You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Controversy has existed in dentistry for years about the “ideal” occlusal vertical dimension (OVD), its loss due to wear, and the predictability of restorative alteration. Practitioners were taught that increasing OVD should be avoided at all costs. Early discussion of vertical dimension painted it as an immutable position. It was postulated that the mandibular rest and speech positions were established shortly after birth and did not change throughout life.1 It was further claimed that there was an optimal neuromuscular position and alteration would lead to pain and dysfunction.2 Poorly designed research in the 1970s and 1980s confirmed these fears.3,4 One problem with the projects was that they increased the OVD only on posterior teeth without anterior contact. Patients reported increased headaches, muscle fatigue, and parafunction. Additionally, the original OVD would reestablish itself by posterior tooth intrusion.4 However, when the anterior teeth were included in the bite opening, the muscles adapted quickly and the rest position reestablished within 1 week.5,6 Currently, most professionals have concluded that humans are very adaptable and can tolerate many different vertical dimensions of their bite within reasonable limits.7,8 While the controversy has been quelled, the trepidation over the technical steps required to reliably increase patients’ OVD still remains. This article will attempt to address some of the more confusing aspects of altering the OVD and offer solutions to improve predictability.
Determining a New OVD
There have been a wide variety of techniques proposed for determining the proper OVD. While a discussion of all of the techniques is beyond the scope of this article, some of the more popular techniques will be discussed. Fabrication of an occlusal appliance to evaluate an increased vertical dimension is a classic prosthodontic technique. Practitioners produce a traditional stabilizing splint adjusted to centric relation. It is to be worn the majority of the day for many weeks. The concept is that the patient is “test-driving” the increased vertical. If the proposed vertical were beyond their physiologic limit of adaptation, clinicians would expect the patient to present with muscle pain, joint discomfort, or headaches. While this seems intuitive, it is not grounded in the literature. There are virtually no papers demonstrating that altering vertical dimension will produce pain in either muscles or joints that last more than 1 to 2 weeks in duration.6 Think of the situation in reverse. If a patient reports to a dental practice with muscle, joint, or headache symptoms, the treatment to relieve the discomfort is to fabricate a stabilizing splint at an increased vertical dimension. Since altering vertical dimension will not produce pain, a trial splint, while it may provide joint resolution and muscle deprogramming, does not provide information on vertical dimension.9 Another common technique is to work only within the patient’s freeway space. This is the distance between the maxillary and mandibular teeth when the mandible is in repose or physiologic rest. It is taught that this space is normally between 2 mm to 4 mm. Students are warned that if this freeway space is violated, the patient will make premature contact with their teeth, increasing the risk of ceramic fracture, muscle pain, and lack of adaptation. It has, however, been demonstrated that when the vertical is altered and obliterates the freeway space, it reprograms almost immediately to the new occlusal relationship.10-12 Because freeway space is recaptured at any vertical opening, it cannot be used as a guide for selecting a working vertical dimension. Finally, many clinicians believe that establishing adequate space for posterior restorations should be used as the primary determinant of OVD. If the vertical dimension of the rehabilitation is chosen by separating the posterior teeth for restorative room, the practitioner runs the risk of losing appropriate anterior guidance. Research on altering vertical dimension isolated the coupling of the anterior teeth as an important component for predictability.5,6 When vertical dimension was increased without anterior coupling, the results were unpredictable. The difficulty is that OVD is not simply altered vertically; it is opened on an arc. This arc has two important effects. First, when the posterior teeth are separated by 1 mm, the mandibular rotation can disocclude the anterior teeth by 3 mm or more.7,9 Patients requiring posterior restoration may introduce a significant opening of the anterior teeth. Simply adding length and contour may not resolve the discrepancy. This is highlighted in the second rotational effect. For every 1 mm the anterior teeth are separated, the mandibular anteriors move 2 mm posteriorly. The risk clinicians run using posterior restorative space as a guide is not having appropriate contact anteriorly as the teeth rapidly move away from one another.
While all of these techniques have been used successfully, they nonetheless have obvious flaws. These deficiencies highlight the fact that patients are extremely adaptable and that there is no single correct vertical dimension. How, then, should clinicians determine the appropriate restorative dimension for their patient? The simplest way to establish an acceptable vertical dimension is to let the anterior teeth become the primary determinant with facial esthetics and phonetics being secondary determinants.7-9 Because the patient’s esthetic desires and the dentist’s functional goals should be the focus, communicating the proper incisal edge position and angle of guidance to the laboratory becomes essential.
