You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
The delivery of scientifically proven restorative dentistry and implant prosthodontics has been significantly advanced by the rapid introduction of innovative digital technologies into clinical practice. These technologies allow for greater ease, cost efficiencies, and improved workflows, which clinicians value as they strive for precision in their quest to achieve equality with nature in dental therapy. Intraoral scanning is one of these technologies that has significantly increased the exactness of measurement for the digital planning of cases and, therefore, has streamlined both the gathering of diagnostics and the predictability of results.
The Evolution of Digital Intraoral Scanning
Before intraoral scanning technology was introduced, clinicians relied solely on conventional impressions, which generally involved using cumbersome metal trays and various material compounds that were subject to distortion. Although analog impressions serve their purpose sufficiently enough to remain in use, a margin for error is inherently built into a system where slight deviations can foster differentials. Experienced clinicians can compensate for these minor impression shortfalls, but in contrast, digital scanning has become an almost infallible resource for effective treatment planning and preventing misfits.
Intraoral scanning dates back several decades but entered the marketplace around 2006. Because a national economic downturn decreased production for all elective healthcare shortly thereafter, the dental profession was slow to implement new high-cost technology into practices.1 The dramatic evolution of digital technology in dentistry, though, came with such force that companies continued rapid expansion of the impression concept with a thrust toward simplification and cost-effectiveness for the clinician as well as increased comfort for the patient. Many of the early challenges have been effectively remedied, and within the past 8 years, the software has been made more intuitive, producing precise results.2 Additionally, the ease of digitally transmitting accurate information to laboratories, along with both time and shipping savings, has influenced many dentists to accept the learning curve required to propel an entirely digital workflow.3
Benefits of Digital Intraoral Scanning
Although the initial paradigm was that of digitally creating an impression, the author postulates that digital impression systems are much more than just data acquisition. The systems are the entry point into an entire ecosystem of digital workflow that results in precision, predictability, and cost and time savings, which in turn creates more comprehensive, affordable solutions for patients.
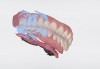
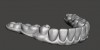
Designing a smile that a patient can preview in advance of treatment has become a critical tool in case acceptance. Clinicians recognize that emotional factors impact treatment planning, and with the assistance of software, they can now incorporate intraoral scanning with 2-dimensional (2D) images and videography to overlay a restorative plan on a patient's photograph, providing a glimpse of what can be expected from treatment4 (Figure 1). From a 2D proposed design, using intraoral scanning to create stereolithic (STL) files and cone-beam computed tomography (CBCT), the design can be translated into a 3D design in various software, which can then be shared with the patient (Figure 2). Patient confidence and satisfaction are both increased when the scanning and design software invite them more intimately into the planning process.
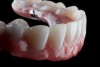
Scanning can continue to drive the workflow after diagnostics have been completed and clinical treatment commences. For preparation of natural teeth, smile design STL files move to a 3D printer or a milling machine to generate provisional crowns. Teeth are then prepared and provisional crowns fitted (Figure 3). New intraoral scans capture the surfaces of the provisional crowns with the teeth in occlusion to create a virtual articulator,5and additional scans of the preparation dictate the digital impression (Figure 4 and Figure 5). All this information can be recorded in a single visit, allowing a comprehensive file to be transported to the laboratory for the fabrication of an accurate definitive prosthesis. The laboratory then imports all of the scans into CAD/CAM systems and then to a milling machine to produce ceramic crowns. A 2015 study of ceramic crowns generated from both digital impressions and conventional silicone impressions concluded that the crowns made from digital impressions had a measurably better fit.6The final visit to deliver the crowns predictably can result in a mutually satisfying experience for doctor and patient, with precise clinical fit and the anticipated esthetics (Figure 6).
