You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Management of soft tissue is one of the most challenging segments of tooth replacement in the world of restorative dentistry, particularly in the anterior zone. Ideal planning and positioning of implants are extremely important when suggested as a treatment. However, achieving the ideal esthetic outcome is not possible without careful consideration of the abutment, restoration, and the emergence profile.1 One of the major challenges in implant dentistry is in predicting the final position of the bone and, relatively, the tissue. This is due to the fact that a considerable amount of hard and soft tissue is often removed during implant placement.2 In order to address the problem of the soft tissue unpredictability, the design of the implant abutment and definitive restoration becomes an essential factor to assess. Often, provisional restorations provide the opportunity of "guiding" the soft tissue to compensate for changes from ideal position, especially in the esthetic zone.3Therefore, a correct design and fabrication of the initial or secondary provisional restorations becomes an essential part of achieving results that are esthetically pleasing, considering the final position of soft tissue when dealing with implant-supported restorations. It is important to realize that a healthy and correctly designed peri-implant soft tissue plays an essential role in the maintenance and stability of implants, besides providing an esthetic outcome.4 Increasing evidence has proven the importance of peri-implant soft tissue health in long-term clinical stability; therefore a complete knowledge of tissue management, including all possible complications, is necessary when restoring dental implants.5 Once clinicians are able to provide a satisfactory soft-tissue position with provisional restorations, transferring the emergence morphology to the final restoration becomes the next most important step. For this reason, there have been a variety of attempts to reproduce the morphology of implant supported provisionals accurately within the final restoration. Current analog techniques have many limitations that stand in the way of precise reproduction of provisional restorations; materials used, technique sensitivity, and human error are a few of many to be considered here.6 Digital dentistry and CAD/CAM technologies have advanced at an extremely high rate.7 Addressing some of the limitations mentioned above, and development of easier, yet more accurate restorative workflows, come parallel with this growing technology. Today, intraoral scanners can be utilized to capture accurate data, from soft tissue form to implant position, in order to fabricate definitive implant abutments and final restorations that promote ideal peri-implant tissue characteristics.
Guidance With Temporary Restorations
The initial opportunity to address management of the tissue after implant placement (if immediate loading is not indicated and considered) is the use of prefabricated or customized healing abutments.8 Often, the initial implant-supported provisional that is loaded, after minimum required bone integration is achieved, becomes the first attempt to guide the soft tissue. This is considering that no surgical manipulation of the tissue, such as grafting or any gingivoplasty, is planned before the final restoration is loaded. Furthermore, prior to loading the definitive restoration, tissue form and guidance are the main objectives behind fabrication of implant-supported provisionals, rather than the esthetics. In many cases, soft-tissue defects around implant restorations are mainly the result of a poor or over-contoured design of the prosthetic crown.9
From a restorative and laboratory perspective, guidance of the tissue is generally achieved by different designs of the provisional contour. Ideally contoured implant restorations illustrate a healthy transition from the circular design of the implant head to the given cervical tooth anatomy; in most anterior cases, the implant abutment is used as a vehicle to provide this transition.10 The abutment contour essentially becomes one of the most important tools to control and shape the peri-implant soft tissue, including the level of gingival margin, height of papillae, labial alveolar profile, and also the color of the gingiva.10
For simplicity, three main categories of the gingival contour of implant-supported provisionals can explain how soft tissue is guided by different designs (Table 1). A normal (or rather concave/under-contoured) design provides an opportunity to either maintain existing tissue level or in some cases allow minimal coronal movement. On the other hand, an over-contoured or convex design allows apical movement of the surrounding tissue. Lastly, an exaggerated contour represents an extremely convex and bulky design, which is one of the most common mistakes in implant restoration design, resulting in the loss of tissue height and papillae.
A Fully Digital Workflow
Once the ideal peri-implant soft tissue is achieved by the correct design of the implant-supported provisional, the next and most important step is replicating that same emergence profile in the definitive restoration. Transferring the emergence profile from provisional to the final restoration has been achieved by various techniques. Addition of composite to the impression coping, fabrication of a working cast to mimic the soft-tissue contour, and various uses of CAD/CAM technology are the few popular ways to perform this transfer.11 In most cases, when CAD/CAM technology is utilized, the transfer of existing emergence profile is still initiated by using composite resins and manual modifications, followed by a digital capture, to fabricate the final abutment design.
