You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Amelogenesis imperfecta (AI) is an inherited disorder of enamel with mutations in five genes—AMEL, ENAM, MMP20, KLK4, and FAM83H—and a wide range of clinical presentations. It affects the structure and appearance of the enamel of all teeth, both in the primary and secondary dentitions.1 Teeth with this condition tend to be unusually small, discolored, pitted or grooved, and prone to rapid wear and breakage. With generalized compromise of enamel, there is loss of vertical dimension as well as lack of interproximal contacts, resulting in food lodgment and problems associated with it. In most cases the esthetic disability is striking.
The high morbidity for such patients presents major restorative challenges during formulation of the treatment plan. Lack of mature enamel for bonding can be a formidable handicap when employing contemporary treatment protocols in adhesive dentistry. For patients suffering from AI, there is a strong need for conservative treatment options that save the existing tooth structure while providing a durable treatment.
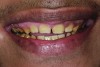
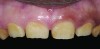
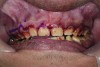
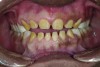
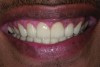
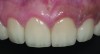
The authors report on a 21-year-old patient who presented with severe discoloration and mild sensitivity of teeth (Figure 1). The teeth visible in his smile were very short, unsightly, and unbecoming for his age.
Clinical Assessment
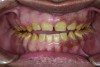
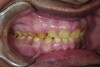
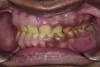
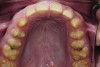
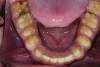
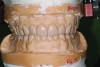
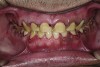
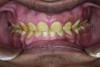
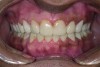
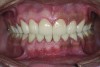
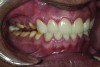
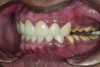
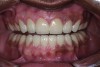
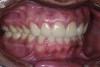
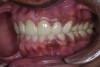
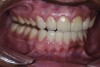
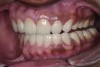
A thorough clinical examination and analysis were carried out to assess the esthetic and functional problems of the patient (Figure 2 through Figure 7). The medical history was non-contributory, except for mild leukoderma. Temporomandibular joint (TMJ) function was within normal range.
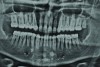
Mounted study casts were used to evaluate occlusion. The relevant findings were as follows2: Facial analysis revealed a canted maxillary occlusal plane and canted dental midline. Dentolabial analysis showed that the maxillary incisors were not adequately visible during repose; it also revealed a reverse smile line, as well as a wide smile showing 12 teeth. Results from the phonetic analysis were that “F” and “V” sounds revealed upper incisal shortening, “M” and “S” pronunciation disclosed a diminished vertical dimension of occlusion (VDO), and “E” sounds showed severe shortening of incisors. Dental analysis revealed thick biotype, asymmetry and inappropriate location of gingival levels and zenith, incorrect axial inclinations, a displeasing width-to-length ratio, and pitted surfaces on most teeth. Interproximal decay was evident on several posterior teeth, as revealed by radiographic analysis. Finally, occlusal examination indicated discrepancy between maximum intercuspation (MIP) and centric relation (CR) as well as a lack of anterior guidance/posterior disclusion.
Risk Assessment
Risk assessment strategies are used to gauge the potential difficulties in treatment execution and understand the potential treatment outcome. A systematic approach was used for periodontal, biomechanical, functional, and dentofacial analysis.3 Periodontally, the patient was low-risk, as there was minimal bone loss and no bleeding on probing, consistent with American Academy of Periodontology (AAP) classification. Biomechanically, the patient was deemed to be at moderate risk, as there was interproximal decay, and, structurally, the lack of enamel would make the teeth susceptible to lower bond strengths with the restorations. Functionally, the patient was considered to be at moderate risk. Although the patient had acceptable function, the MIP was not coincident with CR, and there was occlusal wear on most teeth. Since the occlusal surfaces of all teeth would need restorative treatment to reassign the VDO, CR would be the starting point for reconstruction. Lastly, dentofacially the patient received a moderate risk rating, as there was maximum tooth display and marginal gingival display due to the position of the lip line.
Comprehensive Treatment Concept
The treatment plan was developed by identifying achievable clinical goals that included establishing: the correct VDO; dentofacial harmony, keeping in mind smile design principles; MIP in harmony with CR; and effective anterior guidance to provide posterior disclusion in harmony with the envelope of function.