The application of intraoral scanning and the digital workflow is also highly impactful in dental implant therapies, enabling the clinician to execute prosthodontically driven treatment plans with a reduced number of procedures.7 The information collected by intraoral scanners can all be managed through software tools, permitting the technician to create virtual master models that contain all essential information.7
Case Report: Maxillary Prosthesis
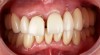
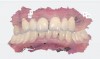
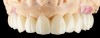
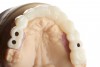
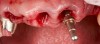
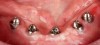
A patient presented for treatment with existing maxillary posterior implants, previously osseointegrated but unrestored, and a periodontally failing anterior dentition (Figure 7). An intraoral scan of the implants (using scan bodies) and the anterior teeth provided the laboratory with the necessary digital file to design posterior teeth that would harmonize with the anterior teeth (Figure 8). The same file was then sent for milling or 3D printing to create the full-arch provisional restoration. It is essential that the laboratory accurately digitize records in order to exactly replicate what was presented clinically8(Figure 9 and Figure 10).
At the patient's second visit, the anterior teeth were extracted and additional anterior implants placed (Figure 11). Abutments were connected and then temporary cylinders were installed. The provisional was screwed into the posterior implants, and the anterior implants were connected to the digitally produced provisional prosthesis (conversion prosthesis protocol: the immediate loading of a nonremovable interim prosthesis)9 (Figure 12). The immediate loading of a fixed transitional prosthesis allows adequate tissue protection and significantly elevates the patient's level of function and self-esteem immediately postoperatively.9
After the appropriate healing time, intraoral scanning of the provisional teeth, all sides and surfaces and in occlusion with the opposing dentition, took place. The provisional prosthesis was then unscrewed, and a material-based impression was made of the implant positions. Along with this one physical analog step, a digital impression of the implants, both anterior and posterior, using scan bodies, was taken. During the same appointment, the master cast was fabricated and mounted using the existing provisional, and then scanning of the provisional on the master cast in occlusion was performed using the intraoral scanner. This entire body of data acquisition, which was made in one clinical visit, provided the body of information required for the laboratory to produce the definitive prosthesis.
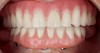
This is a case in which the entire treatment plan from the collection of diagnostics to the delivery of the definitive prosthesis was driven by reliance on digital technology and resulted in an effective functional and esthetic solution that was pleasing to the patient and accomplished in a minimal number of visits.
Case Report: Mandibular Prosthesis
Dental implants have become one of the most widely used treatments for the rehabilitation of edentulism.10 The All-on-4® (Nobel Biocare, nobelbiocare.com) treatment concept, after many studies and published results, has emerged as a conservative, cost-effective protocol for a wide range of patients.
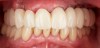
A patient presenting with an edentulous mandible and previously opting for All-on-4 surgical implant placement arrived for a final impression appointment adequately healed and wearing a satisfactory conversion prosthesis (Figure 13). All implants were osseointegrated with no clinical movement, mucosal tissue was uninflamed and healthy, all abutments were firmly connected to the implants, and the patient was comfortable and well-satisfied with the esthetics (Figure 14). All factors were ideally suited to proceed to the final impression and the construction of a definitive prosthesis.
Once again, scanning technology played a major role in the achievement of the result. A physical bite registration was acquired and an analog impression taken following rigid procedural guidelines11 to ensure accuracy of the master cast. This technique is contingent on the abutments being fully seated on the implants with no gaps existing between the abutments and the temporary cylinders of the conversion prosthesis, which is reconnected to the abutments with long guide pins used to make an open tray impression.11A digital scan of the conversion prosthesis mounted in an articulator and intraorally in maximum intercuspation was recorded with an intraoral scanner, completing the file record sent to the laboratory (Figure 15). Finally, the conversion prosthesis was polished, disinfected, and reinstalled in the patient's mouth to await the delivery of the definitive prosthesis-in this case, an acrylic resin prosthesis on a 3D-printed titanium framework.
