You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Adhesive dentistry has made great strides in the last decades. These improvements have revolutionized many aspects of restorative and preventive dentistry. Now, with adhesive materials, it is no longer necessary to prepare the cavity to provide mechanical retention through such features as dovetails, grooves, undercuts, and sharp internal angles to retain the filling.1 These improvements have enabled a trend toward minimally invasive dentistry by conserving large quantities of tooth substance that would otherwise be removed by a dental bur. This article will examine etching techniques, the evolution of bonding agents, and the utility of various dental cements on the market.
Etching
Adhesive systems are generally classified as total etch or self-etch, depending on their procedure of application and mechanism of adhesion. A third method, called selective etch, will also be discussed. Although effective adhesion to enamel is achieved with relative ease, adhesion to dentin poses a challenge.2 The difficulty with dentin adhesion is partly due to the biologic characteristics of dentin, namely its high organic content, its tubular structure, and the presence of the dentin smear layer that forms immediately after cavity preparation.3 This smear layer prevents the adhesive from interacting directly with dentinal tissue.4 Unless the smear layer is modified or removed, neither hybridization nor resin tag formation can occur. Bond strength is affected by the extent of resin infiltration into the exposed collagen network. Different techniques of acid conditioning, application of adhesive resin, and evaporation of solvents can change the amount of resin uptake and the resulting bond strength.5
Total Etch
Total etch systems generally provide a high bond strength to cut and uncut enamel, as well as to sclerotic dentin.6 There is also less risk of microleakage. Microleakage at the tooth-restoration interface is considered to be a major factor influencing the longevity of the restoration. When microleakage occurs, bacteria and oral fluids invade the resin-dentin border, thereby deteriorating the bond area, resulting in teeth sensitivity, secondary caries, or pulp inflammation.7,8
When compared with self-etch systems, total-etch systems have been said to be more technique sensitive due to the separate step of etching enamel and dentin; strict protocols must be followed. With a total-etch system, isolation and a dry field are critical. However, dentin etched with phosphoric acid must not be overdried. Too much water inside the dentinal tubules can make adhesion difficult, but an excess of water indicates that not all the water molecules will attach to acetone molecules and be volatilized. Etching enlarges the size and volume of pores in the enamel and roughens the surface so that the sealant can penetrate and mechanically lock into these spaces.9
Original surface dentin is covered by a smear layer consisting of organic and inorganic debris. Etching and rinsing this surface removes the smear layer and eliminates the apatite from between the collagen fibers. Thus, when the smear layer is removed, the resulting open dentin tubules can lead to postoperative sensitivity, which may be a problem when not managed correctly.10
Self-Etch
Self-etching systems are part of a trend toward simplification.11 Self-etching systems were developed to avoid the adverse effects of over-etching and over- or under-priming. In line with simplification, the removal of the smear layer and smear plugs is not required with self-etching systems because these systems are capable of etching the tooth surface while simultaneously preparing it for adhesion.11
The better durability of mild two-step self-etch adhesives may be attributed to the use of a separate, relatively more hydrophobic resin layer on top of the hydrophilic self-etch primer, which renders the interface less susceptible to water sorption.12 Nevertheless, mild two-step self-etch adhesives are not totally immune to bond degradation, because they are still hydrophilic, and enzymatic hydrolysis of ester bonds may still occur over time.13
Unfortunately, bond strengths to enamel and sclerotic dentin are typically lower with self-etch than with total etch.6 Additionally, bonding to self- or dual-cure composites and cements may be noncompatible without the use of dual-cure activators.14
Selective Etch
Selective etch is a hybrid technique combining both self-etching and total etching. It can be used in a situation where there is some enamel and some dentin. In that case, one would selectively apply phosphoric acid and etch just the enamel, avoiding the dentin. That action would provide high bond strength to cut and uncut enamel, sclerotic dentin, and dentin without acid etching. However, with the sixth and seventh generation of adhesives, an inadvertent etch on dentin could decrease bond strength.15,16
Classification of Bonding Agents
Adhesive dentistry began in 1955 with an article by Dr. Michael Buonocore on the benefits of acid etching.17 With changing technologies, dental adhesives have evolved from no-etch to total-etch (fourth and fifth generation) to self-etch (sixth, seventh, and eighth generation) systems.18
In the 1980s and 1990s, fourth-generation dentin bonding agents were introduced. The fourth-generation materials were the first to achieve complete removal of the smear layer.19 A three-step process is involved; the three primary components (etchant, primer, and bonding) of adhesive dentistry are packaged in separate containers and applied sequentially. The first step is to etch and rinse with phosphoric acid.20 The second step is to apply the hydrophilic primer, which can infiltrate the exposed collagen network forming the hybrid layer, providing high bond strength and a dentin seal.21,22 The third step is to apply the hydrophobic adhesive layer from a separate bottle, which then air-thins and light-cures. The concept of total-etch technique and moist dentinal are hallmarks of the fourth-generation system.23 This system is technique sensitive, is complex, and can be time-consuming.24 Also needed was a way to prevent collagen collapse of demineralized dentin and to minimize, if not totally eliminate, postoperative sensitivity.