Laboratory Communication
Complex restorative dentistry is a compilation of multiple simple steps in which errors compound exponentially. This is especially true when opening vertical dimension. Interdisciplinary communication is not limited to dental specialties but extends to the laboratory. Restorative dentists must provide the laboratory with an accurate representation of the patient’s mouth, registrations required for mounting, photographs necessary for smile analysis, and a proposed anterior tooth length. Common dentist–laboratory communication errors include:
1. Inaccurate Diagnostic Casts
The foundation of the rehabilitation is accurate casts. This is not limited to impressions of prepared teeth; just as important are the preoperative casts. They will be used in the diagnostic waxing and provisional matrix fabrication. Replicating occlusal detail on subjects with aggressively worn teeth and damaged restorations can be a challenge. Casts with occlusal distortions, missing information, or that are poorly poured will lead to mounting and waxing errors. Provisionals will be produced that cannot mimic the features of the laboratory product. Rudd13 outlined the keys for successful alginate impressioning and cast fabrication. A review of these guidelines is recommended. Alginate substitutes are equally accurate when used correctly.
2. No Facebow Transfer
The goal of the facebow registration is to register the anterior–posterior and vertical relationship of the maxilla to the transverse horizontal axis and to transfer this information to the articulator. A transfer error in the horizontal or vertical relationship can result in esthetic error. Failure to transfer the proper anterior–posterior relationship can result in significant errors in the occlusion.14 Unfortunately, the use of a facebow has been reported to be as low as 29.64% for general dentists in private practice, while prosthodontists’ use rate is reported to be as high as 96.22%.15 Complex rehabilitation dentistry at an increased OVD must begin with the use of a facebow.
There are two classifications of facebows: kinematic and arbitrary. The kinematic facebow has the advantage of precision. The registration relates the maxilla to the true hinge axis. One of the advantages of the greater mounting accuracy is that vertical dimension changes made on the articulator will be replicated intraorally given that the articulated casts reproduce the patient’s arc of closure. The disadvantage to a kinematic facebow is that a pantographic tracing is required to locate the true rotational center of the condyle before the facebow can be made. This step is outside the traditional practice of the majority dentists. The earbow facebow provides an arbitrary positioning of the maxillary cast. The arbitrary axis is recorded 95% of the time within 5 mm of the true hinge axis.16 Therefore, the earbow places the casts within a range of acceptability in a majority of cases. This allows for simulated occlusal movement and small modifications of vertical dimension on the articulator. Because the positioning is arbitrary, each case will present variable levels of accuracy. Therefore, casts that are opened and closed on the articulator are subject to positional error. Operators may find that when the casts have been vertically altered, the wax-up may not relate well to the mouth.
3. Lack of Direction on Tooth Positioning and Gingival Alteration
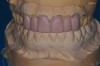
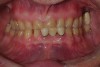
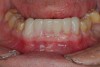
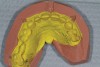
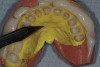
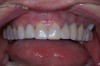
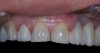
Practitioners must inform the laboratory of the proper amount of incisal edge addition. This decision must be made in the operatory during repose, smiling, and speaking. Robbins has outlined many of these principles.17 These are not static choices that can be made on mounted casts. While photographs of the patient are important for the laboratory, the ultimate decision should rest with the restorative dentist. In addition, if surgical alteration of the gingival architecture is planned, clinicians should mark proposed surgical alteration of the gingival levels on the casts. The laboratory can adjust the stone to mimic the change on the diagnostic wax-up (Figure 1 and Figure 2).
4. Inaccurate or Missing Interocclusal Records
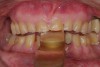
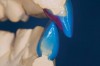
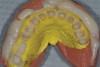
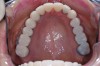
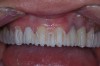
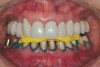
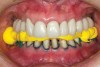
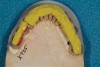
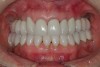
The registration of the transverse hinge axis and transfer with a facebow simply serves to locate the maxillary cast on the articulator. An accurate registration of centric relation allows the laboratory to mount the mandibular cast in a repeatable position for the purposes of reconstruction.18 Commonly, interocclusal records provided to the laboratory are with teeth in contact or the laboratory is asked to hand-articulate without the benefit of a bite registration. Besides a lack of repeatability, casts mounted in contact must be separated to a working vertical dimension. Because the earbow/facebow mounting is an arbitrary positioning of the maxilla, the casts will routinely not be on the same arc of closure as found intraorally. This means that as the casts are separated there is the possibility of a significant anterior–posterior shift.19 The error compounds the farther from the true hinge axis the facebow was fabricated and the greater the casts are opened on the arbitrary arc. Because of this magnifying error, Gracis suggests that interocclusal records should be fabricated at the vertical dimension that they will be rehabilitated.19 Dentists should visualize the ideal incisal edge position of the maxillary incisors and their ability to couple at the proposed vertical. Evaluating the patient’s central incisor display in repose and full smile arrives at this position.17 The author then uses a leaf gauge to separate the anterior teeth enough to accommodate the additional length (Figure 3 through Figure 5). The leaf gauge has the additional benefit of allowing the interocclusal registration to be fabricated with a seated condyle. This is obviously an arbitrary choice. The laboratory technician will alter the position during the diagnostic wax-up. Due to the fact that the registration is fabricated in an open relationship, the amount of modification in the OVD on the articulator will be significantly less. This will minimize the error found in wax-ups fabricated from a closed interocclusal record.