A clinical observation in various cases of full-mouth rehabilitation and in cases of AI is that before post-core restorations, the clinician may devitalize the pulp while performing endodontic treatment for most or all teeth. In some cases, crown-lengthening surgery with bone removal may be necessary to attain sufficient tooth structure and retention form for restorations and to allow the clinician to prepare teeth as needed to gain space for restorative material. However, this approach also leads to weakening of the tooth structure.4
A contemporary approach in cases of AI is to adequately open the VDO within the physiologic limits of esthetics and phonetics and use adhesively retained crowns with minimal tooth preparation. This approach allows teeth to retain their original strength and vitality.
Choice of Restorative Materials and Design
Because the enamel is defective circumferentially around all teeth in AI, full-coverage restoration is the ideal choice. Partial-bonded porcelain restorations may not achieve sufficient bond strength in such cases and leave uncovered defective tooth structure prone to decay. Porcelain-fused-to-metal (PFM) restoration is known to have good strength and reasonable esthetics. However, traditional PFMs require significant tooth reduction to achieve translucency and optical properties, thus necessitating endodontic intervention in AI-affected teeth. Therefore, in this case PFM restorations were not considered as a restorative option.
The restorative material of choice in such cases must have the ability to provide excellent optical properties and esthetics with reasonably good strength. Lithium disilicate is an ideal choice. (In this case, e.max® [Ivoclar Vivadent, www.ivoclarvivadent.com] was used.) Improvements in formulations of lithium disilicate5 have resulted in less tooth structure needing to be removed while still providing good esthetics and strength in thinner layers. Moreover, if the underlying tooth color does not need a drastic shade change, these restorations can be fabricated with supragingival or equigingival margins, thereby eliciting a stable biologic response from the periodontium. With minimal overall tooth preparations, the structural integrity of the tooth is preserved, so as to resist crack propagation.6
Furthermore, using lithium disilicate in monolithic form for full-contour posterior occlusal surfaces provides better strength than layering a core of lithium disilicate with veneering porcelain, thereby eliminating concerns regarding chipping of the veneering porcelain. In addition, its ability to adhesively bond to the underlying substrate eradicates the need for a retentive form in the tooth preparation. Bonding to well-formed enamel is clinically verified by the typical chalk-white enamel surface after phosphoric acid-etching. However, because AI patients suffer from a reduced enamel layer—especially in hypoplastic AI—bonding not only to enamel but also to dentin is important. Short-etching with phosphoric acid (total-etch) or the application of self-etching primers is recommended.7 Recent clinical studies investigating enamel wear of monolithic lithium disilicate demonstrate that it seems to be within the range of normal enamel wear.8
Porcelain-veneered zirconia crowns are another option that can be exercised in AI cases. However, the high rate of fracture (3% to 25%) of veneering porcelain from underlying strong ceramic cores such as zirconia has been shown in the literature.9 Up to 90% of the porcelain-veneered zirconia crowns failed from veneer chip-off fracture in relatively fewer cycles and lesser force as compared with monolithic lithium disilicate.10 Additionally, the inherent opacity of zirconia cores can make achieving good translucency more difficult unless tooth preparation is aggressive and allows for ample room for veneering translucent porcelain.
Diagnostic Esthetic Preview
The first step in a complex case such as this is to create a blueprint for the final restorations in the form of a diagnostic wax-up. The maxillary casts are mounted with a facebow record that aids in correct reproduction of the orientation of the maxilla in the cranium. Deprogramming the mandibular muscles and mounting the lower study casts with a centric record at an increased VDO is done to study the occlusion without interferences from teeth guiding the mandibular condyle away from a fully seated CR. Once the casts are mounted simulating the jaw positions accurately, a decision must be made regarding the VDO and the proportions of the final teeth. There are no specific formulae in determining VDO. Clinical judgment is made based on using some or all of the following guidelines to increase/restore VDO11: cephalometric analysis; esthetics (lip position in rest, repose, and smiling); phonetics (F, V, M, and S sounds); minimum amount of space required to accommodate restorative materials; TMJ x-rays (transcranial views/cone beam computed tomography [CBCT]); freeway space (which can be subjective and unreliable); and patient perception of comfort.
The thickness of the occlusal enamel layer on molars is generally in the range of 2 mm to 2.5 mm.12 In this case, because the entire layer of enamel was missing from both jaws, it was decided to arbitrarily raise the vertical dimension on the articulator by 4 mm. This was the vertical dimension at which the wax-up was generated.
Determining Incisal Edge Position
The starting point in rehabilitation is to determine the horizontal and vertical positions of the incisal edge of the maxillary incisors. The vertical position of the incisal edge governs the length of central incisors and depends on several factors, including: envelope of function; anterior guidance; upper lip positions in rest/repose/smiling; soft-tissue characteristics; facial proportion; cultural variations; and phonetics (F, V, and E sounds). The horizontal position, on the other hand, governs the incisal profile and its labiolingual orientation.13 The horizontal position of the incisal edge must accommodate the patient’s envelope of function.