Quality intraoral scanners have become more accessible in the past few years. This continual advancement of intraoral scanners has created an extremely efficient workflow in everyday dentistry. The alternative use of intraoral scanners, in place of conventional impressions, creates an extremely comfortable and efficient workflow for both the clinician and the patient, besides being more environmentally friendly.12,13
Utilizing digital dentistry, specifically quality chairside intraoral scanners, practitioners can now create an easy, yet accurate, workflow for transferring the existing emergence profile from implant-supported provisional restorations to the definitive restoration. Considering a fully digital workflow, the following steps are to be followed for this transfer:
1. Digital scan of the tissue as soon as provisional is removed
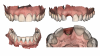
It is important to realize that digital impressions have numerous advantages over physical impression material when it comes to an immediate capture of the soft tissue after removal of implant-supported provisionals; avoidance of inaccuracies caused by impression material strain, movement of implant impression components, and expansion of gypsum material are few of many advantages in utilizing a digital scanner over conventional impression materials.14,15 During this initial step, prior to removing the implant provisional, a full-arch scan is recommended in order to obtain an additional record besides the diagnostic wax up. An immediate digital scan of the tissue socket should be the first step after removing the implant-supported provisional. It is important to acquire this scan immediately, as soft tissue can change quickly without the guidance of the provisional restoration (Figure 1).
2. Digital impression with implant scan bodies
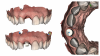
For the final impression of implant-supported crowns, the digital workflow eliminates the need for tray selection, impression materials, transportation, and cast/model production, which drastically improves time efficiency. Additionally, this workflow has been reported to have a much higher acceptance from patients when compared to conventional methods.16 A digital impression, utilizing scan bodies, is the next step after the first digital scan of the tissue (Figure 2).
3. Digital capture of implant-supported provisional with intraoral scanner
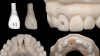
Most intraoral scanners allow auxiliary scans in addition to what is acquired inside the mouth. This opportunity can be used to capture the prefabricated provisional accurately, after all intraoral scans (Steps 1 and 2) are completed, during the same appointment. While the provisional restoration is removed for the initial steps of this workflow, it can be assembled on a laboratory analog. The use of laboratory analog will create an extension to a) allow a complete capture of the entire provisional, and b) create a matching positioning cylindrical extension for future laboratory model work (Figure 3). Note that here, a digital analog is used that corresponds to the implant access diameter, created in printed models by the laboratory. Notice that all the steps so far have been digitally driven. A huge advantage here is that these digital acquisitions are stored in an electronic database in the form of virtual models, which facilitates a faster communication between the clinician and the dental technician and eliminates the risk of losing or damaging parts, models, and physical impressions.17
4. Design of the final restoration based on all digitally acquired information
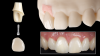
Once all digitally acquired data is received by the laboratory, a printed copy of the provisional restoration will be fitted on the final model. As mentioned before, the laboratory analog used during the acquisition has the same diameter as the access hole created for implant model work. This will allow accurate repositioning of the provisional on the printed model generated from the impression with the scan body. This positioning will be additionally confirmed by the initial scan, acquired prior to removing the provisional. After confirming correct positioning of the printed provisional, these two valuable records allow replication of the emergence profile of the provisional and the surrounding soft tissue: a) the scanned tissue socket, and b) the provisional itself. An additional injection of a soft tissue moulage will allow a third replication of the soft-tissue position based on the acquired information (Figure 4).
These steps will allow the laboratory to design the final restoration accurately, replicating the soft tissue that has been guided using the provisional. All scans acquired will be superimposed and merged onto an imaging software to produce an extremely accurate emergence profile, replicating the final soft-tissue form. This information will then be used to design customized abutments or screw retained final restorations digitally, if implant access does not compromise the esthetics (Figure 5).
Conclusion
This digital workflow allows a simple yet accurate fabrication of the emergence profile for the definitive implant-supported restorations in the esthetic zone. Steps of this workflow are the following: 1) digital scan of the tissue as soon as provisional is removed, 2) digital impression with implant scan bodies, 3) digital capture of implant-supported provisional with intraoral scanner, and 4) design of the final restoration based on all digitally acquired information. This technique allows fabrication of a predictable definitive restoration, appreciating the pre-implant soft tissue in the esthetic zone, while reducing the duration of clinical appointments and procedures.
Discussion
Currently, a significant amount of literature is focused on surgical approaches in implant dentistry in the esthetic zone, when compared to tissue management and restorative workflows following the surgical procedures.18The value of excellent implant positioning and surgical management of bone and tissue will be defeated without predictable esthetic outcomes: the part which patients care about the most. As mentioned before, the ability to form healthy and correctly shaped peri-implant soft tissue plays an extremely important role in the maintenance and stability of implants, in addition to providing ideal esthetic outcomes.4 This report discusses a simple digital workflow that allows a predictable replication of the emergence profile in implant-supported provisionals and the surrounding soft tissue for fabrication of ideal definitive restorations. A limitation of this report is lack of restorative considerations, in a similar workflow, when dealing with replacement of multiple adjacent missing teeth in the esthetic zone. In existing literature, tissue management and esthetic considerations when replacing multiple adjacent teeth with implant restorations is poorly documented.18 Further discussion on how to train and manage soft tissue in multiple-unit cases utilizing digital dentistry is needed. Furthermore, additional elements such as maintenance of the soft tissue should be included in future studies.