Laboratory Technique for Altering Vertical Dimension
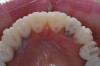
Spear has outlined a laboratory technique to determine if worn anterior teeth can be restored at the existing vertical dimension or if an increase in vertical is required.9 For the purposes of this article, it is assumed that both arches require reconstruction and a proposed OVD has been recorded and transferred to the articulator. The laboratory phase begins by waxing the incisal edge of the maxillary centrals to the proposed length. The lingual is added to ideal contour without the mandibular incisors playing a role in design (Figure 6). Without the casts occluding, the mandibular incisors are waxed to the level of an ideal occlusal plane (Figure 7). At this point, the waxed teeth are closed together and the proposed vertical dimension is evaluated. The incisal pin will either stay on the incisal table or rise from it. If the incisal pin touches the table and the teeth are in contact, the vertical proposed is accepted (Figure 8).
If the incisal pin is on the table and the teeth are out of occlusion (Figure 9), the proposed vertical may be reduced. Lowering the incisal pin reduces the space available in the posterior for restoration. In addition, the risk inherent in altering the vertical dimension on the articulator is that the anterior–posterior shift in the arch relationship may affect the occlusion when placing the provisionals. Contour may be added to the lingual surface of the maxillary teeth (Figure 10). Thicker lingual contours may alter the patient’s ability to phonate clearly. This is a secondary concern and cannot be evaluated until provisionalization. Length may be added to the incisal edges of the mandibular anteriors. This will obviously alter the occlusal plane and could deepen the Curve of Spee. Lastly, a combination of maxillary and mandibular addition (Figure 11) can be done.
When the waxed teeth are occluded, if the incisal pin rises off the table, accept the increased vertical dimension over the proposed vertical dimension and lower the pin to touch the table. The risks previously noted with altering the OVD apply. The maxillary lingual surface may be modified to reduce contour. Available restorative space must be included in this decision. The mandibular incisal edge height may be reduced and the Curve of Spee flattened. A combination of maxillary and mandibular alteration can also be done.
Once the vertical dimension has been accepted, the remaining maxillary teeth are contoured to provide a smooth continuation of incisal edges from anterior to posterior. The ideal occlusal plane will have a 3° to 7° inclination from anterior to posterior.20 The distal–lingual cusp of the maxillary first molar and lingual cusps of the maxillary second molar will incrementally rise off of a flat plane (Figure 12).
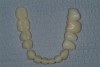
The mandibular teeth are then waxed into a proper occlusal relationship. The mandible, however, does not have the advantage of the palate as a stop for a provisional matrix. Once the teeth are prepared, the dentist lacks a solid bilateral stop to verify positioning of the matrix. This makes it extremely difficult to reproduce the wax-up intraorally. One solution is to complete the mandibular wax-up in stages. If the mandibular anteriors are created first, then a matrix can be produced to complete the anterior provisionals using the posterior teeth as the stop (Figure 13). The posterior teeth are then waxed and a complete arch matrix is fabricated. This allows the mandibular anterior teeth to be prepared and provisionalized in centric relation at the vertical dimension of the wax-up (Figure 14). The posterior teeth can then be prepared and the anterior provisionals are used as the positioning stop for the posterior provisionals (Figure 15).
After the diagnostic wax-up and provisional matrixes are prepared, practitioners must still deal with three problems unique to rehabilitation dentistry at an altered vertical dimension.
Transferring the Diagnostic Design from the Articulator to the Provisionals
A considerable amount of time has been spent in the laboratory producing a working wax-up of the provisional restorations. That time is wasted if the wax-up is not transferred to the mouth at the same anterior–posterior and vertical dimension. Two types of matrix materials can be used depending on the type of provisional to be fabricated. The first is a clear polyvinyl siloxane matrix material that is used for direct bonded composite veneer provisionals. The advantages are the ability to visualize the seating of the matrix and if composite is used for the provisional it may be light-cured through the matrix. The second is a two-stage putty wash matrix. This is appropriate for Bis-acryl and acrylic provisionals. The external putty is rigid. It prevents marginal flexure and distortion. The wash provides the details of the wax-up.
