You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
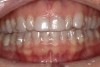
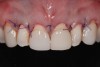
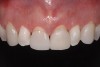
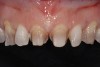
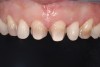
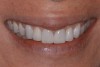
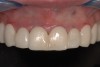
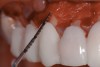
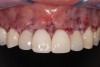
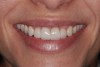
Past and recent studies suggest that high smile lines (Figure 1) are present in a considerable amount of the adult population,1 possibly affecting up to about 29% of patients.2 In a previous article (Part 1), the authors proposed a revised classification of the possible causes of gummy smile (GS) and short tooth syndrome (STS) and suggested a diagnostic process aimed at defining the etiological causes and correlating them to the responsible anatomical area(s).
When this condition is confined to the dental and/or periodontal structures, it is important to identify if the pink/white disproportion is due to incisal wear or an altered eruption. Coslet et al3 classified the altered passive eruption (APE) into four subclasses. More recently, two types of altered eruption have been described: altered active eruption (AAE) and APE.4
APE is determined by the failure of passive dental eruption, giving rise to excessive gingival overlap on the anatomical crown of the tooth while the distance from the bone crest to the cemento-enamel junction (CEJ) remains normal. With AAE, there is primary failure of the active dental eruption phase, which results in the tooth failing to emerge sufficiently from the alveolar bone, thereby leaving the CEJ extremely close to the bone crest. This situation, in turn, would prevent apical migration of the gingiva during the passive eruption phase.4
The clinical analysis of the incisal margins, the localization of the CEJ, and the use of radiographs can be used for diagnosing the intraoral causes of the disproportion. The presence of dental wear, however, does not necessarily exclude the simultaneous presence of an AAE or APE.
Once a precise diagnosis has been made, the goal of interdisciplinary treatment is to obtain the ideal coincidence of anatomical crown and clinical crown, the correct crown width/height proportion, and the ideal 3-dimensional positioning of incisal margin within the “smile stage.”5
In treating GS and STS patients, the periodontist may adopt two different approaches that could be defined as biological or restorative. In the biological approach, the key objective is to reestablish the physiologic distance between the CEJ and gingival margin and, thus, between the CEJ and bone crest. Therefore, this kind of treatment is indicated for patients with gingival hyperplasia,6 as well as AAE or APE. The therapeutic goal of the restorative approach is to improve smile esthetics only by obtaining a harmonious line of the gingival zeniths and by restoring correct proportions of the clinical crowns using crowns and bridges. When using this type of therapeutic approach, a series of compromises may have to be accepted, because final restorations recreate the restorative margin mimicking the CEJ in positions that may differ from their original anatomical positions. This approach is mainly indicated with fixed prostheses.
Surgical Indications and Technique
1. Biological Approach in Gingival Enlargement
The presence of a pseudopocket may confirm the presence of gingival hyperplasia.7 Bone sounding with a periodontal probe under local anesthesia may help to measure the biologic width. The scope of the surgery entails reducing the amount of gingiva and placing the gingival margins at close proximity to the CEJ.8 The most commonly used techniques are gingivectomies with an external bevel9 or an apically positioned flap with an internal bevel.10
2. Biological Approach in Altered Eruption
Sounding under local anesthesia will allow the clinician to differentiate between an active and a passive altered eruption, because these two conditions may coexist in the same area. The surgical guide is not absolutely necessary, because the amount of gingival scalloping is dictated by the position of the CEJ; this could be determined by extrapolating the dimension clinically and radiographically.
A paramarginal incision should be used if a wide band of gingiva is present and at least 2 mm of it would remain after scalloping; if a narrower band of gingiva is present, an intrasulcular incision should be used. The papilla will be incised at the base and be left in place. A full-thickness flap will be raised in cases in which an abundant quantity of gingiva exists; otherwise, a mixed flap will be preferred: full-thickness flap in the more coronal area and partial-thickness flap in the interdental and apical portions. After flap elevation, osteoplasty and ostectomy can be performed. The ostectomy is carried out only in cases of AAE. This phase can be executed with surgical burs mounted on rotatory instruments, or piezoelectric surgical handpieces, which allow a more precise and less traumatic resective surgery.11
During the procedure, the surgical guide is repositioned in the mouth to assess if there is a constant and adequate distance between the osseous margins and the planned outline. After repositioning the flaps, an interdental 5.0 or 6.0 suture is placed. In cases in which a mixed flap is used, the flap is kept in place by suturing it to the underlying periosteum.