In the 1990s, fifth-generation bonding systems sought to simplify the process of fourth-generation adhesion by reducing the clinical steps. The fifth generation combined the primer and adhesive, making it a single-bottle process. This generation achieves high clinical bond strength, but the resin-dentin bond is prone to water degradation.25
The sixth generation, also known as self-etching primers, eliminated the etching step or included it chemically into one of the other steps. It developed from a need to address the issue of sensitivity, so instead of etching with phosphoric acid, one etches with acidic primers. Etch and prime is in the first bottle, and hydrophobic bonding resin material is in the second bottle. The biggest advantage of the sixth generation is that the efficacy appears to be less dependent on the hydration state of the dentin than the total-etch systems.22 The sixth-generation system is highly successful when bonding to dentin but less effective when bonding to enamel.26
Seventh-generation bonding systems were introduced in late 1999 and early 2005. These are all-in-one; all the ingredients required for bonding are placed in and delivered from one bottle.27,28 This greatly simplifies the bonding protocol, limiting the errors that were introduced with previous generations by the dentist or dental assistant who had to mix the separate components with other, more complicated systems. However, these inherently acidic systems tend to have a significant amount of water in their formulations and may be prone to hydrolysis and chemical breakdown.29 They also tend to be more hydrophilic than two-step self-etching systems, which makes them prone to water sorption, limits the depth of resin infiltration into the tooth, and results in voids.30
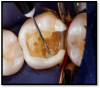
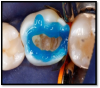
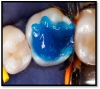
The latest developments in the adhesive marketplace are known as universal adhesives. These systems have the potential to significantly simplify and expedite adhesive protocols. This generation is not only a single step in a single bottle, but also can be used with all three of the bonding modes (total etch, self-etch, or selective etch) (Figure 1 through Figure 3). Additionally, universal adhesives can be used for both direct and indirect restorations, have a low film thickness, and are compatible with light-cure, dual-cure, and self-cure composites and resins. However, the manufacturers of some universal adhesives still recommend the use of separate activator and dedicated primers to optimize bond strength to substrates such as porcelain and zirconia.24 As always, the manufacturer's instructions should be followed.
In summary, the components of an ideal bonding agent include ease of use, fewer steps, versatility, compatibility with curing systems, high bond strength, a low film thickness, no postoperative sensitivity, and no microleakage. Universal bonding adhesives meet these criteria.
Cementation
The characteristics of an ideal cement are that it should be easy to mix, have a low film thickness and low viscosity, have a short setting time, be insoluble in oral fluids, provide a high sheer strength, provide a high tensile strength, provide a high compressive strength, and be able to bond to both tooth structure and restorations. It should also be biocompatible with pulp and soft tissue, available in various shades, and easy to clean up.31 To achieve an optimal clinical performance for cement, there should always be adequate preparation that includes good resistance and retention form.
Cementation materials include zinc phosphate cements, polycarboxylate cements, glass-ionomer cements, polyacid-modified composite cements, resin-based cements, and resin-modified glass ionomer cements. Additionally, the newest cement choices are bioceramic luting cements.
