You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Artificial intelligence (AI) has become a transformative force across numerous sectors, including healthcare. In dentistry, the integration of AI is redefining how care is delivered, managed, and optimized. From diagnostic precision to administrative automation, AI tools are enhancing safety, efficiency, and profitability within dental practices. As dental providers face rising operational costs, workforce shortages, and increasing patient demands, leveraging AI offers a strategic pathway to modernize services while maintaining quality and compliance.
Recent years have seen AI applications expand well beyond early diagnostic imaging tools to encompass specialty-specific treatment planning for implantology and orthodontics, ambient scribing technologies that reduce administrative burden, and sophisticated revenue cycle management platforms. This article explores how AI can enhance five key areas of dental practice management: patient safety, scheduling, operations, marketing, and finances.1,2
Enhancing Patient Safety With AI
AI enhances patient safety in dentistry primarily through improved diagnostics, clinical decision support, and treatment monitoring. AI-enabled imaging systems can detect caries, periodontal disease, and oral cancers earlier and with greater accuracy than traditional radiographic methods.1 These systems utilize deep learning algorithms trained on thousands of annotated images to identify pathology that might be missed by human clinicians.3
The evidence for AI-assisted diagnostics continues to build. Systematic reviews and meta-analyses confirm that AI tools can improve readers’ sensitivity for caries detection on radiographs, with reported accuracies ranging from 82% to 94% for caries detection, 85% to 92% for periodontal disease assessment, and 88% to 96% for oral lesion identification.4 US Food and Drug Administration (FDA)–cleared tools such as Overjet Caries Assist – Pediatric (FDA 510[k] number K233738) and Pearl Second Opinion® have demonstrated performance improvements in multi-reader, multi-case clinical studies.5,6 AI assistance has shown particular value for less-experienced readers, helping reduce inter-clinician variability in diagnosis.
Real-world deployment reviews, however, caution that performance can decline without careful integration protocols and ongoing clinician oversight, underscoring that FDA clearance is a necessary but not sufficient condition for safe clinical use.7,8
Clinical decision support tools integrated into electronic health records (EHRs) provide real-time alerts about drug interactions, allergies, and contraindications.2 These systems help clinicians make safer prescribing decisions and adhere to evidence-based protocols. AI-driven risk assessment models can also stratify patients based on their likelihood of complications, enabling more personalized preventive care.3
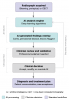
Figure 1 provides an AI-assisted radiographic diagnostic workflow, illustrating the step-by-step clinical pathway from radiograph acquisition through AI analysis, clinician review, and treatment planning.
Safety is further improved through the automation of sterilization tracking and infection control protocols.9 AI can monitor compliance with hand hygiene and instrument sterilization through image recognition or radio frequency identification (RFID) technologies. AI-powered monitoring systems can analyze video footage to assess whether dental assistants are following hand hygiene policies or properly cleaning operatories between patients.4 AI-driven audit tools can flag discrepancies in cleaning logs, ensuring accountability and reducing human error.
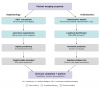
Beyond standard diagnostic imaging, AI has demonstrated growing utility in specialty-specific treatment planning. In implantology, AI-assisted analysis of cone-beam computed tomography (CBCT) scans can automatically segment critical anatomical structures, including the inferior alveolar nerve, identify optimal implant positioning, and predict osseointegration outcomes, with studies reporting up to 96% agreement with expert surgical planning strategies.10 In orthodontics, AI-powered cephalometric analysis tools consistently achieve 95% to 98% landmark identification accuracy, enabling more reliable predictions of tooth movement and treatment duration for both fixed appliances and clear aligner therapy.11 These specialty applications represent some of the most clinically impactful uses of AI in dentistry, moving the technology from passive diagnostic support into active procedural guidance. AI systems can also flag patients who may require premedication due to systemic conditions, suggest diagnostic follow-ups, or generate simulation models to predict treatment outcomes.3 These tools promote evidence-based care and reduce clinical oversights. Figure 2 provides AI-assisted workflows for implantology and orthodontics.
