You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The world appears more polarized than ever, and there appears to be growing intolerance for anyone with an opposing view. While not political, cementation can have its fair share of extremists as well. Some clinicians claim to be "cementalists" while others follow the "adhesivist" agenda. The cementalism platform prefers to avoid the complexity of adhesion at all costs, while adhesivism promotes using bonding agents whenever possible. Many of us are moderates and are members of both parties.
"Follow the science" has been spewed by many without ever even looking at the science. Unfortunately, so too with clinicians. Without challenge, we can all agree that we all desire long-lasting restorations with a high level of patient satisfaction and health. Repeatable, predictable success has been the platform stood upon by most dentists.
More specifically with regards to zirconia restorations, there is the perception that, because the material itself is relatively hard, almost any type of cement type will work.1 However, that cavalier approach has resulted in less-than-ideal long-term clinical results, particularly when the tooth preparation is inadequate or there are high parafunctional stresses.2
Newer, more translucent zirconia allows for more restoration vitality and increased esthetics, overcoming some of the zirconia limitations in the esthetic zone.3 Generally as the opacity decreases, so do the durability and flexural strength.4More translucent zirconia is less durable, so it is even more critical to long-term success that they be placed with a dual-cure self-adhesive resin cement (SARC) or a resin cement preceded by a separate dentin bonding agent.
A "Wakened" View
Zirconia has become a popular choice with many clinicians striving for esthetic, comfortable, durable consistency that is a good value for the patients and the practice.5 This material effectively fits into the arsenal of most practitioners for everything from conservatively prepped veneers to full-coverage crowns and bridges; with proper tooth preparation and cementation, its long-term survival is expected to be excellent.6-8
Debonding, restoration fracture, opacity, chipping, and other issues have been observed by many clinicians.9 Bonded resin cementation with a SARC has been shown to have a beneficial effect on zirconia longevity, particularly when the preparation is compromised, occlusal forces are excessive, or there are multi-unit prostheses.10Two factors in direct control by the clinician that increase long-term clinical success are a retentive preparation and the use of SARCs that have 10-methacryloxydecyl dihydrogen phosphate (10-MDP) chemistry.11 10-MDP is currently regarded as the most stable bond available to zirconia and is found in some bonding agents, primers, and the self-adhesive resin cements.12,13
Concerns over pulpal irritation and bio-intolerance have driven the profession towards higher bio-friendly materials.14 The bio-interactive effects normally involves the release of fluoride and/or calcium and has been applied to composites, cements, pulp capping materials, liners, sealants, and bonding agents.15-18 A "woke" view may be to consider SARCs that may increase restoration durability and promote tissue health.19 Developments over the last few years have been aimed towards highly bio-compatible materials that are antimicrobial, are able to promote tooth remineralization, and contain 10-MDP for superior adhesion and indicated for full-coverage zirconia restorations.20
The desire for less cytotoxic, more bio-compatible materials has in part been solved by the development and excellent clinical performance of self-adhesive dual-cure resin cements that contain 10-MDP and release significant amounts of calcium and fluoride.21 The effect is a zirconia- and dentin-adhering resin that also responds to the oral environment by releasing bio-available ions, which have been shown to reduce microbes, decrease acidity, and increase remineralization.22-23
"Adhesivism" vs "Cementalism": A full-coverage zirconia case
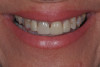
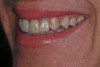
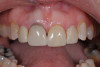
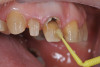
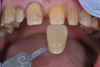
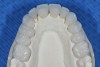
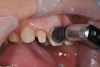
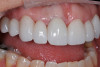
In this case, a middle-aged female with posterior crossbite, interproximal decay, improper midline, and inconsistent color was treatment planned for full-coverage restorations (Figure 1). The plan was for full-coverage maxillary posterior monolithic zirconia and a less opaque anterior zirconia on anterior teeth (Figure 2). Soft tissue health was acceptable, with dark root obvious on tooth No. 8, which had successful endodontic treatment many years earlier (Figure 3).
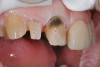
There was significant darkness beneath the porcelain-fused-to-metal restoration on tooth No. 8 and options to lessen its influence on the final restorations were considered (Figure 4). As is often the case, removal of dentin only leads to intensification of the darkness, so here 1 to 2 mm was removed facially and "ditched" subgingivally. A universal dentin bonding agent (All-Bond Universal, Bisco) was applied and agitated to the surface in several layers and light cured (Figure 5).
A thin layer of opaque flowable composite was placed, followed by a dentin opacity composite in a shade that roughly matched the dentin (Figure 6). Preparations were completed with a coarse diamond (NeoDiamond, Microcopy) with the goal of 1.5-mm occlusal clearance, chamfer margins, and rounded line angles to reduce internal stresses. Mandibular occlusion was adjusted to allow for crossbite correction in the final restorations.