3. Surgical Technique in the Esthetic Restorative Approach
This approach is indicated in cases that require anterior crown lengthening surgery, where the CEJ can no longer be the reference point. In patients with anterior wear due to bruxism and parafunction, subsequent compensatory eruption can, in fact, result in irregular CEJ positions and a gingival zenith line instead of a regular parabolic or “W” line,12 or when patients choose not to have orthodontic treatment.
Because the CEJ cannot be used as a reference, the surgical guide, which is fabricated according to the esthetic guidelines, has an important role during the surgery. The incision can be intrasulcular or paramarginal, depending on the amount of keratinized tissue present. In cases in which a paramarginal incision is used, it is important to leave at least 2 mm of gingiva.13
Flap elevation follows the same guidelines as the previous approach, leaving a distance of approximately 3 mm between bone margin and the surgical guide. The bone should have an ideal physiologic form, and the flaps are closed with vertical mattress sutures.
Biological Approach (Case 1)
In case 1 (Figure 2 through Figure 10), the main contributing factor to the gummy smile was AAE. After a thorough clinical and radiographic examination, the therapeutic approach was aimed at resolving the intraoral cause to offset the esthetic problem.
Invisalign® arch alignment (Figure 2) was used to resolve the Bolton discrepancy by expanding the upper and lower arches. This would result in upper incisor diastemas, which initially would emphasize the incisive lateral microdontia but would subsequently be restored with porcelain veneers.
A laboratory-made wax-up was used as the basis of the mock-up, which was carried out to define and study the final esthetics of the patient’s smile. After making changes to the mock-up in consultation with the patient, a surgical guide was produced to indicate the surgical incisions to be made by the periodontist during the surgery.
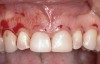
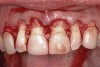
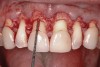
Following anesthesia, a scalloped incision was made on the keratinized tissue (Figure 3). In the interproximal area, a papilla-sparing incision was made. A full-thickness flap was raised to give access to the underlying bone (Figure 4). Both osteoplasty and ostectomy were performed to position the bone crest approximately 2 mm to 3 mm from the CEJ (Figure 5). The gingival tissue was repositioned, coinciding with the initial labial incision and the interproximal papilla. Interrupted sutures were placed (Figure 6), which were removed 7 days following the surgery.
After healing (Figure 7), previous restorations were removed (Figure 8) and the existing preparations were modified; the laterals and canines were also prepared for veneers to the ideal biological position. Pigmented dentin (resulting from tetracycline use) was exposed once the previous restorations were removed, and the new preparations were finalized.
“Masking buildup” was performed (Figure 9), according to the concepts of immediate dentin sealing.14 A slightly opaque veneer composite cement was used for cementation and to enhance the masking effect (Figure 10).
Restorative Approach (Case 2)
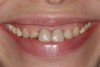
The patient who presented in this case (Figure 11 through Figure 20) had a history of bulimia nervosa. She had previously commenced treatment with another dentist but was dissatisfied with her dental esthetics (Figure 11).
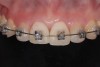
The two central incisor crowns were replaced with new provisionals, and composite was used to restore her canines. Following this, fixed orthodontic therapy was started. The intention was to lingually displace and intrude the anterior teeth and reduce their torque (Figure 12).
The laboratory-made wax-up was used to produce the mock-up (Figure 13), which was aimed at creating the ideal form and proportions of the final restorations and reproducing the gingival zeniths.
A surgical guide was used for the anterior crown-lengthening procedure. It was intended to balance the width-to-height ratios of the teeth and to give an adequate biologic width for the two central incisors (Figure 14). The band of gingiva was preserved, and an intrasulcular incision was made (Figure 15). The flap was elevated, leaving an intact periosteum on the bone of the interdental spaces (Figure 16). The surgical guide was necessary during the bone resection (Figure 17), because there was no reference point. Ostectomy was performed to leave a distance of about 3 mm from the bone crest to the margin of the surgical guide (Figure 18). The flap was repositioned, and periosteal interrupted sutures were used to stabilize it (Figure 19).