A notable success case involves an FDA-cleared AI platform that supports radiograph analysis. In dental practices using this platform, clinicians have reported significantly increased diagnostic accuracy and greater case acceptance among patients.4,5 Nevertheless, Lal et al caution that practices have encountered patient harm and complaints when over-relying on AI imaging tools that lack proper clinical validation or robust integration protocols—a reminder that deployment conditions matter as much as the underlying algorithm.12
While promising, these applications must be accompanied by ethical safeguards to ensure that AI does not override professional judgment or compromise patient autonomy.5 Ensuring transparency in AI-generated recommendations, maintaining clinician oversight, and safeguarding data privacy are essential components of responsible AI use.
Intelligent Scheduling and Patient Flow
Effective scheduling is crucial in dentistry, as optimizing chairtime can significantly affect productivity and patient satisfaction. AI-powered scheduling systems use predictive analytics to forecast appointment durations, identify patterns of late arrivals or no-shows, and optimize provider calendars accordingly.6 By analyzing historical data, these systems can match appointment types with the best time slots and allocate resources efficiently.7
Peer-reviewed research in dental and healthcare settings confirms that machine-learning models can predict no-shows with meaningful discrimination, supporting targeted reminder strategies and intelligent overbooking approaches.13-15 Studies specifically in dental patient populations show that variables, including appointment lead time, patient demographics, and prior no-show history, can be combined into models that outperform simple reminder-only interventions. Importantly, the effectiveness of these models depends heavily on local data quality; models trained in one setting may not generalize to others, requiring practices to invest in training and validating systems on their own patient populations.16
Automated reminder systems using AI chatbots or natural language processing can confirm appointments, answer basic patient questions, and reschedule cancellations in real time.17 These tools can help improve communication, reduce front-desk workload, and increase attendance rates. For AI chatbots to be effective, they must achieve a high level of conversational sophistication. Research comparing dentist-provided and chatbot-provided answers to dental questions finds that while chatbots can match dentists on factual accuracy, they often fall short on empathy and nuanced communication.17 Practices should therefore pilot chatbot platforms carefully, evaluating natural dialogue quality and ensuring escalation pathways to human staff for complex interactions.
Some platforms use AI to manage waitlists dynamically, filling last-minute cancellations with eligible patients on standby.18 Others integrate with telehealth systems to convert missed in-person appointments into virtual consults, preserving revenue and continuity of care.19
In a widely cited industry example, the Simbo.ai platform helped a multilocation dental group reduce scheduling gaps by approximately 25% using AI-based reminders and rescheduling workflows.20 However, separate implementations in practices with fragmented data ecosystems have failed to replicate these gains, demonstrating that no-show prediction and scheduling AI is only as effective as the quality and completeness of the underlying patient data.6
AI also enables intelligent overbooking strategies. By analyzing historical attendance patterns, AI can identify low-risk opportunities for double-booking, helping to fully utilize providers’ time without increasing patient wait times. AI systems can automatically block time for complex procedures or high-need patients, reducing disruptions and improving overall workflow.7
In group practices or dental support organizations (DSOs), centralized AI scheduling can balance patient demand and provider availability across multiple locations, enhancing operational scalability and improving access to care in underserved communities.17 A potential drawback, however, is the risk of reduced personalization. When scheduling is driven primarily by algorithm across a large multisite network, individual patient preferences, provider familiarity, and relationship-based scheduling may be deprioritized. Practices implementing centralized AI scheduling should build in mechanisms for patient preference capture and human override to preserve the personal touch that underpins patient loyalty and retention.
Operational Efficiency and Workflow Optimization
AI is able to streamline many administrative and clinical tasks and enhance the overall workflow of a dental practice. One of the most impactful applications is automated charting and clinical documentation. AI-driven voice recognition systems can transcribe and structure clinical notes in real time, reducing the time clinicians spend on data entry.21 These systems can also populate standard templates, insert International Classification of Diseases (ICD) and Current Dental Technology (CDT) codes, and summarize patient encounters.21
Among the most significant recent operational advances is the emergence of ambient AI—technology that works continuously in the background to capture clinical information without requiring discrete clinician interaction. Unlike earlier voice-to-text tools that required activation and manual correction, ambient AI platforms listen to chairside conversations in real time, automatically populate clinical notes, and can surface treatment opportunities—such as implant or orthodontic candidacy—directly from routine radiographic review within the same workflow. Early adopters report meaningful reductions in after-hours documentation time and more complete clinical records.22
Several ambient AI platforms designed specifically for dentistry have emerged, such as Bola AI (Bola Technologies), Denti.AI Scribe (Denti.AI), and Voice Notes (VideaHealth). Bola AI offers voice-powered documentation, including ambient transcription and structured charting, with verified integration into Dentrix, Eaglesoft, and Open Dental practice management systems.
