You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Introduction
Managing congenitally missing or microdontic lateral incisors presents multiple challenges and requires numerous considerations to achieve an optimal result. The incidence of agenesis in the North American population is estimated to be 3.9%, with a higher incidence in females than males.1 Statistics regarding the prevalence of maxillary lateral incisor microdontia (peg lateral) as opposed to hypodontia are not readily available.
Tooth development, or lack thereof, directly impacts the development of the alveolar bone as well as the maxillofacial skeleton.2 Upon recognizing maxillary lateral incisor hypodontia in a growing child, decisions must be made regarding space closure and cuspid substitution or space opening and prosthetic replacement. Though polarized opinions exist on the subject, the literature reveals that varied esthetic, periodontal, and functional considerations do not establish one approach as uniformly superior or preferential to the other.3,4 As such, the capabilities and limitations of both solutions should be evaluated prior to establishing the best course of action for an individual patient’s situation. In a growing child, opportunities for guiding the development of the alveolar ridge and the maxillofacial skeleton allow for a broader array of potential treatment solutions. Once the facial skeleton has reached skeletal maturity, choices for treatment solutions are typically narrowed to fit within the framework of the gross confines of the existing osseous architecture.
Space Considerations
Lateral incisors have height-to-width proportionality similar to central incisors but their overall size is smaller than that of the central incisors. The golden proportion is often mentioned as a guideline to proportional relationship between the central and lateral incisors. However, it is important to note that the proportional relationship suggested by the concept of golden proportion is a visual relationship as opposed to a dimensional one. Tooth widths, as viewed from the front of the patient, are altered by perceptual influences of tooth rotation, tooth position, and arch form. There is also increased incidence of morpho-dimensional alteration of the central incisors in patients with congenitally missing lateral incisors, which often results in a rectangular instead of a trapezoidal shape.5 Therefore, consideration must also be given to the size and shape of the central incisors in these patients before their morphology is used as a basis for decisions regarding the morphology of the lateral incisors.
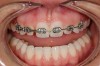
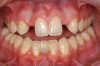
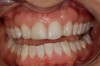
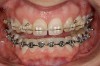
The average width of a lateral incisor is 6.5 mm, but size varies greatly from one patient to the next and even within the same patient.6 The opportunity to vary lateral incisor tooth width can work to the clinician’s advantage and allow other critical components, such as creating harmony with the facial midline or managing the occlusion, to also have a beneficial influence in the decision-making process (Figure 1 through Figure 5).7 The maxillary and mandibular inter-arch relationships must be taken into consideration when deciding the desired width of congenitally missing or malformed lateral incisors. Appropriate amounts of overbite and overjet are needed to satisfy functional requirements and strongly influence decisions regarding space. Cognizance regarding occlusal relationships and the remaining and varied growth potential of children can help lessen the incidence of future occlusal problems.
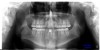
If an implant-supported crown is part of the proposed treatment plan, adequate intra-radicular space, in addition to adequate coronal space, must be ensured. As the coronal tooth structure of the central incisor and cuspids are orthodontically separated, the apices of these teeth tend to converge. Care must be taken in the finishing process to assure that the root position allows adequate room for implant placement (Figure 6 and Figure 7). However, due to the patient’s age and the need to wait for skeletal maturity prior to implant placement, several years can elapse between the completion of orthodontic treatment and implant placement. Despite best efforts, unfavorable changes can occur. Post-orthodontic root approximation due to continued vertical growth, compensatory eruption, or inadequate retention occurs in about one in 10 patients to a degree significant enough to prevent implant placement without additional orthodontic treatment prior to implant placement.8
Implant placement should be centered between the adjacent teeth and allow for 1.5 mm of distance between the fixture and adjacent roots. Root form implants as small as 3.0 mm allow placement in restricted spaces but often come with compromises of which clinicians should be aware. Smaller implants have less surface area available for osseointegration and significantly less tensile and bending strength.9 Prosthetic limitations of smaller implants include an absence of manufacturer-supplied provisional abutment systems and an inability to utilize a zirconia abutment to support the definitive restoration. Optimizing fixture length and minimizing functional forces on the final restoration would appear to be prudent if narrow diameter implants remain the only option for providing an implant-supported restoration.