Impressions were taken with a poly vinyl siloxane (Panasil, Kettenbach) and sent to the laboratory with all photos, bite registrations, and dentofacial analyzer index (Kois Dentofacial Analyzer, Panodent). Temporaries were made for the central incisors, 2% chlorhexidine painted on teeth (Cavity Cleanser, Bisco) and placed with a temporary cement (Zone Free, Pentron). The instructions for the laboratory were for monolithic zirconia restorations Nos. 3 to 14, with particular attention to occlusion, opacity, value, and final shade.
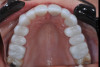
Restorations were returned from the laboratory and full-coverage preparations were self-evaluated on the returned models (Figure 7). Higher-flexural-strength, higher-opacity zirconia were used on posterior teeth, while anterior higher-translucency zirconia was chosen for the anterior teeth (Figure 8). After removal of the temporaries, the teeth were cleaned with a mixture of flower pumice (Preppies, Whip Mix) and 2% chlorhexidine (Cavity Cleanser, Bisco). Restorations were then tried in with water and the desired color verified, with particular attention to consistent opacity and value of No. 8 (Figure 9).
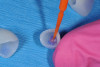
SARCs containing 10-MDP also form a reliable bond to a clean zirconia surface without the need for separate restoration primers or bonding agent as long as the surface is free of phosphates.24 During try-in, phosphates from oral fluids contaminate the intaglio surface and would interfere with the necessary phosphate bond from the 10-MDP, compromising its bond and subsequent retention25 (Figure 10). A restoration cleaner (ZirClean, Bisco) was used to remove such contaminants from the intaglio surface, which was then rinsed and dried (Figure 11).
"Politically" Correct Bio-Friendly Placement
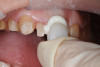
A self-adhesive calcium silicate resin cement (TheraCem, Bisco) was used to cement all the restorations at once, starting from the incisors and working posteriorly (Figure 12). This 10-MDP cement comes in a "natural" shade and provides a strong bond to dentin and most modern dental materials, such as etched lithium disilicate and zirconia.26 The high calcium level in this calcium silicate cement gives the material a slightly opaque, white appearance but influences the final restoration color imperceptibly (Figure 13).
The calcium and fluoride release, easy clean up, and physical properties make this a great choice for routine zirconia and lithium disilicate full-coverage placement (Figure 14). Notable features of this calcium silicate cement are its easy clean-up and excellent clinical performance.27 After allowing initial chemical cure, the material is easily removed and followed with light-curing at the margins.
One week after cementation, the soft tissue response is excellent and esthetics acceptable (Figure 15). Patient expectations were met and the work was evaluated at a follow-up appointment. The results are durable, bio-tolerant restorations with the potential for sustained tissue health (Figure 16 and Figure 17).
About the Author
Jack D. Griffin, Jr., DMD
Private Practice
Lake St. Louis, Missouri
References
1.Dogan S, Raigrodski AJ. Cementation of zirconia-based toothborne restorations: a clinical review. Compend Contin Educ Dent. 2019;40(8):536-540. PMID: 31478701.
2.Blatz MB, Vonderheide M, Conejo J. The effect of resin bonding on long-term success of high-strength ceramics. J Dent Res. 2018;97(2):132-139. doi: 10.1177/0022034517729134. Epub 2017 Sep 6. PMID: 28876966; PMCID: PMC6429574.
3.Kelly JR, Nishimura I, Campbell SD. Ceramics in dentistry: historical roots and current perspectives. J Prosthet Dent. 1996;75:18-32
4.Kontonasaki E, Giasimakopoulos P, Rigos AE. Strength and aging resistance of monolithic zirconia: an update to current knowledge. Jpn Dent Sci Rev. 2020;56(1):1-23. doi: 10.1016/j.jdsr.2019.09.002. Epub 2019 Nov 14. PMID: 31768195; PMCID: PMC6872834.
5.Zarone F, Di Mauro MI, Ausiello P, et al. Current status on lithium disilicate and zirconia: a narrative review. BMC Oral Health. 2019;19:134.
6.G.W. Tysowsky. The science behind lithium disilicate: A metal-free alternative. Dent Today. 2009;28:112-113
7.Rauch A, Reich S, Dalchau L, Schierz O. Clincial survival of chair-side generated monolithic disilicate crowns: 10-year results. Clin Oral Investig. 2012;22:1763-1769
8.Pathan MS, Kheur MG, Patankar AH, Kheur SM. Assessment of antagonist enamel wear and clinical performance of full-contour monolithic zirconia crowns: one-year results of a prospective study. J Prosthodont. 2019;28:e411-e416.