A direct mock-up was carried out in the patient’s mouth with light-cured composite resin used to add length to the incisal edges of the upper anterior teeth. The length and incisal profile was verified for esthetics and phonetics. The lengths of teeth Nos. 8 and 9 with reestablished incisal length were measured from the gingival margin to the incisal edge. All of this incisal edge position information was provided to the laboratory during wax-up (Figure 8).
The wax-up was to be made after correction of gingival levels and zeniths of teeth on the stone models. The gingival levels should be decided on the basis of maintaining the width-to-length ratio of central incisors close to the ideal parameter of 0.8.14 Once the gingival level of the centrals was determined, a tangent drawn to that line onto the cuspids allowed visualization of the proposed gingival level for the cuspids. The greatest corrections in gingival levels were needed in the upper cuspid and bicuspid regions.
Measurements were made from the incisal edge of the cuspids to the proposed new gingival levels on stone casts. These measurements were used to mark the proposed gingival margin for the cuspids in the patient’s mouth. Similar markings were done for all upper teeth, maintaining the principle of having gingival margins of cuspids and centrals at an equal level and having gingival margins of laterals coronal to them.15
Esthetic Repositioning of Gingival Tissues
After administering local anesthesia, a periodontal probe was used to sound the bone on facial and interproximal aspects of all upper teeth. With the upper cuspids and bicuspids, there was insufficient distance between the proposed free gingival margin and the crestal bone (< 3 mm) (Figure 9). In such circumstances, merely trimming the gingival tissues without altering the bone could lead to a violation of biologic width, with its associated complications, one of which is the rebound of gingiva to its original level. Thus, for these teeth, an osteoplasty, along with gingival resection, was carried out. On most other teeth, including the lower anterior and posterior teeth, a gingivectomy was sufficient to achieve correction of gingival levels and proper width-to-length ratios of teeth.
An aspect of crown lengthening in cases of AI is to leave the gingival margins at the cementoenamel junction (CEJ) of the teeth. This is done so that any defective and pitted enamel is exposed and tended to in the final restorative design. Failure to do this may lead to recurrent gingival ill-health due to plaque accumulation in the pitted surfaces. In this case, however, upon raising the mucoperiosteal flap, it was found that the CEJ was missing as a result of total absence of enamel. Thus, the gingival margins were placed at the desired esthetic levels and sutured with monofilament sutures (Figure 10) and reevaluated after a healing period of 4 weeks (Figure 11).
First Provisional Restoration/Mock-up
The wax-up at the desired empirical vertical dimension was finalized and checked for all esthetic and functional parameters. A putty silicone index was made of the full-arch upper and lower wax-up. To record the finer details and texture of the wax-up, the putty index was relined with light-body elastomer (Figure 12).
At 4 weeks after the esthetic repositioning of the gingival levels, the patient was scheduled for fabrication of the provisional restoration. The upper provisionals were fabricated first. All the teeth were cleaned with pumice slurry and etched with 37% phosphoric acid for 3 seconds. After gentle air-drying and isolation, bonding agent was applied to the teeth and light-cured for 20 seconds. The putty-wash index was loaded with bis-acryl composite (Protemp 4™, 3M ESPE, www.3MESPE.com) and placed over the teeth with correct orientation that was verified by checking that the index was fully seated. Undue pressure on any one side of the putty index must be avoided to achieve correct contours on the provisional.
After the material had set, the index was removed. A correctly fabricated index will show a thin uniform flash of excess material, which, in this case, was carefully peeled off and cut with a sharp #12 blade. The provisionals on the lower jaw were fabricated in a similar manner. Once the gross excess was removed, the patient was guided to close in MIP, with the condyles guided to CR. The occlusal contacts were then marked and adjusted until uniform contacts of equal intensity were achieved on both sides and anterior guidance was sufficient to disclude posteriors in all eccentric mandibular positions (Figure 13 and Figure 14).
At this juncture, an evaluation of the esthetics, phonetics, VDO, and all other macro and micro elements15 of smile design should be verified. Any changes—additive or subtractive—can be carried out in the patient’s mouth itself. The full-face smile photographs and close-up views were taken and evaluated. The patient was asked to “test drive” the provisionals for a few weeks and report with any feedback so that necessary corrections could be carried out. At this time, even the functional aspects can be verified, and a transcranial radiograph or a CBCT scan may be taken to verify the position of condyle in the glenoid fossa.