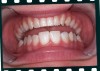
If cuspid substitution is the treatment of choice, considerations must be made to create visual harmony between the central incisors and the cuspids substituted as lateral incisors. This may be done by increasing the width of the central incisors, decreasing the width of the cuspids, or a combination of both. In addition, the vertical position of the cuspids should be modified to best represent the gingival architecture of lateral incisors (Figure 8 through Figure 12).
Ridge Considerations
Edentulous spaces typically result in a deficient alveolar ridge. In 1983 Siebert classified ridge defects into three categories.10 Class I and Class III defects constitute the majority of defects, 33% and 56% respectively.11 Class I defects offer an opportunity for soft-tissue manipulation or grafting by the restorative dentist or specialist. Class III defects may require multiple hard- and soft-tissue grafting procedures as well as orthodontic extrusion of the adjacent teeth to effect vertical changes to papillae. Class III defects are exponentially more complicated to treat to an ideal result and, therefore, require greater skill on the part of the restorative/surgical team and greater commitment by the patient.10,12 Edentulous site development through hard- and/or soft-tissue grafting not only serves to harmonize the prosthetic replacement of a missing tooth within the framework of a natural dentition but in the case of implants, may be necessary to achieve adequate osseous contours for proper fixture placement (Figure 13). Site development can be incorporated into orthodontic treatment of adolescent patients with missing teeth and has been shown to be effective and dimensionally stable.13
Evaluation of the papillae height and radiating symmetry is imperative. The papillae should have a radiating symmetry in which the peak moves in an apical direction when proceeding distally from the midline.14-16 Papilla height primarily relates to the height of the osseous crest of the adjacent tooth.17 The height and shape of the papilla is secondarily influenced by lateral support and biotype. Loss of papilla height on either side of an edentulous site is common. Some of the tissue loss arises from the lack of lateral support created by the absent crown form, but significant contour loss typically reflects remodeling of the adjacent crestal bone. While lateral support can be recreated prosthetically, the vertical loss of interproximal bone height can only predictably be positively altered with orthodontic extrusion (Figure 14).
Gingival Architecture
It is generally agreed that the maxillary incisal plane follows the natural curvature of the lower lip when smiling. The free gingival margin zenith of the maxillary teeth should be parallel to both the incisal edge and the curvature of the lower lip. The free gingival margin of the maxillary lateral incisors can be on the same level as or slightly coronal to a line drawn between the central incisors and canines but should not be positioned apical to this line. Situations where the clinical crowns are not fully exposed due to the patient’s age or delayed passive eruption need to be rectified prior to making definitive decisions about implant position or pontic site development.
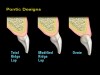
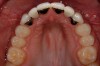
The subgingival contours of the prosthetic tooth replacement, be it a pontic or an implant-supported crown, are important. Ovate pontic forms give rise to lateral support as well as support of the facial free gingival margin and are recommended for use when replacing a missing tooth with a fixed bridge (Figure 15).18 The shape of ovate pontic forms are easily cleaned by the patient on a daily basis and are more conducive to ideal tissue health. The subgingival contours of an implant-supported crown must not be over-contoured or they will give rise to a displacement of the surrounding tissues apically.19 This is also true for an ovate pontic.
Restorative Phase
Long-term provisional restorations to replace congenitally missing lateral incisors may be removable or fixed (Figure 16 through Figure 20). Fixed restorations (typically adhesively retained to prevent unnecessary loss of tooth structure) aid in improved retention of the desired tooth positions.
Several options are available to definitely restore situations that involve congenitally missing lateral incisors. Retained primary lateral incisors or cuspids that are in the lateral incisor position can be altered to resemble the morphology of the permanent lateral incisors with direct (Figure 21 and Figure 22) or indirect restorations. Implants and implant-supported crowns provide a conservative approach that demonstrate long-term predictability as well as provide exceptional esthetics.20 Adhesively retained fixed partial dentures provide less long-term predictability but can still be an esthetic option that is conservative of tooth structure. Fixed partial dentures, while at one time used extensively to replace congenitally missing lateral incisors, are less frequently seen as the treatment of choice due to the need to remove tooth structure from the adjacent teeth.