9.Tang Z, Zhao X, Wang H, Liu B. Clinical evaluation of monolithic zirconia crowns for posterior teeth restorations. Medicine (Baltimore). 2019;98(40):e17385. doi: 10.1097/MD.0000000000017385. PMID: 31577743; PMCID: PMC6783234.
10.Maroulakos G, Thompson GA, Kontogiorgos ED. Effect of cement type on the clinical performance and complications of zirconia and lithium disilicate tooth-supported crowns: A systematic review. Report of the Committee on Research in Fixed Prosthodontics of the American Academy of Fixed Prosthodontics. J Prosthet Dent. 2019;121(5):754-765. doi: 10.1016/j.prosdent.2018.10.011. Epub 2019 Mar 15. PMID: 30885580.
11.Sharafeddin F, Shoale S. Effects of universal and conventional mdp primers on the shear bond strength of zirconia ceramic and nanofilled composite resin. J Dent (Shiraz). 2018;19(1):48-56. PMID: 29492416; PMCID: PMC5817343.
12.Shibuya K, Ohara N, Ono S, et al. Influence of 10-MDP concentration on the adhesion and physical properties of self-adhesive resin cements. Restor Dent Endod. 2019;44(4):e45. Published 2019 Nov 12. doi:10.5395/rde.2019.44.e45
13.De Angelis F, D'Arcangelo C, Buonvivere M, et al. Shear bond strength of glass ionomer and resin-based cements to different types of zirconia. J Esthet Restor Dent. 2020;32(8):806-814. doi: 10.1111/jerd.12638. Epub 2020 Aug 18. PMID: 32810368.
14.Chan DC, Hu W, Chung KH, et al. Reactions: Antibacterial and bioactive dental restorative materials: Do they really work? Am J Dent. 2018;31(Sp Is B):32B-36B. PMID: 31099210.
15.Zhang K, Zhang N, Weir MD, et al. Bioactive dental composites and bonding agents having remineralizing and antibacterial characteristics. Dent Clin North Am. 2017;61(4):669-687. doi: 10.1016/j.cden.2017.05.002. PMID: 28886763; PMCID: PMC5803788.
16.Vallittu PK, Boccaccini AR, Hupa L, Watts DC. Bioactive dental materials -- Do they exist and what does bioactivity mean? Dent Mater. 2018;34(5):693-694. doi: 10.1016/j.dental.2018.03.001. Epub 2018 Mar 20. PMID: 29571660.
17.Turkistani A, Islam S, Shimada Y, et al. Dental cements: Bioactivity, bond strength and demineralization progression around restorations. Am J Dent. 2018;31(Sp Is B):24B-31B. PMID: 31099209.
18.Braga RR, Fronza BM. The use of bioactive particles and biomimetic analogues for increasing the longevity of resin-dentin interfaces: A literature review. Dent Mater J. 2020 31;39(1):62-68. doi: 10.4012/dmj.2019-293. Epub 2019 Nov 14. PMID: 31723068.
19.Zhang K, Zhang N, Weir MD, et al. bioactive dental composites and bonding agents having remineralizing and antibacterial characteristics. Dent Clin North Am. 2017;61(4):669-687. doi: 10.1016/j.cden.2017.05.002. PMID: 28886763; PMCID: PMC5803788.
20.Chen L, Hong S, Suh B. Bioactive dental restorative materials: a review. Am J Dent.2013;26(4):219-27.
21.Dworkin O, Kugel G, Loo C. What is bioactive dentistry: A review. Dentistry Today. 2018;37(1):44-46.
22.Chan DC, Hu W, Chung KH, et al. Antibacterial and bioactive dental restorative materials: Do they really work? Am J Dent. 2018;31:32B-36B.
23.Chen L, Yang J, Wang JR, Suh BI. Physical and biological properties of a newly developed calcium silicate-based self-adhesive cement. Am J Dent. 2018;31:86-90.
24.Yang L, Xie H, Meng H, et al. Effects of luting cements and surface conditioning on composite bonding performance to zirconia. J Adhes Dent. 2018;20(6):549-558. doi: 10.3290/j.jad.a41634. PMID: 30564802.
25.Nagaoka N, Yoshihara K, Feitosa VP, et al. Chemical interaction mechanism of 10-MDP with zirconia. Sci Rep. 2017;30(7):45563. doi: 10.1038/srep45563. PMID: 28358121; PMCID: PMC5372092.
26.Chen L, Yang J, Wang JR, Suh BI. Physical and biological properties of a newly developed calcium silicate-based self-adhesive cement. Am J Dent. 2018;31(2):86-90. PMID: 29630792.
27.Moeeduddin M, Nathanson D, Fan Y. Effect of firing cycle and etching protocols on tensile bond strength of composite cement to zirconium-incorporated lithium-silicate glass ceramic. J Adhes Dent. 2020;22(6):625-633. doi: 10.3290/j.jad.a45518. PMID: 33491406.