The patient was asked to use the provisionals for another 6 weeks. At the end of 12 weeks from the day of gingival surgery, the patient was scheduled for the final impressions.16
Sequence of Fabrication of Final Restorations
The sequencing of final restoration plays a role in simplifying the treatment plan. One option is to fabricate all final restorations together. This requires precise records and use of a semi-adjustable articulator that will allow the accurate simulation of mandibular movements in protrusive and lateral excursions. It also requires the clinician to verify the anterior tooth lengths and contours that will be needed to design the posterior tooth form so that the teeth disclude during eccentric mandibular movements. Preparing all teeth and taking accurate impressions all simultaneously is a clinically demanding procedure.
Another sequencing option is to fabricate the upper and lower anterior teeth first, followed by all posteriors. This option requires the clinician to keep posterior provisionals in place while final impressions of the upper and lower anterior teeth are taken. These posterior provisionals will help maintain the desired VDO. In keeping with esthetic and phonetic guidelines, the anterior final restorations are designed to keep posteriors discluded during eccentric jaw movements. Once the anteriors are bonded, the posterior final impressions are taken, and these restorations are fabricated to conform to the established anterior guidance. This approach helps in simplifying the treatment procedure, but it requires more time and an extra seating for case completion.
Final Restorations
It was decided to follow the latter approach of making the anterior finals first. The approved provisional restorations were removed by cutting them back with burs of a known diameter so that a clearance of 0.5 mm to 1 mm was accomplished on the labial surface and 1.5 mm on the incisal. As the depth cuts were made on the anterior provisionals, it was found that the underlying tooth structure hardly needed any preparation at all. Once all provisional material was stripped off, a medium abrasive disc (Super-Snap®, Shofu, www.shofu.com) was used to smooth out the tooth surfaces (Figure 15). Usually, a chamfer margin is prepared conventionally in such restorative designs; however, since there was no enamel present in the cervical areas, the authors preferred to have a negligible-thickness, knife-edged margin placed equigingivally. The putty index from the provisionals was cut back and used to verify that sufficient clearance was present for the final restorations. The restorations were designed to replace the enamel layer on anterior teeth and also provide a definite CEJ.
Margin placement and tissue management was carried out as per conservative protocols to control the restorative-periodontal interface.17 A #000 retraction cord was packed in the healthy gingival sulcus. The margins were modified to be 0.5 mm intracrevicular. A custom tray was used to take the final impressions with polyether.
A stick bite record was made to orient the upper cast in the laboratory. Centric records were made by interposing warmed wax wafers between anterior teeth only and taking the records at the desired VDO. New provisionals were fabricated using the index from the wax-up.
The anterior restorations were fabricated with low-translucency lithium-disilicate ingots and layered in the incisal half to provide the desired internal characteristics in accordance with the patient’s age. The final anterior restorations were then tried-in and verified for marginal fit, esthetics, and phonetics. After the patient’s approval, they were bonded using dual-cured resin cement (Variolink® II, Ivoclar Vivadent) (Figure 16). Because the enamel in such cases is already compromised, bonding can become clinically unpredictable. A self-etching primer was used on the teeth, followed by a bonding agent (Clearfil™ ST Bond, Kuraray Dental, www.kuraraydental.com) that was light-cured for 20 seconds. The intaglio of the crowns was prepared by etching with 9% buffered hydrofluoric acid for 60 seconds and silanating them to achieve optimum bonds to the resin cement.18
The posterior provisionals were then removed and final preparations on posterior teeth were done (Figure 17 and Figure 18). Minimal occlusal preparation was needed, as the increase in VDO provided the required occlusal clearance. Margin placements were similar to the anterior teeth—knife-edged and equigingival. After recording the final impressions, a facebow record was made to orient the upper working cast with posterior tooth preparations. Centric record was made at the desired VDO with anterior final restorations providing the vertical stop during record making.
The final restorations were fabricated in the laboratory using monolithic lithium disilicate, and then tried-in in the patient’s mouth and verified for esthetics and function. They were then bonded with dual-cured resin cements following the same protocol as outlined for the anterior teeth.
The final restorations depicted restoration of form, function, and beauty, with good harmony of restoration and the periodontium (Figure 19 through Figure 25). MIP was in harmony with CR, and right and left lateral excursion discluded all posteriors with anterior group function. The postoperative orthopantomogram (OPG) (Figure 26) shows the treatment done while maintaining the vitality of anterior teeth.