Conclusion
The management of maxillary lateral incisor agenesis involves multiple considerations and various disciplines. Functional and esthetic parameters play key roles in directing treatment protocols. Orthodontics and restorative dentistry are typically incorporated into the treatment plan regardless of the approach chosen to best manage the missing or malformed tooth/teeth. Younger patients typically have greater treatment options than fully mature patients. Treatment times can span many years and retention is not always predictably maintained. The best treatment solutions predictably and conservatively satisfy the functional and esthetic requirements of the patient.
References
1. Polder BJ, Van’t Hof MA, Van der Linden FP, Kuijpers-Jagtman AM. A meta-analysis of the prevalence of dental agenesis of permanent teeth. Community Dent Oral Epidemiol. 2004;32(3):217-226.
2. Meazzini MC, Donati V, Garattini G, Brusati R. Maxillary growth impairment in cleft lip and palate patients: a simplified approach in the search for a cause. J Craniofac Surg. 2008;19(5):1302-1307.
3. Robertsson S, Mohlin B. The congenitally missing upper lateral incisor. A retrospective study of orthodontic space closure versus restorative treatment. Eur J Orthod. 2000;22(6):697-710.
4. Armbruster PC, Gardiner DM, Whitley JB Jr, Flerra J. The congenitally missing maxillary lateral incisor. Part 1: esthetic judgment of treatment options. World J Orthod. 2005;6(4):369-375.
5. Olivadoti A, Doldo T, Treccani M. Morpho-dimensional analysis of the maxillary central incisor clinical crown in cases of congenitally missing upper lateral incisors. Prog Orthod. 2009;10(1):12-19.
6. Wheeler, RC. Textbook of Dental Anatomy and Physiology. Philadelphia, PA and London, England: WB Saunders Co.; 1947.
7. Chiche GJ, Pinault A. Replacement of deficient crowns. In: Esthetics of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence Publishing: 1994:53-73.
8. Olsen TM, Kokich VG Sr. Postorthodontic root approximation after opening space for maxillary lateral incisor implants. Am J Orthod Dentofacial Orthop. 2010;137(2):158-159.
9. Quek CE, Tan KB, Nicholls JI. Load fatigue performance of a single-tooth implant abutment system: effect of diameter. Int J Oral Maxillofac Implants. 2006;21(6):929-936.
10. Seibert JS. Reconstruction of deformed, partially edentulous ridges, using full thickness onlay grafts. Part I. Technique and wound healing. Compend Contin Educ Dent. 1983;4(5):437-453.
11. Abrams H, Kopczyk RA, Kaplan AL. Incidence of anterior ridge deformities in partially edentulous patients. J Prosthet Dent. 1987;57(2):191-194.
12. Seibert JS. Reconstruction of deformed, partially edentulous ridges, using full thickness onlay grafts. Part II. Prosthetic/periodontal interrelationships. Compend Contin Educ Dent. 1983;4(6):549-562.
13. Kokich VG. Maxillary lateral incisor implants: planning with the aid of orthodontics. J Oral Maxillofac Surg. 2004;62(9 suppl 2):48-56.
14. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence Publishing; 1994.
15. Fradeani M. Esthetic Analysis, A Systematic Approach to Prosthetic Treatment. Chicago, IL: Quintessence Publishing; 2004.
16. Goldstein, RE. Change Your Smile. Chicago, IL: Quintessence Publishing; 1997.
17. Kois JC. Altering gingival levels: The restorative connection Part I: biologic variables. J Esthet Dent. 1994;6(1):3-7.
18. Garber DA, Rosenberg ES. The edentulous ridge in fixed prosthodontics. Compend Contin Educ Dent. 1981;2(4):212-223.
19. Salama H, Salama M, Garber D, Adar P. Developing optimal peri-implant papillae within the esthetic zone: guided soft tissue augmentation. J Esthet Dent. 1995;7(3):125-129.
20. ADA Council on Scientific Affairs. Dental endosseous implant: an update. J Am Dent Assoc. 2004;135(1):92-97.
This article was supported by an unrestricted educational grant from Kerr Corporation.