You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Multiple factors contribute to the formation of "black triangles," or open gingival embrasures. Periodontal concerns contributing to black triangle formation include loss of interproximal bone height, which can occur with age or with attachment loss from periodontal disease, surgery, or trauma. Orthodontic considerations contributing to black triangles are unfavorable root angulation, wide interradicular distance, or a more tapered crown form.1 Black triangles are associated with the changes in the interproximal papilla height between both anterior and posterior teeth. This loss of the interproximal papilla not only is an esthetic issue with some patients, but can also contribute to food retention and be etiologic for periodontal disease.2,3
Solutions for Black Triangles
Direct Restoration
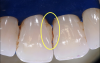
Traditional solutions for black triangles include orthodontic repositioning, interproximal bone graft, soft-tissue graft, papilla reconstruction, and injectibles, which require continued maintenance with repeated treatment.4 A conventional direct restorative method is the placement of hand-manipulated cold pink and/or white composite resin. Although the additive treatment can be conservative to tooth structure, the restoration contours can have a higher incidence of seams, voids, or ledges, which can collect more biofilm (Figure 1).5
Indirect Restoration
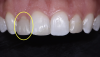
Indirect restorations may require removal of tooth structure to address path of draw and path of insertion concerns. Sometimes a large amount of tooth structure must be sacrificed, especially on lower anteriors (Figure 2). With continued gingival recession, black triangles may again open. Retreatment may necessitate sacrifice of even more tooth structure. Also, the potential abrasiveness of ceramic restorations may lead to unfavorable wear of opposing natural dentition.6
Injection Molding
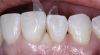
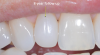
Injection molding with warmed composite is a noninvasive, additive treatment that requires no tooth structure removal. Anatomic Mylar matrices in the difficult to polish subgingival and interproximal areas create smooth contours favorable for tissue adaptation and health. An advantage of the Mylar finish is reduced biofilm and stain accumulation, with any calculus easily removed. Injection molding creates broad incisal gingival and buccolingual contacts that can lend orthodontic stability. Longer contact lengths may result. However, soft color contrasts of pink tissue against white tooth are less visually distracting than the stark contrasts between white teeth and black triangles (Figure 3).6
Case Preparation for Injection Molding
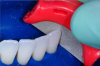
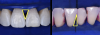
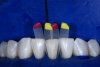
A black triangle gauge is used to assess appropriate matrix size before isolation. Large incisor matrices should be used for maxillary central incisors and cuspids, and small incisor matrices should be used for maxillary lateral incisors and mandibular central and lateral incisors. After they are selected, try-in of the matrices is recommended to confirm appropriate selection. The goal is to minimize the black triangle by at least 85% with the matrices in place. Tissue blanching is a clue that further tissue adaptation may occur with time (Figure 4). Overconstriction of the papilla should be avoided because it may be unesthetic and may cause inflammation. The use of a rubber dam for soft-tissue isolation and retraction is ideal. Rubber dam placement facilitates soft-tissue retraction and isolation from saliva and crevicular fluid. A rubber dam stamp will facilitate proper spacing of punches, but the appropriate diameter punch should be selected for the size of the root. After teeth are isolated and dried, biofilm disclosing solution is applied once.5
Contact sanders are used to clean the contacts and optimize the contact tension before matrix insertion. A safe-sided sander is used primarily to remove any calculus and debris before rubber dam placement to avoid possible tearing. Next, a single-sided light sander is used to optimize the contact tension and remove any stain or biofilm from the contact before matrix placement and injection molding. If needed, a double-sided heavy sander may be used to more aggressively manage the tension of the contacts (Figure 5). Tooth preparation entails contact optimization and removal of all biofilm. After the contacts are cleaned, all remaining biofilm should be removed with the blaster and aluminum trihydroxide powder with high pressure air and water. Acid etch will remove the inorganic, not organic, component of biofilm. Aluminum trihydroxide, which is softer than aluminum oxide, will safely remove biofilm without microetching ceramic restorations or removing the finish off mirrors.5
When a black triangle is being treated, both the shape and the size should be assessed (Figure 6). For a symmetrical black triangle, two matrices of the same size should be chosen to evenly distribute the black triangle between two teeth and avoid creation of a cant. An asymmetrical black triangle calls for mixing matrices so the practitioner can selectively add more volume to one tooth and less to another to maintain a vertical line (Figure 7). When selecting matrices, large incisor matrices should be used for maxillary central incisors and cuspids, while small incisor matrices for maxillary lateral incisors and mandibular central and lateral incisors.4 The selected matrices should then be inserted and checked for full seating and alignment. The incisal edge of the matrices is a visual clue as to whether those matrices are seated equally.
Injection Molding With Warmed Composite
It is estimated that about 14% of dentists currently heat composite, and the number is growing.1 The advantages of warmed composite for injection molding are many. Heating of the composite results in decreased viscosity, which is better for injection molding.