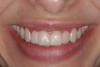
The temporary crowns were replaced with single crowns, and porcelain veneers were used on the upper laterals and canines (Figure 20). Knife-edge preparations were used for the final restorations as they were situated on radicular surfaces of the teeth, though this would affect the adhesion of the restorations.15
Discussion
In GS cases in which the problem may be treated or compensated for with routine periodontal treatment, it is important to first diagnose the presence of an altered passive or active eruption.3,4,16 The aim of the surgery is to restore the dimensions of the anatomical crown with respect to the gingival and osseous tissues, by exposing the portion of enamel surface covered by the gingiva. This is what the authors define as the “biological approach.”
Distinction between active or passive altered eruptions is necessary, because as in the first case the surgery required both osteoplasty and ostectomy, whereas in the second case a gingivectomy may be sufficient.17 Performing only a gingivectomy in areas of AAE would lead to failure of the treatment caused by reestablishment of the biologic width at the same position.17
Some authors suggest that esthetic and prosthetic reference points should be used to outline the surgical incision and also guide the quantity of ostectomy through a surgical guide.18 Often though, asymmetrical wear of incisal margins, consequent asynchronous and asymmetrical compensatory eruption, and frequent possibility of altered eruption are observed. Surgically exposing the CEJ position is important. Orthodontic treatment aligns the teeth in their ideal positions, and, finally, the restorative phase is completed.
Therefore, when performing surgery with a biological approach, the correct reference point is not determined by the surgical guide but by the CEJ. The surgical guide may be used for the soft-tissue incision to transfer the information extracted from clinical and radiographic examinations and not from an esthetically or prosthetically guided stent.
Traditionally, the vertical parameters considered in orthodontic treatment—in relation to the lip line—were the posterior occlusal plane, gingival margins, crown lengths, and incisal plane.19 Teeth were aligned in relation to their incisal margin, but this applies when no incisal wear has occurred. The gingival margin position was also considered20; vertical discrepancies were corrected without taking into consideration if altered eruption was present. This is why the authors propose the necessity of revealing the correct CEJ location with the biological approach.
Maintaining the preparations to within undercut-free areas, which conversely occurs when the preparations are made apical to the CEJ,21 minimizes useless removal of tooth structure. The biological approach is favorable for prosthodontists because final adhesive restorations are placed on the enamel surface, improving the longevity on the restoration margin22 and providing ideal profile and contour of the restoration and long-term periodontal health.
The restorative approach includes cases with previous crowns in which the CEJ can no longer be located, there are malaligned teeth, and teeth with loss of periodontal attachment. In these situations the goal of the surgery is to lengthen the crown using esthetic and structural parameters such as the crown-root ratio, the periodontal status, and the incisal margin position.23 With this approach, where full-crown restorations are already present with margins apical to the CEJ, the emergence profiles are often over-contoured to promote biologically acceptable gingival contours, although this can lead to an esthetic compromise.23
Conclusion
Periodontists may adopt two different approaches when treating GS and STS patients: biological or restorative. Regardless of the planned therapeutic approach, misdiagnosis of an altered eruption due to the absence of a valid and repeatable diagnostic protocol can create esthetic and periodontal failures, such as misproportioned teeth and unnatural lengthening of incisal margins, which may jeopardize the smile and facial esthetics and cause longer anterior guides.24 Furthermore, restorative margins placed too far coronally from the CEJ may be at risk of subsequent and progressive resolution and compensation of the altered eruption with time and, ultimately, esthetic failure.
Disclosure
The authors had no disclosures to report.