In the laboratory, scanning technology continued. The technician scanned the raw master cast with analogs, using scan bodies firmly attached. Scan bodies are used so the data of the resultant scans will have appropriate information about the long axis of the implant.12 This scan, along with the digital scans performed at the single clinical visit, together provided sufficient data for the 3D design and resultant fabrication of the definitive prosthesis (Figure 16). Within the design software, minor adjustments can be made to the position of the teeth and to the articulation. After the virtual design was complete, the virtual files were sent to manufacturing for the production of two aspects of the definitive prosthesis, beginning with the overall position of the teeth in relationship to one another and to the implants. Within the confines of the tooth positions, the framework design was completed (Figure 17). The STL file for the titanium framework went to a laser sintering 3D printer. After framework fabrication, the tooth position file was sent to a 5-axis milling machine, where a polymethyl methacrylate (PMMA) monolithic puck, which was created by embedding the finished titanium framework within it, was shaped to the precise position of the teeth surrounding the titanium framework, thus producing the final hybrid prosthesis13 (Figure 18). The prosthesis then arrived to be delivered to the patient, with no interim visits necessary. It fit precisely because of the accuracy of combining the scans from the intraoral scanner with the single scan from the laboratory scanner of the verified master cast.
The Importance of Digital Scanners for Impressions
Digital implant dentistry has transformed the relationship between the dentist and dental laboratory. Digital impressions have been one of the leading factors driving this trend. Digital impression scanners eliminate tray selection, dispensing and setting of impression materials, disinfection, and costs in both time and dollars for shipping. Most importantly, they contribute to the comfort of the patient throughout the treatment.14
In the operatory, the impression procedure is the first and most essential step in achieving precision.15Current analyses comparing conventional impression techniques with intraoral scanning technology indicate that the digital approach is at least equal, if not superior, in precision to traditional methods, and it significantly streamlines procedures. The accuracy of the impression effectively bears the success of the definitive restoration because inaccuracy compounds all further steps in the process, resulting in remakes and wasted clinical time that can be the cause of both biologic and mechanical complications.16
Karl et al underscored that the accuracy in passive fit between prostheses and implants is the key to avoiding biologic and mechanical failures.17 Their study emphasized the role of the intraoral impression and the integrity of the master cast presented for CAD/CAM technology as the hallmarks that guarantee precision. Their conclusion, supported by previous research, indicated that crowns developed using intraoral scanning technology were preferred over crowns using conventional impressions.18
Conclusions
The impact of digital technology in the dental practice has grown considerably. Marinello stated that virtually all current clinical and technical prosthodontic procedures can be supported by new digital processes and that consequently, communication between the dentist, dental technician, hygienist, and patient has become markedly faster and more efficient.19 Many clinicians who have embraced the complete digital model also realize increased profitability as a result of streamlined efficiency. The technology has affected planning, designing, and manufacturing of surgical guides, provisionals, and fixed and removable final restorations. In some cases, digital technology drives every phase of the treatment plan, from diagnosis to delivery.
Patients benefit substantially from the digital revolution. Less time is spent in the chair, procedures are less invasive, and cost savings to the doctor can be passed to the patients, resulting in availability of care in a wider range. Patients may feel they have some participation in the planning of their treatment, which may positively influence the dentist-patient relationship, acceptance of care, and satisfaction with the results.
Dentistry has kept pace with the medical profession in making great progress with digital enhancements, but some clinicians remain resistant to rapidly advancing technology. In this author's opinion, they are at risk of being left behind. As each new technological achievement emerges and data become available only through software, with automation replacing manual labor, the traditional dogmatic paradigms of restorative fabrication concepts may effectively become obsolete.
The prosthodontic approach to precision is supported and advanced by the dramatic growth of digital concepts for achieving and preserving smiles. Clarity, consistency, reliability, and simplicity are on the front line of the digital revolution. Managing these systems carefully leads to the practice of premium care, profitability, and patient satisfaction, which are the three hallmarks of professional achievement in dentistry.
Acknowledgment
The author thanks Joanne M. Balshi for editorial assistance.