Denti.AI Scribe, which is used by major DSOs including Aspen Dental and Elite Dental Partners, combines ambient clinical documentation with voice periodontal charting, generating structured SOAP (subjective, objective, assessment, and plan), operative, and hygiene notes from natural clinical conversations. Launched in 2025, VideaHealth’s Voice Notes platform similarly captures chairside conversations and populates clinical notes in real time, integrating directly with leading practice management systems.23 As these platforms mature, ambient AI is poised to become a standard operational layer in modern dental practice.
Inventory and supply chain management also benefit from AI. Predictive models can forecast inventory needs based on usage trends and automatically reorder supplies, reducing stockouts and excess ordering. AI platforms can flag anomalies—such as sudden increases in material usage— that may indicate procedural changes, mismanagement, or theft.15
In human resources, AI tools can help balance workloads by analyzing appointment types, staff availability, and patient flow to create optimal daily schedules. Some systems provide real-time dashboards to track performance metrics, identify bottlenecks, and suggest operational adjustments.17 This level of insight enables managers to fine-tune staffing models, improve team productivity, and reduce overtime.
AI also enhances clinical standardization. By analyzing treatment outcomes across providers, AI can identify best practices and reduce variability in care delivery.3 Benchmarking tools powered by AI can flag outliers in productivity, treatment plan acceptance rates, or complication rates, allowing for targeted performance improvement initiatives.
AI-based task management systems can further automate patient follow-ups, postoperative care reminders, and hygiene recall scheduling.17 These automated systems reduce missed revenue opportunities and ensure continuity of care. Machine learning models can optimize operatory turnover times and suggest schedule adjustments in real time to improve clinic throughput.15 However, practices using unsupported or poorly integrated voice-to-text and documentation tools have reported increased documentation errors and patient follow-up failures—a caution that any AI implementation requires robust onboarding, validation, and ongoing quality review.21
AI-Driven Marketing and Patient Engagement
Marketing in dentistry has shifted from traditional channels to digital platforms, where AI plays a critical role in targeting, engagement, and retention. AI algorithms analyze data from websites, social media, and search engines to identify prospective patients and deliver personalized advertising.20 Predictive analytics can identify high-value patient segments and craft campaigns tailored to their specific needs.24
Reputation management platforms use AI to monitor online reviews, analyze sentiment, and recommend responses.17 These tools help practices maintain a strong online presence and respond promptly to feedback. AI systems can alert teams to trends in patient dissatisfaction, enabling proactive service recovery before problems compound.
AI enhances patient engagement through personalized email campaigns, educational content recommendations, and satisfaction surveys.24 By integrating behavioral data, these systems deliver content that aligns with patient interests and treatment needs. A patient who viewed whitening content online may receive a follow-up email with personalized information on whitening procedures and available promotions. Generative AI is also beginning to enable dynamic, personalized patient education materials and before/after treatment visualization tools that can be tailored during chairside consultations—helping patients visualize proposed outcomes in real time and improving case acceptance.25
Practices must exercise caution with behavioral data collection, however. The line between helpful personalization and intrusive data mining is thin. Patients who feel their browsing or health-related behavior is being tracked without clear consent may react negatively, eroding rather than building trust.5 All marketing data uses must be transparently disclosed in patient consent agreements and fully compliant with Health Insurance Portability and Accountability Act (HIPAA) and Federal Trade Commission (FTC) advertising guidelines.
