orthodontic patients display GR several years following orthodontic treatment.3-7 This adverse effect might be due to the movement of the root close to the labial alveolar cortical bone or even outside it, creating a zone with thin alveolar bone or even bone dehiscence. Bone dehiscence caused by tooth movement cannot be seen clinically, thus GR is not observable immediately after its development. Gingival tissue covering a dehiscence may recede with time in the presence of inflammation or mechanical toothbrush abrasion and may be detected only years after orthodontic treatment completion.8,9
Post-orthodontic GR most commonly develops around mandibular incisors. Central incisors have been shown to be more affected than lateral incisors.4-7,10,12 For this reason, the present article focuses on the most common scenario encountered by clinicians—ie, post-orthodontic GR of a lower incisor.
Predisposing Factors
The two main predisposing factors for GR are the gingival biotype and the final root position relative to the cortical plates.
Most people may be classified into two gingival biotypes: thin scalloped and thick flat. Individuals who have a thin scalloped biotype are characterized by reduced labial plate thickness, narrower keratinized tissue width, and increased distance from the CEJ to the initial alveolar crest, resulting in a greater tendency for GR than those with a thick biotype.13,14 In the past, it was suggested that the smaller the apico-coronal dimensions of the keratinized gingiva, the higher the risk of developing GR. Newer studies went on to prove that it is not the width but the thickness of keratinized gingiva that is critical around restored or orthodontically moved teeth.1,9,10,15,16 A thin gingiva (<0.5 mm) seems to be the point of least resistance to stresses such as microbial plaque and toothbrush trauma and to increase the risk of GR.10 Wennstrom17 further suggested that it is the thickness of the soft tissue that is more important than its quality (gingiva vs alveolar mucosa).
With regard to the impact of the final root position on the alveolar bone, Wennstrom17 stated that as long as the tooth can be moved within the envelope of the alveolar process, the risk of harmful side effects on the gingival tissues is minimal, regardless of the dimensions of the soft tissues. In contrast, movement of the root towards the labial cortical bone causes stretching and thinning of the gingiva, which increases the risk of GR secondary to orthodontic treatment.8,9 The risk is further increased in patients with thin gingival biotype.18 Yared et al10 found that gingival thickness had greater relevance to recession than final tooth inclination.
Among orthodontists it is generally accepted that proclination of lower incisors subjects patients to an increased risk of future GR.11,19,20 Yared et al10 found that an inclination of the lower incisors in excess of 95º, increased the risk of GR. However, these findings are still controversial.3,6,21 Moreover, a recent study7 showed that retroclination exposed the lower incisors to an increased risk of recession even more than proclination.
Prevention
The clinical implications of the aforementioned studies are that when orthodontic tooth movement is planned and the tooth position is expected to result in an alveolar bone dehiscence, a careful evaluation of the treated site should be performed.
The examination should include:
a. visual evaluation of the gingival thickness
b. palpation of the labial aspect of the marginal gingiva to detect prominent roots (“washboard effect”)
c. risk assessment of the planned tooth movement
d. 3-dimensional imaging to assess labial alveolar bone thickness in high-risk cases
It has been suggested that in patients with a thin biotype, where the risk of developing GR is high, labial augmentation of the marginal gingiva should be considered before the orthodontic treatment as a preventive measure.9,22-25
Treatment
Once GR develops, the indications for treatment are based on cosmetic considerations, cervical hypersensitivity, and prevention of root caries (in caries-susceptible individuals). In cases of moderate-to-severe GR, where acceptable plaque control cannot be performed, inflammation and further periodontal attachment loss may occur. In such cases, the indication for root coverage is to restore periodontal health and prevent periodontal deterioration by changing the topography of the marginal soft tissues to facilitate plaque control.18 Numerous periodontal mucogingival techniques aimed at root coverage have been introduced over the years. Among them are the connective tissue graft, the coronally advanced flap-free gingival graft, the laterally positioned flap, guided tissue regeneration (GTR), allogeneic soft tissue grafts, etc. A decision tree for selecting the most appropriate and predictable soft-tissue grafting procedure has recently been proposed.26
Successful management of post-orthodontic GRs can be achieved by four treatment alternatives:
a. conservative supportive periodontal treatment (SPT) alone
b. orthodontic tooth movement alone
c. periodontal surgical root coverage alone
d. combined orthodontic-periodontal treatment
Decision Tree for Treatment of Localized Post-Orthodontic GR
A decision tree for choosing the best treatment sequence for post-orthodontic GR is proposed in order to guide the practitioners in achieving optimal treatment outcomes (Figure 1).