About the Authors
Simone Verardi, DDS, MSD Affiliate Assistant Professor, Department of Periodontics, University of Washington School of Dentistry, Seattle, Washington; President, Schluger-Ammons Study Club, Seattle, Washington; Private Practice, Seattle, Washington
Marjan Ghassemian, BDS, DDS Unit of Oral Surgery and Implant-Prosthetic Rehabilitation, Catholic University of the Sacred Heart, Rome, Italy
Andrea Bazzucchi, DDS, MSD Private Practice, Rome, Italy
Antonello F. Pavone, DDS Co-director, Dental Esthetic Center at LaClinic-Montreux-Switzerland; Co-owner and Scientific Director, Solo Sorrisi dental clinics and iSmile Coaching
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Tjan AH, Miller GD, The JG. Some esthetic factors in a smile. J Prosthet Dent. 1984;51(1):24-28.
2. Kokich VO Jr, Kiyak HA, Shapiro PA. Comparing the perception of dentists and lay people to altered dental esthetics. J Esthet Dent. 1999;11(6):311-324.
3. Coslet JG, Vanarsdall R, Weisgold A. Diagnosis and classification of delayed passive eruption of the dentogingival junction in the adult. Alpha Omegan. 1977;70(3):24-28.
4. Chu SJ, Karabin S, Mistry S. Short tooth syndrome: diagnosis, etiology, and treatment management. J Calif Dent Assoc. 2004;32(2):143-152.
5. Janzen EK. A balanced smile—a most important treatment objective. Am J Orthod. 1977;72(4):359-372.
6. Brunet L, Miranda J, Roset P, et al. Prevalence and risk of gingival enlargement in patients treated with anticonvulsant drugs. Eur J Clin Invest. 2001;31(9):781-788.
7. Glossary of Periodontal Terms. 4th ed. Chicago, IL: American Academy of Periodontology; 2001.
8. Cook DR, Mealey BL, Verrett RG, et al. Relationship between clinical periodontal biotype and labial plate thickness: an in vivo study. Int J Periodontics Restorative Dent. 2011;31(4):345-354.
9. Orban B. Indications, technique and post-operative management of gingivectomy in the treatment of the periodontal pocket. J Periodontol. 1941;12:89.
10. Ramfjord S. Gingivectomy—Its place in periodontal treatment. J Periodontol. 1952;23:30.
11. Vercellotti T, Pollack AS. A new bone surgery device: sinus grafting and periodontal surgery. Compend Contin Educ Dent. 2006;27(5):319-325.
12. Townsend CL. Resective surgery: an esthetic application. Quintessence Int. 1993:24(8):535-542.
13. Lang NP, Löe H. The relationship between the width of keratinized gingiva and gingival health. J Periodontol. 1972;43(10):623-627.
14. Magne P. Immediate dentin sealing: a fundamental procedure for indirect bonded restorations. J Esthet Restor Dent. 2005;17(3):144-155.
15. Loi I, Di Felice A. Biologically oriented preparation technique (BOPT): a new approach for prosthetic restoration of periodontically healthy teeth. Eur J Esthet Dent. 2013;8(1):10-23.
16. Alpiste-Illueca F. Altered passive eruption (APE): a little-known clinical situation. Med Oral Patol Oral Cir Bucal. 2011;16(1):e100-e104.
17. Brägger U, Lauchenauer D, Lang NP. Surgical lengthening of the clinical crown. J Clin Periodontol. 1992;19(1):58-63.
18. Scutella F, Landi L, Stellino G, Morgano SM. Surgical template for crown lengthening: a clinical report. J Prosthet Dent. 1999;82(3):253-256.
19. Kokich V. Esthetics and anterior tooth position: an orthodontic perspective. Part II: Vertical position. J Esthet Dent. 1993;5(4):174-178.
20. Bellamy LJ, Kokich VG, Weissman JA. Using orthodontic intrusion of abraded incisors to facilitate restoration: the technique’s effects on alveolar bone level and root length. J Am Dent Assoc. 2008;139(6):725-733.
21. Magne P, Magne M, Belser U. The esthetic width in fixed prosthodontics. J Prosthodont. 1999;8(2):106-118.
22. Layton D, Walton T. An up to 16-year prospective study of 304 porcelain veneers. Int J Prosthodont. 2007;20(4):389-396.
23. Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000. 1996;11:29-38.
24. Ekfeldt A, Karlsson S. Changes of masticatory movement characteristics after prosthodontic rehabilitation of individuals with extensive tooth wear. Int J Prosthodont. 1996;9(6):539-546.