Chatbots powered by AI provide real-time support for new and returning patients, answering questions about services, insurance, directions, and appointment availability while maintaining consistent messaging.17 This capability frees up staff for more complex tasks and extends office hours digitally. AI also supports conversion rate optimization; by tracking website behavior, AI can suggest changes to layout, content, and calls-to-action to increase inquiries and appointment bookings.17 Data-driven marketing campaigns powered by AI analytics consistently outperform generic advertising, offering better return on investment and more sustainable patient growth.3
Financial Management and Revenue Optimization With AI
AI is transforming the financial operations of dental practices by automating billing, improving claims processing, and supporting revenue forecasting. Automated coding tools analyze clinical documentation to assign accurate procedure codes, reducing errors and denials.15 Claims management platforms use machine learning to flag anomalies, detect patterns consistent with potential fraud, and optimize reimbursement workflows.6
AI-driven claims denial prevention is an increasingly valuable tool in practice finance. Platforms now analyze historical denial patterns by payer, procedure code, and documentation characteristics to identify submissions at high risk of rejection before they are submitted, enabling proactive correction. This predictive approach can substantially reduce denial rates and the administrative cost of rework, directly improving net revenue.15
AI-driven revenue cycle management tools can predict cash flow, analyze payer behavior, and identify underperforming services.3 This allows practices to make data-driven decisions about pricing, service mix, and operational adjustments.17 Budgeting and expense tracking are enhanced by AI platforms that categorize spending, detect irregularities, and offer financial planning insights. These tools can project the ROI of new investments, such as the adoption of new equipment or the expansion of service lines.8
Financial reporting tools can use natural language processing to generate real-time, customizable dashboards for dentists and practice managers, supporting budgeting, forecasting, and strategic planning.17 AI also enhances collections processes: predictive analytics can identify which patients are most likely to delay or default on payments, prompting early outreach or alternative payment plan offers. This proactive approach reduces accounts receivable aging and improves cash flow.25
In multisite practices and DSOs, AI tools can analyze the profitability of different providers, procedures, or locations, enabling evidence-based decisions on resource allocation and fee adjustments.3 Ultimately, AI enables more proactive financial oversight and helps small and midsize practices remain competitive in an increasingly complex healthcare market.17
Challenges and Considerations for Implementation
Despite its promise, implementing AI in dental practice is not without challenges. Data privacy and security are paramount, especially when integrating AI with EHRs and cloud-based platforms.5 Practices must ensure compliance with HIPAA and invest in secure infrastructure. Cybersecurity deserves specific attention, as dental practices may be targets of ransomware and data breaches. AI vendors should be vetted for their security architecture, and practices should implement multifactor authentication, encrypted data transmission, regular security audits, and staff training on phishing and social engineering threats.2
Staff training and change management are critical to adoption. Resistance to technology and fear of job displacement can be mitigated through transparent communication and ongoing education. Staff must understand the benefits of AI, how it augments rather than replaces their work, and how to troubleshoot AI outputs responsibly.3 Successful AI adoption requires a multidisciplinary governance structure, with clinical, operational, technical, and compliance stakeholders sharing responsibility for oversight, evaluation, and continuous improvement (Table 1).
Integration with existing systems can be complex and may require technical support or new software investments. Vendor selection, system compatibility, and data migration planning are all essential elements of a successful AI implementation.5
Ethical concerns regarding transparency, accountability, and clinical decision-making must also be addressed. A persistent challenge in AI deployment is the “black box” problem: many high-performing AI models—particularly deep learning systems—cannot fully explain how they arrive at a given output. This lack of explainability creates accountability gaps when AI-assisted diagnoses contribute to patient harm. Clinicians must retain final authority over care decisions, and AI tools should, whenever possible, be explainable and auditable. Practices should create policies to govern the responsible use of AI in patient interactions, marketing, and financial forecasting.5
Algorithmic bias and health equity represent underappreciated challenges in dental AI adoption. Most commercial AI imaging systems were trained predominantly on datasets from academic dental centers and larger practices, which may not reflect the demographic diversity of the broader patient population. If training data underrepresents certain racial, ethnic, or socioeconomic groups, AI performance may be systematically inferior for those patients—potentially compounding existing oral health disparities rather than reducing them.2 Practices and researchers must advocate for more representative training datasets and conduct ongoing performance audits stratified by patient demographics.