The etiology of GR should be first identified in an attempt to achieve a successful and stable long-term result. After plaque control and elimination of inflammation in the affected site are attained, any additional adverse factors, such as aggressive toothbrushing, harmful habits, and high frenum pull, should be addressed and eliminated.
In the periodontal literature, the prognosis of the surgical treatment of GR is commonly assessed using Miller’s classification.27 Most post-orthodontic GRs are classified as Miller Class I and II, where the interdental alveolar bone and soft tissues are intact, suggesting that complete root coverage is obtainable.7 However, this classification does not relate to the extent of root prominence and to the inclination of the tooth. Clinical experience shows that achieving full root coverage of prominent roots is challenging. In this context, it has been shown that in a labially positioned tooth with bone dehiscence, bone may re-form and gingival thickness may increase when the tooth is moved lingually, leading to more favorable conditions for surgical root coverage.8,9,28,29
Consequently, the next step in the decision tree, before referring to Miller’s classification, should be a thorough clinical evaluation of the tooth position, which consists of visual and tactile assessment. This visual inspection examines the root position in relation to the alveolar bone and its B-L inclination relative to the adjacent teeth. Next, manual palpation of the labial and lingual gingival contour is performed to inspect the existence and extent of root prominence (“washboard effect”), as well as possible bony dehiscences.
When the tooth is properly aligned within the arch, treatment is managed with reference to Miller’s classification.7 Because most post-orthodontic GR cases are classified as Miller Class I and II defects, the authors focus on the management of these two classes only, and within the scope of this article, Miller Class III and IV defects are not addressed. Surgical root coverage of both Miller Class I and II defects is one treatment choice. However, in Miller Class I cases, a conservative approach can be considered, as well. Such an approach consists of supportive periodontal treatment (SPT)—professional periodic deposit removal every 2 to 3 months during a 1- to 2-year period. The authors’ clinical experience shows that spontaneous root coverage may occur following this conservative approach, particularly in young patients (Figure 2 and Figure 3). Similar results have been reported in a 3-year prospective study in which recession defects healed spontaneously following improvement in oral hygiene standards in children.30 In cases in which no root coverage is observed at the end of the follow-up period, surgical root coverage can be considered.
When teeth with GR present with an increased labial root inclination and prominence, orthodontic correction of tooth position should be then considered. The decision about whether orthodontic treatment is possible depends on the thickness of the bone lingual to the affected root. The only modality to accurately assess the labio-lingual thickness of the alveolar bone is cone-beam computerized tomography (CBCT) imaging. Studies that compared measurements on cadavers and CBCT showed that CBCT measurements are an accurate representation of the clinical bone thickness.31-33
The lingual bone thickness of mandibular permanent teeth in a sample of adolescent and young adults before orthodontic treatment has been reported.34 The measurements were performed on axial sections of CBCT, 4 mm and 8 mm apical to the CEJ. The average lingual bone thickness was 0.79 mm and 1.02 mm for central and lateral incisors, respectively, at 4 mm distance from CEJ. At 8 mm apical to the CEJ, the width increased to 1.81 mm and 1.75 mm for central and lateral incisors, respectively.34 Another study on cadavers reported an average thickness of 2.5 mm and 2.6 mm for central and lateral incisors, respectively, at 6 mm from the alveolar crest, meaning approximately 8 mm distance from the CEJ.35
Based on these data, a minimum of 2.5 mm of lingual alveolar bone thickness, measured on CBCT views at 8 mm apical to the CEJ, is recommended for orthodontic tooth repositioning of a labially displaced root.