Performing injection molding with dual-viscosity composites allows creation of a monolithic composite form around the tooth that can be easily shaped back to create a restoration with good long-term stability, stain resistance, and esthetics. The composites have shown monolithic uniform color stability without staining or ditching, with smooth subgingival contours. Figure 8 shows a restoration in which the quality has been maintained after 8 years. The composite is warmed by inserting the composite guns, flowable syringes, or composite capsules into the heating device (Figure 9). An example of a composite warmer is shown in Figure 9, which shows the Bioclear HeatSync composite warmer.
The process begins with acid-etching the entire tooth for 20 seconds, followed by rinsing and drying. If immediate dentin sealing is needed, an adhesive dentin bonding agent should be applied and cured in accordance with the manufacturer's instructions for use (IFU) before injection molding. The curing light used had an irradiance of 1,470 mW/cm2.7
The injection molding steps begin with wetting the entire tooth with adhesive (eg, 3M™Scotchbond™ Universal Adhesive, Kuraray ClearFil™ Universal Bond, or BISCO All-Bond Universal®), and then it is air thinned but not cured. Next, heated flowable composite (eg, 3M Filtek™ Supreme Ultra Flowable, Kuraray ClearFil Majesty™ Flow, or Ivoclar Vivadent Heliomolar® Flow) is deliberately applied to the entire tooth to flow into constricted spaces. Warmed universal composite (eg, 3M Filtek Universal Restorative, Ivoclar Vivadent IPS Empress® Direct, or Coltene Miris®2) is then injected into the pool of uncured flowable. Curing should be performed according to the composite's IFU (in the case in this article, three-point curing with a full 20 seconds each on the facial, incisal, and lingual was performed). After the composite is fully cured, an explorer should be used to peel away each matrix, ensuring each is fully released below the contact. A hemostat should be used to remove the matrices as needed. Initial amputation is done while cutting dry with a coarse flame diamond bur. The incisal excess should be amputated to about a half millimeter of the final incisal edge and facial contour. An egg-shaped carbide bur is used to trim the lingual excess, which can later be finished with a brownie. A second round of three-point curing should be done to ensure full depth of cure.8
Final shaping is performed with a large, coarse disc (eg, 3M Sof-Lex™ XT, Shofu Disk HC, or Clinician's Choice Finishing and Polishing Discs). The disc serves as a multifaceted tool. With continued use, the abrasiveness declines and the disc becomes more supple. The disking should be performed dry. The clinician should start with a fresh disc to trim the incisal edge to the final length. The same disc is used to bring in the incisal facial half of the tooth. Next, the same disc is used to blend the gingival half with the incisal half. Then, finally, the palatal line angles are refined.
Polishing starts with refining the surface texture using a prepolish with multiple grits of pumice (an aluminum oxide mix). A generous scoop should be used with a white rubber prophylaxis (prophy) cup. The prepolish should be massaged into the surface of the tooth at medium speed and medium pressure. Final glossy polish is achieved with a diamond-impregnated polisher (eg, Komet One Step Composite Polishing Cup, SS White Jazz® Polishing Cup, or Bioclear RS Polishing Cup).
The advantages of a smooth Mylar finished composite are reduced biofilm attraction, increased stain resistance, and good color stability. These restorations will not have the microsurface texture that might accumulate stain and biofilm.
Conclusion
Injection molding for elimination of black triangles offers significant advantages over traditional direct and indirect restorative solutions. These benefits include reduced biofilm accumulation, increased stain resistance, and increased abrasion resistance. The treatment is conservative, and the technique can be rapidly mastered. The result is superior esthetics and longevity of the restoration with no tooth structure removal.
About the Author
Jihyon Kim, DDS
Consultant for 3M
Private Practice, Bellevue and
Tacoma, Washington
References
1. 3M market research, January 2018. https://multimedia.3m.com/mws/media/1739682O/3m-filtek-dental-restoratives.pdf. Accessed April 15, 2020.
2. Chen MC, Liao YF, Chan CP, et al. Factors influencing the presence of interproximal dental papillae between maxillary anterior teeth. J Periodontol. 2010;81(2):318-324.
3. Singh VP, Uppoor AS, Nayak DG, Shah D. Black triangle dilemma and its management in esthetic dentistry. Dent Res J (Isfahan). 2013;10(3):296-301.
4. Kim, Jihyon. (2019, October 2). Direct Restorative Solutions to treat "Black Triangles. Viva Learning.
5. Øilo M, Bakken V. Biofilm and dental biomaterials. Materials (Basel). 2015;8(6):2887-2900.
6. Cunliffe J, Pretty I. Patients' ranking of interdental "black triangles" against other common aesthetic problems. Eur J Prosthodont Restor Dent. 2009;17(4):177-181.
7.3M. 2017. 3M™ Elipar™ DeepCure-S LED Curing Light Brochure. St. Paul, MN.
8. Sherawat S, Tewari S, Duhan J, et al. Effect of rotary cutting instruments on the resin-tooth interfacial ultra structure: an in vivo study. J Clin Exp Dent. 2014;6(5):e467-e473.