About the Author
Sundeep Rawal, DMD
Senior Vice President, Implant Support at Aspen Dental
Private Practice Specializing in Prosthodontics
Cofounder, Digital Dentistry Institute
References
1. Avery D. Digital impression technology. Inside Dental Technology. 2012;3(11). https://www.aegisdentalnetwork.com/idt/2012/12/digital-impression-technology. Accessed October 31, 2019.
2. Jurim B, Jurim A. A review of intraoral scanning technology. Inside Dental Technology. 2019;10(9):40-42.
3. Raudys D. Traveling behind the scenes with an intraoral scan. Glidewell. Inclusive. 2019;5(3). https://glidewelldental.com/education/inclusive-dental-implant-magazine/volume-5-issue-3/traveling-behind-the-scenes-with-an-intraoral-scan/. Accessed October 31, 2019.
4. Coachman C, Calamita MA, Coachman FG, et al. Facially generated and cephalometric guided 3D digital design for complete mouth implant rehabilitation: a clinical report. J Prosthet Dent. 2017;117(5):577-586.
5. Balshi TJ, Wolfinger GJ, Balshi SF. Positioning handle and occlusal locks for Teeth-in-a-Day Protocol. J Prosthet Dent. 2016;115(3):274-277.
6. Rhee YK, Huh YH, Cho LR, Park CJ. Comparison of intraoral scanning and conventional impression techniques using 3-dimensional superimposition. J Adv Prosthodont. 2015;7(6):460-467.
7. Monaco C, Scheda L, Baldissara P, Zucchelli G. Implant digital impression in the esthetic area. J Prosthodont. 2019;28(5):536-540.
8. Balshi TJ, Balshi SF. A new digital solution for implant-supported restorations. Inside Dental Technology. 2017;8(3):40-46.
9. Parel SM, Balshi TJ, Sullivan DY. Modifications of existing prosthesis with osseointegrated implants. J Prosthet Dent. 1986;56(1):61-65.
10. Agustín-Panadero R, Peñarrocha-Oltra D, Gomar-Vercher S, Peñarrocha-Diago M. Stereophotogrammetry for recording the position of multiple implants: technical description. Int J Prosthodont; 28(6):631-636.
11. Balshi TJ, Wolfinger GJ, Alfano SG, et al. Fabricating an accurate implant master cast: a technique report. J Prosthodont. 2015;24(8):654-660.
12. Giménez B, Özcan M, Martínez-Rus F, Pradíes G. Accuracy of a digital impression system based on parallel confocal laser technology for implants with consideration of operator experience and implant angulation and depth. Int J Oral Maxillofac Implants. 2014;29(4):853-862.
13. Kattadiyil MT, Goodacre CJ, Lozada JL, Garbacea A. Digitally planned and fabricated mandibular fixed complete denture. Part 2. Prosthodontic phase. Int J Prosthodont. 2015;28(2):119-123.
14. Christensen GJ. Impressions are changing: deciding on conventional, digital or digital plus in-office milling. J Am Dent Assoc. 2009;140(10):1301-1304.
15.Papaspyridakos P, Gallucci GO, Chen CJ, et al. Digital versus conventional implant impressions for edentulous patients: accuracy outcomes. Clin Oral Implants Res. 2016;27(4):465-472.
16. Chia VA, Esguerra RJ, Teoh KH, et al. In vitro three-dimensional accuracy of digital implant impressions: the effect of implant angulation. Int J Oral Maxillofac Implants. 2017;32(2):313-320.
17. Karl M, Graef F, Schubinski P, Taylor T. Effect of intraoral scanning on the passivity of fit of implant-supported fixed dental prostheses. Quintessence Int. 2012;43(7):555-561.
18. Henkel GL. A comparison of fixed prostheses generated from conventional vs digitally scanned dental impressions. Compend Contin Educ Dent. 2007;28(8):422-431.
19. Marinello C. The digital revolution's impact on prosthodontics. Int J Prosthodont. 2016;29(5):431-433.