It is noteworthy that the facial growth pattern has an influence on the morphology and thickness of the labial and lingual bone plates; patients with a vertical growth pattern (hyperdivergent) exhibit a thinner mandibular symphysis and a thinner alveolar ridge in the anterior region of the mandible compared with patients who have horizontal growth (hypodivergent) or a normal growth pattern.36,37 Therefore, the clinician should be aware that the chances of finding adequate thickness of lingual bone for root repositioning in a long-faced hyperdivergent patient are significantly smaller.
In cases with thin lingual bone, as measured on CBCT (<2.5 mm at a level of 8 mm apical to the CEJ), orthodontic treatment is not advisable, leaving surgical root coverage as the only option. However, the prognosis for this procedure is poorer, because the predominant cause is not addressed. Figure 4 shows the frontal clinical view of a patient with a hyperdivergent growth pattern who presented with post-orthodontic GR of a labially displaced lower central incisor. The sagittal CBCT view (Figure 5) shows complete absence of lingual bone, which contraindicated orthodontic tooth repositioning.
In cases in which adequate lingual bone thickness (≥2.5 mm) is measured on CBCT, orthodontic retreatment should be encouraged (Figure 6 through Figure 8). Most of these patients present with a fixed orthodontic retainer bonded on the lingual aspect of the lower teeth. Therefore, the crown of the affected tooth is splinted and aligned relative to the adjacent teeth, while only the root is displaced toward the labial alveolar plate. Consequently, the orthodontic movement should consist of lingual root torque around a center of rotation placed in the crown. The torque can be easily achieved with rectangular wires or torqueing springs inserted underneath a heavy round base arch, which provides anchorage from the neighboring teeth.
It should be understood that this type of orthodontic movement requires reinsertion of a fixed orthodontic appliance in the lower arch for several months. Therefore, many of these patients reject retreatment. In such cases, surgical root coverage remains the only viable option; however, patients should be aware of the poor prognosis for complete root coverage and be prepared to accept compromised treatment outcomes (Figure 9 through Figure 11).
When the patient agrees to orthodontic retreatment, the recommended treatment sequence is determined by the patient’s Miller’s classification.
In Miller Class I recessions, orthodontic tooth movement alone may be sufficient. After correction of root position, spontaneous root coverage may occur, making surgical intervention superfluous (Figure 12 and Figure 13). However, if residual recession persists, the practitioner can choose either to follow up the case with SPT for 1 to 2 years, aiming for further spontaneous improvement, or proceed directly to surgical root coverage.
In Miller Class II cases, a combined orthodontic-periodontal treatment is usually needed. The orthodontic correction generally reduces the M-D dimensions of the GR, thus creating more favorable conditions for the success of the surgical root coverage, as shown in the case presented. It has been shown that defect size is a factor that limits the complete success of mucogingival root coverage procedures.38
In the case report below, a patient with post-orthodontic GR was successfully treated with the combined orthodontic-periodontal approach.
Case Report
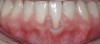
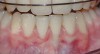
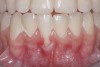
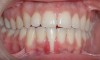
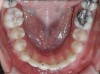
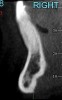
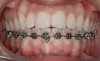
A 19-year-old female complaining of gingival recession in the lower right central incisor presented to the authors’ clinic 5 years after completion of orthodontic treatment. The clinical evaluation showed Miller Class II GR accompanied by gingival inflammation (Figure 14). Two years later, despite conservative periodontal treatment, the GR had worsened (Figure 15). The occlusal view shows the presence of a fixed lingual retainer and a significant labial displacement of the root of the affected incisor (Figure 16 and Figure 17). At this stage, orthodontic treatment was considered. The patient was referred for CBCT, which showed no labial bone coverage of the root but 2.5 mm lingual bone thickness at 8 mm distance from the CEJ (Figure 18). After 6 months of orthodontic treatment with fixed appliances (Figure 19), the B-L inclination of the affected tooth was corrected (Figure 20). The frontal clinical view shows narrowing of the GR (Figure 21). Surgical coverage of the exposed root was subsequently performed by connective tissue graft (Figure 22). A long-term stable and esthetic result was achieved (Figure 23).