A problem with all matrixes is that the resin may not exit rapidly enough to prevent being trapped when the matrix is seated. This trapped resin prevents complete seating and will introduce error to the provisionals. Routinely, these provisionals will be high in occlusion and must be aggressively adjusted. These adjustments can destroy the precision of the work done in the laboratory. A possible solution is to create deep escape vents in the matrix beyond the free gingival margin (Figure 16). Multiple vents are required in a full-arch provisional. This allows an easy escape for the excess resin and allows more ideal positioning. Dentists may verify seating by evaluating the thickness of resin captured on the palate in the maxilla or on the tooth stops in the mandible (Figure 17 and Figure 18). If an excess amount of acrylic remains, then the provisional is high and the vertical dimension and occlusion of the wax-up have not been transferred. Rather than grinding resin haphazardly, the provisional should be remade with more vents cut to improve seating.
Some additional tips for improved rehabilitation provisionals include creating a midline notch in matrix. This is used as a seating guide. When lined up with the maxillary or mandibular frenum, it helps to eliminate the uncertainty of the proper horizontal alignment of the matrix. When injecting, the tip of the Bis-acryl material’s syringe should be placed in the matrix near the incisal edges and the flow monitored to ensure that all of the embrasures are filled (Figure 19). This will minimize problems with voids at the incisal embrasures and occlusal cusp tips. The Bis-acryl should then be injected around finish lines of the preparation before seating the matrix. This step ensures good capture of the marginal detail. After removal, the Bis-acryl will possess a slimy oxygen-inhibited layer. Make any void repairs and correct marginal misfits before removing this layer. The oxygen-inhibited layer should be removed with alcohol before trimming. This leaves a hard surface that trims easily without a powdery residue.
Difficulty Judging Reduction
It is difficult for practitioners to know exactly how much reduction is required when the teeth are worn and malpositioned. It becomes especially demanding when the vertical dimension is being increased. Without a reduction guide, clinicians must simply guess at the proper amount of reduction, all the while mentally factoring in the proposed vertical alteration. Clinicians may under-reduce the teeth leading to esthetic compromises and/or overcontoured restorations or over-reduce yielding endodontic complications and/or tooth fracture. A simple reduction guide may be fabricated quickly and accurately using the modified provisional matrix. After the patient has been anesthetized, the matrix is filled with a fast-set Bis-acryl material and seated. Once the matrix is removed, a resin guide will remain on the teeth captured by the interproximal undercuts (Figure 20 and Figure 21). Reduction burs are used on the matrix to demonstrate the proper space for ceramic or metal (Figure 22 and Figure 23). The shell is then peeled from the teeth. The depth cuts transferred to the teeth act a guide for reduction (Figure 24). Extremely malpositioned teeth may require a separate matrix to be fabricated to account for the additional reduction required.
Accurate Interocclusal Records
One of the most difficult procedures in rehabilitation dentistry is the interocclusal—or bite—registration. This is especially true when working at an altered vertical dimension. It is important that practitioners plan the sequencing of impressioning and interocclusal record fabrication at the beginning of treatment rather than make it more difficult through poor planning. When possible, clinicians should attempt to use properly adjusted and sectioned provisionals as a platform for the interocclusal record and make sectional registrations.
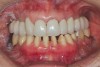
Provisionals waxed to a centric relation position must be adjusted to the same position intraorally. Once the provisionals are adjusted to an acceptable static occlusal relationship, the eccentric adjustments are made. Before cementation, restorative dentists should have a plan for the bite registration. The provisionals are sectioned into units allowing for easy access for impressioning and providing enough teeth for a solid registration. This usually means sectioning the full-arch provisionals at the distal of the canines or first bicuspids, but will vary according to the unique characteristics of each case (Figure 25).
After creating casts of the provisionals for the laboratory, the sectional bite technique calls for the removal of a portion of the provisionals and fabrication of an interocclusal record. Usually practitioners begin in the anterior, making it easier to verify when the registration is reseated properly. Once that section is recorded, it should be trimmed to eliminate tissue contact and deep details. Both may keep the registration from reseating properly. The remaining provisionals are removed, the sectional interocclusal registration is reseated, and the preparation reduction verified (Figure 26 through Figure 28). Registration material is then placed over the remaining sections as the patient returns to a closed position. There are two important technique notes. First, the new registration material should not be allowed to overlap the existing registration. If the material overlaps, it will alter the vertical orientation of the casts and create instability in the mounting (Figure 29). If necessary, practitioners should make the registration in three distinct sections to prevent this error. Second, the patient is instructed to bite half-hard into the matrix. Without a solid posterior stop, a firm bite will overseat the condyle and the occlusion will be impacted. A half-hard bite will minimize the condylar displacement and maintain a proper interocclusal relationship (Figure 30 and Figure 31).