Conclusion
Amelogenesis imperfecta leads to malformation of enamel, which in turn leads to structurally weaker teeth that are prone to decay. Several members of the dental team may be called upon to provide multidisciplinary treatment for these patients. As reported in this article, to stop further breakdown of the dentition in adult patients with involvement of the entire secondary dentition, a conservative restorative approach is paramount. The key elements for treatment planning such cases conservatively is to increase the VDO, use minimally invasive tooth preparations, use materials like lithium disilicate in a thickness that will preserve enamel, and use bonding protocols to adhesively retain the restorations.6 Achieving responsible esthetics19 without damaging the existing dentition will greatly benefit these young patients with congenital dental disorders such as AI.
ACKNOWLEDGMENTS
The authors wish to acknowledge the following dental team members: Sushrut Prabhudesai, MDS, for the osteoplasty and crown-lengthening procedure; and Bhakti Tunkiwala, MDS, for the laser-assisted gingival-level determination and gingivectomy in the lower anteriors.
DISCLOSURE
The authors have no affiliation with any of the products mentioned in this article.
ABOUT THE AUTHORS
Aliasger Tunkiwala, BDS, MDS
Private Practice with emphasis on Prosthetic and Implant Dentistry, Mumbai, India
Danesh Vazifdar
Owner, Adaro Dental Laboratory, Mumbai, India
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
REFERENCES
1. Gadhia K, McDonald S, Arkutu N, Malik K. Amelogenesis imperfecta: an introduction. Br Dent J. 2012;212(8):377-379.
2. Fradeani M. Esthetic Rehabilitation in Fixed Prosthodontics: Esthetic Analysis Volume 1. Chicago, IL: Quintessence Publishing; 2004.
3. Kois JC. New challenges in treatment planning-part 2. J Cosmet Dent. 2011;27(1):110-121.
4. Torbjörner A, Fransson B. Biomechanical aspects of prosthetic treatment of structurally compromised teeth. Int J Prosthodont. 2004;17(2):135-141.
5. Stappert CF, Att W, Gerds T, Strub JR. Fracture resistance of different partial-coverage ceramic molar restorations: an in-vitro investigation. J Am Dent Assoc. 2006;137(4):514-522.
6. Fradeani M, Barducci G, Bacherini L, Brennan M. Esthetic rehabilitation of severely worn dentition with minimally invasive prosthetic procedure (MIPP). Int J Periodontics Restorative Dent. 2012;32(2):135-147.
7. Kwong SM, Cheung GS, Kei LH, et al. Micro-tensile bond strengths to sclerotic dentin using a self-etching and a total etching technique. Dent Mater. 2002;18(5):359-369.
8. Esquivel-Upshaw J, Rose W, Oliveira ER, Anusavice KJ. In vivo analyses of enamel wear against ceramic materials [abstract]. J Dent Res. 2009;88(spec iss A): Abstract 1009.
9. Edelhoff D, Sorensen JA. Tooth structure removal associated with various preparation designs for posterior teeth. Int J Periodontics Restorative Dent. 2002;22(3):241-249.
10. Guess PC, Zavanelli RA, Silva NR, et al. Monolithic CAD/CAM lithium disilicate versus veneered Y-TZP crowns: comparison of failure modes and reliability after fatigue. Int J Prothodont. 2010;23(5):434-442.
11. Dawson PE. Evaluation, Diagnosis, and Treatment of Occlusal Problems. 2nd ed. St. Louis, MO: Mosby; 1989.
12. Nanci A. Ten Cate’s Oral Histology: Development, Structure, and Function. 6th ed. St. Louis, MO: Mosby; 2003.
13. Hess LA. Altering the incisal edge position for optimal function and esthetics. VISTAS Complete Predictable Dent. 2010;3(2):4-13.
14. Blitz N, Steele C, Wilhite C. Diagnosis and treatment evaluation in cosmetic dentistry: a guide to accreditation criteria. Madison, WI: Am Acad Cosmetic Dent; 2001.
15. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Chicago, IL: Quintessence Publishing; 2002.
16. Pontoriero R, Carnevale G. Surgical crown lengthening: a 12-month clinical wound healing study. J Periodontol. 2001;72(7):841-848.
17. Tunkiwala A. Controlling the periodontal-restorative interface to provide esthetic dentistry for an esthetically high-risk patient. Compend Contin Educ Dent. 2013;34(2):120-129.
18. Barghi N, Fischer DE, Vatani L. Effects of porcelain leucite content, types of etchants, and etching time on porcelain–composite bond. J Esthet Restor Dent. 2006;18(1):47-52.
19. Bakeman EM, Goldstein RE, Sesemann MR. Responsible esthetics: Is there a return to conservative esthetic dentistry? Inside Dentistry. 2010;6(6):36.