About the Authors
Sam Alawie, MDT
Founder & President
Beverly Hills Dental Laboratory
Beverly Hills, California
Mehrdad Razaghy, DDS
Private Practice
Beverly Hills, California
References
1. Steigmann M, Monje A, Chan HL, Wang HL. Emergence profile design based on implant position in the esthetic zone. Int J Periodontics Restorative Dent. 2014;34(4):559-563.
2. Schropp L, Kostopoulos L, Wenzel A. Bone healing following immediate versus delayed placement of titanium implants into extraction sockets: A prospective clinical study. Int J Oral Maxillofac Implants. 2003;18(2):189-199.
3. Spyropoulou PE, Razzoog M, Sierraalta M. Restoring implants in the esthetic zone after sculpting and capturing the periimplant tissues in rest position: a clinical report. J Prosthet Dent. 2009;102(6):345-347.
4. Del Amo FSL, Yu SH, Sammartino G,et al. Peri-implant Soft Tissue Management: Cairo Opinion Consensus Conference. Int J Environ Res Public Health. 2020;17(7):2281.
5. Chackartchi T, Romanos GE, Sculean A. Soft tissue-related complications and management around dental implants. Periodontol 2000. 2019;81(1):124-138.
6. Kurosaki Y, Mino T, Maekawa K, et al. Digital transfer of the subgingival contour and emergence profile of the provisional restoration to the final bone-anchored fixed restoration. J Prosthodont Res.2019;63(1):125-129.
7. Alsharbaty MHM, Alikhasi M, Zarrati S, Shamshiri AR. A clinical comparative study of 3-dimensional accuracy between digital and conventional implant impression techniques. J Prosthodont. 2019;28(4):e902-e908.
8. Ruales-Carrera E, Pauletto P, Apaza-Bedoya K, et al. Peri-implant tissue management after immediate implant placement using a customized healing abutment. J Esthet Restor Dent. 2019;31(6):533-541.
9. Zucchelli G, Mazzotti C, Mounssif I, et al. Esthetic treatment of peri-implant soft tissue defects: a case report of a modified surgical-prosthetic approach. Int J Periodontics Restorative Dent. 2013;33(3):327-335.
10. Su H, Gonzalez-Martin O, Weisgold A, Lee E. Considerations of implant abutment and crown contour: critical contour and subcritical contour. Int J Periodontics Restorative Dent. 2010;30(4):335-343.
11.Papadopoulos I, Pozidi G, Goussias H, Kourtis S. Transferring the emergence profile from the provisional to the final restoration. J Esthet Restor Dent. 2014;26(3):154-161.
12. Chiu A, Chen YW, Hayashi J, Sadr A. Accuracy of CAD/CAM digital impressions with different intraoral scanner parameters. Sensors (Basel). 2020;20(4):1157.
13. Yuzbasioglu E, Kurt H, Turunc R, Bilir H. Comparison of digital and conventional impression techniques: Evaluation of patients' perception, treatment comfort, effectiveness and clinical outcomes. BMC Oral Health. 2014;14:10.
14. Lee SJ, Betensky RA, Gianneschi GE, Gallucci GO. Accuracy of digital versus conventional implant impressions. Clin Oral Implants Res. 2015;26(6):715-719.
15. Ahlholm P, Sipila K, Vallittu P, et al. Digital versus conventional impressions in fixed prosthodontics: a review. J Prosthodont.2018;27(1):35-41.
16. Joda, T., Lenherr, P., Dedem, P., Kovaltschuk, I., Bragger, U., & Zitzmann, N. U. (2017). Time efficiency, difficulty, and operator's preference comparing digital and conventional implant impressions: a randomized controlled trial. Clin Oral Implants Res. 2017;28(10):1318-1323.
17. Mangano F, Gandolfi A, Luongo G, Logozzo S. Intraoral scanners in dentistry: a review of the current literature. BMC Oral Health.2017;17(1):149.
18. Belser UC, Schmid B, Higginbottom F, Buser D. Outcome analysis of implant restorations located in the anterior maxilla: a review of the recent literature. Int J Oral Maxillofac Implants. 2004;19 Suppl:30-42.