Regulatory considerations add another dimension of complexity. AI systems used in clinical diagnosis fall under FDA oversight as software as a medical device (SaMD), and clinicians should verify FDA clearance status before deploying any diagnostic AI tool. Regulatory frameworks continue to evolve, and practices should monitor updates from the FDA’s Digital Health Center of Excellence and relevant professional associations.12
Finally, practices must evaluate the return on investment for AI solutions. Not all technologies yield immediate financial benefits, and strategic planning is essential to ensure long-term value. Piloting technologies, measuring key performance indicators, and soliciting feedback from staff and patients can guide sustainable integration.17
Conclusion and Future Directions
AI holds transformative potential for dental practices across clinical and administrative domains. From improving patient safety through better diagnostics to streamlining operations and enhancing financial management, AI offers tangible benefits that can elevate practice performance and patient care. As the technology matures, dental professionals must remain informed, strategic, and ethical in their adoption. By thoughtfully integrating AI into their workflows, practices can improve outcomes, reduce costs, and meet the evolving expectations of today’s healthcare consumers.
Looking ahead, several near-term developments warrant particular attention. Ambient AI scribing platforms are transitioning from early adopter status to mainstream deployment, and practices that invest in ambient documentation infrastructure now will be well-positioned for the broader shift toward AI-integrated care environments. AI-assisted implant and orthodontic treatment planning tools are moving rapidly from research settings into commercial availability, promising to reduce planning time, improve precision, and enhance patient communication through visualization.10,11 Wearable biosensors, AI-powered intraoral scanners, and patient-facing decision aids will become increasingly common as diagnostic AI migrates to handheld and point-of-care devices.
Multimodal AI systems—capable of synthesizing imaging data, clinical notes, patient history, and genomic or biomarker information simultaneously—represent a particularly powerful frontier. Large language models are already enabling AI systems to engage with patients and clinicians in nuanced natural language, summarizing clinical notes, drafting referral letters, answering complex patient queries, and flagging documentation gaps in real time.21 As these capabilities converge, the vision of a truly integrated AI-enhanced practice—where clinical, operational, and financial functions communicate seamlessly—becomes increasingly achievable.
To realize these benefits equitably and safely, dental leaders must collaborate with AI developers, regulators, and professional associations to create standards for safe, transparent, and bias-aware AI use. Investment in staff education, vendor due diligence, and outcome monitoring will be essential. With a clear vision and a commitment to continuous learning, dental professionals can harness AI not as a replacement for human care, but as a powerful tool to enhance it in every dimension.
ABOUT THE AUTHORS
James Dockins, EdD, MBA
Associate Professor of Management, College of Business and Technology, Rockhurst University, Kansas City, Missouri
Dave Lingerfelt, EdD, MBA
Clinical Assistant Professor of Management and Analytics, College of Business and Technology, Rockhurst University, Kansas City, Missouri
Jeffery Moyer, DMD
Assistant Professor, College of Dental Medicine, Kansas City University, Kansas City, Missouri
Queries to the author regarding this course may be submitted to authorqueries@conexiant.com.
REFERENCES
1. Batra AM, Reche A. A new era of dental care: harnessing artificial intelligence for better diagnosis and treatment. Cureus. 2023;15(11):e49319.
2. Elani HW, Giannobile WV. Harnessing artificial intelligence to address oral health disparities. JAMA Health Forum. 2024;5(4):e240642.
3. Surdu A, Budala DG, Luchian I, et al. Using AI in optimizing oral and dental diagnoses—a narrative review. Diagnostics (Basel). 2024;14(24):2804.
4. Carvalho BKG, Nolden EL, Wenning AS, et al. Diagnostic accuracy of artificial intelligence for approximal caries on bitewing radiographs: a systematic review and meta-analysis. J Dent. 2024;151:105388.
5. US Food and Drug Administration. 510(k) Summary: Overjet Caries Assist—Pediatric (K233738). March 4, 2024. https://www.accessdata.fda.gov/cdrh_docs/pdf23/K233738.pdf. Accessed March 19, 2026.