Conclusion
The four options for treatment of post-orthodontic gingival recessions of lower incisors include: conservative periodontal treatment, orthodontic tooth movement alone, periodontal surgical root coverage alone, and a combined orthodontic-periodontal treatment. The decision tree proposed is designed to facilitate the clinician in choosing the most appropriate approach for a successful and long-term stable treatment outcome.
REFERENCES
1. Wennström JL. Mucogingival considerations in orthodontic treatment. Semin Orthod. 1996;2(1):46-54.
2. Wennstrom JL, Zucchelli G, Prato GPP. Mucogingival therapy-periodontal plastic surgery. In: Lindhe J, Lang NP, Karring T, eds. Clinical Periodontology and Implant Dentistry. Oxford, UK: Blackwell Munksgaard; 2008:955-1028.
3. Djeu G, Hayes C, Zawaideh S. Correlation between mandibular central incisor proclination and gingival recession during fixed appliance therapy. Angle Orthod. 2002;72(3):238-245.
4. Renkema AM, Fudalej PS, Renkema A, Kiekens R, Katsaros C. Development of labial gingival recessions in orthodontically treated patients. Am J Orthod Dentofacial Orthop. 2013;143(2):206-512.
5. Allais D, Melsen B. Does labial movement of lower incisors influence the level of the gingival margin? A case-control study of adult orthodontic patients. Eur J Orthod. 2003;25(4):343-352.
6. Melsen B, Allais D. Factors of importance for the development of dehiscences during labial movement of mandibular incisors: a retrospective study of adult orthodontic patients. Am J Orthod Dentofacial Orthop. 2005;127(5):552-561; quiz 625.
7. Vasconcelos G, Kjellsen K, Preus H, Vandevska-Radunovic V, Hansen BF. Prevalence and severity of vestibular recession in mandibular incisors after orthodontic treatment. Angle Orthod. 2012;82(1):42-47.
8. Steiner GG, Pearson JK, Ainamo J. Changes of the marginal periodontium as a result of labial tooth movement in monkeys. J Periodontol. 1981;52(6):314-320.
9. Wennström JL, Lindhe J, Sinclair F, Thilander B. Some periodontal tissue reactions to orthodontic tooth movement in monkeys. J Clin Periodontol. 1987;14(3):121-129.
10. Yared KF, Zenobio EG, Pacheco W. Periodontal status of mandibular central incisors after orthodontic proclination in adults. Am J Orthod Dentofacial Orthop. 2006;130(1):6 e1-8.
11. Artun J, Krogstad O. Periodontal status of mandibular incisors following excessive proclination. A study in adults with surgically treated mandibular prognathism. Am J Orthod Dentofacial Orthop. 1987;91(3):225-232.
12. Artun J, Grobéty D. Periodontal status of mandibular incisors after pronounced orthodontic advancement during adolescence: a follow-up evaluation. Am J Orthod Dentofacial Orthop. 2001;119(1):2-10.
13. Kassab MM, Cohen RE. The etiology and prevalence of gingival recession. J Am Dent Assoc. 2003;134(2):220-225.
14. Cook DR, Mealey BL, Verrett RG, et al. Relationship between clinical periodontal biotype and labial plate thickness: an in vivo study. Int J Periodontics Restorative Dent. 2011;31(4):345-354.
15. Ericsson I, Lindhe J. Recession in sites with inadequate width of the keratinized gingiva. An experimental study in the dog. J Clin Periodontol. 1984;11(2):95-103.
16. Dorfman HS. Mucogingival changes resulting from mandibular incisor tooth movement. Am J Orthod. 1978;74(3):286-297.
17. Wennström JL. The significance of the width and thickness of the gingiva in orthodontic treatment. Dtsch Zahnarztl Z. 1990;45(3):136-141.
18. Zhur O, Hurzeler M. Treatment of gingival recession. In: Plastic-Esthetic Periodontal and Implant Surgery: A Microsurgical Approach. Hanover Park, IL: Quintessence Publishing Co. Ltd.; 2012:266-267.