With conventional cementation, the tooth is simply rinsed and dried and the restoration is cleaned, rinsed, and dried. There are no primers on the tooth, nor on the restoration. Zinc phosphate is relatively inexpensive, easy to mix and clean up, and radiopaque. Unfortunately, it has a very low pH, relatively low bond to tooth structure, and solubility in oral fluids, and it often induces pulpitis.32 Polycarboxylate cements are difficult to clean up, and they undergo a relatively fast viscosity change after mixing.32 Glass-ionomer cements release fluoride and have strong bonds in their adhesion to enamel and dentin. However, they too can irritate the pulpal tissue due to their acidic nature. Polyacid-modified composite cements provide relatively high bond strength and low solubility in oral fluids, although they do undergo hygroscopic expansion and thus lose bond strength quickly.33 Resin-modified glass-ionomer cements are easy to use, are relatively stable, and release fluoride. Unfortunately, they are also acidic in nature and hydrophilic.34 Resin-based cements can be either dual-cure, light-cure, or both. They provide high bond strength, are not water soluble, and do not tend to irritate pulpal tissue. They are, however, extremely technique sensitive.35
The most recent addition to cementation options, bioactive cements, are also known as ion-releasing and recharge cements. A desirable bioactive restorative material would create a bond with surrounding tooth structure and release ions to allow remineralization at tooth margins after an acid challenge. A bioactive cement may have the additional benefit of attracting calcium phosphate precipitates to its surface to occlude an existing cement gap.36 Some of these newer cements contain a regenerative ability. Hydraulic silicate cements, such as mineral trioxide aggregate, total fill, and calcium-enriched cement, have claims of bioactivity.37 However, the retention strength of current bioactive materials should not yet be expected to match that of an adhesive resin cement.36
Conclusion
This article has discussed the evolution of materials and techniques that enable the trend toward minimally invasive dentistry. Minimally invasive dentistry involves the ability to bond various materials in a predictable manner to both enamel and dentin substrates, enabling dentists to routinely place porcelain veneers, direct and indirect composites, and a plethora of other restorative and esthetic materials. The increasing demand for esthetic restorative treatments has led to great advances in dentistry, including the development of adhesive integrated materials (such as adhesive systems and composites) and techniques aimed at restoring natural tooth appearance. Success in adhesive dentistry results in long-lasting restorations. Choosing the right materials and techniques is key to achieving a successful restoration.
About the Author
Thomas E. Dudney, DMD
Private Practice
Alabaster, Alabama
References
1. Vaidyanathan TK, Vaidyanathan J. Recent advances in the theory and mechanism of adhesive resin bonding to dentin: a critical review. J Biomed Mater Res B Appl Biomater. 2009;88(2):558-578.
2. Swift EJ Jr, Perdigão J, Heymann HO. Bonding to enamel and dentin: a brief history and state of the art, 1995. Quintessence Int. 1995;26(2):95-110.
3. Lopes GC, Baratieri LN, Caldeira de Andrada MA, Vieira LC. Dental adhesion: present state of the art and future perspectives. Quintessence Int. 2002;33(3):213-224.
4. Gwinnett AJ. Smear layer: morphological considerations. Oper Dent. 1984;3(suppl):2-12.
5. Hashimoto M, Sano H, Yoshida E, et al. Effects of multiple adhesive coatings on dentin bonding. Oper Dent. 2004;29(4):416-423.
6. Hatrick CD, Eakle WS. Principles of bonding. In: Dental Materials: Clinical Applications for Dental Assistants and Dental Hygienists. St. Louis, MO: Elsevier; 2016:44-63.
7. Alani AH, Toh CG. Detection of microleakage around dental restorations: a review. Oper Dent. 1997;22(4):173-185.
8. Gagliardi RM, Avelar RP. Evaluation of microleakage using different bonding agents. Oper Dent. 2002;27(6):582-586.
9. Hatrick CD, Eakle WS. Preventive and desensitizing materials. Dental Materials: Clinical Applications for Dental Assistants and Dental Hygienists. St. Louis, MO: Elsevier; 2016:100-114.
10. Freedman GA. Contemporary Esthetic Dentistry. St. Louis, MO: Elsevier; 2012.
11. Sensi LG, Lopes GC, Monteiro S Jr, et al. Dentin bond strength of self-etching primers/adhesives. Oper Dent. 2005;30(1):63-68.
12. De Munck J, Mine A, Van den Steen PE, et al. Enzymatic degradation of adhesive-dentin interfaces produced by mild self-etch adhesives. Eur J Oral Sci. 2010;118(5):494-501.
13. Liu Y, Tjäderhane L, Breschi L. Limitations in bonding to dentin and experimental strategies to prevent bond degradation. J Dent Res. 2011;90(8):953-968.
14. Gutiérrez MF, Sutil E, Malaquias P, et al. Effect of self-curing activators and curing protocols on adhesive properties of universal adhesives bonded to dual-cured composites. Dent Mater. 2017;33(7):775‐787.