Conclusion
While it should be accomplished with care, increasing vertical dimension is an occasionally necessary component of rehabilitation dentistry. Altering OVD is not traditional dentistry for most practices and requires significantly more accuracy in records and greater communication with the laboratory. Because provisional restorations allow evaluation of the proposed esthetics and function, they are an important part of the overall treatment. Relationships developed on properly designed wax-ups at an increased vertical dimension must be transferred to the mouth accurately. Guidelines were provided in this article for designing and altering a provisional matrix to ensure that the provisionals copy the detail of the wax-up. The provisionals may also act as a guide for proper reduction of tooth structure and maintaining a proper anterior–posterior and vertical relationship during the fabrication of an interocclusal registration.
References
1. Silverman MM. Accurate measurement of vertical dimension by phonetics and the speaking centric space. Part 1. Dental Digest. 1951;57:261-265.
2. Beyron HL. Characteristics of functionally optimal occlusion and principles of occlusal rehabilitation. J Am Dent Assoc. 1954;48:648-656.
3. Christensen J. Effect of occlusion-raising procedures on the chewing system. Dent Pract Dent Rec. 1970;20:233-238.
4. Ramfjord SP, Blankenship JR. Increased occlusal vertical dimension in monkeys. J Prosthet Dent. 1981;45:74-83.
5. Carlsson GE, Ingervall B, Kocak G. Effect of increasing vertical dimension on the masticatory system in subjects with natural teeth. J Prosthet Dent. 1979;41:284-289.
6. Gross MD, Ormianer Z. A preliminary study on the effect of vertical dimension increase on mandibular postural rest position. Int J Prosthodont. 1994;7:216-226.
7. Kois JC, Phillips KM. Occlusal vertical dimension: alteration concerns. Compend Contin Educ Dent. 1997;18:1169-1177.
8. Mack RM. Vertical dimension: A dynamic concept based on facial form and oropharyngeal function. J Prosthet Dent. 1991;66:478-485.
9. Spear FM. Approaches to vertical dimension. Advanced Esthetics & Interdisciplinary Dentistry. 2006;2:2-12.
10. Rugh JD, Drago CJ. Vertical dimension: a study of clinical rest position and jaw muscle activity. J Prosthet Dent. 1981;45:670-675.
11. Hellsing G. Functional adaptation to changes in vertical dimension. J Prosthet Dent. 1984;52:867-870.
12. Ormianer Z, Gross M. A 2-year follow-up of mandibular posture following an increase in occlusal vertical dimension beyond the clinical rest position with fixed restorations. J Oral Rehab. 1998;25:877-883.
13. Rudd KD, Morrow RM, Strunk RR. Accurate alginate impressions. J Prosthet Dent. 1969;22:294-300.
14. Pitchford JH. A reevaluation of the axis-orbital plane and the use of the orbital in a facebow transfer record. J Prosthet Dent. 1991;66:349-355.
15. Clark DM, Oyen OJ, Feil P. The use of specific dental school-taught restorative techniques by practicing clinicians. J Dent Educ. 2001;65:760-765.
16. Schallhorn RG. A study of the arbitrary center and the kinematic center of rotation for face-bow mountings. J Prosthet Dent. 1957;7:162-169.
17. Robbins JW. Esthetic diagnosis by the numbers. Tex Dent J. 2002;119:1170-1172.
18. McKee JR. Comparing condylar position repeatability for standardized versus nonstandardized methods of achieving centric relation. J Prosthet Dent. 1997;77:280-284.
19. Gracis S. Clinical considerations and rationale for the use of a simplified instrumentation in occlusal rehabilitation. Part 1: Mounting of the models on the articulator. Int J Periodontics Restorative Dent. 2003;23:57-67.
20. L’Estrange PR, Vig PS. A comparative study of the occlusal plane in dentulous and edentulous subjects. J Prosthet Dent. 1975;33:495-503.
About the Author
Jeffrey S. Rouse, DDS
Private Practice Prosthodontist
Clinical Adjunct Associate Professor,
Department of Graduate Prosthodontics
University of Texas Health Science Center San Antonio Dental School
San Antonio, Texas