19. Hollender L, Rönnerman A, Thilander B. Root resorption, marginal bone support and clinical crown length in orthodontically treated patients. Eur J Orthod. 1980;2(4):197-205.
20. Joss-Vassalli I, Grebenstein C, Topouzelis N, Sculean A, Katsaros C. Orthodontic therapy and gingival recession: a systematic review. Orthod Craniofac Res. 2010;13(3):127-141.
21. Ruf S, Hansen K, Pancherz H. Does orthodontic proclination of lower incisors in children and adolescents cause gingival recession? Am J Orthod Dentofacial Orthop. 1998;114(1):100-106.
22. Foushee DG, Moriarty JD, Simpson DM. Effects of mandibular orthognathic treatment on mucogingival tissues. J Periodontol. 1985;56(12):
727-733.
23. Coatoam GW, Behrents RG, Bissada NF. The width of keratinized gingiva during orthodontic treatment: its significance and impact on periodontal status. J Periodontol. 1981;52(6):307-313.
24. Maynard JG. The rationale for mucogingival therapy in the child and adolescent. Int J Periodontics Restorative Dent. 1987;7(1):36-51.
25. Holmes HD, Tennant M, Goonewardene MS. Augmentation of faciolingual gingival dimensions with free connective tissue grafts before labial orthodontic tooth movement: an experimental study with a canine model. Am J Orthod Dentofacial Orthop. 2005;127(5):562-572.
26. Leong DJ, Wang HL. A decision tree for soft tissue grafting. Int J Periodontics Restorative Dent. 2011;31(3):307-313.
27. Miller PD Jr. A classification of marginal tissue recession. Int J Periodontics Restorative Dent. 1985;5(2):8-13.
28. Karring T, Nyman S, Thilander B, Magnusson I. Bone regeneration in orthodontically produced alveolar bone dehiscences. J Periodontal Res. 1982;17(3):309-315.
29. Engelking G, Zachrisson BU. Effects of incisor repositioning on monkey periodontium after expansion through the cortical plate. Am J Orthod. 1982;82(1):23-32.
30. Andlin-Sobocki A, Marcusson A, Persson M. 3-year observations on gingival recession in mandibular incisors in children. J Clin Periodontol. 1991;18(3):155-159.
31. Timock AM, Cook V, McDonald T, et al. Accuracy and reliability of buccal bone height and thickness measurements from cone-beam computed tomography imaging. Am J Orthod Dentofacial Orthop. 2011;140(5):734-744.
32. Patcas R, Markic G, Muller L, et al. Accuracy of linear intraoral measurements using cone beam CT and multidetector CT: a tale of two CTs. Dentomaxillofac Radiol. 2012;41(8):637-644.
33. Fu JH, Yeh CY, Chan HL, et al. Tissue biotype and its relation to the underlying bone morphology. J Periodontol. 2010;81(4):569-574.
34. Garib DG, Yatabe MS, Ozawa TO, da Silva Filho OG. Alveolar bone morphology under the perspective of the computed tomography: defining the biological limits of tooth movement. Dent Press J Orthod. 2010;15
(5):192-205.
35. Han JY, Jung GU. Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans. J Periodontal Implant Sci. 2011;41(2):60-66.
36. Tsunori M, Mashita M, Kasai K. Relationship between facial types and tooth and bone characteristics of the mandible obtained by CT scanning. Angle Orthod. 1998;68(6):557-562.
37. Beckmann SH, Kuitert RB, Prahl-Andersen B, et al. Alveolar and skeletal dimensions associated with overbite. Am J Orthod Dentofacial Orthop. 1998;113(4):443-452.
38. Sterrett JD. The management of large mucogingival defects with an “epithelial embossed” connective tissue graft. Int J Periodontics Restorative Dent. 2008;28(6):577-583.
ABOUT THE AUTHORS
Stella Chaushu, DMD, PhD
Department of Orthodontics, Hebrew University-Hadassah, School of Dental Medicine
Jerusalem, Israel
Ayala Stabholz, DMD
Department of Periodontics, Hebrew University-Hadassah School of Dental Medicine
Jerusalem, Israel