6. US Food and Drug Administration. 510(k) Summary: Pearl Second Opinion®—Caries Segmentation (K243234). June 12, 2025. https://www.accessdata.fda.gov/cdrh_docs/pdf24/K243234.pdf. Accessed March 19, 2026.
7. Pul U, Tichy A, Pitchika V, Schwendicke F. Impact of artificial intelligence assistance on diagnosing periapical radiolucencies: a randomized controlled trial. J Dent. 2025;160:105868.
8. Slashcheva LD, Schroeder K, Heaton LJ, et al. Artificial intelligence–produced radiographic enhancements in dental clinical care: provider and patient perspectives. Front Oral Health. 2025;6:1473877.
9. Zhang JW, Fan J, Zhao FB, et al. Diagnostic accuracy of artificial intelligence–assisted caries detection: a clinical study. BMC Oral Health. 2024;24(1):1095.
10. Zaww K, Abbas H, Vanegas Sáenz JR, Hong G. AI-driven innovations for dental implant treatment planning: a systematic review. J Prosthodont Res. 2025. doi:10.2186/jpr.JPR_D_24_00338.
11. Hamdan M, Alhendi O, Baqain Z, et al. Artificial intelligence applications in dentistry: a systematic review. Dent J. 2025;5(4):90.
12. Lal A, Nooruddin A, Umer F. Concerns regarding deployment of AI-based applications in dentistry – a review. BDJ Open. 2025;11(1):27.
13. Ocampo Osorio F, Pedroza Gomez S, Rebellón Sanchez DE, et al. Predicting no-shows at outpatient appointments in internal medicine using machine learning models. PeerJ Comput Sci. 2025;11:e2762.
14. Alabdulkarim Y, Almukaynizi M, Almaslukh A, et al. Predicting no-shows for dental appointments. PeerJ Comput Sci. 2022;8:e1147.
15. Deina C, Fogliatto FS, da Silveira GJC, Anzanello MJ. Decision analysis framework for predicting no-shows to appointments using machine learning algorithms. BMC Health Serv Res. 2024;24(1):37.
16. Rosenthal JT, Beecy A, Sabuncu MR. Rethinking clinical trials for medical AI with dynamic deployments of adaptive systems. NPJ Digit Med. 2025;8(1):252.
17. Maruska EE, Elgreatly A, Madaio W, et al. Comparing dentist and chatbot answers to dental questions for quality and empathy. JADA Found Sci. 2025;4:100044.
18. Kaushik R, Rapaka R. AI-driven evolution in teledentistry: a comprehensive overview of technology and clinical applications. Dentistry Review. 2025;5(2):100154.
19. Chuang YS, Lee CT, Lin GH, et al. Cross-institutional dental electronic health record entity extraction via generative artificial intelligence and synthetic notes. JAMIA Open. 2025;8(3):ooaf061.
20. El Arab RA, Abu-Mahfouz MS, Abuadas FH, et al. Bridging the gap: from AI success in clinical trials to real-world implementation – a narrative review. Healthcare (Basel). 2025;13(7):701.
21. Stephan D, Bertsch A, Burwinkel M, et al. AI in dental radiology—improving the efficiency of reporting with ChatGPT: comparative study. J Med Internet Res. 2024;26:e60684.
22. Olson KD, Meeker D, Troup M, et al. Use of ambient AI scribes to reduce administrative burden and professional burnout. JAMA Netw Open. 2025;8(10):e2534976.
23. Musleh D, Almossaeed H, Balhareth F, et al. Advancing dental diagnostics: a review of artificial intelligence applications and challenges in dentistry. Big Data Cogn Comput. 2024;8(6):66.
24. Rahim A, Khatoon R, Khan TA, et al. Artificial intelligence-powered dentistry: probing the potential, challenges, and ethicality of artificial intelligence in dentistry. Digit Health. 2024;10:20552076241291345.
25. Yarlagadda SK, Samavati N, Ghorbanifarajzadeh M, et al. Development and validation of an AI-enabled oral score using large-scale dental data. Sci Rep. 2025;15(1):20398.