15. Van Landuyt KL, Kanumilli P, De Munck J, et al. Bond strength of a mild self-etch adhesive with and without prior acid-etching. J Dent. 2006;34(1):77-85.
16. Ikeda M, Tsubota K, Takamizawa T, et al. Bonding durability of single-step adhesives to previously acid-etched dentin. Oper Dent. 2008;33(6):702-709.
17. Babu NV, Joseph R. Dr. Michael Buonocore - "Adhesive Dentistry - 1955." J Conserv Dent. 2005;8(3):43-44.
18. Joseph P, Yadav C, Satheesh K, Rahna R. Comparative evaluation of the bonding efficacy of sixth, seventh and eight generation bonding agents: an in vitro study. Int Res J Pharm. 2013;4(9):143-147.
19. Kugel G, Ferrari M. The science of bonding: from first to sixth generation. J Am Dent Assoc. 2000;131(suppl):20S-25S.
20. Tay FR, Gwinnett AJ, Pang KM, Wei SH. Structural evidence of a sealed tissue interface with total-etch wet-bonding technique in vivo. J Dent Res. 1994;73(3):629-636.
21. Nakabayashi N, Kojima K, Masuhara E. The promotion of adhesion by the infiltration of monomers into tooth substrates. J Biomed Mater Res. 1982;16(3):265-273.
22. Alex G. Adhesive considerations in the placement of direct composite restorations. Compend Contin Educ Dent. 2007;28(spec iss 1):20-25.
23. Kanca J III. A method for bonding to tooth structure using phosphoric acid as a dentin-enamel conditioner. Quintessence Int. 1991;22(4):285-290.
24. Sofan E, Sofan A, Palaia G, et al. Classification review of dental adhesive systems: from the IV generation to the universal type. Ann Stomatol (Roma). 2017;8(1):1-17.
25. Toshniwal N, Singh N, Dhanjani V, et al. Self etching system v/s conventional bonding: advantages, disadvantages. Int J Appl Dent Sci. 2019;5(3):379-383.
26. Fabianelli A, Vichi A, Kugel G, Ferrari M. Influence of self-etching-priming bonding systems on sealing ability of Class II restorations: leakage and SEM evaluations. Paper presented at: Annual Meeting of the International Association for Dental Research; Washington, DC: April 6, 2000.
27. Moszner N, Salz U, Zimmermann J. Chemical aspects of self-etching enamel-dentin adhesives: a systematic review. Dent Mater. 2005;21(10):895-910.
28. Yaseen SM, Subba Reddy VV. Comparative evaluation of shear bond strength of two self-etching adhesive (sixth and seventh generation) on dentin of primary and permanent teeth: an in vitro study. J Indian Soc Pedod Prev Dent. 2009;27(1):33-38.
29. Nishiyama N, Tay FR, Fujita K, et al. Hydrolysis of functional monomers in single-bottle self-etching primer-correlation of 13C NMR and TEM findings. J Dent Res. 2006;85(5):422-426.
30. Tay FR, Pashly DH. Have dentin adhesives become too hydrophilic? J Can Dent Assoc. 2003;69(11):726-731.
31. Jacobs MS, Windeler AS. An investigation of dental luting cement solubility as a function of the marginal gap. J Prosthet Dent. 1991;65(3):436-442.
32. Ladha K, Verma M. Conventional and contemporary luting cements: an overview. J Indian Prosthodont Soc. 2010;10(2):79-88.
33. Cattani-Lorente MA, Dupuis V, Moya F, et al. Comparative study of the physical properties of a polyacid-modified composite resin and a resin-modified glass ionomer cement. Dent Mater. 1999;15(1):21-32.
34. Sidhu SK, Watson TF. Resin-modified glass ionomer materials. A status report for the American Journal of Dentistry. Am J Dent. 1995;8(1):59-67.
35. Abo-Hamar SE, Hiller KA, Jung H, et al. Bond strength of a new universal self-adhesive resin luting cement to dentin and enamel. Clin Oral Investig. 2005;9(3)161-167.
36. Lawson N. Examining bioactive restorative materials. Decisions in Dentistry. 2018;4(4):24-27.
37. Loison-Robert LS, Tassin M, Bonte E, et al. In vitro effects of two silicate-based materials, Biodentine and BioRoot RCS, on dental pulp stem cells in models of reactionary and reparative dentinogenesis. PLoS One. 2018;13(1)e0190014.